As the number of elderly patients increases, nurses and other healthcare providers must become knowledgeable about the special healthcare needs of the geriatric population. Undesired weight loss and malnutrition in the elderly are significant problems, leading to increased morbidity and mortality. Residents of skilled nursing facilities are at special risk. Geriatric failure to thrive is a diagnosis commonly used in geriatrics, and the four chief characteristics are impaired physical function, malnutrition, depression, and cognitive impairment. Participants who complete this course will learn about the identification, evaluation, and assessment of geriatric failure to thrive, including use of the Mini Nutritional Assessment, the Mini Mental Status Evaluation, and the Geriatric Depression Scale. Diagnostic/laboratory and physical assessment skills will be reviewed with a focus on weight-loss assessment. Creation of a multidisciplinary treatment plan with review of pharmaceutical options will be explored. This will give the healthcare professional the knowledge and tools necessary to identify this syndrome early. This activity will help promote better health outcomes for the geriatric population by education of the care providers and with the promotion of evidence-based practice.
This intermediate course is designed for psychologists who work in or are interested in learning more about geriatrics.
Continuing Education (CE) credits for psychologists are provided through the co-sponsorship of the American Psychological Association (APA) Office of Continuing Education in Psychology (CEP). The APA CEP Office maintains responsibility for the content of the programs.
NetCE designates this continuing education activity for 5 credit(s).
The purpose of this course is to educate psychologists regarding geriatric failure to thrive and to promote evidence-based clinical practice when caring for patients with this condition.
Upon completion of this course, you should be able to:
- Define the various conditions responsible for unintended weight loss in geriatric patients, including geriatric failure to thrive.
- Analyze various ethical and legal issues that can arise when treating geriatric failure to thrive patients and the role of advance directives in ameliorating some of these issues.
- Outline necessary components of the physical assessment and differential diagnosis of geriatric failure to thrive.
- Evaluate the role of polypharmacy in unintended weight loss in elderly patients.
- Describe the role of mental health screening in geriatric failure to thrive patients.
- Create a treatment plan for a geriatric failure to thrive patients, including possible pharmacotherapy approaches and areas for monitoring and follow-up.
- Identify geriatric failure to thrive patients for whom hospice referral should be considered.
Susan Waterbury, MSN, FNP-BC, ACHPN, entered the medical field in 1985 as a certified medical assistant and basic x-ray operator. She achieved her RN in 1990 and practiced in a variety of settings, including hospital, home health care, and hospice. Ms. Waterbury achieved her BSN in 1996 and her MSN as a Family Nurse Practitioner in 1999. She was board-certified as an FNP-BC in 2000 and has practiced in family practice, geriatrics, corporate leadership, hospice, and palliative care settings. She holds RN and NP licenses in Florida and Arizona.
In addition to her clinical roles, Ms. Waterbury continues to play an active role in educating and mentoring nurses and healthcare professionals. She has been a faculty member of the University of Phoenix since 2015, teaching in the nurse practitioner and MSN programs. She develops and presents educational programs for a variety of healthcare organizations and community groups.
Contributing faculty, Susan Waterbury, MSN, FNP-BC, ACHPN, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Margaret Donohue, PhD
The division planner has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#69204: Geriatric Failure to Thrive: A Multidimensional Problem
Undesired weight loss in the elderly causes a reduced quality of life and contributes to serious illness. Elderly residents of nursing facilities who lose 5% of their body weight in one month are 4.6 times more likely to die within a year[1]. Poor prognosis is also associated with low prealbumin and cholesterol levels. Malnutrition in the elderly can result in pressure sores, functional decline, longer rehabilitation, and multiple medical complications.
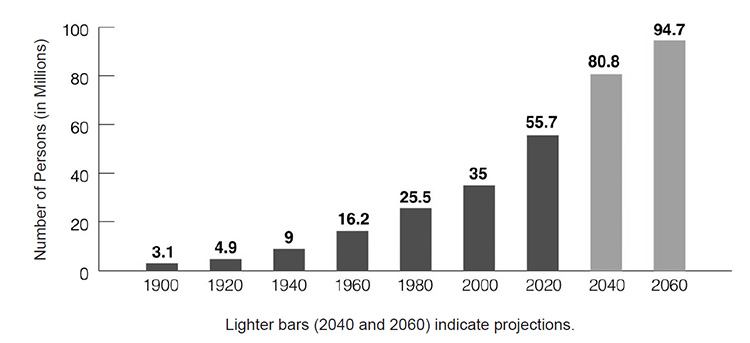
The "baby boomers" will continue to account for a substantial increase in the elderly population (Figure 1). By 2060, persons older than 65 years of age are projected to make up 24.4% of the population [2]. The number of the "oldest old," those 85 years of age and older, is expected to increase from 6.7 million in 2020 to 14.4 million in 2040 [3]. More elderly persons will be dependent on others for their survival, with increasing numbers living in skilled nursing and assisted living facilities. Healthcare providers should become prepared for the projected growth of the elderly population and be prepared to treat the various conditions unique to this group.
The term "failure to thrive" was originally used to identify abnormal growth and development patterns in children. The term was borrowed from pediatrics in the 1970s to describe a similar syndrome that affected geriatric patients. Failure to thrive is a common diagnosis in geriatrics. As of October 2014, the Centers for Medicare and Medicaid Services (CMS) no longer accepts adult failure to thrive as a principal diagnosis for hospice claims, but it has been noted that access to hospice is not impeded by this fact because the principal diagnosis may instead be, for example, one of or a combination of cachexia, malnutrition, dysphagia, or muscle weakness, with an additional diagnosis of adult failure to thrive [4,5].
Failure to thrive is defined by the Institute of Medicine as "weight loss of more than 5%, decreased appetite, poor nutrition, and physical inactivity, often associated with dehydration, depression, immune dysfunction, and low cholesterol" [6]. It is not a single disease or medical condition. Rather, it is a multidimensional problem that requires a multidisciplinary approach for its treatment. The four chief characteristics of geriatric failure to thrive are impaired physical function, malnutrition, depression, and cognitive impairment [7]. Failure to thrive is commonly used as a nonspecific diagnosis when a patient loses weight due to an unknown cause. After the diagnosis is made, it stimulates further assessment and interventions. Each of the domains of geriatric failure to thrive should be evaluated to determine areas in which the elder is having difficulty.
Geriatric practitioners often order extensive diagnostic work-ups for these patients, which do not always reveal a reversible cause. It is a challenge to differentiate disease states common for older patients versus "normal aging." Furthermore, large amounts of Medicare dollars are paid to hospitals at the very end of the patient's life [8]. This raises the ethical dilemma of providing "futile care" that is cost intensive and yields few benefits.
Despite costly, time-intensive medical evaluations, 25% to 35% of patients with geriatric failure to thrive have no obvious medical cause for this weight loss [1,9]. If weight loss is attributed to the normal aging process, this can prevent early interventions from being employed.
Sarcopenia can be defined as an age-related loss of skeletal muscle mass and strength that usually occurs after 60 years of age [10]. Decreased strength leads to decreased function, and this functional decline can result in multiple complications, including falls, fractures, cognitive impairment, depression, and loss of independence. Nursing home residents are at special risk, as inactivity and immobility lead to muscle wasting [11,12,13]. This wasting is accelerated when nutritional deficits are present, and studies report that 18% to 60% of residents of nursing facilities are undernourished [14,15].
Cachexia is a physical wasting with weight and muscle mass loss, usually secondary to chronic progressive diseases such as cancer, acquired immune deficiency syndrome (AIDS), and chronic obstructive pulmonary disease (COPD). An estimated 10% of nursing home residents in the United States have cachexia [16]. Cachexia is a hypermetabolic state in which loss of body mass cannot be reversed nutritionally. The mechanisms that cause cachexia are poorly understood, but inflammatory cytokines and metabolic imbalances probably play a role [17,18]. Cachectic patients often have a poor prognosis due to multiple medical comorbidities. Cachexia is seen in the late stages of almost every major chronic illness, affecting an estimated 16% to 42% of people with heart failure, 30% of those with COPD, and up to 60% of people with kidney disease [18].
Anorexia of aging, also known as age-related wasting, is a complex problem with physical, psychologic, and sociologic causes [19]:
Physical causes: Medical illness, comor- bidities, functional decline, sensory loss, reduced smell and taste, water and sodium imbalance, reduced thirst and ability to concentrate urine, medication side effects, and early satiety
Psychologic causes: Cognitive impairment, delirium, depression, and/or psychiatric illness
Sociologic causes: Poverty, lack of family support, isolation, dependency, substandard living conditions, and elder abuse
In addition, there is usually a component of sarcopenia and/or cachexia present. When undesired weight loss and/or malnutrition occur in the elderly patient, it becomes a complex problem requiring a multidisciplinary approach. Unless this syndrome is identified early and interventions begun, the prognosis can be quite poor. An age- or illness-related weight loss or physical decline can quickly progress to a terminal hospice diagnosis.
Weight loss is a serious issue in nursing facilities, and state and federal regulatory agencies monitor undesired weight loss as a quality indicator. It is also an area of focus for plaintiff attorneys, and advertisements may encourage loved ones to sue facilities/care providers for weight loss, accusing neglect. Furthermore, inadequate treatment and monitoring of the patient with dysphagia has become a malpractice litigation issue. Plaintiffs may accuse the nursing home or staff members of inadequate screening, evaluation, and/or treatment of the patient with dysphagia [20]. Plaintiff attorneys may assert that adequate treatment and supervision could have prevented aspiration and death.
Undesired weight loss can usually be attributed to medical illness, terminal condition, food refusal, cognitive impairment, psychologic illness, or hypermetabolic state; however, one in four older adults experiencing weight loss have no discernible medical cause [21]. Careful communication with the patient and healthcare proxy, with adequate documentation of options for treatment, provides a basis for defense. Nursing facilities can protect themselves by responding quickly and appropriately, using established protocols for dysphagia management.
Advance healthcare directives allow the patient and family to determine what medical care is desired. State regulations vary regarding how and when advance directives can be used. It is important for healthcare providers to be familiar with laws governing the use of advance directives in the state in which they practice [22]. While it is desirable for a patient to have an advance directive, it may never be a condition of admission or continuance of their stay in a nursing facility.
When caring for any patient with failure to thrive, it should first be determined if advance directives exist, and copies of any documents should be obtained. If no advance directives exist, it should be determined if the patient is capable of making his or her own healthcare decisions. This is called a determination of capacity and usually requires the signatures of two physicians. If the patient is deemed incapable of making medical decisions, the healthcare proxy will assume the role of medical decision maker. A healthcare proxy is a person that is chosen by the patient/family to make healthcare decisions for the patient. If there is not a surrogate designated, a close family member or personal friend may be appointed the proxy.
There are many types of medical care that a living will can address [22]. A do not resuscitate (DNR) order is a pre-hospital determination stating that the patient does not want cardiopulmonary resuscitation (CPR), ventilatory support, or other heroic lifesaving measures. It is important to note that this does not prevent other life-sustaining treatments (e.g., artificial nutrition, hydration) and will not compromise the level of care given [22].
The concept of living wills grew from the limitations of DNR orders. These legal documents predetermine the medical care that will be accepted and refused. It may also designate a healthcare proxy or organ donation. If lifesaving or life-prolonging treatment is warranted and the patient is unable to communicate his or her preferences, the living will is activated. The living will should be as detailed as possible, and a physician should review the contents with the patient, if possible, to ensure understanding. A nutrition/hydration directive may be created in order to ensure that a patient's/proxy's wishes regarding nutrition and hydration care are followed. This clarifies whether a feeding tube may be inserted or IV fluids administered. In some cases, patients may refuse a gastric feeding tube but allow IV hydration or blood transfusion [22].
If a patient/proxy and healthcare provider determine that further hospitalizations would not be beneficial, a do not hospitalize (DNH) order may be made. A DNH allows care to be provided in a nursing facility or home. These orders are often made when further hospitalizations would most likely cause further pain, suffering, or complications, and the patient would rather be cared for by familiar caregivers. If a patient's/proxy's wishes are contrary to a healthcare professional's recommendations, he or she may be required to sign a refusal of treatment. This document indicates that the patient or responsible party has received informed consent regarding treatments, procedures, specialty referrals, diagnostics, and recommendations and has declined the recommendation. In addition, a waiver of responsibility may be necessary. This form is designed to relieve responsibility of the nursing facility when a patient does not follow recommendations. It is most commonly used when the patient/proxy refuses fluid restrictions, dietary modification, or thickened liquids. Many facilities do not allow waivers, as they may not adequately protect from litigation.
At times, advance directives may be difficult to implement due to pressure from family or the facility. When a patient has a living will and has clearly communicated end-stage desires and wishes to family, problems following a directive should be minimal. In other cases, there may be no advance directive and family members must make these difficult, and often divisive, decisions without knowing the patient's last wishes. Family members who may or may not have a close relationship with the patient can revoke living wills, DNRs, and other directives; they may be in denial of the patient's declining condition or have a personal agenda. Social workers are instrumental in the process of determining advance directives and communicating with families.
Medically futile care consists of medical diagnostics, treatments, or procedures that most likely will not provide a meaningful benefit to the patient. This is a difficult issue, particularly when the physician recommends withdrawing or withholding treatments and the family wants everything possible done. Ethics committees are useful resources when there is conflict that cannot be resolved.
It can take several hospitalizations or trips to the emergency room before family members or patients will be ready to sign DNR or DNH directives. In addition to debilitating illness, patients may be physically restrained at the hospital, usually to prevent them from falling or pulling out IVs or tubes. Physical or chemical restraint causes a forced immobility, potentially leading to pressure sores and muscle wasting.
Long-term care facilities have regulations and practices regarding physical restraints and have protocols to be followed when a restraint is required; some pride themselves on being a restraint-free environment. These facilities can utilize creative means to keep patients from harming themselves, including bed and chair alarms, activity programs, and low beds with mats on either side to prevent injury should the patient get up unassisted and fall. Physical and occupational therapists can be instrumental in initiating programs to promote patient safety and prevent falls. The least restrictive method of physical restraint is the most desirable for patients and facilities.
Gastric feeding tubes are commonly seen in nursing facilities, and they can be used for years to provide medications, hydration, and nutrition. Feeding tubes are routinely used for progressive neurologic diseases (e.g., Parkinson disease), stroke, and radiation therapy of the head or neck. However, gastric feeding tubes are not recommended for patients with advanced dementia, and there is no evidence that placement of a feeding tube improves the quality of life or survival in these patients [23,24]. Complications that can occur with a feeding tube include aspiration, infection, and tube dysfunction. In some cases, gastric feeding tubes prolong pain and suffering at the end of life. The impact of these potential complications should be considered before a gastric feeding tube is prescribed. Evidence-based information about feeding tube placement should be given to patients and family members to assist them to make informed decisions.
Most nursing facilities have protocols to be followed when a resident has a 5% weight loss in one month or a 10% weight loss in six months. Physician notification, dietician consults, and speech therapy evaluations are usually the first interventions.
Dieticians perform nutritional assessments, recommend liquid supplements, discontinue restrictive diets, obtain calorie counts, determine food preferences, recommend protein supplements, and add nutritious snacks. Dieticians or dietary technicians should evaluate a patient's nutritional status regularly: upon admission to a nursing facility, quarterly, and in case of significant change in weight.
The Mini Nutritional Assessment (MNA) is a validated tool often used to evaluate the nutritional status of elderly persons [25,26,27]. The MNA is inexpensive, quick, and easy to administer. The short-form version consists of a six-item checklist that assesses the patient's food intake, mobility, weight loss, psychologic stresses and problems, and body mass index (BMI). Calf circumference can be substituted if BMI cannot be obtained. The MNA can quickly identify elderly at risk of malnutrition and guide nutritional intervention. A copy of the MNA may be accessed online at https://www.mna-elderly.com.
Assessment and interventions for causes of dysphagia are often necessary in patients with geriatric failure to thrive. A speech therapist will evaluate the patient's swallowing ability and can test for sensory deficits. Dysphagia assessments may include bedside assessment of swallow, the videofluoroscopic swallowing study (VFSS), and the fiberoptic endoscopic evaluation of swallowing (FEES) [28,29]. Both the VFSS and the FEES can detect laryngeal penetration, tracheal aspiration, and pharyngeal residue. The VFSS is more commonly known as the modified barium swallow study, which is usually performed at acute care or diagnostic facilities [28].
During the assessment period, the speech therapist will try different food and fluid consistencies. Thickening of liquids is one of the most common treatments for dysphagia, and thickened liquids are routinely tried during modified barium swallow studies, especially if a patient demonstrates difficulty with thin liquids. The degrees of thickness or viscosity are generally categorized as regular or unthickened (nothing added); nectar-like or nectar-thick; honey-like or honey-thick; or pudding-like or pudding-thick [30]. After assessment and testing, the speech therapist will determine the consistency of food and fluids most appropriate for the patient.
Patients often are at risk for aspiration secondary to dysphagia, and this complication is considered life-threatening. Therefore, patients with a diagnosis of dysphagia should be carefully monitored for signs of choking and/or pneumonia. Signs of dysphagia or aspiration include [31]:
Coughing or choking associated with eating
Excessive swallowing
Throat clearing
Gargling sound while eating
Wet voice
Sensation that something is stuck in throat
Food or liquid spilling from the mouth
Sneezing
Food pocketing in mouth
Recurrent pneumonia
Chest or lung congestion
Desaturation while eating
After a thorough assessment of a patient's swallowing and speaking ability is complete, a program to restore nutrition and intake by mouth will be established. The restorative dining program consists of intensive education, assistance, and supervision with meals to restore swallowing ability. The speech therapist may also work with patients with gastric feeding tubes in order to restore oral feedings.
The use of neuromuscular electrical stimulation (NMES) to provide assistance in swallowing rehabilitation has been extensively studied. This involves the application of electrodes to the neck that provide small electric currents to strengthen and retrain the muscles involved in swallowing. Patients who are unable to regain their swallowing function after a stroke or other debilitating illness may be good candidates for this type of therapy, especially when other techniques have failed. Most experts agree that NMES is a promising technique for swallowing rehabilitation; however, they also state that additional research is needed to provide evidence of its efficacy [32,33,34,35,36].
In cases of irreversible dysphagia, a gastric feeding tube may be the only option to maintain nutrition. Either the patient or the healthcare proxy may decline a feeding tube and elect to have oral feedings despite the risk of aspiration and choking. This is an instance in which obtaining a waiver of responsibility may be appropriate. Some facilities may be uncomfortable allowing a patient to eat a regular diet or drink thin liquids when tests have proven the patient to be at high risk for aspiration. It is important to note that a waiver may not provide adequate legal protection against litigation.
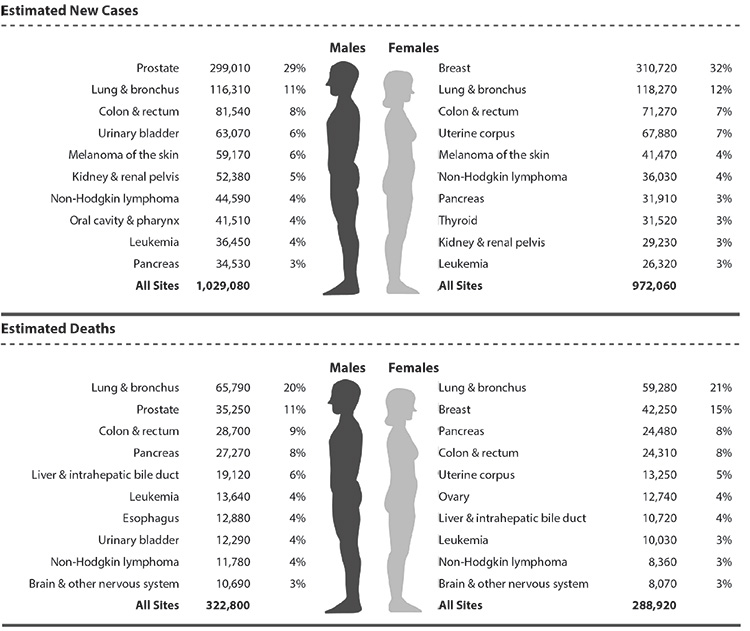
It is important to evaluate patients for metabolic or treatable causes of weight loss, including cancer. The incidence of cancer increases with age, and screening for cancer and evaluation of risk factors are essential parts of the assessment of geriatric failure to thrive, with special focus on screening for the most common types of cancer (Figure 2).
Each patient should be carefully evaluated on an individual basis, taking into consideration patient age, advance directive, and functional and mental status. Clear communication with the patient and/or healthcare proxy along with clarification of any and all advance directives is necessary. Patients or patient representatives should feel empowered to accept or decline diagnostic procedures or treatments.
Digital rectal exam (in men), fecal occult blood test, prostate-specific antigen test (PSA), breast exam or mammogram (in women), and a chest x-ray are vital aspects of a comprehensive cancer screening when cancer is suspected; routine screening of older individuals with limited life expectancy is generally not recommended. Diagnostic and laboratory tests may be completed, even when surgery or treatment is not advised, in order to guide the treatment of geriatric failure to thrive.
A thorough baseline evaluation is necessary for all patients with unexplained weight loss. History taking and a complete and accurate physical assessment lay the foundation for further treatment, monitoring, and follow-up. A patient's baseline physical function and health should be determined before assessing for abnormalities. Changes associated with normal aging may include loss of subcutaneous fat from face and periphery (re-deposited to the abdomen and hips), shorter stature, shrinkage of muscle mass, kyphosis, and senile ptosis or ectropion. Many geriatric patients have chronic medical conditions, and seemingly abnormal exam findings may actually reflect these long-term illnesses (Table 1) [7]. Common findings in the geriatric patient may include heart murmurs and cardiac arrhythmias, chronic skin lesions such as seborrheic keratoses, orthostatic hypotension, sensory deficit (e.g. visual, hearing), and arthritic deformities. Good history taking with input from family members and staff will help differentiate problems that require intervention from normal findings for that patient. In addition to standard physical assessment, special attention should be paid to cancer detection, as discussed, and gastrointestinal tract disorders.
COMMON MEDICAL CONDITIONS ASSOCIATED WITH GERIATRIC FAILURE TO THRIVE
| Medical Condition | Cause of Failure to Thrive |
|---|---|
| Cancer | Metastases, malnutrition, cancer cachexia |
| Chronic lung disease | Respiratory failure |
| Chronic renal insufficiency | Renal failure |
| Chronic steroid use | Steroid myopathy, diabetes, osteoporosis, vision loss |
| Cirrhosis, history of hepatitis | Hepatic failure |
| Depression, other psychiatric disorder | Major depression, psychosis, poor functional status, cognitive loss |
| Diabetes | Malabsorption, poor glucose homeostasis, end-organ damage |
| Hip, other large-bone fracture | Functional impairment |
| Inflammatory bowel disease | Malabsorption, malnutrition |
| Myocardial infarction, congestive heart failure | Cardiac failure |
| Previous gastrointestinal surgery | Malabsorption, malnutrition |
| Recurrent urinary infections or pneumonia | Chronic infection, functional impairment |
| Rheumatologic disease (e.g., temporal arteritis, rheumatoid arthritis, lupus erythematosus) | Chronic inflammation |
| Stroke | Dysphagia, depression, cognitive loss, functional impairment |
| Tuberculosis, other systemic infection | Chronic infection |
The initial physical assessment includes baseline measures of BMI, height, weight, triceps skinfold measurement, calf measurement, full vital signs, and oxygen saturation. To calculate the BMI it is necessary to have an accurate height and weight. BMI calculators and charts are readily available for easy calculation. If either height or weight is unavailable, calf circumference may be used. Patients with a BMI of less than 22 are considered at risk (Table 2).
Oral examination findings in patients with geriatric failure to thrive may include candidiasis, dental problems, oral lesions, xerostomia, and post-nasal drainage. Monitoring oxygen saturation while having the patient swallow fluids can detect risk of aspiration. Choking or coughing while drinking fluids may or may not indicate aspiration; coughing may actually be a defense mechanism preventing aspiration. If a patient's oxygen saturation drops while eating or drinking, further evaluation and referral to speech therapy is necessary.
Xerostomia, or dry mouth, is a common complaint in geriatric patients [9]. It can be a side effect of a medication or of radiation to the head or neck. Poor dentition is a contributing factor. Over-the-counter sprays, mouthwashes, hard candies, or ice chips can provide some relief. Medications with anticholinergic effects are not generally recommended for elderly patients due to potential adverse effects, such as dry mouth, dysgeusia, constipation, and changes in mental status [7]. If the use of an agent with anticholinergic effects is necessary, the lowest effective dose should be utilized.
Referral to a dentist for management of any dental problems or concerns is crucial. Dental problems lead to decreased oral intake and weight loss. Caries and broken teeth should be restored, and the fit of dental prosthesis should be verified.
Post-nasal drainage and vasomotor rhinitis can contribute to decreased nutritional intake. In these cases, treatment of allergic conditions can help improve oral intake.
Auscultation of the heart and lungs is also necessary in order to evaluate chronic diseases and detect new problems [7]. Normal age-related changes to physiology and parameters should be noted. The chest often increases in anteroposterior diameter with aging. Occasional ectopic beats are common and do not necessarily indicate underlying heart disease. Systolic blood pressure commonly increases with age; diastolic blood pressure usually stays constant. For patients with abnormal cardiovascular findings, additional diagnostics include chest x-ray, electrocardiogram, echocardiogram, and 24-hour Holter monitoring.
Disorders of the gastrointestinal tract can cause weight loss. The aging abdomen often has increased deposits of subcutaneous fat and thinner musculature. Peristalsis may be visible, in the absence of obesity. Osteoporotic kyphosis causes a protuberant appearance of the abdomen. Medications may cause gastrointestinal side effects, such as nausea, heartburn, and constipation.
Examination of the abdomen may reveal hepatomegaly, masses, constipation, distention, hernias, ascites, and tenderness. Bowel and bladder patterns and function should be assessed, using the patient's normal patterns as a baseline. Conditions such as atrophic gastritis, gastric or peptic ulcer, constipation, lactose intolerance, diverticulosis, colitis, and diabetic gastroparesis may be the cause of significant weight loss. Diagnostic approaches for abnormal exam findings may include abdominal or pelvic ultrasounds, fecal occult blood test, and kidneys, ureters, and bladder x-ray. Referral to a gastroenterologist can be crucial for patients' treatment and outcome.
Thyroid function should also be assessed, as both hypothyroidism and hyperthyroidism may result in impaired absorption of nutrients and weight fluctuations. Some patients with hypothyroidism may develop decreased peristalsis, leading to chronic constipation and impaired absorption of nutrients. With hyperthyroidism, patients may display increased appetite secondary to increased peristalsis, diarrhea, and weight loss. If there is accompanying vomiting with abdominal pain, this can lead to malnutrition and a negative nitrogen balance. Screening for thyroid dysfunction, and treating when present, may improve weight loss in some elderly patients.
The neurologic assessment should include sensory evaluation, cranial nerves, focal deficits, strength against resistance, and ambulation/gait evaluation. Documentation of baseline functional status is necessary, noting any assistive devices the patient uses for ambulation, including any splints or braces. If a patient is non-ambulatory and requires assistance for activities of daily living, this should be documented. Elderly patients may have slower responses, benign tremors, and a slower and more deliberate gait. Deep tendon reflexes are less brisk. Assessment of cognitive and mental status is an important aspect of the neurologic evaluation and will be thoroughly explored later in this course.
Baseline physical assessment lays the foundation for the ultimate plan of care. It also facilitates diagnosis of comorbid medical conditions. Documentation of serial measures of BMI, weight, and triceps skinfold thickness will help to track progress or decline. Depending on the patient's progress, the treatment plan can be revised or continued.
Impaired physical function is one of the four domains of geriatric failure to thrive, and evaluation of physical functioning is an integral part of the geriatric evaluation [7]. It is important to determine any changes in mobility and evaluate for signs of a functional decline. This decline may be rapid, in cases of hospitalization and severe illness, or gradual, with the patient experiencing decreased mobility and independence over a period of time. Occupational therapists can provide a complete assessment of a patient's mobility and ability to perform activities of daily living (ADLs) and instrumental activities of daily living (IADL). The Katz ADL scale assesses six activities: bathing, dressing, toileting, transferring, continence, and eating [38,39]. The Lawton IADL scale assesses a patient's ability to use the telephone, shop, take transportation, manage a budget, adhere to medication regimens, cook, and perform housekeeping and laundry chores [40]. Approximately 34% of adults 65 years of age or older reported having some type of disability (i.e., difficulty in hearing, vision, cognition, ambulation, self-care, or independent living), and 49% of adults 75 years of age and older reported having difficulty in physical functioning. This ranged from 5% reporting it was very difficult (or impossible) to sit for two hours, to 33% reporting it was very difficult (or impossible) to stand for two hours [3]. For patients with failure to thrive, assessment of eating and ability to feed oneself is particularly important. Recommendations regarding contracture management and prevention, need for splints, positioning in wheelchairs or specialty chairs, and the need for assistive devices to help with eating may be made. A rehabilitation plan to assist the patient to regain independence in daily activities can be helpful.
The patient's current strength, mobility, balance, and safety awareness should all be evaluated. Based on this assessment, assistive devices, such as walkers, canes, wheelchairs, and splints, may be prescribed. For a patient who has declined in function, a physical therapist may create a plan of rehabilitation to return the patient to his or her prior level of function. Rehabilitation may include therapeutic exercises, resistance exercise training, pain management modalities, and gait and ambulation training [41,42].
Polypharmacy has been described as the use of more than 5 medications, and excessive polypharmacy is defined as the use of more than 10 medications [43]. Known hazards of polypharmacy include lack of adherence, overtreatment, adverse drug reactions (including unexplained weight loss), and incorrect dose and administration regimen. In addition to these factors, physiologic changes of aging cause differences in the absorption, distribution, metabolism, and excretion of medications [44].
Elderly patients commonly take medications for many chronic conditions, including diabetes, hypertension, arthritis, and cardiovascular disease, making them at increased risk for the adverse effects of polypharmacy. Geriatric illnesses are often more complex and require referral to medical specialists. Each specialist may order diagnostic testing and medications without a complete knowledge of the patient's comorbidities and other treatments [44]. The primary care provider should perform a risk and benefit analysis to evaluate the need for multiple medications or tests. The primary care provider may then accept or refuse the specialist's recommendation, but should justify any refusal.
Assessment of each patient's medication regimen is crucial and should identify medications that may be causing problems. In each evaluation of a geriatric patient, medication side effects should be an initial consideration, including evaluation of over-the-counter medications, vitamins, and herbal remedies and supplements [44].
As an elderly patient begins to decline or lose weight, some previously prescribed medications may no longer be necessary. For example, lipid-lowering medications may not be necessary in patients who have lost weight or declined. Diuretic doses should be adjusted as necessary, as overdosing can cause azotemia. Insulin dosages should be titrated to reflect weight loss or poor food intake. Collaboration with multiple specialists may be beneficial to determine the necessity of certain medications. For example, a cardiologist may be consulted before stopping or changing doses of beta-blockers or angiotensin-converting enzyme inhibitors.
The risks of certain medications may outweigh the potential benefits in many cases. For instance, a patient 85 years of age with a longstanding history of treatment for atrial fibrillation may no longer be a candidate for anticoagulants. If the patient is at risk for falls, gastrointestinal bleeding, or hemorrhagic stroke, the risks of anticoagulation outweigh the potential benefit and the medication should be stopped. Another important consideration is the patient's adherence to prescribed medications and necessary monitoring. Patients who cannot or will not undergo regular blood test monitoring should not be on a warfarin regimen.
Patients with dysphagia may require changes to their medication routes to accommodate the condition. In some cases, medications may be crushed; if this method is chosen, controlled-release medications should be changed to a formulation that allows this administration. A nurse or family member can provide information regarding whether the patient requires crushed or liquid medications and whether the patient refuses any medications. Consultation with a pharmacist may help to identify any medications that can be reduced or stopped. The consultant pharmacist usually reviews the records monthly and makes recommendations according to state regulations.
The Beers list is a collection of medications potentially inappropriate for the elderly patient for a variety of reasons [45,46]. This list identifies medications not recommended for patients 65 years of age or older and identifies potentially harmful prescribing practices. Certain medications may be detrimental to elderly patients due to extended half-lives, interactions, or side effects. For example, benzodiazepines are associated with risk of cognitive impairment, delirium, falls, fractures, and motor vehicle accidents in the elderly, and before prescribing these medications, it should be clear that the potential benefits outweigh the risks [46]. Common medications on the Beers list include alprazolam, digoxin, cimetidine, diphenhydramine, lorazepam, and naproxen [45,46].
Many patients take over-the-counter allergy, cold, or cough medications as sleeping aids, some of which contain acetaminophen/diphenhydramine. Elderly patients should be advised to avoid such use, as diphenhydramine is associated with falls in this population; another sleep aid can be prescribed [46,47]. Medications that patients have taken for years may require re-evaluation if changes in health status occur.
There are a variety of laboratory and diagnostic tests available to evaluate elderly patients whose health is failing, but it is important to refrain from ordering unnecessary tests that will not benefit the patient. Initial laboratory tests to evaluate unintentional weight loss include complete blood count, chemistry profile, thyroid, carcinoembryonic antigen in patients with cancer, urinalysis with culture (if indicated), and fecal occult blood test. Further laboratory and diagnostic tests should be guided by the results of these tests and by history, physical exam, and patient wishes. More extensive testing can include a chest x-ray, PSA, tumor markers, nutritional markers (e.g. vitamin D, vitamin B complex), anemia work-up, drug levels (e.g., phenytoin, digoxin), prealbumin, and albumin.
Cognitive impairment is another domain of geriatric failure to thrive. To fully evaluate geriatric failure to thrive, it is necessary to also assess psychologic and sociologic functioning. The Mini-Mental State Examination (MMSE) or Folstein test may be used as an objective assessment of cognition, either to establish a baseline measurement of mental status or to track progress or decline [48]. It is a 30-item exam that takes approximately 10 to 15 minutes to complete. A correct answer for each item is awarded 1 point, and a score of 25 or more is considered normal. Lesser scores can indicate severe (≤9 points), moderate (10–20 points), or mild (21–24 points) cognitive impairment. It is helpful to document serial scores in the medical record.
Another screening test for dementia is the clock drawing test [49,50]. There are variations in how this test is administered, but it generally consists of asking the patient to draw a picture of an analog clock, complete with numbers, set to a certain time. In some cases, the circle will be predrawn for the patient. Just as there are variations in the test, scoring methods also vary. One system is based on a score of five points as follows: 1 point for the clock circle, 1 point for all the numbers being in the correct order, 1 point for the numbers being in the proper place on the clock face, 1 point for the two hands of the clock, and 1 point for the correct time. Scores of 4 or 5 are considered normal. Studies are mixed on whether the complicated scoring, which is used to determine the severity or stage of dementia, is more effective than a simple pass/fail, but the consensus among experts is that the test is useful for determining whether further testing is required, regardless of the scoring method used [51,52].
This clock becomes part of the medical record and can clearly identify moderate-to-advanced cognitive impairment, although it is not sensitive for mild cognitive impairment or early Alzheimer disease. The clock drawing test is cost-effective and can be performed by trained assistants. Serial clock drawings incorporated into the medical record can document the onset and progression of dementia for geriatric clients [53].
Depression is a major cause of weight loss in the elderly, and geriatric depression is a significant health risk, affecting function and quality of life. Assessment for depression is crucial in the patient who has had an unintentional weight loss. Delay in diagnosis may accelerate the decline associated with failure to thrive and may increase morbidity and mortality [7]. Geriatric patients have often experienced multiple losses, including the death of a spouse, peers, or children; loss of independence; loss of health or mobility; and loss of physical or financial independence. Each of these events can induce depression.
The stigma of psychiatric illness may prevent elderly patients from seeking help for depression. They are more likely to complain of physical problems than to mention conventional depressive symptoms (e.g., mood changes) [7]. Therefore, screening should be incorporated into each clinical contact with a geriatric patient. Depression in the elderly may present with confusion, forgetfulness, apathy, slowing of thinking and movement, lack of interest in personal hygiene, and unexplained physical symptoms, including weight loss; however, these signs are often misdiagnosed as dementia in the elderly, making accurate assessment essential [7]. Disruption in sleep, changes in appetite, and psychomotor changes may prompt a patient to seek medical care. When a patient has multiple vague physical symptoms, depression should be included in the differential diagnosis. Suicidal ideation or attempt should be considered a medical emergency.
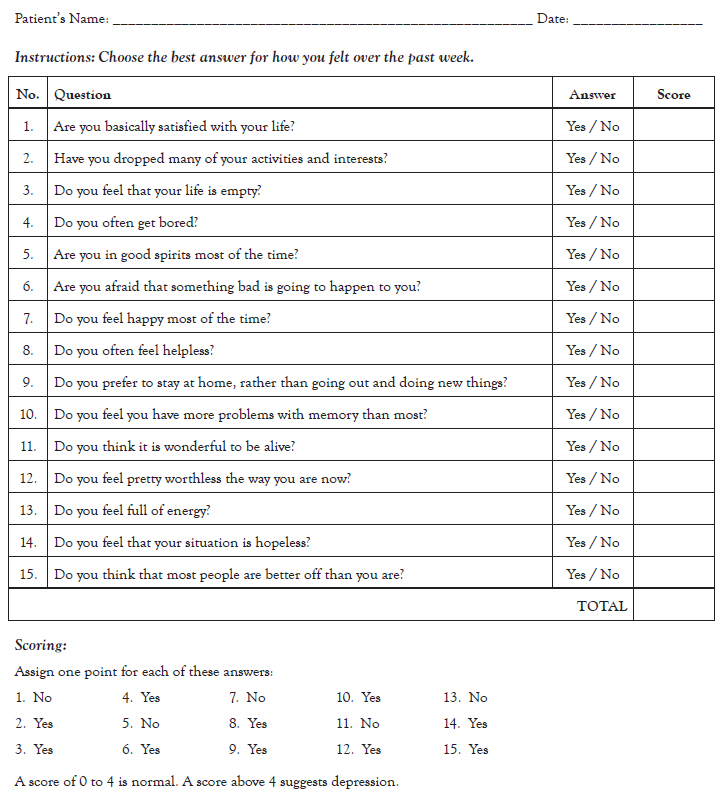
The Geriatric Depression Scale (GDS) is a self-report measure of depression that may be utilized to screen for depression in elderly patients (Figure 3) [7,54,55]. The shortened version (GDS-S) consists of 15 questions (taken from the long form) that assess mood and hopelessness. The GDS-S can be completed in five to seven minutes, which makes it ideal for patients who are easily fatigued or limited in their ability to concentrate for longer periods of time [55]. A score of 5 or greater on this test is considered positive. If a test is positive, referral to a psychiatrist specializing in geriatric patients should be made, as these patients do respond to depression treatment (e.g., psychotherapy, pharmacotherapy).
Older patients who present with dehydration, malnutrition, and/or failure to thrive may be exhibiting signs of neglect or abuse. In a systematic review that represented 28 different countries, the overall prevalence rate of elder abuse was assessed at 15.7%; 11.6% had experienced psychologic abuse [57]. It is estimated that approximately 1 in 10 Americans older than 60 years of age has been the victim of abuse, including physical abuse, psychologic or verbal abuse, sexual abuse, financial exploitation, and neglect [58,59,60]. Denying food has been explicitly identified as a form of neglect.
Persons being assessed for geriatric failure to thrive should be evaluated for abuse. Certain situations may make some elders more vulnerable to elder abuse [61]. Any elder, for example, who is incapable of taking care of his/her own daily needs and is dependent on another person is automatically in an at-risk situation. The Elder Abuse Suspicion Index (EASI) is a five-item tool that provides practitioners with a very quick sense of whether there is potential presence of elder abuse [62]. It is validated to screen for abuse in patients who are cognitively intact [63]. The EASI has been recommended by the U.S. Preventive Services Task Force and was originally developed for use by physicians, but it can be used by practitioners in diverse disciplines [64]. The following items comprise the index [62]:
Have you relied on people for any of the following: bathing, dressing, shopping, banking, or meals?
Has anyone prevented you from food, clothes, medication, glasses, hearing aids, or medical care, or from being with people you wanted to be with?
Have you been upset because someone talked to you in a way that made you feel shamed or threatened?
Has anyone tried to force you to sign papers or use your money against your will?
Has anyone made you afraid, touched you in ways that you did not want, or hurt you physically?
When developing a treatment plan, it is important to take a holistic and interdisciplinary approach in order to address all of the domains of geriatric failure to thrive [7]. Input from medical specialists, nursing staff, social workers, and physical, speech, and occupational therapists should be considered. Treatment efforts addressing only the physical effects of geriatric failure to thrive will most likely not achieve the desired results. For patients with both acute and chronic illnesses, acute infections and conditions should be resolved before a longer term plan is implemented.
During periods of acute illness, an elderly patient can experience a decline in function, and resolution of the acute condition may return the patient to his or her baseline. Common acute illnesses that cause physical and cognitive function deficits in older adults include urinary tract infection, pneumonia, dehydration, and exacerbation of congestive heart failure or COPD. Extended periods of bed rest also prove detrimental and can cause severe debility. Delirium can develop, requiring the use of physical or chemical restraints. Acute medical conditions also increase nutritional requirements at a time when nutritional intake is often reduced secondary to poor eating. After the acute issue is resolved, medical treatment may be provided for any other conditions present. Optimization of treatment of chronic illnesses is crucial in the care of patients with failure to thrive.
Family meetings may be difficult but are often productive interactions. These conferences provide an opportunity to present the results of the specialty consults and the tests and assessments that have been performed and for the patient and family to ask questions or request additional information. If further medical care and treatments would be futile or serve to prolong the dying process, this should be conveyed to the patient and family. Advance directives should be reviewed and updated. Any concerns expressed by the patient or family should be fully addressed. The healthcare provider, family members, and patient should leave the meeting with an agreement regarding the plan of care and treatment desired. When patients and family members have a good understanding of the options available, including potential benefits and risks, they are in a position to provide informed consent, and this can help to prevent misunderstandings later.
Correction of vitamin and nutritional deficits is necessary to reverse malnutrition. As such, collaboration with a dietician and a speech therapist is essential when caring for patients with failure to thrive. The speech therapist can determine the consistency of food best suited for the patient's needs and can recommend modifications to the established diet. The patient may require thickened liquids, puréed diet, mechanical soft diet, or other variation. Some patients will benefit from a restorative dining program, as supervision, encouragement, and socialization may increase food intake.
Discontinuation of restricted diets is an appropriate step for the patient with malnourishment. Therapeutic and restrictive diets do not promote adequate energy intake and should be thoroughly reviewed for each patient [65]. For example, the American Dietetic Association recommends a liberalized diet approach for nursing home residents [66]. A dietician should assess patients' food preferences and determine if oral nutritional supplements would be appropriate and accepted by the patient. The most common approach is to provide liquid nutritional supplements, shakes, and puddings between meals, with the goal of increasing calorie consumption. Geriatric patients may eat most of their calories at breakfast, which should be accommodated. It is important to provide high-calorie, fortified foods when the patient's appetite is greatest [7].
The first line of treatment for most patients living in nursing facilities is administration of oral liquid nutritional supplements. These are added to the plan of care and generally administered by nursing staff and dietary assistants. Compliance with the treatment plan can be an issue, and it is essential to evaluate whether the supplements are offered and taken as prescribed.
Fortified foods are prepared with extra protein and calories to provide a more calorie-dense food. The addition of one-third cup of instant, nonfat dry milk adds 80 calories, 8 g protein, and 12 g carbohydrates. The addition of butter, milk, and cream boosts calorie intake as well, and oral protein supplements are available to help reverse protein malnutrition. Making the supplements appealing to the patient is an ongoing challenge.
Families can play a large role in reversing malnutrition in a nursing facility. When the family is present for a meal or brings in the patient's favorite food, intake is improved [7]. Patients may complain that they do not like the food that is served, and family members are better equipped to cater to any ethnic preferences. Family members can often coax their loved one to eat their meal and take liquid nutritional supplements. Dedicated staff members and caregivers can promote positive outcomes by making sure supplements are offered and taken.
A number of common vitamin and mineral deficiencies may occur in patients with failure to thrive. Deficiencies may occur from not consuming enough fresh, nutrient-rich foods and/or from malabsorption disorders of the gastrointestinal tract. Common nutrient deficiencies include vitamin B12, vitamin D, iron, and zinc. In most cases, deficiencies will resolve with the administration of vitamins and supplements.
The consequences of vitamin D deficiency include muscle weakness, body sway, osteomalacia, and a tendency for falls and fractures [67]. Many elderly persons are not exposed to enough sunlight each day for adequate vitamin D synthesis. Supplementation with 800 IU of vitamin D daily is recommended and has been shown to reduce falls [68,69].
Vitamin B12 deficiency occurs due to inadequate dietary intake or impaired absorption. It may be associated with neurologic symptoms such as tingling of extremities, fatigue, irritability, depression, weakened concentration, and impaired memory [70]. It is fairly common in the elderly population due to decreased or absent intrinsic factor secondary to atrophic gastritis, achlorhydria, or previous gastric surgery. Deficiency may also be caused by medication side effects, such as those associated with the prolonged use of proton pump inhibitors. Vitamin B12 deficiency is traditionally treated by injectable cobalamin but is also effectively addressed with an oral supplement 1–2 grams daily.
Eldertonic is a vitamin B complex elixir with zinc, manganese, and magnesium in an alcohol base. The usual dose is 15 cc given three times daily, just before meals [70]. It is similar to a before meal alcoholic drink with a sherry base. Although some patients may find it distasteful and refuse to take it, no significant side effects have been noted [71]. It is associated with a mild anecdotal appetite improvement, which may be the result of correcting zinc and vitamin deficiencies.
Zinc deficiency is common in the institutionalized and homebound elderly patient. Zinc is needed for protein synthesis and is important in wound healing and skin repair and renewal. Zinc deficiency is caused by inadequate intake, gastrointestinal malabsorption, or increased zinc losses from the body (e.g., with diarrhea) and is associated with increased inflammation in older patients [72]. A diet lacking in zinc can lead to frequent infections, delayed wound healing, reduced appetite, decreased taste and smell, poor skin condition, and white flecks on the nails. A replacement dose of 50 mg elemental zinc per day is recommended.
Iron deficiency leading to anemia is a common finding in the elderly patient, affecting an estimated 3 million elderly Americans [73]. The most common causes include iron deficiency (with or without blood loss), chronic disease/inflammation, and chronic kidney disease [73,74]. Serum ferritin levels less than 45 mcg/L are suspicious for iron deficiency in the elderly [75]. Iron replacement therapy should be undertaken cautiously, as high iron stores can also be detrimental.
It is important to identify the cause of anemia and to treat accordingly. This often includes a gastroenterology evaluation [73]. Ferrous sulfate 200 mg three times a day is usually sufficient to replenish iron stores. It is important to consider ordering stool softeners at the same time, as constipation and fecal impaction are side effects. Supplementation should continue for three months past correction of the deficiency.
In addition to multiple medical comorbidities and psychiatric disorders associated with aging (e.g., dementia), the geriatric patient may have longstanding psychiatric illness, such as bipolar disorder or psychosis, requiring multiple medications [76]. This makes treating the geriatric psychiatric patient quite complex.
There are multiple long-term complications associated with typical and atypical antipsychotic medications, including pharmacokinetic and pharmacodynamic changes, limitations, and cardiovascular and other adverse effects (e.g., gastrointestinal, liver) [76]. A patient may develop a Parkinsonian syndrome secondary to long-term antipsychotic use, resulting in dysphagia, tremors, difficulty performing activities of daily living, and difficulty feeding, all of which can result in unintentional weight loss [76]. Prior to changing longstanding medication regimens, a geriatric psychiatrist should be consulted in order to help prevent exacerbation of the underlying psychiatric illness.
Psychiatric symptoms associated with dementia, such as anxiety or agitation, may cause an increased energy demand. Psychiatric symptoms such as pacing, hyperactivity, repetitive behaviors, insomnia, and mania all can lead to weight loss. These symptoms should be effectively managed. Referral to a psychiatrist or psychologist is recommended in cases of continued weight loss, treatment failures, and additional behavioral problems.
Potential underlying causes of unintentional weight loss should be fully assessed and treated prior to initiating pharmacotherapy for geriatric failure to thrive. Each patient should be evaluated on an individual basis prior to prescribing an appetite stimulant. The medications commonly used and discussed in the following section are not approved by the U.S. Food and Drug Administration (FDA) for appetite stimulation in patients with failure to thrive.
Mirtazapine is an atypical antidepressant with noradrenergic and specific serotonergic effects. It is indicated for major depressive disorder in the elderly; the starting geriatric dose is 7.5 mg at bedtime [47]. This can be increased to a maximum of 45 mg, if necessary. Mirtazapine's antihistamine-like effects are more pronounced at the 15 mg daily dosage. Mirtazapine has been studied for treatment of depression, anxiety, and anorexia nervosa with depression, with weight gain as a secondary endpoint. The weight gain usually occurs early in therapy. It has not been shown to be effective for weight gain in nondepressed individuals. Its sedating effects can be useful for patients with sleep disturbances or anxiety.
Dronabinol is a schedule III drug that contains delta-9-tetrahydrocannabinol (THC), the major active component of cannabis. It is FDA-approved to treat AIDS-related anorexia and refractory nausea and vomiting secondary to chemotherapy [47]. Dronabinol may also improve disturbed behavior in patients with Alzheimer disease [83]. Dronabinol is available in doses of 2.5 mg, 5 mg, and 10 mg in a gel cap that cannot be crushed and as an oral solution with a calibrated oral dosing syringe [47]. When used for geriatric failure to thrive, it is usually given one hour before meals (lunch and dinner). It has also been used as a single dose at bedtime due to central nervous system (CNS) side effects.
More research is needed regarding the use of dronabinol in the elderly population. Precautions should be used if this drug is prescribed to patients with liver disorders or seizure disorders [47]. There may be significant CNS side effects, including somnolence, emotional lability, and euphoria.
Megestrol acetate is a synthetic progestin and antineoplastic agent product, originally used for patients with cancer. Its use for weight loss in geriatric patients without cancer or AIDS is considered off label [47]. In small studies, megestrol has been effective at increasing appetite in certain geriatric patients at higher doses, although the actual impact on weight gain appears slight and side effects are common [77,78,79,80]. It has the potential to increase hypercoagulability, leading to thromboembolism. In addition, megestrol has glucocorticoid-like activity, which can potentially cause adrenal insufficiency and worsening of diabetes. New-onset diabetes and exacerbation of pre-existing diabetes have been reported with long-term use [47]. A case report associated megestrol acetate to two cases of osteoporosis; higher dosages of megestrol are associated with decreased bone density and may be associated with bone loss and fractures [82].
While megestrol has had some positive results for weight gain in the past, the potential drawbacks limit its use in practice. Patients with a history of thromboembolism should not receive megestrol. The Beers list includes megestrol acetate as a potentially harmful drug in the elderly, and its use should generally be avoided [81].
Anabolic steroids have been used in elderly patients with unintended weight loss with varying results. However, the side effects may prohibit their use in the geriatric population. Adverse reactions may include hyperglycemia, aggression, agitation, psychosis, and osteoporosis [84]. Anabolic steroids are possibly best well known as the substance that athletes use to increase muscle volume and strength. The Anabolic Steroids Control Act classifies steroids as a controlled substance [85,86]. It is a criminal offense for providers to prescribe an anabolic steroid unless it is used to treat a disease or medical condition.
The anabolic steroid nandrolone decanoate was the subject of a study of hip fracture recovery in elderly women [87]. In this study, a small dose was administered to determine if it could preserve lean body mass. The authors suggest that nandrolone decanoate with vitamin D and calcium supplementation improved body composition, bone mineral density, and clinical function. However, a systematic review found insufficient evidence to support the use of anabolic steroids for rehabilitation after hip fracture in the elderly and recommended that future research focus on a combined intervention of anabolic steroids and nutritional supplements [88].
Administration of testosterone, growth hormone, and essential amino acids are other approaches to geriatric sarcopenia and cachexia that have had variable results [89,90]. Growth hormone was found to increase lean body mass and decrease fat mass. The side effects may prohibit its use, however, except for in controlled trials [89]. Growth hormone was found to cause insulin resistance, diabetes, and carpal tunnel syndrome. More clinical research is necessary before the use of anabolic steroids, amino acids, or growth hormones can be recommended for geriatric weight loss.
Close monitoring of the geriatric patient with failure to thrive is essential, with special attention to each applicable domain. In addition, referral to a specialist to better address each domain's unique challenges may be necessary.
Patients being treated for geriatric failure to thrive will undergo regular physical and occupational therapy; the progress reports for this therapy should be reviewed with the patient and family, at which point one can discuss any medical concerns that may be interfering with rehabilitation, including dizziness, medication side effects, uncontrolled pain, unresolved infections, and balance problems. Recommendations for adaptive or assistive devices based on these reports may be made. Referral to neurology, rheumatology, or orthopedics may be considered if physical function is drastically impaired [7].
Patients should be weighed and have a BMI calculated weekly; this can decrease to monthly as the patient stabilizes. A speech therapist will continue assessing for dysphagia. It is important to monitor intake, particularly of liquid oral supplements and vitamin, mineral, and protein replacement. This requires ongoing dietician assessment and monitoring of nutritional status and consideration of a gastric feeding tube, when appropriate. Some patients will require referral to gastroenterology for treatment of underlying medical conditions leading to poor intake (e.g., gastroesophageal reflux contributing to dysphagia, esophageal stricture requiring dilation). Patients should also be assessed for oral pathology, ill-fitting dentures, speech or swallowing difficulties, medication use that might cause anorexia or dysgeusia, and financial or social problems [7].
Depression is the most common psychiatric condition in older persons [7]. Geriatric patients with failure to thrive should continue to be evaluated for signs and symptoms of depression and suicidal ideation. If prescribed, the efficacy of antidepressant therapy should be monitored, including adverse drug reactions and necessary adjustments in the medication regimen. Referral to a social worker, psychiatrist, and/or psychologist is strongly advised.
Evaluation of psychosocial function should include an assessment of the patient's cognitive status, mood, and social setting [7]. Any behavior problems should be reviewed with the patient, family, and staff. Results of cognitive assessments, such as the MMSE and the clock drawing test, should be evaluated on a regular basis. The role of medical conditions or medication side effects should be considered. If dementia treatment has been attempted, efficacy of the prescribed regimen will be assessed. If necessary, the patient may be referred to neurology, psychiatry, or social work.
Despite adequate evaluation and treatment, certain patients with failure to thrive will not respond to interventions. These patients will continue to lose weight and decline. If the BMI is less than 22 and significant physical impairment is causing disability, the patient qualifies for hospice care [91]. When the patient has declined parenteral feeding or has not responded to nutritional support despite adequate caloric intake, a referral to hospice should be considered. As noted, geriatric failure to thrive is no longer an acceptable diagnosis for hospice according to CMS [4]. Instead, the underlying condition most contributory to the patient's terminal prognosis should be noted (e.g., malnutrition).
The first step in initiating hospice is to obtain terminal evaluations by two physicians along with an evaluation of competency. After the patient has been certified as terminal, the next step is to have a meeting with the patient and healthcare proxy. Options for hospice care should be thoroughly discussed. When hospice services are recommended as an option, the patient and proxy may be shocked by the seriousness of the patient's condition. If the patient and healthcare proxy desire a conservative and comfort approach to care, then a referral to hospice is initiated. For a patient in a nursing facility, the hospice services will be rendered in the facility; others may use a home hospice service. The patient and family members should be supported through the dying process.
Patient E is a woman, 82 years of age, recently hospitalized for pneumonia. Her medical history is positive for hypertension, diabetes, coronary artery disease, and heart failure. She is admitted to the rehabilitation center with functional decline, unsteady gait, weight loss, and difficulty swallowing; the rehabilitation will be short term.
During the initial medical evaluation, the patient appears frail, alert, and cooperative. She is able to answer questions appropriately. Patient E has been living alone in a senior independent living apartment for the last seven years. She has a daughter who lives nearby who is very involved in her care. The daughter states that Patient E has been slowly losing weight over the last six months. The patient states she has never been a big eater but admits her appetite is not what it used to be. The daughter has noticed the patient coughing and clearing her throat frequently while eating. Since the pneumonia, Patient E has had poor activity tolerance and requires frequent rest periods.
Patient E has both a healthcare proxy and a DNR on record. Her chief complaints are fatigue, poor appetite, leg weakness, and nonproductive cough. Her weight is 107 pounds and height is 5 feet 4 inches, with a BMI of 18.4, which is slightly underweight. She appears frail, though alert and cooperative. She is in no apparent pain or distress sitting up in a wheelchair. Upon initial physical examination, her blood pressure is 104/60 mm Hg, apical pulse 86 beats per minute, regular rate and rhythm with systolic ejection murmur (grade 2/6). Her respirations are 22 breaths per minute, with an oxygen saturation of 92% (on room air). Respirations are even and unlabored at rest, and crackles are noted in the right base. Patient E's abdomen is soft and nontender with active bowel sounds. Trace ankle edema are present bilaterally, and muscle atrophy and kyphosis are noted. The patient displays no focal deficit, and cranial nerves are normal.
Several assessment tests are administered, and the scores of each are noted:
MMSE: 24 (mild cognitive impairment)
Clock-drawing test: 4 (normal)
GDS: 6 (suspicious for depression)
MNA: 7 (malnourished)
In addition, several laboratory/diagnostic tests are ordered. The results are as follows:
Hemoglobin: 10.4 g/dL
Hematocrit: 31%
Platelet: 132 platelets/L
Comprehensive metabolic panel
Glucose: 124 mg/dL
Blood urea nitrogen (BUN): 35 mg/dL
Creatinine: 1.4 mg/dL
CO2: 30 mmol/L
Albumin: 2.9 g/dL
Estimated glomerular filtration rate: 36 mL/min
Thyroid stimulating hormone: 2.05 mIU/L, urinalysis-negative
Vitamin B12: 318 pg/mL
Vitamin D hydroxyl: 18 ng/mL
Zinc: 55 mmol/L
A chest x-ray shows right lower lobe infiltrate and cardiomegaly. Finally, the modified barium swallow test indicates aspiration on thin liquids.
The patient is referred to several specialists for evaluation of potential causes of weight loss and continued failure to thrive. After two weeks, the results of the consultations are available. The physical therapist indicates muscle disuse atrophy of both lower extremities, poor endurance, and dizziness upon standing; however, the patient is able to walk 10 feet with assistance and walker. Occupational therapy indicates that Patient E requires assistance with bathing, dressing, and eating. The speech therapist recommends that the patient be placed on a mechanical soft diet with thickened liquids. Finally, the dietician finds that the patient's appetite is fair to poor, as she eats only 25% to 50% of meals. Patient E is resistant to modified diet and supplements; therefore, the dietician recommends liberalization of diet to regular with fortified foods.
Based on abnormal exam and laboratory findings, Patient E is diagnosed with anemia, chronic kidney disease, pneumonia (still on treatment), and functional decline, particularly a decline in mobility and nutritional status. She also displays evidence of vitamin and mineral deficiencies, with low vitamin D, protein, and zinc levels. Her vitamin B12 level is also borderline low. The blood pressure is below normal and may be responsible for the patient's dizziness. She is malnourished, with a low BMI, and symptoms of depression are present.
Patient E is taking several daily medications, all of which are assessed for necessity and potential interactions. Her current regimen includes:
Coated aspirin: 81 mg/day
Metoprolol: 50 mg twice per day
Furosemide: 40 mg/day
Potassium chloride: 20 mEq/day
Metformin: 500 mg twice per day
Levofloxacin: 500 mg daily for five more days
Ipratropium/albuterol: Unit dose per nebulizer every four hours as needed
Evaluation of the medication regimen indicates that the patient's dizziness or weakness upon standing may be due to medication side effects. Furthermore, metoprolol is associated with fatigue in the elderly. Patient E's diuretic dose may need to be decreased due to her elevated BUN level. Metformin is not recommended in patients older than 80 years of age or with creatinine levels 1.4 mg/dL or greater. As a result of this information, the physician orders that the patient's prescriptions for furosemide and potassium chloride be halved to 20 mg/day and 10 mEq/day, respectively. The metoprolol dose is tapered gradually and held if the systolic blood pressure is less than 110 mm Hg.
In addition to adjustments to the patient's existing medication regimen, it was determined that Patient E could benefit from the addition of a medication to address the signs of osteoporosis and a vitamin and mineral supplement. The physician prescribes calcium carbonate with vitamin D 500 mg/200 mg twice daily as well as a daily multivitamin. To treat the patient's depressive symptoms, 7.5 mg of mirtazapine is prescribed to be taken at bedtime.
Supplementary diagnostic tests are ordered, including anemia profile, ferritin level, stool for presence of occult blood, and folate level. Patient E is instructed to return in one week for a follow-up appointment, at which time another blood test and metabolic profile will be completed.
When Patient E returns for her one-week follow-up appointment, her lungs are clearer and she appears to be more alert. Although she continues to complain of fatigue and poor endurance, she is experiencing less dizziness. She has completed the antibiotic therapy for her pneumonia and has been participating in skilled therapy, increasing her assisted walk distance to 25 to 50 feet.
Her vital signs are normal, indicating a blood pressure of 112/64 mm Hg, pulse 88 beats per minute, and respirations 18 breaths per minute.
The patient intake has also improved, as she is reportedly consuming 50% of most meals and accepts one to two cans of liquid supplement daily. She has gained three pounds, to a weight of 110 pounds and a BMI of 18.9, which is considered healthy. Her completed blood test and metabolic panel indicate the following values:
Occult blood test: Negative
Hemoglobin: 10.5 g/dL
Hematocrit: 31.8%
Ferritin: 245 mcg/L
Folate: 18 mcg/L
Serum iron: 54 mcg/dL
Blood glucose: less than 150 mg/dL
BUN: 29 mg/dL
Creatinine: 1.4 mg/dL
The physician instructs Patient E and her family to continue on the current plan of care. She is scheduled for a follow-up chest x-ray to confirm the absence of pneumonia, and she is instructed to return to the physician in one month to evaluate the continued effectiveness of the treatment plan.
At her one-month follow-up appointment, Patient E has continued to have daily rehabilitation and her weight has stabilized. She is lucky to have the support of her daughter, who encourages her through the process. Her medical conditions have stabilized, which required adjustments to her medication regimen. The patient has progressed well and is discharged home to her apartment. Future considerations for health maintenance include a dual-energy x-ray absorptiometry scan to evaluate osteoporosis treatment, a mammogram, and a colonoscopy.
Patient S is a man, 70 years of age, who was admitted to the hospital with altered mental status, exhibiting symptoms of delirium, agitation, and confusion. He was found to have a urinary tract infection and obstructive uropathy leading to acute renal failure. His condition is stabilized, and he is admitted to the rehabilitation facility. The physician completed the initial assessment shortly after his admission to the rehabilitation center. Findings from medical record review indicate a positive history for hypertension and hyperlipidemia. The patient has no advance directives on record, and medical care prior to hospitalization was sporadic. Patient S has lived in a studio apartment for 12 years and does not have any close family members. His support system consists of friends and neighbors. He smokes one-half pack of cigarettes per day and usually drinks two to three beers each day. Prior to hospitalization, he was found by a neighbor; he was delirious, with poor hygiene and incontinent of urine and stool.
Patient S is examined while sitting bedside. His chief complaint is pain in his right knee with walking, though no injury is noted. He also complains of stomach discomfort, gas, and constipation. The patient appears to be suspicious of the physician and makes it clear that he is not staying long. He requests discharge as soon as possible. The patient has gaps in his memory as to what happened prior to hospitalization. He indicates that he eats regularly and does not know why he has lost weight. When dinner is provided, he requests that a beer be provided as well. The Foley catheter is maintained pending further urologic evaluations and treatments.
The initial physical examination indicates that Patient S's height is 5 feet 8 inches, weight 140 pounds, and BMI 21.3; however, the patient's usual weight is 158 pounds. His blood pressure is 134/82 mm Hg, apical pulse 82 beats per minute, and respirations 20 breaths per minute. He has poor dentition, but the mouth is otherwise healthy. The lungs are essentially clear, with slightly diminished breath sounds in the bases. His abdomen is soft and nontender, with active bowel sounds, and the Foley catheter is draining clear, yellow urine. The right knee is mildly edematous and warm to touch. Slight resting tremor is noted of the right hand, but there is no focal deficit. A complete blood test, metabolic panel, and knee x-ray are ordered, as are physical therapy, occupational therapy, speech therapy, and dietician evaluations.
Assessments of function, nutrition, and depression are administered and indicate:
MMSE: 18 (moderate cognitive impairment)
GDS: 10 (moderate depression)
MNA: 9 (at risk of malnutrition)
The laboratory tests return the following results:
Hemoglobin: 12.8 g/dL
Hematocrit: 38%
BUN: 22 mg/dL
Creatinine: 1.0 mg/dL
Thyroid-stimulating hormone: 3.86 mIU/L, urinalysis-negative
Vitamin B12: 585 pg/mL
Vitamin D hydroxyl: 22 ng/mL
Zinc: 88 mmol/L
The knee x-ray displays evidence of mild degenerative joint disease. The physical therapist's report indicates that Patient S has weakness of the lower extremities with unsteady gait. The patient's right knee pain is causing limited range of motion and mobility. In spite of these limitations, the occupational therapist finds that the patient requires minimal assistance with activities of daily living and hygiene. The speech therapist finds that the patient has poor short-term memory and retention, but no difficulty swallowing. Finally, the dietician notes that Patient S eats about 50% of most meals, refuses liquid supplements, and refuses to go to the dining room because "it is depressing looking at all those sick people."
Because the patient has no advance directives on file, he is referred to a social worker for assistance in planning his care. The patient declines DNR and names a neighbor as his healthcare proxy. The social worker notes that it is questionable if the patient will be able to live alone after rehabilitation is completed due to the lack of regular caregiver and the presence of cognitive deficits.
Finally, the patient's medication regimen is assessed. Patient S is currently prescribed the following medications:
Coated aspirin: 325 mg/day
Amlodipine: 5 mg/day
Simvastatin: 20 mg/day at bedtime
Trimethoprim/sulfamethoxazole: One double-strength tablet twice daily for three more days
Dutasteride: 0.5 mg/day
Based on the laboratory and examination findings, Patient S is diagnosed with moderate cognitive impairment/dementia and has symptoms of depression. The degenerative nature of the patient's joint impairment indicates osteoarthritis of the right knee. Alcohol dependence is suspected, though the patient refuses assistance with smoking or alcohol cessation. The patient is dyspeptic and constipated. He has developed obstructive uropathy due to undercare of urology.
Assessment of Patient S's medication regimen shows several undertreated conditions, including no medication prescribed for depression, dementia, or vitamin/mineral deficiencies (resulting from weight loss). It is also noted that the aspirin may be causing adverse gastric effects and that side effects related to antibiotic use may be contributing to the decrease in appetite and food intake.
Patient S is started on a regular diet with fortified foods and high-calorie snacks, with the addition of a daily multivitamin. However, the physician advises the patient to decrease alcohol intake to one beer daily (preferably a low-alcohol type). To address the constipation, daily prune juice and milk of magnesia (30 cc as needed) are recommended. Omeprazole 20 mg taken 30 minutes before a meal is prescribed for the patient's continued dyspepsia. Finally, acetaminophen (1 g three times per day) is added to Patient S's regimen to treat his arthritic knee pain. If the patient experiences side effects of the oral acetaminophen, a topical nonsteroidal anti-inflammatory drug may be substituted. The patient is also instructed on physical therapy modalities to manage his pain, including heat, use of a brace, and massage. He continues physical, speech, and occupational therapy for therapeutic exercises, strengthening, endurance, gait training, and cognitive/memory training.
In addition, Patient S is referred to a urologist, psychiatrist, and social worker for continued care planning. It is important that the patient consider options for long-term care, assisted living, and financial assistance, as returning to living alone in his apartment will likely not be a possibility. He is instructed to return in one week for a follow-up appointment.
At Patient S's one-week follow-up appointment, the patient states that his right knee is still sore but slightly improved and his stomach discomfort is relieved, with improvement in constipation. The patient appears mildly confused but is able to answer questions appropriately. He does have multiple complaints regarding food, staff, and policies of the skilled nursing facility where he has been living. He feels he is making good progress with his therapy and is eager for discharge. The patient also expresses a hope that his catheter will be removed soon. He continues to decline assistance with smoking cessation.
At this visit, Patient S's blood pressure is 130/80 mm Hg, pulse 74 beats per minute, respirations 16 breaths per minute, weight 141 pounds, and BMI 21.4. The report from the urologist indicates the ongoing need for the Foley catheter due to obstructive uropathy. The patient has been scheduled for cystoscopy and ultrasound of the bladder and kidneys. Occupational and speech therapies are to be discontinued this week, but continued physical therapy is necessary for gait training, therapeutic exercises, mobility, and balance with a cane.
The psychiatrist reports an MMSE result of 19 and has diagnosed Patient S with depression and vascular dementia. She recommends computed tomography (CT) scan of the brain with contrast. The patient has been prescribed citalopram 20 mg/day, and the future consideration of cholinesterase inhibitors for dementia treatment is noted. His physician instructs Patient S to continue with the current treatment plan, including following up with psychiatry and urology as necessary.
Although Patient S's weight stabilizes, he never regains the weight loss of 18 pounds. The CT of his brain shows microvascular ischemic changes consistent with vascular dementia, possibly a result of the combined risk factors of alcohol and tobacco use, hyperlipidemia, and hypertension. The potential for self-neglect and inadequate medical care is high, and Patient S is not able to return to his apartment to live independently. The lack of family or caregiver is a contributing factor.
After many discussions and care meetings and the intervention of a social worker, the patient moves into an assisted living facility that is subsidized by the government. He continues to be treated by his urologist and psychiatrist. His appetite improves, but he never returns to his pre-illness status.
Geriatric failure to thrive is a challenging condition for healthcare providers. It is vital to remember that undesired weight loss in the elderly is generally not a normal part of aging. However, in up to 35% of patients there is no obvious cause for the weight loss.
The four domains of geriatric failure to thrive are impaired physical function, malnutrition, depression, and cognitive impairment. The patient should be evaluated and treated for each area. The MMSE, MNA, and GDS are useful tools for evaluating cognition, nutrition, and depression in these patients. Serial measurements may be used to track progress or decline. A complete physical assessment is also necessary, noting any changes that are the result of normal aging.
Polypharmacy is a significant problem in this population due to side effects, interactions, noncompliance, and use errors. Evaluating patients for adverse drug reactions is crucial. The Beers list of potentially inappropriate medications in the elderly can be used as a guide for prescribing medications. If it is necessary to prescribe a potentially inappropriate medication, the lowest effective dose should be used.
Advance directives are important in determining the care plan. Conferences with the patient and family are crucial for clarifying the goals of care. Taking a multidisciplinary approach is helpful. Referrals to a dietician and/or physical, occupational, and speech therapy are made as indicated. Medical specialists are consulted, as needed, depending on patient needs.
There should be adequate follow-up and monitoring of any interventions taken, with revision of the plan of care when necessary. For patients who do not respond to treatments, geriatric failure to thrive may progress to a terminal condition with poor prognosis. A hospice referral may be appropriate for end-stage care.
1. Ryan C, Bryant E, Eleazer P, Rhodes A, Guest K. Unintentional weight loss in long-term care: predictor of mortality in the elderly. South Med J. 1995;88(7):721-724.
2. U.S. Census Bureau. 2023 National Population Projections. Available at https://www2.census.gov/programs-surveys/popproj/tables/2023/2023-summary-tables/np2023-t2.xlsx. Last accessed March 7, 2024.
3. U.S. Administration for Community Living. 2021 Profile of Older Americans. Available at https://acl.gov/sites/default/files/Profile of OA/2021 Profile of OA/2021ProfileOlderAmericans_508.pdf. Last accessed March 7, 2024.
4. Centers for Medicare and Medicaid Services. Hospice Manual Update for Diagnosis Reporting and Filing Hospice Notice of Election (NOE) and Termination or Revocation of Election. Available at https://www.hhs.gov/guidance/sites/defaults/files/hhs-guidance-documents/MM8877.pdf. Last accessed March 7, 2024.
5. Brandon ST. Can Someone with Debility or Adult Failure to Thrive Still be Admitted to Hospice? Available at https://www.geripal.org/2014/09/principle-hospice-diagnosis-versus-hospice-eligibility.html. Last accessed March 7, 2024.
6. Ali N. Failure to Thrive in Elderly Adults. Available at https://emedicine.medscape.com/article/2096163-overview. Last accessed March 7, 2024.
8. The Henry J. Kaiser Family Foundation. End-of-Life Hospital Spending for Medicare Beneficiaries with Chronic Health Conditions Varies Widely, Study Finds. Available at https://khn.org/morning-breakout/dr00051385. Last accessed March 8, 2024.
9. Smith KL, Greenwood C, Payette H, Alibhai SMH. An approach to the nonpharmacologic and pharmacologic management of unintentional weight loss among older adults. Geriatr Aging. 2007;10(2):91-98.
10. Morley JE, Baumgartner RN, Roubenoff R, Mayer J, Nair KS. Sarcopenia. J Lab Clin Med. 2001;137(4):231-243.
11. Vandewoude MF, Alish CJ, Sauer AC, Hegazi RA. Malnutrition-sarcopenia syndrome: is this the future of nutrition screening and assessment for older adults? J Aging Res. 2012;651570.
12. Agarwal E, Miller M, Yaxley A, Isenring E. Malnutrition in the elderly: a narrative review. Maturitas. 2013;76(4):296-302.
13. Landi F, Liperoti R, Fusco D, et al. Prevalence and risk factors of sarcopenia among nursing home older residents. J Gerontol A Biol Sci Med Sci. 2012;67(1):48-55.
14. Verbrugghe M, Beeckman D, Van Hecke A, et al. Malnutrition and associated factors in nursing home residents: a cross-sectional, multi-centre study. Clin Nutr. 2013;32(3):438-443.
15. Stange I, Poeschl K, Stehle P, Sieber CC, Volkert D, Screening for malnutrition in nursing home residents: a comparison of different risk markers and their association to functional impairment. J Nutr Health Aging. 2013;17(4):357-363.
16. Kimyagarov S, Klid R, Fleissig Y, Kopel B, Arad M, Adunsky A. Skeletal muscle mass abnormalities are associated with survival rates of institutionalized elderly nursing home residents. J Nutr Health Aging. 2012;16(5):432-436.
17. Morley JE, Thomas DR, Wilson MMG. Cachexia: pathophysiology and clinical relevance. Am J Clin Nutr. 2006;83(4):735-743.
19. Martone AM, Onder G, Vetrano DL, et al. Anorexia of aging: a modifiable risk factor for frailty. Nutrients. 2013;5(10):4126-4133.
20. Tanner DC. Lessons from nursing home dysphagia malpractice litigation. J Gerontol Nurs. 2010;36(3):41-46.
21. Alibhai SM, Greenwood C, Payette H. An approach to the management of unintentional weight loss in elderly people. CMAJ. 2005;172:773-80.
22. National Cancer Institute. Advance Directives. Available at https://www.cancer.gov/about-cancer/managing-care/advance-directives. Last accessed March 8, 2024.
23. Sampson EL, Candy B, Jones L. Enteral tube feeding for older people with advanced dementia. Cochrane Database Syst Rev. 2009;(2):CD007209.
24. Cai S, Gozalo PL, Mitchell SL, et al. Do patients with advanced cognitive impairment admitted to hospitals with higher rates of feeding tube insertion have improved survival? J Pain Symptom Manage. 2013;45(3):524-533.
25. Vellas B, Villars H, Abellan G, et al. Overview of the MNA: its history and challenges. J Nutr Health Aging. 2006;10(6):456-465.
26. Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B. Screening for undernutrition in geriatric practice: developing the short-form Mini Nutritional Assessment (MNA-SF). J Gerontol. 2001;56(6):M366-M372.
27. Guigoz Y. The Mini Nutritional Assessment (MNA) review of the literature: what does it tell us? J Nutr Health Aging. 2006;10(6):466-487.
28. American Speech-Language-Hearing Association. Videofluoroscopic Swallowing Study (VFSS). Available at https://www.asha.org/public/speech/swallowing/Videofluoroscopic-Swallowing-Study. Last accessed March 8, 2024.
29. American Speech-Language-Hearing Association. Endoscopic Evaluation of Swallowing. Available at https://www.asha.org/public/speech/swallowing/endoscopy. Last accessed March 8, 2024.
30. Steele CM, Peladeau-Pigeon M, Barbon CAE, et al. Reference values for healthy swallowing across the range from thin to extremely thick liquids. J Speech Lang Hear Res. 2019;62(5):1338-1363.
31. American Speech-Language-Hearing Association. Adult Dysphagia. Available at https://www.asha.org/practice-portal/clinical-topics/adult-dysphagia. Last accessed March 8, 2024.
32. Humbert IA, Michou E, MacRae PR, Crujido L. Electrical stimulation and swallowing: how much do we know? Semin Speech Lang. 2012;33(3):203-216.
33. Clark H, Lazarus C, Arvedson J, Schooling T, Frymark T. Evidence-based systematic review: effects of neuromuscular electrical stimulation on swallowing and neural activation. Am J Speech Lang Pathol. 2009;18(4):361-375.
34. Carnaby-Mann GD, Crary MA. Examining the evidence on neuromuscular electrical stimulation for swallowing: a meta-analysis. Arch Otolaryngol Head Neck Surg. 2007;133(6):564-571.
35. Tan C, Liu Y, Li W, Liu J, Chen L. Transcutaneous neuromuscular electrical stimulation can improve swallowing function in patients with dysphagia caused by non-stroke diseases: a meta-analysis. J Oral Rehabil. 2013;40(6):472-480.
36. Shune S, Moon JB. Neuromuscular electrical stimulation in dysphagia management: clinician use and perceived barriers. Contemp Issues Commun Sci Disord. 2012;39:55-68.
38. Katz S, Ford AB, Moskowitz RW, Jackson BA, Jaffe MW. Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA. 1963;185:914-919.
39. Gerrard P. The hierarchy of the activities of daily living in the Katz index in residents of skilled nursing facilities. J Geriatr Phys Ther. 2013;36(2):87-91.
40. Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9:179-186.
41. McCormick R, Vasilaki A. Age-related changes in skeletal muscle: changes to life-style as a therapy. Biogerontology. 2018;19(6):519-536.
42. Marzuca-Nassr GN, Martín-Calísto YS. Guerra-Vega P. Skeletal muscle aging atrophy: assessment and exercise-based treatment. Adv Exp Med Biol. 2020;1260:123-158.
43. Haider SI, Johnell K, Weitoft GR, Thorslund M, Fastbom J. The influence of educational level on polypharmacy and inappropriate drug use: a register-based study of more than 600,000 older people. J Am Geriatr Soc. 2009;57(1):62-69.
44. Halli-Tierney AD, Scarbrough C, Carroll D. Polypharmacy: evaluating risks and deprescribing. Am Fam Physician. 2019;100(1):32-38.
45. Fick DM, Cooper JW, Wade WE, Waller JL, Maclean JR, Beers MH. Updating the Beers Criteria for potentially inappropriate medication use in older adults: results of a U.S. consensus panel of experts. Arch Intern Med. 2003;163(22):2716-2724.
46. American Geriatrics Society 2019 Updated AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2019;67(4):674-694.
47. Lexicomp Online. Available at https://online.lexi.com. Last accessed March 7, 2024.
48. Folstein MF, Folstein SE, McHugh PR. "Mini-mental state:" a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189-198.
49. Wolf-Klein GP, Silverstone FA, Levy AP, Brod MS. Screening for Alzheimer's disease by clock drawing. J Am Geriatr Soc. 1989;37(8):730-734.
50. Aprahamian I, Martinelli JE, Neri AL, Yassuda MS. The accuracy of the Clock Drawing Test compared to that of standard screening tests for Alzheimer's disease: results from a study of Brazilian elderly with heterogeneous educational backgrounds. Int Psychogeriatr. 2010;22(1):64-71.
51. Dementia Care Central. Alzheimer's/Dementia Clock-Drawing Test: Everything Caregivers Need to Know. Available at https://www.dementiacarecentral.com/alzheimers-clock-test. Last accessed March 8, 2024.
52. Spenciere B, Alves H, Charchat-Fichman H. Scoring systems for the Clock Drawing Test: a historical review. Dement Neuropsychol. 2017;11(1):6-14.
53. Shah J. Only time will tell: clock drawing as an early indicator of neurological dysfunction. P&S Medical Review. 2002;7(2):30-34.
54. Sheikh JI, Yesavage JA. Geriatric Depression Scale (GDS): recent evidence and development of a shorter version. In: Brink TL (ed). Clinical Gerontology: A Guide to Assessment and Intervention. New York, NY: The Haworth Press; 1986: 165-173.
55. American Psychological Association. Geriatric Depression Scale. Available at https://www.apa.org/pi/about/publications/caregivers/practice-settings/assessment/tools/geriatric-depression. Last accessed March 7, 2024.
56. Yesavage JA, Brink TL, Rose TL, et al. Development and validation of a geriatric depression screening scale: a preliminary report.J Psychiatr Res. 1983;17(1):37-49.
57. Yon Y, Mikton CR, Gassoumis ZD, Wilber KH. Elder abuse prevalence in community settings: a systematic review and meta-analysis. Lancet Glob Health. 2017;5(2):e147-e156.
58. National Center on Elder Abuse. Statistics and Data. Available at https://ncea.acl.gov/researchstatisticsanddata - gsc.tab=0. Last accessed March 7, 2024.
59. National Council on Aging. Elder Abuse Facts. Available at https://www.ncoa.org/article/get-the-facts-on-elder-abuse. Last accessed March 7, 2024.
61. Sengstock MC, Barrett SA. Abuse and neglect of the elderly in family settings. In: Campbell J, Humphreys J (eds). Nursing Care of Survivors of Family Violence. St. Louis, MO: Mosby; 1993:173-208.
62. Yaffe MJ, Wolfson C, Lithwick M, Weiss D. Development and validation of a tool to improve physician identification of elder abuse: the Elder Abuse Suspicion Index (EASI). J Elder Abuse Negl. 2008;20(3):276-300.
63. Hoover RM, Polson M. Detecting elder abuse and neglect: assessment and intervention. Am Fam Physician. 2014;89(6):453-460.
64. Wang XM, Brisbin S, Loo T, Straus S. Elder abuse: an approach to identification, assessment and intervention. CMAJ. 2015;187(8):575-581.
65. Asai JL. Nutrition and the geriatric rehabilitation patient: challenges and solutions. Top Geriatr Rehabil. 2004;20(1):34-45.
66. Dorner B, Friedrich EK, Posthauer ME. Practice paper of the American Dietetic Association: individualized nutrition approaches for older adults in health care communities. J Am Diet Assoc. 2010;110(10):1554-1563.
68. Venning G. Recent developments in vitamin D deficiency and muscle weakness among elderly people. BMJ. 2005;330(7490): 524-526.
69. Gatto S, Gimigliano F, Gimigliano R, Iolascon G. Prevention of falls and role of calcium and vitamin D. Aging Clin Exp Res. 2011;23(2 Suppl):20-21.
70. Drugs.com Eldertonic. Available at https://www.drugs.com/drp/eldertonic.html. Last accessed March 8, 2024.
71. Niedert KC, Carlson MP (eds). Nutrition Care of the Older Adult: A Handbook for Dietetics Professionals Working Throughout the Continuum of Care. 3ed ed. Chicago, IL: American Dietetic Association; 2016.
72. Wong CP, Magnusson KR, Ho E. Increased inflammatory response in aged mice is associated with age-related zinc deficiency and zinc transporter dysregulation. J Nutr Biochem. 2013;24(1):353-359.
73. Guralnik JM, Eisenstaedt RS, Ferrucci L, Klein HG, Woodman RC. Prevalence of anemia in persons 65 years and older in the United States: evidence for a high rate of unexplained anemia. Blood. 2004;104(8):2263-2268.
74. Artz AS, Fergusson D, Drinka PJ, et al. Mechanisms of unexplained anemia in the nursing home. J Am Geriatr Soc. 2004;52(3):423-427.
75. Mukhopadhyay D, Mohanaruban K. Iron deficiency anaemia in older people: investigation, management and treatment. Age Ageing. 2002;31:87-91.
76. Varma S, Sareen H, Trivedi JK. The geriatric population and psychiatric medication. Mens Sana Monogr. 2010;8(1):30-51.
77. Yeh SS, Lovitt S, Schuster MW. Usage of megestrol acetate in the treatment of anorexia-cachexia syndrome in the elderly. J Nutr Health Aging. 2009;13(5):448-454.
78. Yeh SS, Wu SY, Lee TP, et al. Improvement in quality-of-life measures and stimulation of weight gain after treatment with megestrol acetate oral suspension in geriatric cachexia: results of a double-blind, placebo-controlled study. J Am Geriatr Soc. 2000;48(5):485-492.
79. Sarkisian CA, Lachs MS. "Failure to thrive" in older adults. Ann Intern Med. 1996;124(12):1072-1078.
80. Reuben DB, Hirsch SH, Zhou K, Greendale GA. The effects of megestrol acetate suspension for elderly patients with reduced appetite after hospitalization: a phase II randomized clinical trial. J Am Geriatr Soc. 2005;53(6):970-975.
81. American Geriatrics Society Beers Criteria Update Expert Panel. American Geriatrics Society 2023 updated AGS Beers Criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2023;71(7):2052-2081.
82. Wermers RA, Hurley DL, Kearns AE. Osteoporosis associated with megestrol acetate. Mayo Clin Proc. 2004;79(12):1557-1561.
83. Volicer L, Stelly M, McLaughlin J, Volicer BJ. Effects of dronabinol on anorexia and disturbed behavior in patients with Alzheimer's disease. Int J Geriatr Psychiatry. 1997;12(9):913-919.
84. Narayanan R, Mohler ML, Bohl CE, Miller DD, Dalton JT. Selective androgen receptor modulators in preclinical and clinical development. Nucl Recept Signal. 2008;6:e010.
85. US Department of Justice, Drug Enforcement Administration. Fed Regist. 2005;70(241):74653-74658.
86. U.S. Department of Justice Drug Enforcement Administration Diversion Control Division. Anabolic Steroids. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/anabolic.pdf - search=Anabolic Steroids. Last accessed March 8, 2024.
87. Hedström M., Sjöberg K, Brosjö E, Åström K, Sjöberg H, Dalén N. Positive effects of anabolic steroids, vitamin D and calcium on muscle mass, bone mineral density and clinical function after a hip fracture: a randomised study of 63 women. J Bone Joint Surg Br. 2002;84(4):497-503.
88. Farooqi V, van den Berg MEL, Cameron ID, Crotty M. Anabolic steroids for rehabilitation after hip fracture in older people. Cochrane Database Syst Rev. 2014;(10):CD008887.
89. Blackman MR, Sorkin JD, Munzer T, et al. Growth hormone and sex steroid administration in healthy aged women and men. JAMA. 2002;288(18):2282-2292.
90. Henderson GC, Irving BA, Nair KS. Potential application of essential amino acid supplementation to treat sarcopenia in elderly people. J Clin Endocrinol Metab. 2009;94(5):1524-1526.
91. National Association for Home Care and Hospice. Hospice Regulatory Resources. Available at https://nahc.org/advocacy/hospice-regulatory-resources/. Last accessed March 8, 2024.
1. Gaddey HL, Holder KK. Unintentional weight loss in older adults. Am Fam Physician. 2021;104(1):34-40. Available at https://www.aafp.org/pubs/afp/issues/2021/0700/p34.html. Last accessed March 22, 2024.
2. American Geriatric Society. Choosing Wisely and the American Geriatrics Society. Available at https://www.americangeriatrics.org/sites/default/files/inline-files/AGS%20Choosing%20Wisely%20Poster.pdf. Last accessed March 22, 2024.
Mention of commercial products does not indicate endorsement.