Identifying the potential causes, as well as the appropriate assessments and any treatment required, is critical to intervening or consulting in a timely and meaningful way. This course provides a discussion of the differential diagnosis of a few of the many hemorrhagic conditions that may present during pregnancy, including the incidence and potential causes of early pregnancy loss and second and third trimester bleeding. Furthermore, nonobstetric causes of genital bleeding in pregnancy should be part of any differential diagnosis. Knowledge of appropriate history, physical, laboratory, and diagnostic data required to reach an accurate diagnosis and management plan is vital in providing optimal care to obstetric patients. The patient and her family's needs for education and support should also be addressed.
- INTRODUCTION
- SCOPE OF THE PROBLEM
- AN OVERVIEW OF SPONTANEOUS ABORTION
- THREATENED ABORTION
- COMPLETE ABORTION
- INCOMPLETE ABORTION
- MISSED ABORTION
- SEPTIC ABORTION
- ECTOPIC PREGNANCY
- GESTATIONAL TROPHOBLASTIC DISEASE
- PLACENTA PREVIA
- ABRUPTIO PLACENTA
- EVALUATION OF OTHER CAUSES OF BLEEDING IN PREGNANCY
- COMMUNICATION WITH NON-ENGLISH-PROFICIENT PATIENTS
- CASE STUDIES
- CONCLUSION
- GLOSSARY
- APPENDIX
- Works Cited
- Evidence-Based Practice Recommendations Citations
This course is designed for all nurses, physicians, and physician assistants, especially those working in clinics, private practice, obstetric/gynecologic practice, or emergency room settings.
Bleeding during pregnancy is a frightening and potentially life-threatening event occurring in one out of every five pregnancies. The purpose of this course is to assist nurses, nurse practitioners, physicians, and physician assistants working in a variety of settings to understand, triage, and manage bleeding in pregnancy in order to facilitate more efficient diagnoses and treatment, resulting in better patient outcomes.
Upon completion of this course, you should be able to:
- Discuss the epidemiology of hemorrhagic conditions in pregnancy.
- Identify potential causes of bleeding in pregnancy and pregnancy loss.
- Compare the presentation and management of the different types of spontaneous abortion, including patient education and support needs.
- Describe the risk factors and signs and symptoms associated with ectopic pregnancy.
- Discuss the management and treatment of ectopic pregnancy, including the role of ultrasound.
- Describe gestational trophoblastic disease (GTD) and hydatidiform molar pregnancy.
- Review the differential diagnosis of and complications correlated with complete, partial, and marginal placenta previa.
- Define abruptio placenta and identify the associated risk factors.
- Review the appropriate management of abruptio placenta.
- Describe the evaluation of additional causes of bleeding in pregnancy.
- Outline the importance of an interpreter in caring for non-English-proficient patients.
Denise Wheeler, MS, ARNP, is a certified nurse-midwife in Des Moines, Iowa. She earned an Associate degree in Nursing in 1975, a Bachelor’s degree in Nursing from St. Louis University in 1982 and a Master’s degree in Nursing Sciences from the University of Illinois at Chicago in 1983. She has worked in a variety of settings, from out-of-hospital birth centers to tertiary care centers, and has gained significant experience in caring for women experiencing bleeding in pregnancy. She has authored papers and book chapters for publication and has been a guest lecturer at conferences for undergraduate and graduate nursing education programs.
Contributing faculty, Denise Wheeler, MS, ARNP, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
John V. Jurica, MD, MPH
Jane C. Norman, RN, MSN, CNE, PhD
The division planners have disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#93253: Bleeding During Pregnancy
Healthcare providers will often find themselves triaging the care of a patient experiencing bleeding in pregnancy. While bleeding in pregnancy is alarming to patients and their families, the assessment and initial management can also be intimidating to non-obstetric healthcare providers. For purposes of this course, bleeding during pregnancy means bleeding from the uterus, vagina, or non-genital pelvic sources, manifest as sudden awareness of blood coming from the vaginal area. Identifying potential causes, as well as appropriate assessments and any treatment required, is critical to intervening or consulting in a timely and meaningful way. This course will cover the differential diagnosis of common hemorrhagic conditions that may present during pregnancy, including the incidence and causes of early pregnancy loss and second and third trimester bleeding. Furthermore, non-obstetric causes of genital bleeding in pregnancy should be part of any differential diagnosis. Knowledge of appropriate history, physical, laboratory, and diagnostic data required to reach an accurate diagnosis and management plan is vital in providing optimal care to obstetric patients. The patient and the family's needs for education and support should also be addressed.
Approximately 20% of women experience at least one episode of vaginal or uterine bleeding during pregnancy [1]. In fact, the awareness of blood issuing from the vaginal area is one of the most common reasons for unscheduled calls and visits to the office and emergency room. This condition is potentially life-threatening and frightening for patients and family members. Studies indicate that 15% to 20% of recognized pregnancies abort spontaneously; the actual number may approach 50% of all pregnancies, but many are misinterpreted as a "late period" [1]. Because many patients do not recognize their own early signs of pregnancy, it is difficult to know how the incidence rate of preimplantation pregnancy losses compares with postimplantation pregnancy loss [1,2]. Patients with first trimester vaginal bleeding may be at higher risk for preterm delivery, low birth weight at term, and neonatal death [3]. Bleeding during pregnancy requires a thorough, compassionate evaluation to avoid possible complications, and address the meaning and importance of pregnancy to the patient and/or their family.
Bleeding during pregnancy has a variety of causes, the most important of which involve the gravid uterus (Table 1). However, bleeding that initially appears to be vaginal might actually have its origin in sites other than those connected to the genital tract. A methodical approach using the history, physical exam, laboratory analysis, ultrasound, and appropriate follow-up usually reveals the correct diagnosis and avoids potential complications or misdiagnoses. Common causes of bleeding in the first trimester are threatened abortion, early pregnancy loss, and ectopic pregnancy; later, the differential diagnosis expands to include spontaneous abortion (miscarriage), hydatidiform molar pregnancy, placenta previa, placenta abruption, and bleeding from the cervix, bladder, vagina, or rectum.
DIFFERENTIAL DIAGNOSIS OF BLEEDING IN PREGNANCY
|
The first bleeding episode in an otherwise normal pregnancy may be implantation bleeding, which typically coincides with an expected menses, 5 to 12 days after ovulation/conception. Often, this bleeding occurs before patients are aware that they have conceived. Implantation bleeding is usually lighter and shorter than a normal menses. The bleeding may be pink or brownish in color. Implantation bleeding has been thought to occur when the trophoblast attaches itself to the endometrium of the uterus, disrupting maternal blood vessels. The duration of implantation bleeding varies considerably, from several hours to several days [3,4]. A survey of 221 women attempting pregnancy was conducted to determine the frequency of very early pregnancy bleeding. Bleeding was defined as one or more days of bleeding or spotting between conception and the end of follow-up, usually eight weeks after the last menstrual period [4]. The women kept daily diaries and provided daily urine samples. Of the 151 women who conceived, 9% recorded at least one day of bleeding during the first eight weeks of pregnancy. Bleeding that resulted in expulsion of a pregnancy was not included in the analysis. Bleeding tended to occur around the time of an expected menses, but rarely on the day of implantation. Most bleeding episodes began five days after implantation; however, no pattern of the timing emerged from this small study. Women who smoked marijuana had a slight increase in bleeding (20% of marijuana smokers versus 8% of those who did not use the drug). Intercourse was not associated with vaginal bleeding. These data suggest that a few days of bleeding in early pregnancy is common and unrelated to pregnancy outcome. Bleeding that stops and then resumes may be associated with higher rates of spontaneous pregnancy loss.
The most common complication of pregnancy is spontaneous abortion (SAB), also referred to as miscarriage. The working medical definition of abortion is termination of a pregnancy by any cause before the fetus is viable. In the United States, an abortion is considered to occur if the pregnancy ends before 20 weeks' gestation or before the fetus weighs more than 500 grams [5]. Because 80% of spontaneous miscarriages occur in the first trimester (i.e., the first 12 weeks of a pregnancy), this is becoming the more commonly used definition of miscarriage [6]. Because the word "abortion" is often associated with elective pregnancy termination, the terms "miscarriage" or "spontaneous pregnancy loss" are often used when talking with patients. The terms "early pregnancy failure" and "failed pregnancy" can be emotionally charged phrases that unintentionally imply failure to the patient and their family and should be avoided. Approximately 80% to 90% of women with a single spontaneous abortion are able to deliver a viable live infant in the next pregnancy [7].
Approximately 2.5% of those trying to conceive experience recurrent pregnancy loss, defined as the loss of two or more clinically recognized pregnancies before 20 to 24 weeks' gestation [181]. Progress in predicting risk and preventing recurrent pregnancy loss has been difficult because of variable clinical presentation and uncertainties about pathogenesis. The common causes include chromosomal errors, anatomic abnormalities of the uterus, autoimmune disorders, and endometrial dysfunction. For most couples, the prognosis for an eventual successful pregnancy is good; however, the likelihood depends on maternal age and number of previous losses [181]. Among 104 patients who underwent a multidisciplinary evaluation for recurrent pregnancy loss, the success rate was 91% for the large subset (80%) with an identified diagnosis and specific treatment [182]. Among the 19 patients without a specific diagnosis who were treated with in vitro fertilization, the success rate was 60%.
The etiologies of miscarriage are only partially understood, and consecutive miscarriages in the same patient are not always due to the same cause [8]. Additionally, the etiology of miscarriage will vary greatly according to gestational age. Preimplantation losses, prefetal losses, and losses with only rudimentary fetal remains generally are due to intrinsic fetal problems (e.g., chromosome abnormality); later losses generally are due to either extrinsic or maternal factors [7,9].
One common cause of spontaneous abortion is a blighted ovum. The blighted ovum involves the fertilization of an egg that results in presence of a gestational sac and placenta but the absence of a fetus. Blighted ovum may be the result of a chromosomal abnormality and will always result in a miscarriage [10]. It has been estimated that at least 50% of clinically recognized SABs are the result of chromosomal anomalies, although some researchers have indicated that the frequency may be as high as 75% to 90% [7,11]. The most common genetic defect is trisomy (i.e., the possession of three copies of a particular chromosome instead of two), followed by X monosomy (i.e., possessing only one copy of a particular chromosome), and polyploidy (i.e., possessing several complete sets of the same chromosomes) [7,11]. Because these abnormalities are random genetic mutations, the statistics still fail to explain a large number of SABs.
The two strongest indicators of threatened spontaneous abortion are extremes of maternal age (younger than 20 years of age or older than 35 years of age) and the presence of vaginal bleeding. Patients 25 to 30 years of age generally have the lowest risk of spontaneous abortion. Those who experience moderate-to-severe bleeding in the first trimester, particularly when accompanied by pain, have been found to be significantly more likely to miscarry than those with less bleeding [12]. Complaints of pain, human chorionic gonadotropin (hCG) levels greater than 500 mIU/mL, and concurrent cervical infection all have been negatively associated with miscarriage [13].
Environmental, autoimmune, mechanical, hormonal influences, plus paternal genetic factors are thought to be responsible for the remaining SABs. Factors not found to be statistically associated with miscarriage include gravidity, parity, prior ectopic pregnancy, one prior miscarriage, prior pelvic surgery, prior cesarean section delivery, prior pelvic inflammatory disease (PID), prior chlamydial or gonorrheal infection, or prior intrauterine device (IUD) use [13].
There are many recognized and as yet unrecognized teratogens that patients may be exposed to in pregnancy. A teratogen is a substance or organism that results in death or abnormality when a fetus or embryo is exposed to it. Vigorous criteria are applied to prove human teratogenicity, including proven exposure to the agent at critical times in the prenatal period, consistent reporting of similar outcomes in epidemiologic studies, careful documentation of clinical cases and presentation, teratogenicity in animals, biologic sense, and experimental proof. A listing of known and suspected teratogens has been catalogued [14]. Teratogens may include infections, such as toxoplasmosis, cytomegalovirus, rubella, parvovirus B19, herpes simplex virus types 1 and 2, human immunodeficiency virus (HIV), Lyme disease, Listeria, and Salmonella[15]. The presence of a sexually transmitted infection (STI) also has been associated with miscarriage. Syphilis, gonorrhea, and chlamydia have all been identified in specimens from first trimester aborted fetuses [2]. Although known infectious causes are rarely to blame for miscarriage, evidence of infection should not be ignored [7,8,9].
Caffeine
There is no evidence that a modest intake of caffeine (e.g., 200 mg/day) alters the risk of pregnancy loss. There are data showing that caffeine consumption greater than 300 mg/day is associated with increased risk of spontaneous abortion, whether of a normal karyotype or chromosome complement fetus [16,17]. The amount of caffeine consumed in food and beverage obviously varies. As a general guide, a 6-ounce serving of coffee contains about 100 mg caffeine [16]. Chocolate consumption has not been associated with an adverse pregnancy outcome [18].
Smoking
Cigarette smoking negatively affects pregnancy in many different ways. The risks appear to be dose dependent. Those who smoke more than 10 to 20 cigarettes a day have almost twice the risk of miscarriage as nonsmokers [19,20]. Prenatal smoking has been associated with 30% of small-for-gestational-age infants, 10% of preterm infants, and 5% of infant deaths. Cigarette smoking before conception may cause reduced fertility and conception delay. Maternal cigarette smoking during pregnancy increases the risk for pregnancy complications (e.g., placental previa, placental abruption, and premature rupture of the membrane) and poor pregnancy outcomes (e.g., preterm delivery, restricted fetal growth, and sudden infant death syndrome [SIDS]) [21; 22]. Between 2000 and 2004, an estimated 776 infants died annually from causes attributed to maternal smoking during pregnancy [22].
Although no increase in overall congenital malformations among smokers has been demonstrated, nicotine may be teratogenic when used in nicotine substitutes, such as nicotine gum or patches [23]. This effect may be the result of higher peak doses achieved by nicotine substitutes over smoking. However, it is possible that the teratogenic effect of tobacco smoke may be masked by the fetotoxic effects that result in spontaneous abortion, thus appearing to increase the teratogenic effects of nicotine substitutes. Passive smoking has been associated with second trimester bleeding and recurrent spontaneous abortion [24,25]. Electronic cigarettes (e-cigarettes) also contain nicotine and are not safe to use during pregnancy. Additionally, some of the flavorings used in e-cigarettes may be harmful to a developing fetus [26].
Alcohol
Alcohol use during pregnancy has been associated with health problems that adversely affect both the patient and fetus. Because there is no clear threshold of safe alcohol intake, no amount of alcohol intake is considered safe in pregnancy [27]. Persons with a very high intake of alcohol have demonstrated an increased risk of preterm delivery and stillbirth; additionally, a high intake during pregnancy may be teratogenic for some. Few studies have been done on the relationship between male alcohol intake and spontaneous abortions; the ones that have been published found no evidence of a direct link. An association has been shown, however, between alcohol consumption and aneuploidy in sperm cells, and spontaneously aborted embryos are frequently abnormal chromosomally [28]. Because alcohol is present in semen shortly after ingestion, it may indirectly interfere with conception and consequently with implantation. Male alcohol intake may, therefore, affect the risk of early pregnancy loss [28]. Abuse of drugs such as cocaine, methamphetamines, and other illicit drugs also has been shown to increase miscarriage rates [11,19].
Chemicals
Environmental exposures to lead, radiation, chemicals, medication, and anesthetic agents such as nitrous oxide have been implicated in pregnancy loss [9]. Spontaneous abortion has been associated with exposure to anesthetic gases, but only in conjunction with several additional factors (i.e., age >35 years, gravida >1, exercise during pregnancy, percentage of inhalational anesthetics >75%, and pediatric anesthesia practice >75%) [29]. However, the American Society of Anesthesiologists has concluded that the case for adverse health effects has not been proven [30].
All pesticides must be approved by the Environmental Protection Agency (EPA) before being sold in the United States. Pesticides are evaluated by the agency based on their effects on children and fetuses, women (especially related to reproductive risks), and minority and disadvantaged persons, whose exposures are often higher due to housing options. An increase has been reported in late fetal and neonatal deaths due to congenital anomalies between 20 weeks and full term in those exposed to pesticides [31]. The risk of fetal or neonatal death was greatest when pregnant patients lived within a mile of the area where the pesticide was applied and were exposed during the third to eighth week of pregnancy. Increased abortion rates have been described in those who have had exposures to multiple pesticides [31]. Occupational exposure to pesticides may increase the risk of spontaneous abortion and adverse reproductive outcomes [32,33,34].
Exposure to high levels of lead during pregnancy also has been found to contribute to miscarriage [35]. Few individuals are exposed to these high levels of lead; however, potential sources include herbal products and nutritional supplements containing lead; older homes with deteriorating lead-based paints; drinking water in homes with soldered pipes; lead crystal cookware and ceramic dishware; some arts and crafts products; work in auto repair shops; and some construction sites [35]. The Occupational Safety and Health Administration (OSHA) has issued standards for lead, mercury, ethylene oxide, ionizing radiation, and dibromochloropropane based on the negative effects on pregnancy, including spontaneous abortion [19,36].
Arsenic also is suspected of increasing the risk of pregnancy loss [37]. Arsenic can be found in higher doses in those living or working near metal smelting plants or whose drinking water is contaminated with runoff of arsenic-based fertilizers. The use of inorganic arsenic compounds has been banned in agriculture [37].
A variety of medications available by prescription have been associated with spontaneous pregnancy loss. For example, retinoid medications, such as isotretinoin, have been associated not only with congenital malformations but with miscarriage as well [38]. Another medication implicated is methotrexate, which may be used for cancer treatments, rheumatoid arthritis, and psoriasis treatments; its use is contraindicated in pregnant patients. Methotrexate interferes with DNA synthesis and cell reproduction and has been used as an abortifacient, although this use is off label [39,40]. Nonsteroidal anti-inflammatory drugs (NSAIDs) also have been associated with pregnancy loss [41,42,43]. Lithium, androgen hormones, captopril, cocaine, warfarin, enalapril, mercury, tetracyclines, thalidomide, and valproic acid have been listed among other teratogens [14].
Malnutrition
Severe malnutrition, as sometimes seen in patients with anorexia or bulimia, may predispose to pregnancy loss. Persons with obesity also have been found to be significantly more likely to have early pregnancy losses and recurrent early losses [44,45].
Stress
Although stress does not appear to have an association with pregnancy loss, individuals experiencing higher stress levels have been found to be more likely to use cigarettes and other substances that do appear to increase early pregnancy loss. Cortisol levels are thought to be a physiologic measure of stress. Pregnancies with increased maternal cortisol levels during the first three weeks of gestation have been found to be more likely to result in early abortion. So, while stress does not appear to play a role in the loss of recognized pregnancies, it may play a role in very early pregnancy loss [46,47,48]. More research is needed in this area before definitive recommendations may be made.
Antiphospholipid syndrome is an autoimmune disorder characterized by the presence of significant levels of antiphospholipid antibodies. Two pertinent antibodies are the lupus anticoagulant and anticardiolipin [49,50]. Antiphospholipid syndrome has been shown to cause recurrent early pregnancy losses [7,50]. Certain endocrine disorders such as hypothyroidism, hyperthyroidism, and poorly controlled diabetes also have been associated with increased pregnancy loss [7,11]. Patients with polycystic ovarian disease may have an increased risk of spontaneous abortion due to elevated levels of luteinizing hormone [7].
Anatomic disorders of the uterus (e.g., fibroids, adhesions, anomalies) and insufficient cervix are mechanical factors contributing to the overall risk of pregnancy loss. Fibroids are benign muscle growths on the uterus. While fibroids are considered to be a normal finding in patients older than 35 years of age, those with multiple smaller fibroids have demonstrated a 67% increased risk of pregnancy loss [51].
Anatomic uterine anomalies have been found in 15% of patients who undergo evaluation for recurrent spontaneous abortion, defined as three or more consecutive miscarriages [52]. Anomalies such as unicornuate uterus, bicornuate uterus, arcuate uterus, septate uterus, and uterine didelphys, have long been identified causes of spontaneous abortion. Theoretically, the mechanism is a combination of space constraints in the uterus and inadequate placental implantation due to vascular changes in the uterus [15]. Pregnancy outcome has been found to be better in uterus didelphys than in unicornuate uterus. Patients with a bicornuate uterus have a 60% likelihood of a successful pregnancy outcome; however, they are at high risk of cervical insufficiency. Septate uterus has generally been associated with poor obstetric outcome [53].
Asherman syndrome is an acquired uterine disorder characterized by the presence of extensive adhesions or scarring in the uterus and is another recognized cause of recurrent abortion. The adhesions of Asherman syndrome are thought to interfere with normal placenta implantation and lead to pregnancy loss [52,54]. Adhesions may follow aggressive dilation and curettage (D&C), intrauterine surgery, or endometritis [11]. Up to 90% of patients with Asherman syndrome have undergone postabortal or postpartum uterine curettage [54].
Diethylstilbestrol (DES) is an estrogen product initially introduced in the 1940s in the United States to treat recurrent pregnancy loss. An estimated 5 to 10 million persons in the United States were exposed to DES between 1938 and 1971, including pregnant women prescribed DES and their children [55]. Uterine abnormalities were common, occurring in about 69% of women exposed to DES in utero [52]. Although banned from use in 1971, it is still possible to encounter pregnant women with DES exposures [55].
Cervical insufficiency, also referred to as cervical incompetence, is diagnosed after pregnancy loss has occurred secondary to painless dilatation of the cervix, usually in the second trimester. It has been associated with uterine abnormalities, DES exposure, obstetric or surgical trauma, cone biopsy, loop electrosurgical excision procedures, use of fertility drugs such as clomiphene, and previous miscarriage during the second trimester [56]. One of the early warning signs of cervical insufficiency may be a pink discharge or bleeding.
At the time of ovulation, the ruptured ovarian follicle develops into a corpus luteum cyst. If an ovum is fertilized, the corpus luteum becomes the corpus luteum of pregnancy, which maintains the uterine lining by producing progesterone during the earliest phases of pregnancy. It has been hypothesized that luteal phase deficiency occurs when the corpus luteum fails to produce sufficient progesterone to maintain a pregnancy [57]. Miscarriages that occur very early in pregnancy may be the result of a corpus luteal defect, although some consider this to be a rare cause of fetal loss [11]. Clinical trial results have suggested that progesterone supplementation may improve pregnancy outcomes in patients with bleeding in early pregnancy, but efficacy data are inconclusive [11,58]. Among 4,153 women enrolled in a randomized, double-blind, placebo-controlled trial commencing from the time of bleeding through 16 weeks' gestation, progesterone therapy did not result in a significantly higher incidence of live births than placebo [183]. The incidence of live births after at least 34 weeks' gestation was 75% in the progesterone group and 72% in the placebo group. It is possible that using progesterone earlier in the first trimester before onset of bleeding might improve outcomes for high-risk patients with the history of recurrent SAB [58,178].
A drug or chemical must be very highly concentrated in seminal fluid to expose an unfertilized ovum directly, although a significant increase in spontaneous abortion has been identified when the father was exposed to lead [19]. While the mechanism is not well understood, it is well accepted that chronic alcohol misuse can impair male fertility by decreasing sperm production [19,59,60]. Studies on animals have shown that paternal alcohol abuse may have an adverse effect on the offspring's immune response and hormone secretion. Furthermore, these animal models indicate that consumption of alcohol may cause damage to sperm, in turn affecting the fetus. Advanced paternal age has been shown to increase the risk for spontaneous abortion as well as genetic abnormalities in offspring due to multiple factors, including DNA damage from abnormal apoptosis and reactive oxygen species [61]. Cellular mutations resulting in conditions such as neurofibromatosis and achondroplasia (a form of dwarfism) have been found more frequently in the children of older fathers [62]. Paternal age also may significantly affect the incidence of Down syndrome [63].
Spontaneous abortions have been categorized into several different types. This includes threatened abortion, complete abortion, incomplete abortion, missed abortion, and septic abortion (Table 2). Each of these types has a unique etiology and recommended treatment plan.
CATEGORIES OF SPONTANEOUS ABORTION
| Type of Abortion | Definition |
|---|---|
| Threatened | Considered when any vaginal bleeding occurs during the first half of a pregnancy |
| Complete | Spontaneous expulsion of the entire products of conception, fetus, placenta, and membranes |
| Incomplete | Spontaneous expulsion of only part of the products of conception, with retained products remaining in the uterus |
| Missed | Death of the fetus without signs or symptoms of pregnancy loss |
| Septic | An abortion resulting in uterine infection with pathogens from the bowel and/or vagina |
A threatened abortion should be considered whenever a patient presents with any vaginal bleeding in the first half of a pregnancy. The bleeding may be bright red, pink, or brown and may or may not be accompanied by uterine cramping. Approximately 15% to 25% of pregnant patients will have first trimester bleeding; 31% to 50% of those will spontaneously abort the pregnancy [64,65,66,67]. This is not preventable. Evaluation of bleeding in pregnancy will include a targeted history, thorough physical exam (including pelvic exam), laboratory analysis, and an ultrasound examination if indicated. Patients with threatened miscarriage have a higher risk of antepartum hemorrhage of unknown origin, placenta previa, manual removal of the placenta, elective cesarean delivery, low birth weight infants, preterm delivery, and malpresentation of the fetus at term than those who do not suffer from threatened miscarriage [24,68,69]. Knowledge of these complications is helpful for healthcare providers continuing to care for patients throughout their pregnancies following a threatened miscarriage. Individuals should be counseled appropriately, and clinicians must be alert to the signs and symptoms of these potential complications.
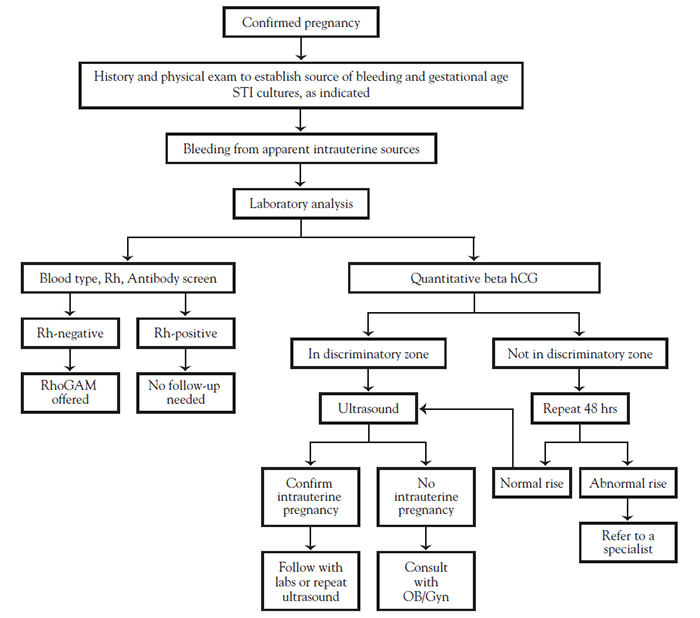
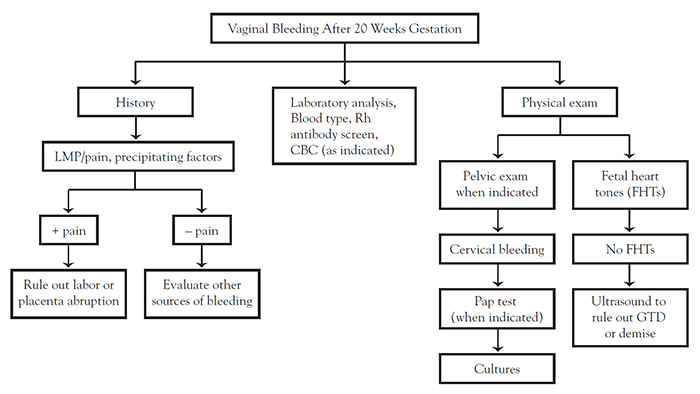
The diagnosis of spontaneous abortion pieces together several diagnostic components. A combination of ultrasound examination and serum hCG levels should be used in tandem with history and physical examination (Figure 1 and Figure 2).
Whether a patient presents in the office setting or emergency room, a thorough interview is the first step in assessing likelihood of threatened abortion [1]. The history should include the patient's gravidity, parity, and number of abortions, whether spontaneous or induced [70]. The patient should be questioned about the first day of the last menstrual period and/or a suspected date of conception. The date of first positive pregnancy test may be useful. Individuals may mistake early pregnancy spotting or implantation bleeding as a light menses; the last normal menstrual period provides a more reliable indicator of gestational age. Inquire also about any history of bleeding disorders.
The amount of bleeding described can be useful to help differentiate SAB from ectopic pregnancy. Moderate-to-severe bleeding has been strongly associated with an ultimate diagnosis of miscarriage [12,13]. Ectopic pregnancy is often heralded by intermittent bright red spotting, while the bleeding that accompanies threatened abortion usually resembles menstrual blood in color and consistency. If the bleeding is heavy or the patient is febrile, immediate referral to an obstetrician/gynecologist is indicated.
Some pregnant patients will experience cervical bleeding following intercourse, bowel movement, and occasionally, heavy lifting. Inquiring about precipitating factors can reassure both provider and patient of the most likely source of such bleeding. However, if a miscarriage is diagnosed, the patient and partner should be reassured that miscarriages are not caused by sexual activity or physical exertion.
The presence of menstrual-like cramps is associated with SAB. Intermittent cramping is most often noted. Severe localized or focal pain more likely reflects another diagnosis, such as ectopic pregnancy [70]. Patients who have experienced SAB often will share whether their previous miscarriage followed a similar course. Their fears, anxiety, and familiarity with their own bodies should be acknowledged.
A careful pelvic exam should be performed. Explanation that a speculum exam is done to evaluate the amount of bleeding and the origin of the bleeding (i.e., vaginal, cervical, or uterine) should be provided to the patient. Careful examination of vaginal discharge also should be done [70]. Common vaginal infections, such as candidiasis, trichomoniasis, and bacterial vaginosis, may be evaluated with laboratory culture. Gonorrhea and chlamydia cultures should be obtained at the same time. Couples who object to, or are offended by, testing for STIs often are reassured by a simple explanation that STIs can go undiagnosed for long periods of time, and testing is a routine part of any complete evaluation of bleeding in pregnancy.
With threatened abortion, the cervix will be closed. If the cervix is dilated and tissue is present at the cervical os, it is considered an inevitable abortion and the tissue should be carefully removed with a ring forceps. The specimen should be sent to the pathology department for identification and evaluation [67,70]. The patient should be informed about the inevitability of the abortion in order to avoid misunderstandings about the treatment.
A bimanual exam follows to estimate gestational age by uterine size. Cervical dilatation must be assessed. The presence, location, and characteristics of pain should be carefully noted [70]. A finding of pelvic masses suggesting ovarian cysts, ectopic pregnancy, or uterine fibroids may lead the examiner to order a pelvic ultrasound exam for more diagnostic information.
First, it is important to confirm the pregnancy with a urine pregnancy test. These are inexpensive and generally accurate, and results are available in minutes. There are other causes of abnormal uterine or vaginal bleeding besides miscarriage, and significant time and money can be saved by first confirming a positive pregnancy test. Laboratory testing also should include potassium hydroxide and "wet prep" microscopy of any vaginal discharge [1].
Quantitative beta hCG levels are useful in assessing threatened abortion [1,70]. HCG is a protein produced in the placenta. It can be detected as early as seven to eight days after conception [1,71]. Production of hCG increases during early viable pregnancy in a predictable pattern, and levels reach their maximum at approximately 10 to 14 weeks' gestation. They then decrease and remain stable throughout the rest of the pregnancy [1,71,72]. When hCG levels are used to assess normal pregnancy viability, a doubling time is used. The commonly accepted doubling rate is a 66% increase in 48 hours [40]. More data have demonstrated that a 53% increase in two days is the minimum rise expected in a viable pregnancy [7,72]. Because there is tremendous overlap in normal ranges, quantitative beta hCGs cannot be used to accurately determine gestational age. Individuals with miscarriage have been found to be more likely to have hCG levels less than 500 mIU/mL than those with ectopic or continuing intrauterine pregnancy, but a single test cannot be used to reliably predict pregnancy loss [13,71].
If bleeding is heavy or the patient complains of light-headedness, fainting, or dizziness, a complete blood count (CBC) should be done [73]. Threatened abortions will seldom result in blood loss significant enough to cause symptoms of anemia. However, patients with hemoglobin less than 10 in the absence of active bleeding should be started on iron supplementation and scheduled for a follow-up appointment. If symptoms exist that make the clinician suspicious for septic abortion, a white blood cell count (WBC) and differential may be useful. Septic abortion should be confirmed by pregnancy testing and usually ultrasonography [70,73].
Rhesus factor (Rh) disease of the newborn is caused by an incompatibility between the blood of a fetus and its mother. It can cause destruction of the fetal red blood cells and subsequent multiorgan involvement. Fifteen percent of the White population and 7% of African Americans lack the Rhesus protein in their blood and are considered Rh negative [74]. If the fetus of an Rh-negative patient has Rh-positive blood, there is a danger that some of the fetus's blood may enter the maternal blood stream, causing the mother's immune system to produce antibodies against this "foreign" blood type. When antibody titers develop, the patient is said to be sensitized or alloimmunized. About 10% of alloimmunizations occur as a result of antenatal hemorrhage, although most occur in the third trimester [75,76]. The amount of fetal blood needed to cause sensitization is less than 0.1 mL, and spontaneous abortions have been associated with a 1.5% to 2% risk of alloimmunization [76].
Blood type, Rh type, and antibody screen should be done on all patients unless written documentation of Rh type is available. RhD antigen has been reported on fetal erythrocytes as early as 38 days' gestation [1,75]. Some providers do not administer Rho(D) immune globulin (RhoGAM), a protectant against an immune reaction, prior to 12 weeks' gestation in those with threatened abortions because the fetal red blood cell mass is so small. Smaller doses of immune globulin (i.e., 50 mcg) are available that may protect against sensitization by quantities less than 2.5 mL of red blood cells [75]. In general, patients who are Rh negative should be offered RhoGAM.
Administration of RhoGAM decreases the risk of developing antibody titers in the event of a maternal-fetal transfusion. For antepartum prophylaxis, RhoGAM should be given at 28 weeks. If given early in pregnancy, it should be administered every 12 weeks to ensure adequate levels of passively acquired anti-Rh. For postpartum prophylaxis, the dose should be administered as soon as possible after delivery, preferably within 72 hours of the first episode of bleeding [76]. It may be given up to 28 days following delivery [39]. However, some experts have recommended administration of RhoGAM whenever the patient presents for bleeding evaluation.
RhoGAM is a blood product, and as such, it may contain infectious agents that could transmit disease [39]. The donated blood used to produce RhoGAM is tested for HIV and hepatitis and treated with a substance that kills bacteria and viruses. There have been no known transmissions of infectious diseases by the administration of RhoGAM in the United States since these treatments were instituted in 1978 [76]. In addition to RhoGAM, other U.S. brand names for the Rho(D) immune globulin include HyperRHO S/D Full Dose, HyperRHO S/D Mini Dose, MICRhoGAM, Rhophylac, and WinRho SDF [39]. Some providers may order a serum progesterone level as well, particularly when the diagnosis is unclear [77]. Progesterone levels greater than 25 ng/mL are considered normal [40]. Progesterone levels less than 5 ng/mL are often correlated with abnormal or nonviable pregnancies. Progesterone values between 10 and 20 ng/mL have little diagnostic value. Because the diagnostic and predictive value of this test has not been proven, it is not often used to make management decisions. In fact, there are several conditions that result in lower progesterone levels than expected during pregnancy, including both maternal and fetal congenital protein and enzyme abnormalities, usually in the cholesterol-producing cascade, which inhibit the production of progesterone [40]. The use of progesterone remains controversial [73].
Ultrasound may be another useful diagnostic tool in the evaluation of first trimester bleeding and threatened abortion. Improved ultrasound technology has enabled early diagnosis of abnormal and ectopic pregnancies, thus decreasing maternal morbidity and mortality [66]. An abnormally shaped gestational sac or slow embryonic heart rate may suggest impending loss [6]. However, the presence of a viable fetus in a patient with bleeding does not always negate the need for quantitative beta hCG testing. Transvaginal ultrasound will usually identify a fetus at quantitative beta hCG levels of 1,500–2,000 mIU/mL [40,67]. Transvaginal ultrasound examination can identify a gestational sac by about four to five weeks' gestation and fetal cardiac activity by five to seven weeks [78,79]. However, multiple gestations with separate placentas and pregnancies with large placentas may demonstrate hCG levels in the 1,500–2,000 mIU/mL range several days before intrauterine pregnancy can be confirmed sonographically [40]. The presence of fetal heartbeat on ultrasound has been shown to be highly predictive of viability of the pregnancy, even in the presence of vaginal bleeding [1,80]. Ultrasound before five weeks' gestation probably is not useful in identifying the uterine or ectopic location of a pregnancy. Prior to seven weeks' gestation, fetal death cannot be confidently ruled out with ultrasound [81].
Some providers order first trimester ultrasound exams to determine whether bleeding has occurred around or behind the placenta or amniotic membranes. Subchorionic hematomas are sometimes found on ultrasound. These hematomas are a collection of fluid believed to be caused by a partial separation of the trophoblast from the uterine wall. The incidence of subchorionic hemorrhage is approximately 1.3% of all pregnancies. Incidences as high as 20% to 25% have been identified in those with vaginal bleeding [83,179]. The clinical significance of subchorionic hemorrhages is unknown. Maternal age, gestational age at the time of diagnosis, and the volume of the hematoma may all contribute to the clinical outcome. Research has suggested that the diagnosis of a subchorionic hematoma at a gestational age less than nine weeks is significantly associated with spontaneous abortion [82].
If the patient is hemodynamically stable, expectant management is the first line of therapy in threatened abortion [1,67]. When a patient initially presents to the office with first trimester bleeding, a quantitative beta hCG should be drawn. The second hCG should be scheduled for approximately 48 hours later. If the patient is seen in the emergency or urgent care department, a second hCG should be scheduled in 48 hours, either with a primary provider, an obstetrician/gynecologist, a nurse practitioner or midwife, or at the initial site. Every effort should be made not to lose the patient to follow-up. It is important to explain to the patient the importance of a second blood test. It can be frustrating to families to learn that the result of the first blood sample is not sufficient to determine whether or not the pregnancy can be expected to continue normally.
Guidelines have been established for ultrasound detection of early pregnancy based on anticipated rise in hCG levels and sensitivity of ultrasonography. Patients with appropriately rising quantitative beta hCG levels should be examined with ultrasound as soon as the levels reach 2,000 mIU/mL [67]. However, the discriminatory hCG level varies with the type of ultrasound machine used; most radiology departments develop their own criteria regarding the level of hCG at which an early pregnancy should be visible. Providers should be familiar with their facilities' capabilities. Ectopic pregnancy can usually be ruled out by normally rising hCG levels and identification of an intrauterine pregnancy. Early pregnancy loss can be diagnosed in patients with ultrasound findings of a mean gestational sac diameter >25 mm with no embryo and no fetal cardiac activity when the crown-rump length is at least 7 mm [184].
Patients should be advised that bed rest will not prevent miscarriage [84]. Normal, reasonable daily activities may be continued. Pelvic rest is indicated until the follow-up appointment has been attended; orgasm and sexual activity should be avoided [85]. Nothing should be inserted into the vagina until bleeding has stopped. Aspirin and NSAIDs may increase bleeding and should not be taken. Acetaminophen is generally considered safe during pregnancy when used at therapeutic doses for short periods of time [39].
One of the most frequently heard complaints is the lack of follow-up and consistency in managing SAB or threatened abortion. When possible, patients should interact with the same provider for follow-up and phone calls. Telephone calls to the patient to offer support and determine if new symptoms have arisen are often appreciated. Such efforts communicate to the patient that the provider understands that the experience is a difficult and, at times, traumatic event.
Whenever managing the care of a patient with a threatened abortion, the availability of someone to promptly evacuate the uterus if hemorrhage occurs is vital. While expectant management may be appropriate, anticipating complications is crucial. Nurse-midwives, nurse practitioners, physician assistants, and family physicians should have ready access to a surgeon who can manage any complications resulting from spontaneous abortion.
Spontaneous expulsion of the entire products of conception is called a complete abortion [1]. Typically, patients will present with complaints of heavy vaginal bleeding and cramping followed by the passage of tissue. The pain and bleeding subside after tissue is passed. It is sometimes difficult to determine that a complete abortion has occurred until some time has passed. Continued bleeding suggests an incomplete rather than a complete abortion.
Pathology evaluation of tissue is recommended in some cases to confirm intrauterine pregnancy and rule out trophoblastic disease [2].
Historical data similar to that obtained with a threatened abortion apply to the assessment of a complete abortion. Patients should be questioned about the first day of their last normal menstrual period and/or a suspected date of conception. The date of the first positive pregnancy test may be useful. The first day of the last menstrual period should also be documented to help identify gestational age and provide a point of reference for physical findings.
Patients should be questioned about the onset, duration, and amount of bleeding and the passage of any tissue or clots. Information about uterine cramping is useful. If the bleeding diminished significantly and cramping resolved after the passage of tissue, a complete abortion is likely.
Both speculum and bimanual examinations are indicated for the evaluation of a complete abortion. Speculum exam is performed to evaluate the condition of the cervical os, bleeding and the presence of cervical or vaginal discharge, and signs of vaginal or cervical infections. Speculum exam will most likely reveal a closed or partially open cervical os.
If the products of conception have not been completely expelled, tissue may be visible at the os. The tissue should be carefully removed with a ring forceps and sent for pathology examination. The amount and color of the bleeding should be noted.
A bimanual examination is done to assess the size of the uterus and the presence of any pain or tenderness. While mild cramping and tenderness would be expected with a complete abortion, any significant pain requires further evaluation for infection. A WBC should be ordered if there is any evidence of endometritis, such as uterine tenderness, fever, or chills [86].
The pregnancy should be confirmed with a urine pregnancy test [70]. Pregnancy tests may remain positive for several weeks after spontaneous abortion. A negative pregnancy test most likely points to other causes of the bleeding. Laboratory evaluation of blood type, Rh type, and antibody screen to determine the need for RhoGAM should be done on all patients unless written, trusted documentation of blood type and Rh are readily available [70]. An antibody screen is indicated for those who are Rh-negative. RhoGAM should be offered to all of these patients.
Because the bleeding that accompanies spontaneous abortion can be significant, a hemoglobin and hematocrit/CBC will be useful to determine the need for additional iron supplementation, especially in those who may have been anemic prior to conception.
Quantitative beta hCG levels may be useful if the bleeding continues but need not be done immediately if complete abortion is suspected. HCG levels should return to negative 9 to 35 days after the abortion. The average length of time for the hCG to return to negative is 19 days [87].
Ultrasound examination is only useful in the management of complete abortion to identify retained products of conception if bleeding continues [88]. Some practitioners do order ultrasound exams, but they are not conclusive and are only used as an adjunct to other management and diagnostic tools.
Patients and their families should be educated about what to expect following a complete abortion. Bleeding should be monitored closely. Most will continue to have bleeding similar to a light period for about one week after a spontaneous abortion. Spotting may continue longer, but should be reported if it persists more than 10 days. Any foul-smelling discharge, fever, chills, increasing pain, or bright red bleeding that saturates one pad an hour should be reported immediately [85]. Providers should also be notified of any flu-like symptoms.
Pain control can usually be achieved with NSAIDs. Prescription narcotics are not usually needed, but this must be individualized. Application of ice and/or heat to the lower back may alleviate some pain.
Acknowledgment of a patient's grief and a discussion of the common feelings of guilt, anger, and helplessness are appropriate. Planned and unplanned pregnancies bring complex emotional responses. The loss of the pregnancy can be extremely stressful for patients and their support system [6]. Pregnancy loss can result in both acute stress disorder and post-traumatic stress disorder (PTSD) [89]. Most patients will adequately deal with their grief with the support of family, friends, and healthcare providers. However, the magnitude of the loss should not be underestimated. For some, the emotional trauma comes from realizing that the miscarriage is irreversible and is perceived as an unbearable, life-altering event. Some may mourn for much longer than expected, even after the birth of a healthy child [90]. Involved partners also struggle with the loss. Couples may grieve differently and move through the stages of grief at different paces. One should remember to ask the partner if they have any questions or if anything can be done for them [90]. Grief support groups for miscarriage are available, and many Internet sites can offer support and information (Appendix). Patients and their families should be reminded to call if any signs of depression occur, including appetite changes, daily crying for more than one week, sleep pattern changes, hopelessness, and suicidal thoughts or ideation.
Patients are advised that they may resume their normal activities after a day or two of rest. If bleeding becomes heavier after activity, too much activity has probably been resumed too soon. If bleeding becomes heavy enough to saturate one pad an hour, they should be seen immediately. Encourage the patient to consume a healthy diet and an adequate fluid intake. If a patient has been taking prenatal vitamins or a multivitamin, those should be continued.
Vaginal abstinence is stressed until the two-week follow-up appointment has been completed. At two weeks, a pelvic exam should be done to evaluate uterine size and tenderness. Testing for STIs may be completed as appropriate. A urine pregnancy test may be adequate to confirm resolution of the hCG levels, if known.
At the follow-up visit, the patient and partner will often want to discuss planning a future pregnancy. There are two factors that should be taken into consideration during this discussion. The first is physical healing. There is no physiologic evidence for delaying pregnancy attempts following non-molar, non-ectopic pregnancy loss before 20 weeks' gestation. A 2016 study concluded that those who waited three months or less achieved higher live birth rates than those who waited more than three months before trying to conceive [91].
Nevertheless, individuals need time to heal from a loss. Loss of a pregnancy, desired or unwanted, is difficult. Patients and their partners should be advised to delay another pregnancy until they are emotionally able to face the risk of another pregnancy loss. While another loss may be unlikely, it is possible.
If another pregnancy is not desired, birth control options should be discussed and prescribed. Fertility can return as early as 10 days after an abortion. Patients may start an appropriate contraceptive method (e.g., pills, patch, ring, shot, IUD, hormone implant) immediately after a completed spontaneous abortion if desired [92].
When some of the products of conception are passed but more remain inside the uterus, an incomplete abortion has occurred [1,70]. Prior to 10 weeks' gestation, the fetus and placenta are most often expelled together. After 10 weeks' gestation, the placenta may be retained.
Patients being assessed for incomplete abortion should be questioned about the first day of their last menstrual period, suspected date of conception, and/or the date of first positive pregnancy test. Inquiry about any history of bleeding disorders is also useful. Information regarding the amount of bleeding and the passage of any suspected tissue or clots should be noted [70]. Referral to an obstetrician/gynecologist is indicated for significant blood loss or suspected infection. Incomplete or inevitable abortion is characterized by bleeding, gross rupture of membranes, severe menstrual-like cramping, and cervical dilatation [6,68]. A history of passing tissue or "blood clots" may be reported. The blood clots may be described as tan or gray colored. Bleeding can be profuse and may produce hypovolemia [93].
An undiagnosed pregnancy should always be considered when a patient presents with vaginal bleeding and pain; a urine pregnancy test should be completed. Blood type, Rh type, and antibody screen are indicated and, as is almost always the case, RhoGAM should be offered to the pregnant Rh-negative patient.
The patient may have been bleeding heavily or for an extended period of time with an incomplete abortion [68]. Therefore, a CBC or at least a hemoglobin, hematocrit, and WBC are indicated. While disseminated intravascular coagulation (DIC) is a concern for patients with fetal demise in the second half of pregnancy, evaluation of bleeding studies is not indicated for first trimester or early second trimester (before 18 weeks) incomplete or missed abortions [6].
Tissue may be found at the cervical os during speculum exam. If tissue is seen, it should be carefully grasped with a ring forceps and removed. This facilitates uterine contractions and hemostasis [68]. Any tissue recovered must be sent to the pathology lab for evaluation. The cervix may be dilated or closed [68]. If tissue is removed, bleeding will usually subside. If no tissue can be removed, a D&C may be required. Cervical cultures and a sample of the discharge should be examined to identify the presence of any STIs or vaginal infections. Any infections should be treated to minimize the risk of ascending uterine infection resulting in endometritis.
A bimanual examination is done to assess the size of the uterus and the presence of any unusual pain or tenderness. Exam may reveal an enlarged and soft uterus [68]. Any pain out of proportion to the clinical presentation requires further evaluation for infection. Again, a WBC should be ordered if there is any evidence of endometritis.
Expectant, medical, or surgical management may be appropriate. Immediate surgical treatment or hemotransfusion may be indicated for some patients, such as those who are hemodynamically unstable as a result of heavy bleeding, or those in whom a septic abortion is suspected [68]. In other cases, expectant management (i.e., watchful waiting while conducting necessary examinations and tests) may be chosen [10].
Expectant management is recommended as first-line treatment for patients with incomplete abortion; 82% to 96% of these patients will complete the process spontaneously within two to four weeks [1,184]. The probabilities for successful treatment have been demonstrated to be comparable, but not superior to, medical and surgical intervention. Given the lack of clear superiority among the options, the patient's preference should play a dominant role in the decision making [80,94,95,96,97]. Researchers have found that those undergoing management of first trimester miscarriage would value being offered alternatives (i.e., medical management or surgical management) to expectant management [95,97,98,99,100]. Physician recommendations have been reported to play an important role in patient decision making [98,100].
A D&C or suction curettage may be necessary to complete the abortion in early gestations. Consultation with an obstetrician/gynecologist or a provider qualified to perform the procedure is indicated. When the miscarriage is inevitable, surgical treatment may be necessary to stop the bleeding [10]. In more advanced gestations, high-dose oxytocin may be used to cause the uterus to contract and expel its contents [101]. Once again, the presence of a provider able to perform a D&C and/or manage the complications that may be encountered is critical to patient safety. Pain medication should be used appropriately.
Incomplete abortion has continued to disproportionately contribute to maternal morbidity and mortality in much of the developing world. Although surgical management has been the standard of care worldwide for years, medical management using misoprostol has been gaining attention as a safe, effective, and low-cost alternative treatment [57,97,102]. Misoprostol use avoids surgery and its associated complications and, when compared to expectant management, has demonstrated higher success and acceptability rates in some studies, whereas other studies indicate that expectant management is equally safe and prevents surgery for most [102,103,104,105,106]. Many regimens for using single-dose misoprostol have been studied. One common regimen is 800 mcg vaginally, with a repeat dose 24 to 48 hours later if the first is unsuccessful [184]. A more effective regimen for medical management has been reported, using pretreatment with 200 mg of oral mifepristone (Mifeprex), followed in 24 hours by 800 mcg of vaginally administered misoprostol. In a randomized trial (300 patients), pretreatment with mifepristone followed by treatment with misoprostol resulted in a higher likelihood of successful management (87%) than treatment with misoprostol alone (67%) [185]. Among patients undergoing medical management of incomplete abortion, cramping pain and vaginal bleeding is to be expected for several days, which may persist for two weeks or longer [104].
Misoprostol has not been approved by the U.S. Food and Drug Administration (FDA) for induction of labor, and it carries a boxed warning for pregnant patients who may receive the drug [39,108]. The FDA-approved use of misoprostol (in conjunction with mifepristone) is for the medical termination of pregnancy of ≤63 days [39].
If a patient undergoing medical abortion has symptoms of nausea, vomiting, diarrhea, or weakness, without fever or other signs of infection, sepsis should be considered. Treatment with antibiotics, with coverage that includes anaerobic bacteria, has been recommended in these cases [39]. Follow-up care of a patient experiencing an incomplete abortion is similar to that for a patient experiencing a complete abortion. Quantitative beta hCG levels are used in this case to confirm that the uterus has been emptied completely; this test should be done weekly until negative. Ultrasound exams are not usually indicated for follow-up in the absence of complications but may be used as an additional diagnostic tool if incomplete abortion status cannot be confirmed with history and exam [57]. However, ultrasound studies prior to suction curettage may be indicated. On rare occasions, one fetus of a multiple gestation is aborted and a normal retained fetus can be delivered at term [6].
Bleeding should be monitored closely. Most patients will continue to have bleeding similar to a light period for about one week after surgical treatment. Spotting may continue longer, but should be reported if it lasts more than 10 days. Patients are advised that they may resume their normal activities within a day or two. Any abnormal symptoms, including persistent heavy bleeding, fever, chills, or vaginal discharge, should be reported immediately. Furthermore, patients should be encouraged to maintain a healthy diet, adequate fluid intake, and consumption of prenatal or multivitamins.
The experience of incomplete abortion interferes with a patient's daily activities and may cause significant emotional and physical pain. Reminders of healthy self-caring activities can help patients and their significant others become grounded again in daily life. Information about what to expect in the coming weeks may help individuals regain a sense of control in their lives.
The physical discomfort accompanying miscarriage quickly resolves [10]. Most report their cramping is gone within days and managed effectively by over-the-counter NSAIDs. If patients have medical contraindications to or intolerance of NSAIDs, stronger prescription pain relief may be indicated.
The patient's partner, when involved, should also be encouraged to return to normal daily activities as soon as possible. Grief and frustration should be acknowledged [10]. Because everyone grieves differently, some patients report feeling like their partners did not understand how hard this loss was for them [109]. Giving permission for a discussion of their feelings of helplessness, anger, failure, and guilt is important. Some partners are simply grateful that their loved one is safe. Patients without an involved partner may experience special challenges locating a source of support. A listing of community and Internet sources of support can be found at the end of this course (Appendix).
Sexual activity should be discouraged until the two-week follow-up appointment has been attended. A pelvic exam is usually done at that time to determine if the uterine size has returned to normal and if any pelvic tenderness exists. Testing for STIs and a Pap test can be performed at this appointment, if indicated. Fertility can return quickly after miscarriage, and birth control should be provided if desired. If another pregnancy is desired, a discussion of both physical and emotional healing is important.
A missed abortion occurs when the fetus has died without signs or symptoms of pregnancy loss. The products of conception may be retained for several weeks while the pregnancy appears outwardly normal [70].
Those who experience missed abortions may or may not have bleeding. Typically, the uterine size is less than would be expected based on gestational age, there is an absence of fetal heart tones, and the patient may report a subjective loss of pregnancy symptoms such as nausea, vomiting, fatigue, and breast tenderness. Maternal weight loss and/or regression of mammary changes of pregnancy may be noted [7,70,85].
If a patient is seen with symptoms of a missed abortion, ultrasound evaluation is indicated to assess pregnancy viability. Missed abortion may be confirmed if ultrasonography reveals the disappearance of a previously detected embryonic or fetal cardiac activity or the absence of such activity at more than seven weeks in a well-dated intrauterine pregnancy [7,70]. Because of the limits of ultrasonography, a good menstrual history will be useful to determine expected gestational age. Depending on the estimated gestational age, a repeat ultrasound may be indicated two weeks after the first ultrasound reveals absence of fetal life. In some instances, the estimated gestational age is incorrect and repeating the ultrasound in two weeks will demonstrate a viable intrauterine pregnancy.
Laboratory evaluation with hCG levels may be used to identify intrauterine fetal death. Failure of the hCG levels to rise as expected or falling hCGs may be used to confirm the diagnosis of pregnancy loss. Coagulation defects due to retained products of conception in the first half of pregnancy are possible, but rare [6].
Again, blood type, Rh type, and antibody screen are necessary to prevent Rh disease. RhoGAM should be offered to all Rh-negative individuals as soon as the missed abortion is identified and management initiated.
Treatment of missed abortion is generally either uterine evacuation or, at less than 10 weeks, waiting for spontaneous passage of the products of conception. Evacuation usually involves suction curettage (at ≤12 weeks); dilation and evacuation (at 12 to 23 weeks); or medical induction (for those without prior uterine surgery) at 16 weeks to 23 weeks (for the treatment of late fetal death). Late evacuation increases the potential for placental bleeding, uterine perforation, and difficulties dilating the cervix. Preoperative use of cervical dilators (e.g., laminaria), misoprostol, or mifepristone may reduce the incidence of these complications [6]. Surgical evacuation of the uterus for missed abortion is common. Follow-up care of a patient experiencing a surgically complete abortion is similar to that for a patient experiencing a complete abortion. Quantitative beta hCG levels are used in this case to confirm that the uterus has been emptied completely. They should be done weekly until negative [6].
Although evacuation of the uterus using misoprostol has been determined to be an acceptable treatment for missed abortion, there have been reported cases of adverse events and death from the medication [39]. More than 85% of patients reportedly respond to the first dose of misoprostol, and reported success rates following administration of misoprostol have been high [6,110]. Candidates for misoprostol treatment of missed abortions should not have an IUD in place; be free of signs or symptoms of endometritis or sepsis; and have ectopic pregnancy ruled out [57]. Patients must also have immediate access to emergency care, transportation, and communication. Side effects vary but include nausea, vomiting, diarrhea, chills, and pain [39].
The delayed identification of a pregnancy loss that inevitably accompanies missed abortion can compound patient and family grief. Many have already shared the news of their pregnancy with family, friends, and coworkers and now find themselves needing to tell these same people of the loss. Some express regret at having shared their pregnancy too soon. It may be helpful to remind couples that their friends and family would feel saddened knowing that such a loss had occurred and that they were unable to offer their support and help. Care providers should offer open support and information and direct the family to appropriate resources [74,109].
Although septic abortion (once a leading cause of maternal mortality) has become less frequent due to changes in abortion laws, any type of SAB can be complicated. Usually, pathogens from the bowel and vagina are implicated in the infectious process. Polymicrobes such as Escherichia coli and other gram-negative rods are encountered. Staphylococci and streptococci are also seen [6]. Bleeding, pain, fever, chills, and a foul-smelling vaginal discharge are the hallmarks of the endometritis that accompanies septic abortion [10]. A septic abortion may result in endometritis, parametritis, peritonitis, and septicemia. Acute renal failure and septic shock may follow.
The initial evaluation for septic abortion should include a physical and pelvic exam. A urine test to confirm the existence of a pregnancy is important to rule out other sources of infection, such as pelvic inflammatory disease or toxic shock syndrome. Smears from the cervix should be taken to identify microbes [6]. CBC, electrolyte, blood urea nitrogen (BUN), and creatinine studies are appropriate. Blood type, Rh type, and antibody screen are indicated. Anaerobic and aerobic blood cultures and any available products of conception should be obtained for evaluation [6].
Prompt referral to a provider able to admit the patient, empty the uterus of any remaining products of conception, and initiate treatment with IV antibiotics is critical. A large-bore angiocatheter should be started, and tetanus toxoid should be administered. Abdominal x-rays help detect free air or foreign bodies [6].
Prompt evacuation of the uterus is critical and should be performed within a few hours after initiation of parenteral antibiotics. A regimen of high-dose, broad-spectrum antibiotics is recommended, directed against common gram-positive pathogens, enteric gram-negative bacilli, and anaerobes such as Bacteroides fragilis[6].
Often, in the face of a life-threatening event, the loss of a pregnancy is not recognized until recovery from the crisis has occurred. Patients with septic abortion have many feelings about their experience, and referral to a skilled grief counselor may be helpful. Bleeding must be monitored, and the patient should be encouraged to call a provider with any malodorous discharge, increases in pain, fever, chills, heavy bleeding, or other symptoms of discomfort. Birth control options should be offered to the patient at the follow-up visit, although they may be started sooner if requested.
The implantation and growth of fetus and placenta outside the uterine cavity is called an ectopic pregnancy. While ectopic pregnancies occur most commonly in the fallopian tubes, ectopic pregnancies have been described in the ovaries, cervix, uterine cornua, abdomen, and other remote sites (Table 3) [40,111,112,113].
The incidence of ectopic pregnancy among all pregnancies is 1% to 2% in the United States. Serious complications arise from bleeding into the fallopian tube and rupture into the pelvic cavity. The mortality rate from ectopic pregnancy has decreased over the past four decades. For the period 1980–1984, the rate was 1.15 deaths per 100,000 and by 2004–2007 the rate had decreased to 0.50 deaths per 100,000 [186]. Despite this decline in incidence, ectopic pregnancy remains the leading cause of first trimester pregnancy-related deaths, accounting for 9% to 15% of all maternal deaths in early pregnancy [111,114]. A patient's reproductive future also may be compromised by ectopic pregnancy. Ectopic pregnancies were described as early as the 11th century and have historically been thought to be universally fatal [40,114].
A lack of clear reporting standards and the treatment of many ectopic pregnancies in outpatient facilities have made quantifying their incidence difficult [113]. The actual incidence may be higher than 2% due to a variety of epidemiologic trends, such as [113]:
A continued increase in the number of associated risk factors (e.g., tubal surgery, tubal ligation, previous ectopic pregnancy)
Improved diagnostic methods
Increased use of assisted reproductive technology (ART)
The early detection of pregnancy, improvements in aseptic technique, antibiotics, anesthetic agents, availability of blood and blood products, and surgical techniques have contributed to the decline in maternal mortality. Treatment has evolved beyond saving the life of the patient to preserving their future fertility.
Any event that impairs ability of the tube to transport gametes or embryos will predispose an individual to ectopic pregnancy [111,113]. The most common site of ectopic pregnancy is the fallopian tube, accounting for more than 98% of all ectopic gestations [113]. While most who present with ectopic pregnancy have no identifiable risk factors, several factors have been associated with ectopic pregnancy, including a history of PID, history of ectopic pregnancy, history of prior tubal surgery, use of ART, use of IUD for contraception, advanced maternal age, and altered tubal motility [40,111,112,113,114,115]. Because IUDs are effective contraception, the incidence of ectopic pregnancy in those using IUDs is low. However, if a person conceives while using a hormone-releasing IUD, there is an up to 50% chance the pregnancy will be ectopic [116,117]. The risk of ectopic pregnancy in clinical trials of women with IUDs and no other risk factors was about 1 in 1,000 users per year [116,117].
The most common cause of PID is Chlamydia trachomatis. Patients with chlamydial infection have a range of clinical presentations, from salpingitis to PID; more than 50% of infected women are unaware of their exposure. Other organisms that cause PID (e.g., Neisseria gonorrhoeae) may also increase the risk of ectopic pregnancy. A history of salpingitis has been found to increase the risk four-fold [114]. Recurrent pelvic infections have been shown to increase the likelihood of tubal occlusions by as much as 13% after one infection, 35% after two infections, and 75% after three or more infections [113,114].
Patients who have had a prior ectopic pregnancy are six to eight times more likely to experience another; 7% to 14% of patients experience more than one ectopic pregnancy [113,114]. The rate of recurrent ectopic pregnancy has been estimated to be approximately 13% after a history of one, 35% after two previous ectopics, and 75% after three episodes [113,114].
Pregnancy after tubal ligation or tubal surgery has been demonstrated to increase the risk of ectopic pregnancy; however, the increase depends on the nature of the surgery and the extent of anatomic damage [114]. When pregnancy occurs following tubal surgery, suspicion for ectopic pregnancy should be high [113,114]. An estimated 35% to 50% of patients who conceive after tubal ligations have been reported to experience an ectopic pregnancy, usually two or more years following sterilization [114]. Patients who have chosen to reverse tubal ligation have demonstrated an increased risk of ectopic pregnancy due to scars and/or adhesions that may decrease tubal motility [40].
Use of ART has been associated with adverse maternal and infant outcomes, such as placenta previa, preterm delivery, cesarean delivery, low birth weight, and infant mortality [118]. Ovulation induction with clomiphene citrate (brand names Clomid and Serophene) or injectable gonadotropin therapy has been associated with an increased risk of multiple pregnancy and a four-fold increase in the risk of ectopic pregnancy [114,119]. Variation in ectopic pregnancy rates has been observed based on the type of procedure performed [115]. Infertility patients with luteal phase defects have demonstrated a higher rate of ectopic pregnancy than patients whose infertility is caused by anovulation, and their risk increases dramatically when ART, such as in vitro fertilization (IVF) or gamete intrafallopian transfer (GIFT), has been used [113,114].
The presence of an inert copper-containing or progesterone-eluting IUD traditionally has been thought to be a risk factor for ectopic pregnancy. However, findings have indicated that the use of an IUD does not increase the risk of ectopic pregnancy and that, overall, the incidence is very low (i.e., 1 in 1,000 during a five-year insertion) [120].
Although IUDs are more effective in protecting from intrauterine pregnancy than from ectopic pregnancy, IUDs are highly protective against ectopic pregnancy due to their high efficacy in preventing any pregnancy. Patients who use copper-bearing IUDs have a lower risk of ectopic pregnancy than those who use no contraception. Of the rare pregnancies that do occur in those who use IUDs, 92% to 94% will not be ectopic [121].
Patients 35 to 44 years of age have a three- to four-fold greater risk of ectopic pregnancy than those 15 to 24 years of age [113,114].
Altered tubal motility is another risk factor for ectopic pregnancy. Causes of altered tubal motility include smoking, peritubal adhesions resulting from prior salpingitis, endometriosis or tubal surgery, developmental abnormalities of the uterus or tubes, tubal distortion caused by myomas, adnexal mass, or loss of myoelectrical activity in the fallopian tube as a result of aging [113,122].
Technologic improvements have made possible the early diagnosis of ectopic pregnancy [114]. Its hallmark has historically been abdominal pain with spotting, usually occurring six to eight weeks after the last normal menstrual period; however, up to 30% of patients with ectopic pregnancies present with no vaginal bleeding [111,114,123]. The pain is generally described as sharp and stabbing. It may be intermittent, vary in intensity, and localize to one side of the pelvis. Other symptoms depend on the location of the ectopic pregnancy and may include chest or shoulder pain, nausea, pain with intercourse, vertigo, syncope, and orthostatic blood pressure changes [111,114]. Amenorrhea may not be present; some simply report a delay in menses or spotting. Approximately 20% of patients with ectopic pregnancy are hemodynamically unstable at presentation [113,114]. Ectopic pregnancy may present with symptoms similar to other conditions, and the differential diagnoses may include appendicitis, salpingitis, spontaneous abortion, ovarian cyst, ovarian torsion, urinary tract infections, degenerating uterine fibroids, and normal pregnancy (Table 4).
Approximately 40% to 50% of ectopic pregnancies are misdiagnosed at initial presentation to an emergency department, primarily due to failure to identify risk factors. Proper history, physical examination, and identification of risk factors are critical to an accurate, timely diagnosis [111,123].
A menstrual history is useful in assessing ectopic pregnancy. Many report a delayed or lighter menses than normal. The bleeding that accompanies ectopic pregnancy is intermittent and may be brownish in color or bright red.
A high index of suspicion is necessary for any patient who has a positive pregnancy test, pelvic pain or tenderness, and spotting. Abdominal tenderness is present in 90% and rebound tenderness in 70% of patients with ectopic pregnancies [113]. Significant abdominal tenderness may suggest ruptured ectopic pregnancy [123]. On pelvic exam, the uterus is usually enlarged appropriate to gestational age. Uterine enlargement in early pregnancy is the result of hypertrophy of the uterine wall under stimulation by estrogen and progesterone. After the third month of pregnancy, uterine enlargement is also due in part to the mechanical stretching of the enlarging fetus [124]. Adnexal mass and/or tenderness may also be noted during pelvic examination. The cervix may be displaced to one side due to adnexal mass, and cervical motion tenderness may be present [85,123]. It is important to note that no combination of physical findings can reliably exclude ectopic pregnancy [123].
Diagnostic tests include a urine pregnancy test, ultrasonography, beta hCG measurement, and occasionally, diagnostic curettage [123].
In hemodynamically stable patients, serial hCGs may be useful in the evaluation and diagnosis of ectopic pregnancy. As previously noted, the quantitative beta hCG levels in a normal intrauterine pregnancy should increase 66% during a 48-hour period [40]. An increase in beta hCG levels less than 66% reflects an abnormal intrauterine pregnancy or an ectopic pregnancy. However, it is important to note that approximately 10% of all ectopic pregnancies will have normally rising hCG levels [40,114]. Serial beta hCG levels that do not appropriately increase have been found to be only 36% sensitive and 65% specific for detection of ectopic pregnancy [123]. hCG levels alone cannot be used to diagnose ectopic pregnancy with absolute certainty. Although serum progesterone levels are useful for detecting pregnancy failure and identifying patients who may be at risk for ectopic pregnancy, they are not diagnostic of ectopic pregnancy and may create the potential for delayed diagnosis [114,125]. The sensitivity of progesterone levels is low (15%), and 85% of patients with ectopic pregnancy will have normal serum progesterone levels [123].
Blood type, Rh type, and antibody screen should be done on all patients; Rh disease of the newborn may occur in ectopic pregnancies.
Ultrasound may be one of the most useful tools in the diagnosis of ectopic pregnancy. Its limitations are based largely on availability and the gestational age of the pregnancy [123]. Visualization of an intrauterine gestational sac, with or without a fetal pole (i.e., thickening on the margin of the yolk sac), may be enough to exclude ectopic pregnancy. Most intrauterine pregnancies will be visible by transvaginal ultrasound by five to six weeks' gestation [6,123,126]. Visualization of ectopic cardiac activity, on the other hand, is considered diagnostic for ectopic pregnancy. Presence of an ectopic gestational sac or an ectopic mass and fluid in the pouch of Douglas is strong evidence of ectopic pregnancy [113,123].
Although rare, heterotopic pregnancies (i.e., ectopic and intrauterine twin gestations) do occur. The risk of heterotopic pregnancy is thought to be about 1 in 4,000 pregnancies but may increase with ART [113,126]. Findings of an extrauterine ectopic pregnancy on ultrasound may include a live extrauterine embryo, absence of an intrauterine gestational sac, free fluid in the pelvis or peritoneum, adnexal mass, hematosalpinx, and/or adnexal ring sign on a color Doppler ultrasound [112].
A "discriminatory zone" of levels of hCG has been developed and designated as the level of hCG at which ultrasound evidence of pregnancy may be consistently seen [123]. Most facilities establish their own zone. With transvaginal sonography, it is commonly between 1,500 and 1,800 mIU/mL [112,113,114,123]. With transabdominal sonography, the value is >6,500 mIU/mL [113,123]. Compared with abdominal ultrasonography, transvaginal ultrasonography diagnoses intrauterine pregnancies an average of one week earlier due to its higher sensitivity and lower discriminatory zone. If transvaginal ultrasound does not reveal an intrauterine pregnancy at the expected discriminatory zone, an extrauterine pregnancy can generally be diagnosed [123]. Despite the accuracy of transvaginal ultrasound, an adnexal mass will not be found in 15% to 35% of patients with an ectopic pregnancy [113]. Thus, a high level of suspicion is often necessary to reach the correct conclusion.
If an abnormal pregnancy is diagnosed by abnormally rising or falling beta hCG levels, a D&C may be used to determine if an intrauterine pregnancy is present. Chorionic villi float in saline, permitting identification of tissue obtained by curettage, although microscopic examination is more accurate [113,126]. If fetal and/or placental tissue is present in the uterine contents following D&C, an ectopic pregnancy can be ruled out with some confidence. Curettage should only be considered when beta hCG levels are falling or when levels are elevated and ultrasonography has not shown intrauterine pregnancy. Diagnostic uterine curettage could terminate a desired pregnancy [123].
A rarely used and less accurate method of diagnosing ectopic pregnancy is a culdocentesis [127]. A needle is inserted into the posterior vaginal fornix of the cul-de-sac and aspiration of blood is attempted. If non-clotting blood is found, a ruptured ectopic pregnancy is suspected and operative evaluation indicated [114]. Because ultrasonography can reveal the presence of any free fluid, culdocentesis is used primarily when ultrasonography is not readily available [127].
Patients who are hemodynamically unstable may have the diagnosis of ectopic pregnancy made at the time of laparoscopy or laparotomy [127]. However, laparoscopy can miss up to 4% of early ectopic gestations [113,114].
A variety of new laboratory markers are under development to accurately identify ectopic pregnancy at an early stage. Vascular endothelial growth factor, pregnancy-associated plasma protein A, and human placental lactogen, alone and in combination, have been investigated [126]. Validation studies are now necessary.
The treatment options for ectopic pregnancy include surgery, medical treatment with a variety of drugs, and expectant management [128].
Historically, laparotomy and salpingectomy have both been used to treat ectopic pregnancy. However, laparoscopic surgery has now become the standard approach in most cases [114,128]. Laparotomy is reserved for patients who are hemodynamically unstable [114].
The mode of surgical treatment of ectopic pregnancy may vary depending on the location of the pregnancy [40]. Most laparoscopic surgical approaches include a linear salpingostomy and the removal of the products of conception in an unruptured pregnancy. Every effort is made to minimize damage to the fallopian tube and preserve the patient's reproductive future. Removal of the affected tube may be necessary and, although extreme, can be an effective treatment. It is the procedure of choice in patients who have completed childbearing and no longer desire fertility, who have a history of ectopic pregnancy in the same tube, or who have severely damaged tubes [114,126].
Treatment failures do occur with laparoscopic procedures [128]. After tubal-sparing surgery, hCG levels should be monitored. A fall in hCG levels of at least 20% every 72 hours is indicative of success [114]. Following surgical treatment of ectopic pregnancy, the elimination of hCG appears to follow a two-phase distribution. The major elimination phase has a half-life of 5 to 9 hours, and the second elimination phase has a 22- to 32-hour half-life [129]. Treatment with methotrexate may be necessary if falling hCG levels do not indicate successful surgical treatment [114,126].
Methotrexate is a folate antagonist that blocks DNA synthesis by inactivating the enzyme dihydrofolate reductase. Its main action is on the cell cycle phase that mediates cell division. Methotrexate was developed as a chemotherapeutic agent but also acts on rapidly dividing cells at the placental implantation site, most notably trophoblast cells [186]. Methotrexate for the treatment of ectopic pregnancy is administered as single or multiple intramuscular injections. Its use has also been successful in the treatment of nontubal ectopic pregnancy [114,126]. Although commonly used in the treatment of ectopic pregnancy, methotrexate does not have FDA approval for this use [39].
Candidates for methotrexate treatment must be hemodynamically stable; patients must also be reliable and able to return for follow-up. Additionally, the gestational age and size are factors in determining the appropriateness of methotrexate use. Relative contraindications include an unruptured mass greater than 3.5 cm in size, fetal heart activity, quantitative hCG levels greater than 6,000–15,000 IU/L, and the presence of fluid in the cul-de-sac [113,114,186]. Absolute contraindications to methotrexate include hypersensitivity or allergy to the drug, immunodeficiency, alcoholism, chronic liver disease, blood dyscrasias (leukopenia, thrombocytopenia, anemia), pulmonary disease, and peptic ulcer disease [39,114]. In addition, patients with intrauterine pregnancy and those who are breastfeeding are also not candidates for methotrexate treatment. Methotrexate, even at low doses, can be fatal in patients with renal insufficiency [39,130].
Sixty percent of patients will experience at least one episode of increased abdominal pain after methotrexate injection [114,126]. This discomfort is believed to be caused by the separation of the placenta from the implantation site and expulsion of the products of conception from the fallopian tube. This pain usually occurs two to seven days after the onset of treatment, is mild, and lasts 24 to 48 hours [113,114]. The presence of pain can be confusing for the patient and the attending healthcare professional. Patients should be taught to expect the discomfort, but to call their providers with severe pain or any questions.
Adverse effects of methotrexate may include nausea and vomiting, diarrhea, gastric upset, dizziness, and occasionally, transient elevations in liver enzymes. The side effects usually abate within three to seven days of therapy being discontinued [39,113,114]. Serious side effects, such as bone marrow suppression, are rare at the doses used to treat ectopic pregnancy. A variable dose regimen has been shown to improve treatment success equal to that of laparoscopic salpingostomy [128]. However, the multiple dosage regimen has fallen out of favor in the United States due to the higher incidence of adverse effects and the increased need for patient motivation and compliance [98]. The more frequently used dosing regimen of methotrexate is a single-dose injection [114]. The efficacy of systemic single-dose methotrexate alone has been shown to be significantly less successful than when combined with mifepristone [128]. Those being treated with methotrexate should be cautioned to avoid alcohol, multivitamins with folic acid, and NSAIDs. Vaginal abstinence is advised until therapy is completed and hCG levels are negative. Exposure to the sun should be avoided due to the increased photosensitivity caused by methotrexate [114].
hCG levels should be observed at four days and seven days after methotrexate injection. An initial increase is not uncommon, peaking three to four days after treatment [114,129]. Four to seven days post-injection, the level should decline by at least 15% [114]. Treatment is considered successful if the hCG level has declined by 15% from day 4 to day 7. However, a second dose may be administered if a 15% drop is not observed, or surgery may be indicated [114,129,186]. With appropriately declining levels at day 7, hCG can be evaluated weekly until negative.
Patients should be counseled on the possible signs and symptoms associated with ruptured ectopic pregnancy, which remains a risk during the course of methotrexate therapy. They should contact their provider immediately upon onset of worsening pain, heavy vaginal bleeding, tachycardia, or syncope [114]. Reliable transportation is crucial. Rupture of ectopic pregnancy during methotrexate treatment is reported to range from 7% to 14%, and the rate of rise in hCG levels is one predictor [186].
Candidates for successful expectant management should be asymptomatic with no evidence of rupture or hemodynamic instability; they also should portray objective evidence of resolution, such as declining hCG levels. They should additionally be fully compliant and willing to accept the risks of tubal rupture [114]. Ectopic pregnancies may resolve on their own. In patients who present with initial hCG levels less than 200 mIU/mL, 88% have experienced spontaneous resolution [114,129]. Falling beta hCG levels less than 1,000 mIU/mL have been followed without medical or surgical intervention in select cases. However, no conclusive data exists to support the expectant management of ectopic pregnancy in clinical practice [113,114].
hCG levels are followed until undetectable, regardless of the mode of treatment. Because the risk of recurrence of tubal pregnancy is high, some providers offer a post-treatment hysterosalpingogram to evaluate tubal patency [126].
During treatment for ectopic pregnancy, it is easy to forget that the family has lost a pregnancy. Patients and their families understand that the diagnosis of ectopic pregnancy can be life-threatening and may not initially focus on the loss. However, the patient and their family may still need assistance with grief, including the possible loss of future fertility.
Gestational trophoblastic disease (GTD) is a heterogeneous group of benign and malignant conditions arising from developmental anomalies and malformations of the placenta [107]. Trophoblasts are specialized cells derived from a normally developing embryo. These cells facilitate implantation of the embryo into the uterus and become components of the placenta that promote normal growth and development of the fetus. During formation of the placenta, there is rapid expansion and differentiation of trophoblast cells into villous cytotrophoblasts and syncytiotrophoblasts, eventually forming an intricate network to anchor the embryonic sac into the endometrium. On rare occasions, when a defective ovum (egg) is fertilized, this intricate developmental process becomes distorted; instead of normal placenta, abnormal growths, or tumors arise from placental villous and extravillous trophoblast cells.
The most common benign form of GTD is hydatidiform mole (complete or partial), so named because diffuse villous enlargement and hydropic change gives the appearance of a "bunch of grapes". Hydatidiform moles are caused by abnormal gametogenesis and fertilization. The incidence varies geographically and is higher in Asia (1 in 500) and Africa (1 in 1,000) than in Europe and North America (1 in 1,500) [107]. A complete hydatidiform molar pregnancy occurs when an empty ovum (egg) is fertilized by one sperm, 90% followed by duplication of paternal chromosomes to a 46XX karyotype. A partial molar pregnancy occurs when an empty egg is fertilized by two sperm, resulting in triploid karyotypes (69XXX, 69XXY, or 69XYY) [107,132,133,134]. Examination of complete molar pregnancies usually shows absence of embryonic sac and an absent or remnant fetal tissue; partial molar pregnancies often contain a nonviable fetus and remnant amniotic sac. GTD is a collective term encompassing complete hydatidiform molar pregnancy, partial hydatidiform molar pregnancy, and placental site trophoblastic disease [135]. The incidence of GTD is about 1 in 1,500 to 1 in 2,000 pregnancies [131,136].
While the hydatidiform mole is usually a benign condition, it does have the potential to develop into a malignant choriocarcinoma [136]. The risk of developing choriocarcinoma is 20% following a complete molar pregnancy, with a lower risk after a partial molar pregnancy [137,138]. Clinical risk factors that appear to increase the probability of persistent GTD include delayed hemorrhage after a pregnancy immediately preceding the current one, excessive uterine enlargement, theca-lutein cysts, hCG levels greater than 100,000 mIU/mL, prior molar pregnancy, prior miscarriage, blood type A or AB, use of birth control pills, and maternal age older than 40 years and younger than 20 years. The risk is highest for patients older than 50 years; recurrence rates are 1% to 2% [137,138]. Twin gestations involving a complete molar pregnancy and a normal fetus are rare [132,133].
Signs and symptoms that may indicate a diagnosis of GTD include vaginal bleeding, unusual uterine growth rate, absence of usual fetal indications, hyperemesis, hyperthyroidism, pre-eclampsia, anemia, and enlarged ovaries [138].
Almost all patients with GTD will have irregular or intermittent bleeding. The bleeding generally starts during the first trimester and is often spotty, watery, and brown, with some reporting passing mucinous, honeycomb-like structures [138].
The growth rate of the uterus may appear out of proportion to the size expected based on gestational age. This is more often seen with a complete molar pregnancy. Abnormal uterine enlargement occurs in approximately one out of four patients with complete hydatidiform molar pregnancies; it occurs rarely in those with partial molar pregnancies [138].
The absence of usual fetal indications may support a diagnosis of GTD [136]. Ultrasound examination should be ordered if fetal heart tones are absent, no fetal movement is detected by 20 to 24 weeks, or a fetus cannot be palpated through the uterine wall [139].
Many patients are bothered by nausea and vomiting in pregnancy. Those with GTD may experience severe vomiting [136,138]. Left untreated, these patients will become dehydrated and suffer weight loss [137]. Consequently, ultrasound examination is generally appropriate for those experiencing hyperemesis in order to rule out GTD.
Transient hyperthyroidism may be caused by partial and complete hydatidiform moles and choriocarcinoma. Patients may present with varying degrees of symptoms, including congestive heart failure [137].
Pre-eclampsia is a pregnancy complication characterized by hypertension usually seen in the third trimester [138]. Elevations in blood pressure or proteinuria prior to 24 weeks' gestation should trigger a complete evaluation to rule out GTD. Pre-eclampsia affects about 25% of those with complete molar pregnancies [138].
About 50% of those with molar pregnancies will develop anemia due to the chronic small blood losses. The anemia may be accompanied by fatigue, dyspnea, or exercise intolerance [138].
Enlarged ovaries may be palpated or seen on ultrasound examination. Ovarian cysts known as theca luteal cysts result from the abnormally high hCG levels. Ovarian size may exceed 6 cm in diameter [135]. Enlargement regresses spontaneously several weeks after evacuation of the molar pregnancy and rarely requires surgery [131].
Most patients with GTD are diagnosed due to the use of blood tests and ultrasound early in pregnancy [138]. Diagnosis of GTD is most often made with ultrasound. Hydatidiform molar pregnancies have a characteristic structural pattern and size on ultrasound examination. In partial molar pregnancies, fetal tissue may be seen but the appearance of the placenta shows diagnostic features of GTD [135]. Occasionally, imaging abnormalities such as hydropic villi, retroplacental hematomas, chorioangiomas of the placenta, degenerative uterine fibroids, and aborted tissue will lead to confusion about the diagnosis [137].
The ultrasound diagnosis of a partial molar pregnancy is complex. The finding of multiple soft markers (e.g., cystic spaces in the placenta) is required for a reliable diagnosis of a partial molar pregnancy. Estimation of hCG levels may be of value. When diagnostic doubt exists about the possibility of a combined molar pregnancy with a viable fetus, then ultrasound examination should be repeated before intervention. In the situation of a twin pregnancy, where there is one viable fetus and the other pregnancy is molar, the pregnancy should be allowed to proceed if the patient wishes, following appropriate counseling [140].
GTD releases more hCG than normal pregnancies, most likely due to larger volume of the placental structure, and the hCG levels rise more quickly than usually seen in normal gestations [138]. However, the same may be true of multiple gestations, and not all patients with GTD have hCG levels that are higher than those seen in a normal pregnancy. Laboratory testing is generally more useful during treatment and follow-up of GTD than during diagnosis [138].
Treatment of GTD depends on many factors, including the location and extent of the disease, the type of GTD present, the level of hCG, the duration of the disease, sites of metastasis if any, and the extent of prior treatment [138]. Referral to a specialist able to adequately manage and follow-up GTD should be immediate. Suction curettage is the method of choice of evacuation for complete molar pregnancies. Medical termination of complete molar pregnancies, including cervical preparation prior to suction evacuation, should be avoided where possible [140]. Suction curettage often is the choice for patients who may want to have children in the future [138]. Data from the management of molar pregnancies with mifepristone are limited. Evacuation of complete molar pregnancies with this agent should be avoided because it increases the sensitivity of the uterus to prostaglandins [140].
Tissue should be sent to the pathology lab for final diagnosis and confirmation of GTD. Because of the difficulty in making a diagnosis of a molar pregnancy before evacuation, the laboratory assessment is recommended in order to exclude trophoblastic neoplasia [140]. If an older patient requests sterilization, hysterectomy may be considered [137,138]. Following evacuation of the uterus, hCG levels are recorded at 48 hours and on days 7, 14, and 21 [135]. When hCG levels are no longer elevated, values are obtained at monthly intervals for at least six months. Treatment with methotrexate is not indicated unless the hCG levels continue to rise or remain elevated.
A chest x-ray may be performed as a post-treatment baseline to determine if GTD has spread to the lungs [141]. In some cases, other imaging studies may follow. If GTD is suspected before D&C, a chest x-ray should be performed prior to uterine evacuation [141]. Pelvic ultrasound is performed to identify the presence of theca-lutein cysts [137]. A complete blood count with platelet count and clotting factors, renal and liver function tests, blood type and antibody screen, and hCG level are obtained prior to uterine evacuation in suspected GTD.
Patients are strongly encouraged not to conceive for at least one year after treatment [141]. A pregnancy sooner than one year after treatment will mask any rises in hCG caused by persistent GTD and may delay treatment. An effective contraceptive method should be provided [135].
Blood type, Rh type, and antibody screen are typically ordered. Threatened abortions, ectopic pregnancies, and hydatidiform moles all have risks of fetomaternal hemorrhage and, therefore, can cause RhD alloimmunization [76]. Because the differentiation of partial and complete molar pregnancy may be delayed, it seems reasonable to offer RhoGAM to those with suspected molar pregnancy [76].
Patients and their families will require education, including that a partial molar pregnancy means that normal fetal development and viability are not possible when two sperm fertilize one egg, resulting in severe chromosomal abnormalities. Nevertheless, grief support is an important part of the follow-up of this condition. The fear of carcinoma may delay a patient's reaction to the fact that a pregnancy was lost. Attention should be given to the family's grief. In cases of partial hydatidiform molar pregnancies, the grief may be compounded by the somewhat elective decision to terminate a fetus, even one whose chromosomes are not compatible with life. Follow-up and referrals are appropriate.
Placenta previa occurs when the position of the placenta is such that it covers the cervical os, either partially or completely. The placenta normally implants in the upper uterine segment, but infrequently it may implant elsewhere in the uterus [142]. Placenta previa is one of the leading causes of vaginal bleeding in the second and third trimesters [143]. It occurs in approximately 1 of every 200 pregnancies and is more common in multiparous patients, occurring in as many as 1 in 20 grand multiparous individuals [143,144,145]. Data recorded between 1989 and 1997 have indicated that placenta previa complicated 2.8 per 1,000 live births in the United States, with a mortality rate of 0.03% [143]. The significance of race remains controversial [143].
Three types of placentae previa have traditionally been recognized [142,143,144,145,146]:
Complete (total) placenta previa: The placenta completely covers the cervical os. This occurs in 20% to 43% of previa presentations.
Partial placenta previa: The placenta only partially covers the cervical os. This accounts for approximately 31% of previa presentations.
Marginal placenta previa: An edge of the placenta is at the margin of the cervical os but does not cover any of it. Patients with a placenta edge at least 2 cm from the internal os most often deliver vaginally without complication. However, those with a placental edge less than 1 cm from the cervical os tend to have cesarean sections because they are more likely to present with symptoms of bleeding.
Because the differences between partial and marginal are subtle and vary according to the timing and method of diagnosis, contemporary classification of placenta previa consists of two variations: placenta previa (i.e., the cervical os is covered by placental tissue) and marginal placenta previa (i.e., the placenta lies within 2–3 cm of the cervical os but does not cover it) [145]. Providers may also see the term "low-lying placenta" on ultrasound reports. Ultrasonographers and radiologists diagnose the presence of a low placenta when the placenta extends into the lower uterine segment but does not reach the internal os [142,146]. Most often, these placentas cause no obstetric complications. The definitive diagnosis of most low-lying placentas is achieved with ultrasound [147]. Depending on the gestational age at which it is originally identified, a low-lying placenta may be monitored with a follow-up ultrasound later in pregnancy.
The risk factors that are associated with placenta previa include maternal age older than 35 years, African American or other minority races, increased gravidity and parity, prior uterine surgery or cesarean section, prior induced abortion, cigarette smoking, large placenta, multiple gestation, and a prior history of placenta previa [142,145,146]. Some reports have additionally documented a higher association of fetal malpresentation, preterm premature rupture of membranes, and intrauterine growth restriction with placenta previa [145]. The exact pathophysiology is unknown, although placenta previa has been associated with scarring in the endometrium, presumably decreasing the surface area available for placental implantation [143,144,146].
Because the placenta is vascular, any stretching or pulling of the structure can cause blood vessels to rupture and bleed. The lower part of the uterus and upper part of the cervix (isthmus) thins and "pulls up" during the last trimester and while in labor. Bleeding is thought to occur as a result of the changes in the lower uterine segment in the third trimester [145,146]. The first bleeding typically occurs at 27 to 32 weeks' gestation [143]. Approximately 25% of patients do not bleed until 36 weeks' gestation [144]. Those with complete placenta previa are more likely to experience bleeding earlier than those with marginal or partial placenta previa. Bright red, painless bleeding during the third trimester in a patient not in labor must be evaluated for placenta previa. The bleeding may be minimal; however, at times it can present as hemorrhage. Some patients with placenta previa will also have uterine irritability accompanying the bleeding. Spotting may occur for several days and then taper off, but it almost always returns after a few days [143,146].
In those with undiagnosed placenta previa close to term, it may be noted that the fetus does not "drop" into the pelvis as expected because of the presence of the placenta blocking the inlet. Fetal malpresentation may also be noted.
Prior to the availability of ultrasound, placenta previa was diagnosed with a very careful and gentle speculum exam and/or a digital exam. Technologic advances have made it unnecessary and inadvisable to perform a pelvic examination on a patient with vaginal bleeding after the point of fetal viability without first obtaining an ultrasound exam. The diagnosis of placenta previa is easily made by ultrasound in the third trimester of pregnancy, and both careful transvaginal and translabial scanning have shown sensitivity in diagnosing placenta previa [145]. Transabdominal ultrasound has an accuracy of 93% to 98%, although false-positive results may occur secondary to focal uterine contractions or bladder distention [143]. Because transvaginal scanning does not increase the risk of bleeding, it is the imaging modality of choice [142]. Studies have indicated that it is safer and more accurate than the transabdominal method [142,143,145,147,148]. Transperineal ultrasonography has been suggested as an alternate method, particularly if instrumentation of the vaginal canal with a probe is a concern. This method may compliment transabdominal ultrasonography and help eliminate the false-positive results [143].
Placenta previa is often misdiagnosed early in pregnancy. The myth of the "migrating placenta" developed because, early in pregnancy, low-lying placentas are not uncommon. The placenta does not move or migrate in pregnancy. As pregnancy advances, the uterine wall stretches and thins. It is also thought that the placenta grows preferentially toward the fundus and moves farther away from the cervical os as the uterus enlarges [142,146]. Ninety percent of patients who have placenta previa diagnosed in the first trimester will not have a placenta previa at term [145,149]. Of those with second trimester ultrasound diagnosis of total placenta previa, only 26% will have persistent placenta previa at term; only 2.5% of partial and marginal placenta previa diagnosed during the second trimester will remain at term [145].
The treatment of placenta previa depends on a number of factors, including the amount of vaginal bleeding, whether the bleeding has stopped, the fetus's gestational age, the patient's health, the fetus's health, and the position of the placenta and the fetus [146]. If hemorrhage is life-threatening, immediate delivery by cesarean section is indicated. If the bleeding is slight, the patient may be sent home after 48 hours of in-house observation or kept in the hospital for the remainder of the pregnancy. Home-based care should occur only if the patient is in close proximity to a hospital, has the constant presence of a companion, and has given fully informed consent for such care [147,148]. Patients who do not have access to emergency transportation should be kept hospitalized. Bed rest may be prescribed to prevent uterine contractions that can result in bleeding [143,146]. Although there is no data to support the practice, pelvic precautions are often prescribed, including avoidance of vaginal intercourse, insertion of items into the vagina, and orgasm, which might result in uterine contractions [143,146]. Patients are otherwise allowed their usual activities, without any excessive exertion [144].
Depending on the amount of bleeding, IV fluids should be started and the patient should be blood typed and screened for crossmatch [143]. Few antepartum patients require emergency transfusions [144]. Baseline CBC, hemoglobin, hematocrit, and platelet functions must be obtained. Increases in blood volume and the hemodynamic changes in pregnancy mask early hypovolemic symptoms. Significant hemorrhage may occur by the time changes are noted in the vital signs. In the absence of massive bleeding or other complications, coagulation studies are not necessary [142].
Timing of delivery is based on gestational age and the severity of the bleeding. In most situations, an elective cesarean section will be scheduled prior to the due date [146]. Some patients with partial or marginal placenta previa can deliver vaginally because the fetal head will descend and act as a tamponade. In some cases, massive hemorrhage prompts delivery [146]. Usually, the blood is maternal and the fetus is not in jeopardy as long as the patient is stabilized [144]. Fetal status should be documented, and electronic fetal monitoring, when available, should be initiated. When the patient and fetus are stable, the use of tocolytics, medications used to inhibit labor, in those with placenta previa has been described. Steroids may be administered between 24 and 34 weeks' gestation to promote fetal lung maturity if delivery is imminent [142,146].
Whenever bleeding occurs in pregnancy, blood type, Rh type, and antibody screen should be reviewed, and all Rh-negative patients should be offered RhoGAM. A Kleihauer-Betke test, which measures fetal hemoglobin transferred to the patient's bloodstream, should be performed to determine if significant fetomaternal hemorrhage has occurred [143,145]. RhoGAM doses are calculated based on the amount of hemorrhage identified.
Patients with placenta previa and their families must be educated to contact their provider immediately if any bleeding occurs, even light spotting.
Obviously, maternal hemorrhage is the most common and life-threatening complication of placenta previa [144]. Anemia and shock may follow. Placenta previa has been associated with intrauterine growth restriction. However, when controlled for gestational age, studies have not found an association between placenta previa and low birth weight [144].
Preterm labor and birth may accompany placenta previa [146]. In about 20% of placenta previa cases, the uterus contracts prematurely [144]. Efforts to arrest preterm labor may be undertaken, and in the third trimester, antenatal steroids may be indicated [144]. Other complications include a prolonged hospital stay, intrapartum hemorrhage, septicemia, thrombophlebitis, cesarean delivery, abruptio placenta, fetal malpresentation, maternal death, DIC, blood transfusion, and hysterectomy [142,144].
Placenta accreta, placenta increta, and placenta percreta are also complications of placenta previa [146]. Placenta accreta refers to the abnormal attachment of the placenta to the myometrium. Placenta accreta spectrum is becoming increasingly common and is associated with significant morbidity and mortality [180]. Placenta increta is seen when the villi invade the myometrium, and placenta percreta is diagnosed when the villi penetrate the uterine wall and extend into the bladder or rectum [144]. Although not completely accurate, practitioners often use the term "placenta accreta" to describe all three situations.
Prior cesarean section or other uterine surgeries are most often associated with placenta accreta [145,147,148]. The placenta accreta rate has increased over the past 50 years, most likely as a result of the increasing cesarean section rates [142,150]. The incidence is now estimated to be 1 in 2,500 deliveries. Ultrasound may be helpful in the prenatal diagnosis of placenta accreta. Magnetic resonance imaging (MRI) and color Doppler studies may also be useful, although MRI is not the preferred recommended modality for initial evaluation [142,143,146,147,150]. The average blood loss recorded at the time of delivery in those with placenta accreta is 3,000–5,000 mL and is a common cause of cesarean hysterectomy [142]. Prenatal diagnosis by imaging, followed by planned, multidisciplinary peripartum management may help reduce morbidity and mortality [142,151,152]. Scheduled cesarean hysterectomy with preoperative ureteric stent placement and avoiding attempted placental removal have been associated with reduced maternal morbidity in those with suspected placenta accreta [153].
Other rare conditions often grouped with placenta previa include placental abruption and vasa previa [146]. Placental abruption occurs when the placenta separates from the uterus before birth, potentially depriving the baby of oxygen and nutrients and resulting in dangerous bleeding [146]. Vasa previa occurs when the fetal blood vessels, unsupported by the placenta or umbilical cord, extend across the lower uterine segment and/or cervical os. These may accompany a velamentous cord insertion or a succenturiate lobed placenta [144]. Velamentous cord insertions occur when the umbilical cord does not insert directly into the placenta itself. The vessels are supported only by membranes between the umbilical cord and the placenta. Because fetal blood volume is only 80 to 100 mL/kg, laceration of the fetal vessels will cause hemorrhage and rapid fetal death [142,145,146]. Risk factors for vasa previa include a bilobed or succenturiate lobed placenta, low-lying placenta, multiple gestation, marginal insertion of the umbilical cord into the placenta, and velamentous cord insertion [144].
The incidence rate of vasa previa ranges from 1 in 2,000 to 1 in 6,000 pregnancies [154]. Diagnosis is often made at the time of presentation or rupture of membranes. With ultrasound, diagnosis of bilobed placentas or velamentous or marginal cord insertions can be seen, and the patients at high risk for vasa previa can be identified [142,154]. If vasa previa is suspected, transvaginal ultrasound color Doppler may be used to facilitate the diagnosis; however, even with the use of transvaginal ultrasound color Doppler, vasa previa may be missed. When vasa previa is diagnosed prenatally, an elective cesarean delivery should be offered prior to the onset of labor. Because premature delivery is likely, consideration should be given to administration of corticosteroids at 28 to 32 weeks to promote fetal lung maturation and to hospitalization at about 30 to 32 weeks [154]. When the diagnosis of vasa previa is made prenatally, more than 96% of fetuses survive. Nearly 45% of infants die when the diagnosis is made at the time of labor [154].
When bleeding occurs during pregnancy or in labor, the Apt or Kleihauer-Betke test may be used to determine if fetal cells are present in the vaginal blood to assist in diagnosis [142,143]. If vasa previa is diagnosed antenatally, hospitalization of the patient at about 30 to 32 weeks is considered and steroids administered to promote fetal lung maturity. Amniocentesis is often performed to determine fetal lung maturity before elective delivery. In cases of antenatally diagnosed vasa previa, the obstetrician may choose to deliver at 35 to 36 weeks' gestation without amniocentesis to avoid the potential for laceration of the fetal vessels [142].
Abruptio placenta is the premature separation of a normally implanted placenta from the uterine wall. Hemorrhage can be concealed or obvious. Placental abruption complicates an estimated 1 in 75 to 1 in 226 deliveries [145]. Eighty percent of cases of abruptio placenta occur before the onset of labor [145]. Placenta abruption is one of the leading causes of fetal and neonatal mortality [144].
There are three recognized grades of placenta abruption [145]:
Grade 1: A small amount of vaginal bleeding is present with some uterine irritability. Maternal blood pressure is normal. Fetal status is normal. Grade 1 placenta abruptions account for 40% of all abruptions.
Grade 2: External uterine bleeding is mild to moderate. The uterus may be irritable or tetanic. Maternal blood pressure is normal, but pulse rate may be increased. The fetal heart rate may show signs of compromise. Grade 2 abruptions represent 45% of all abruptions.
Grade 3: Bleeding is moderate to severe but may be concealed. The uterus is tetanic and painful. Maternal hypotension is present, and fetal death may have occurred. Coagulation abnormalities may be present. Grade 3 abruptions account for 15% of all abruptions.
The locations of placental abruptions may vary. Retroplacental abruptions occur between the placenta and the myometrium. They are often large and can quickly result in fetal death [145]. A subchorionic placenta abruption occurs between the placenta and the membranes, and a subamniotic abruption occurs between the placenta and the amniotic fluid. These have little clinical significance [144]. The majority of abruptions (80%) occur before the onset of labor [145].
While the exact causes of placenta abruption are unknown, some factors have been associated with their occurrence. These factors include [144,145]:
Grand multiparity
Pregnancy-induced hypertension or pre-eclampsia
Chronic hypertension (>140/90 mm Hg)
Premature rupture of membranes
Pregestational diabetes
Substance abuse, particularly cocaine use
Hydramnios
Blunt force trauma, such as motor vehicle accidents and maternal battering
Smoking
Uterine fibroids
Multiple gestations (distension of the uterus, rapid decompression of the uterus with the delivery of the first infant)
Extremes of maternal age
Vascular abnormalities in the placenta bed
History of placenta abruption (recurrence rates are 5% to 17%); if the abruption was severe enough to result in fetal death, the recurrence rates of placenta abruption again resulting in fetal demise is 11%
Uterine anomalies
Thrombophilias, such as factor V Leiden mutations
Sudden decompression of the uterus, such as with amniocentesis
Circumvallate placenta. A circumvallate placenta is an unusually shaped placenta. It is abnormally thickened with a smaller surface area over the uterine wall. Because the membranes do not insert at the edge of the placenta, there are villi left uncovered by the membranes, resulting in bleeding and increasing the possibility of placenta abruption as well as other complications.
Absolute diagnosis of placenta abruption can only occur after examination of the placenta reveals an adherent clot or loss of functioning placental tissue. This diagnosis may not be accurate if the abruption is recent. Diagnosis is usually based on clinical findings, with supportive evidence from sonographic, laboratory, and pathologic studies [145].
Although vaginal bleeding is the hallmark sign of placental abruption, 10% to 20% of affected patients may have occult or concealed hemorrhage [145]. Other clinical findings include uterine bleeding, abdominal pain, uterine contractions, uterine tenderness, concerning fetal heart rate patterns or fetal death, and DIC [145,155]. The signs and symptoms of placenta abruption depend on the location of the placenta and the degree of separation involved. Abruption of a placenta implanted on the posterior uterine wall may present with severe back pain and contractions [156].
A patient's perception of pain may seem out of proportion to what the provider observes. There is increased uterine tone between contractions; the uterus may never completely relax between contractions. The classic "board-like" description of the abdominal wall will occur with complete or significant abruptions, but not with marginal or small abruptions.
Bleeding may be obvious or absent, although nearly 80% of patients with placenta abruption will exhibit external bleeding [144]. Patients with concealed abruption are often given the diagnosis of preterm labor. Bleeding may occur into the uterine wall, resulting in uterine enlargement. Uterine contractions and tenderness may be seen [144]. The uterine muscle may be saturated with blood, resulting in a Couvelaire uterus. Couvelaire uterus is seldom seen, but the appearance is that of a blue-tinted uterus at the time of cesarean section [144].
With significant abruption, fetal distress may be apparent on electronic fetal monitor tracings. The fetus will tolerate some loss of placental surface area without distress; however, large interruptions in blood flow will be evident on the fetal heart rate monitor.
Often, placenta abruption is a diagnosis of exclusion. If placenta previa and other causes of vaginal bleeding have been ruled out, placenta abruption becomes the most likely diagnosis [145]. Ultrasound imaging may be useful in only about 50% of placenta abruptions, and false-positive diagnoses have been reported [144,145]. Serum markers for the early identification of placenta abruption have been under investigation [157,158,159]. Possible markers include hCG, maternal serum alpha fetoprotein (MSAFP), and inhibin A. Elevated levels of MSAFP have been associated with a ten-fold increase of placenta abruption [144]. The Kleihauer-Betke test has not proven to be useful to detect placenta abruption [144].
Maternal hemorrhage is the most common and life-threatening complication of placenta abruption, accounting for 6% of all maternal mortality [145]. Fetal mortality has been reported to be as high as 25% to 30% [145]. Significant neonatal mortality and morbidity is due to premature birth.
Other complications include a prolonged hospital stay, cesarean delivery, blood transfusions, and hysterectomy. Severe placenta abruption stimulates the clotting cascade that can result in DIC [144].
The majority of abruptions are marginal, and patients are usually hemodynamically stable on presentation. However, after the diagnosis of placenta abruption has been made, immediate referral to a physician able to manage the problem is indicated. A large-bore IV catheter should be placed to assure intravenous access. An indwelling Foley catheter will permit assessment of maternal urine output. If bleeding is significant, typing and crossmatch for blood transfusion should be ordered [144,145]. Routine laboratory studies include hemoglobin, hematocrit, WBC, and platelet count. Coagulation studies are advisable, to include prothrombin time (PT), partial thromboplastin time (PTT), fibrinogen degradation product, and fibrinogen level should be drawn if significant blood loss is present [144]. A red-topped laboratory tube (i.e., clot tube) can be used to quickly assess bleeding defects. The blood drawn into the tube should form a clot within six minutes. The clot should lyse within 30 minutes. If clotting and lysing do not occur, a coagulation defect has probably occurred [145]. Continuous monitoring of fetal status and uterine activity has been recommended [144].
Timing of delivery is dependent on the degree of separation and maternal or fetal status. With grade 1 abruption, close observation of maternal and fetal status is essential. When the fetus is mature, a controlled induction of labor can be pursued [145]. In patients remote from term and clinically stable, the use of tocolytic agents to inhibit contractions has been described [145]. Unfortunately, a small placenta abruption can stimulate uterine irritability, which causes the placenta to separate further. While bleeding was once considered to be a contraindication to tocolytics, it has become more acceptable to consider a short course of tocolytics in patients with mild bleeding and contractions. If the patient is stable and fetal well-being is established, tocolysis may be valuable to prolong pregnancy 48 hours in order to initiate antenatal steroids for fetal lung maturation. Magnesium sulfate is the most accepted agent for this purpose, although use as a labor tocolytic is off-label for this medication and controversial [144,160]. Evidence of fetal distress can prompt immediate cesarean section. Sixty percent of fetuses will become distressed in labor; continuous electronic fetal monitoring is associated with excellent fetal survival in these cases [145]. The cesarean rate associated with placenta abruption has been reported as 50% to 75% [145].
Patients with mild bleeding may be sent home after evaluation. The decision to send any patient home after a bleeding episode will depend on the help the patient has at home, distance to hospital, ability to comply with medical instructions, and prompt access to transportation [144]. Patients with an abruption should be counseled about the increased risk of recurrence (estimated at about 25%) and associated risk factors [144].
Other causes of apparent bleeding during pregnancy should also be considered. The bleeding may be from the cervix, the vaginal structures, the rectum, or urologic sources.
The vascular changes that occur in the cervix during pregnancy, such as hyperemia and an altered squamous epithelium, predispose individuals to bleeding following intercourse. Inquiry regarding recent sexual activity, evaluation of the cervix, and reassurances about the status of the pregnancy may be all that is required in these cases.
Cervical infections such as chlamydia and gonorrhea may result in cervical bleeding. Cultures should be obtained whenever a patient presents with unexplained vaginal bleeding in pregnancy. If cervicitis is diagnosed, the Centers for Disease Control and Prevention (CDC) protocols for the treatment of STIs in pregnancy should be followed [161].
Another possible cause of cervical bleeding is cervical polyps. Cervical polyps occur in about 2% to 5% of persons with cervices [162]. If cervical polyps are discovered in pregnancy, they should not be removed because significant blood loss could result. The patient must be reassured that bleeding may recur from cervical polyps and that any heavy bleeding should still be reported to a provider. Evaluation by a provider able to distinguish normal cervical polyps from potential pathologic cervical disorders should be made [162,163].
Evaluation for lower genital tract malignancy should be considered whenever one encounters vaginal bleeding. Overall, 1 of every 34 persons diagnosed with cervical cancer is pregnant [164]. Although cervical cancer is a rare complication of pregnancy, it remains the most common gynecologic malignancy associated with pregnancy [137,165]. While the incidence of cervical cancer has decreased worldwide, largely due to screening in Westernized societies, the mean age of diagnosis of cervical cancer is 50 years of age [166,167]. The most common complaint of pregnant patients with cervical cancer is bleeding [164]. In general, increases in vaginal discharge and bleeding are the most common symptoms reported with this malignancy. More advanced cancers may be accompanied by malodorous, serosanguineous, or yellow discharge [164]. However, many with cervical cancer are asymptomatic, and diagnosis is made on routine screening [166]. Pelvic pain is less common. Pap tests should be done if any suspicion of cervical pathology exists. False-negative cervical cytology is possible due to the increased mucus and bleeding from cervical eversion in pregnancy. Biopsy by a physician skilled in the procedure may be indicated in ulcerative lesions. If a Pap test is not performed in an urgent care facility or emergency room, the patient should be specifically told it was not obtained. Many arrive in their primary providers' offices assuming that if a speculum examination was conducted, a Pap test was obtained.
Cervical eversion or erosion may present with vaginal bleeding. Cervical eversion is identified by the presence of an irregularly shaped area of reddened, raw tissue around the cervical os. The superficial layers of the squamous epithelium are lost. Cervical eversion can be caused by chronic cervicitis, pregnancy, tampon use, intercourse, and a variety of other triggers [168].
The onset of labor at term, prematurely, or in the event of an insufficient cervical os may be heralded by vaginal bleeding. Bloody show can be frank red, pink, or brown. It may be described as mucousy or watery. The bleeding may be first noticed following cervical examination at term. After placenta previa has been ruled out, perhaps by the availability of a previous ultrasound study, a careful, gentle digital examination of the cervix can confirm labor as the cause of bleeding. In gestations remote from term, when digital exams are not routinely advised, speculum exam or ultrasound may also diagnose cervical dilatation.
Vaginal causes of bleeding that should be evaluated include vaginitis, which may cause excoriation and therefore bleeding, vaginal trauma or laceration, or vulvovaginal cancer. The amount of bleeding and patient discomfort may make assessment of vaginal trauma difficult. Appropriate management and help with visualization are necessary. Although rare, vulvar and vaginal cancers do sometimes occur in persons of childbearing age [169]. It has been suggested that there are two subtypes of vulvar cancer: one that is associated with human papillomavirus (HPV) and one that is not [170]. Genital warts increase the risk of vulvar and cervical cancer and may be a source of bleeding in pregnancy. Nearly 90% of vulvar cancers in younger individuals have been associated with HPV [169]. Vulvar cancers represent approximately 6% to 7% of all gynecologic cancers in the United States [171]. Most are squamous cell carcinoma; melanoma and basal cell carcinoma are less common [169,170]. Fewer than 20 cases of vulvar carcinoma during pregnancy have been reported in the medical literature [137]. Most patients with vulvar cancer present with burning, itching, bleeding, or pain in the vulva. Visual lesions are usually available to biopsy. Referral to the appropriate specialist should be made whenever vulvar or vaginal pathology is suspected [171].
Vaginal infections are another possible cause of bleeding during pregnancy. Infections such as candidiasis, trichomoniasis, and bacterial vaginosis may cause tissue damage significant enough to result in vaginal bleeding during pregnancy. Microscopic evaluation of vaginal discharge and pH testing can quickly diagnose infections that should be treated. Initial herpes infections may result in bleeding from vesicles that have been scratched or from attempted home treatments. Visible lesions should be cultured for herpes simplex virus, and open sores should alert the clinician to the need for additional testing for syphilis and other STIs. As noted, all STIs diagnosed during pregnancy should be treated according to CDC guidelines [161]. Vaginitis treatments are also appropriate during pregnancy.
Careful examination of the anus and rectum should reveal any evidence of genital warts, hemorrhoids, fissures or rectal polyps, ruptured rectal varicosities, or trauma as sources of bleeding. Bleeding from sources higher in the colon, such as Crohn disease, irritable bowel syndrome, and colorectal cancer, are rare but may be appropriately evaluated during pregnancy. The majority of colorectal cancer in pregnancy is rectal and can be palpated on rectal exam. The incidence of colon cancer during pregnancy is about 1 in 13,000 [137].
Severe lower urinary tract infections, such as cystitis and urethritis, may result in the presence of significant blood in the urine. Because asymptomatic bacteriuria is a common risk factor for subsequent pyelonephritis, any evidence of this condition must be attended to. Individuals in advanced pregnancy may not be able to provide a sufficient clean catch urine specimen, and the need for catheterization should be weighed against the risks. Acute pyelonephritis occurs in 1% to 2% of all pregnancies and may result in maternal morbidity and mortality [172,173]. Most pyelonephritis occurs during the second or third trimesters and is believed to be the result of increasing obstruction of the ureters and stasis caused by the pregnant uterus.
Renal stones complicate 0.1% to 0.3% of pregnancies [174]. Urolithiasis is usually accompanied by colicky abdominal pain, recurrent urinary tract infections, and hematuria [174]. Although it is not a frequent cause of noticeable blood in pregnancy, it should be considered. Treatment is conservative, consisting of pain management and hydration [174]. Lithotripsy is contraindicated in pregnancy [175]. Urinary tract cancers are rare during pregnancy.
Another unusual cause of bleeding in pregnancy is the dehiscence of a cesarean section scar. Bloodless, asymptomatic dehiscence of the cesarean section scar usually carries little or no adverse impact on the pregnancy. However, uterine rupture can be life-threatening and may occur in the absence of labor. The incidence of uterine rupture is difficult to determine and is influenced by the type and location of the previous incision, obstetric history, interval between pregnancies, and the type of closure of the hysterotomy incision at the time of primary cesarean section [176,177]. Signs of uterine rupture may include fetal distress, maternal shock, vaginal bleeding, and abdominal or uterine pain [177]. Providers suspicious of uterine rupture should stabilize the patient and immediately transfer to a surgeon who is capable of performing an emergency cesarean section and dealing with the consequences of such an obstetric catastrophe.
In a few cases, the cause of antepartum bleeding cannot be determined. Careful monitoring of the fetus and patient can result in a healthy pregnancy outcome.
Because diagnosing the cause of bleeding during pregnancy is often dependent on a detailed patient history, and successful treatment relies on patient understanding and compliance with recommended plans, effective communication is an essential aspect of managing the patient who is bleeding during pregnancy. The general population of the United States is diverse and becoming more so. Therefore, adjustments should be made for patients who are not proficient in spoken and/or written English. When there is an obvious disconnect in the communication process between the practitioner and patient, an interpreter is required.
In this multicultural landscape, interpreters are a valuable resource to help bridge the communication and cultural gap between patients and practitioners. Interpreters are more than passive agents who translate and transmit information back and forth from party to party. When they are enlisted and treated as part of the interdisciplinary clinical team, interpreters serve as cultural brokers who ultimately enhance the clinical encounter. When providing care for patients for whom English is a second language, consideration of the use of an interpreter and/or patient education materials in their native language may improve patient understanding and outcomes.
Patient A is a woman, 24 years of age, gravida three para two, who reported she believes she is about seven weeks pregnant. Three days previous, she noted some pink vaginal spotting. She presented with painless, dark red vaginal spotting. Patient A reported her last intercourse was more than a week ago. She denied any itching, burning, or malodorous discharge prior to the onset of her symptoms. She denied fever but thinks she had been having chills. Some nausea was reported but no vomiting. She did have a positive home pregnancy test one month ago. She denied uterine cramping, but admitted to some mild upper abdominal cramping. The patient complained of suprapubic pain after urination. The pain occurred after each voiding. The pain did not localize elsewhere and lasted for just a few minutes. Patient A reported some frequency, but attributed this to her pregnancy. Bowel function has been normal. She was appropriately concerned, as her previous pregnancies were uncomplicated. During the previous six months, Patient A has been diagnosed and treated for gonorrhea once and chlamydia twice. Follow-up testing was negative. Patient A has also been treated for recurrent lower urinary tract infection and bacterial vaginosis during the same period of time.
The differential diagnosis for Patient A includes:
Urinary tract infection
Lower genital tract infection
Threatened abortion
Ectopic pregnancy
Normal pregnancy
Examination revealed normal external genitalia. The vagina was pink with moderate amounts of maroon-colored watery discharge noted. The cervix was pink and appeared closed. No exudate or lesions were noted on the cervix. Cultures for gonorrhea and chlamydia were obtained. Bimanual examination revealed a nontender uterus, anteverted, enlarged to a six- to seven-week gestational size. No masses were appreciated. The uterus was normal shape and configuration. The cervix was long and closed. Cervical motion tenderness was absent. Adnexa were slightly tender to palpation, without mass. Rectal examination was confirmatory.
Urinalysis in the office revealed 10 to 20 WBCs per high-powered field, 20 to 30 RBCs, no bacteria, moderate epithelial cells, and some casts. A urine sample was forwarded to the lab for culture and sensitivity. The routine pregnancy laboratory tests were obtained, and an ultrasound exam was ordered.
Laboratory findings revealed that Patient A is Rh negative with a negative antibody screen. She was offered RhoGAM per protocol and accepted. Her hemoglobin was 12.4, with the remainder of her lab work within normal limits. Her quantitative beta hCG was 14,283 mIU/mL. With an hCG that high, one would expect to be able to identify a fetus or products of conception on ultrasound. The radiologist immediately called to report that Patient A's ultrasound demonstrated a thickened endometrium and a slightly enlarged uterus measuring 9 cm x 6 cm x 8 cm. No gestational sac was noted. The left adnexa revealed a significantly increased vascularity adjacent to the left ovary. The right ovary was normal, with several small follicles.
Ectopic pregnancy was suspected. The hCG levels were borderline for the administration of methotrexate. With the uncertainty of the location of the gestation and the question of the patient's ability to return for close follow-up, the patient was prepared for surgery. At the time of diagnostic laparoscopy, a 4 cm x 5 cm cornual pregnancy was noted on the left side. The tubes and ovaries were normal bilaterally. The left cornu was removed in its entirety to the level of the endometrium; however, the endometrium was not entered.
Cornual pregnancies implant in the area where the fallopian tube enters the uterus. Approximately 1% to 5% of ectopic pregnancies occur in the cornua [40,99,112,113]. The uterine muscle surrounding the cornua permits the pregnancy to grow to a more advanced age, often 12 to 16 weeks, before rupture. Because this area is so vascular, ruptured cornual pregnancies can result in a profuse, rapid, and fatal hemorrhage. This patient's cornual pregnancy was not ruptured at the time of identification, and her postoperative recovery was normal. Urine culture done at the time of the office visit was negative. However, the chlamydia culture was positive, and the patient was treated according to CDC guidelines [161].
Because additional pregnancies were desired, the patient was started on hormone contraception and advised not to conceive for at least one year after her surgery in an effort to allow the uterine incision site to completely heal.
Patient R is 38 years of age, gravida 4 para 2, who had a spontaneous abortion eight months previous. She presented at 15 weeks' gestation. Her initial obstetric appointment was completed at 11 weeks' gestation. No fetal heart tones were auscultated. Because the patient had a definite last menstrual period and the uterine size was appropriate at the time of the examination, no ultrasound was performed. Plans were made to schedule an ultrasound at 20 to 22 weeks' gestation for complete evaluation secondary to a family history of cardiac anomaly.
Laboratory results from her first appointment were as follows:
Hemoglobin (Hgb): 12.2
Hematocrit (Hct): 36%
WBC: 8,200
Platelets: 172,000
Blood type: B
Rh: Positive
Antibody screen: Negative
Venereal disease research test: Negative
Hepatitis B (HBsAg): Negative
HIV: Negative
Urine culture: Negative
Urinalysis: Within normal limits; protein and glucose negative
Pap test: Normal
Gonorrhea culture: Negative
Chlamydia culture: Negative
Rubella: Immune
Physical examination at the time of her first examination revealed a height of 65 inches, weight 212 lbs, and pulse 80 beats/minute. Her blood pressure was 114/72 mm Hg. Uterine size was measured to be 10 to 12 weeks' gestation; cervix was noted to be long and closed.
The patient returned with complaints of brown spotting "off and on" for several days, headache, fatigue, nausea, vomiting, and swelling in her legs. She had been unable to keep food or fluids down for 24 hours.
Her second exam reported a weight of 222 lbs, pulse of 86 beats/minute, and blood pressure of 162/94 mm Hg. Fundal height was recorded as 20 cm, and no fetal heart tones were monitored. Urinalysis (dipped) revealed 1+ protein and negative glucose with large ketones. Mucous membranes are dry, and the patient appears pale. Pitting edema in the calves is noted.
The differential diagnosis for Patient R includes:
Pre-eclampsia
Multiple gestation
Hyperemesis
Molar pregnancy
Partial molar pregnancy
An ultrasound exam was ordered and revealed no fetus but the presence of characteristic grape-like clusters in the uterus, and the diagnosis of complete hydatidiform molar pregnancy was made.
The patient was referred to an obstetrician for evacuation and management of this pregnancy. Because diagnosis was made before surgical evacuation of the uterus, a chest x-ray was performed preoperatively. It was within normal limits. CBC, platelet count, PT, PTT, liver function tests, and renal function tests were obtained. An hCG level was also obtained for baseline. Blood type and Rh type were known from her prenatal work-up. The patient did not require RhoGAM.
Patient C is a married woman, 22 years of age, gravida 1 para 0, at seven weeks' gestation according to her last menstrual period. This is a planned and welcome pregnancy. She called the office with complaints of bright red bleeding, lighter than a menstrual period but requiring sanitary pad protection. She also reported intermittent cramping. She denied lightheadedness, dizziness, nausea, vomiting, or focal pain. Although she had not experienced any nausea or vomiting, she reported continued breast tenderness.
On arrival in the office, her vital signs were obtained. Her height was 65 inches; weight 142 lbs; blood pressure 112/68 mm Hg; pulse 76 beats/minute. She appeared to be in some discomfort from the cramping, but her color was good and she was able to answer questions without difficulty. Upon questioning, she denied any trauma, recent intercourse, or changes in discharge preceding the onset of bleeding. Her last Pap test was done four months previous and was normal. Routine cervical cultures at the time were negative for chlamydia and gonorrhea.
Pelvic examination reveals the following:
External genitalia: A small amount of dark red blood is noted at the vaginal introitus. No lesion, trauma, or lacerations are noted.
Vagina: Pink, a small amount of dark red, mucinous blood is noted in the vaginal vault. No trauma or lacerations are visible.
Cervix: Appears closed, pink without exudates or lesion. A small amount of dark blood is noted coming from the cervical os.
Bimanual exam indicated a seven- to eight-week gestation-sized, anteverted uterus, mildly tender to palpation. No adnexal masses were appreciated; the cervix felt closed.
The results of laboratory studies indicated:
Blood type: A
Rh: Positive
Antibody screen: Negative
CBC: Within normal limits
hCG: 2,400 mIU/mL
An ultrasound examination was performed. An intrauterine pregnancy was noted, with a fetus and fetal cardiac activity of 136 beats per minute. A normal gestational sac was seen consistent with a pregnancy of seven weeks two days. The placenta was low lying but did not cover the cervical os. No subchorionic hemorrhage was apparent.
The differential diagnosis for Patient C includes:
Normal pregnancy
Threatened abortion
Because the patient continued to bleed, a repeat quantitative beta hCG in 48 hours was ordered. When bleeding is light, it is also appropriate to repeat the ultrasound exam in two weeks to follow growth and viability.
The patient was educated about the warning signs and symptoms of spontaneous abortion. She was encouraged to call with changes in symptoms, including bleeding saturating more than a pad an hour, passage of clots, severe cramping, lightheadedness, dizziness, fever, chills, or any other symptoms that make her uncomfortable.
Two days later, the patient returned to have her hCG repeated. She was accompanied to the office by her husband. Her repeat hCG was 1,500 mIU/mL. She continued to bleed lightly but had not saturated a pad an hour. She denied fever, chills, or passing any clots. Her vital signs remained stable, and she was afebrile.
The pelvic exam was unchanged from two days previous, with the exception of the bimanual examination. Palpation of the uterus was more uncomfortable for the patient than noted in the previous exam.
Patient C and her husband were told that the falling hCG levels indicate a pregnancy loss or miscarriage. Definitive diagnosis was made when the ultrasound revealed intrauterine fetal death, no fetal cardiac activity, and a collapsing gestational sac. A diagnosis of incomplete abortion or abortion in progress was made.
The options of care were discussed with the patient and her husband. They were offered the choices of expectant management, medical management, or surgical evacuation of the uterus. This couple chose expectant management and was sent home with instructions to call if the bleeding saturated a pad an hour, the bleeding became foul smelling, or if she developed fever or chills. Vaginal abstinence was encouraged. The patient was instructed in NSAID pain relief measures but was asked to call if additional pain control is needed. Plans were made for a follow-up telephone call later that week, and the couple was encouraged to call with any questions or concerns. A follow-up appointment was scheduled in two weeks, at which time hCG levels could be measured if indicated, birth control provided, and the patient's grief response assessed.
Providers in a variety of settings will encounter pregnant persons at various gestational ages who present with bleeding. In some instances, the bleeding will be life-threatening or herald the loss of a pregnancy. In other instances, the bleeding will be from a nonobstetric cause having little impact on health of the patient or fetus. In all cases, a compassionate, systematic, and thorough approach to the evaluation and diagnosis of any patient presenting with hemorrhagic symptoms in pregnancy will improve patient safety, satisfaction with care, and outcomes.
Bleeding in pregnancy can have many causes; only a few of the most common have been presented here in order to prepare providers to better care for patients. An understanding of the reasons pregnant patients bleed, including differential diagnoses, appropriate laboratory tests, imaging studies, and physical evaluation, is vital to ensure that patients receive timely care. Appropriate follow-up and the importance of timely referral are encouraged. Although not all providers in urgent care or office settings will be in a position to make management decisions about the care of the patient, it is important to understand treatment options. Being able to communicate treatment and follow-up information to the patient and her family enhances patient safety by emphasizing the importance of keeping scheduled appointments and following through as recommended. Patients who understand what procedures or treatments may be indicated will be less fearful of attending follow-up appointments and perhaps less anxious about the situation itself.
An actual or threatened pregnancy loss can have a significant and lasting psychologic impact on patients. Identification of those at risk for or presenting with serious post-pregnancy-loss symptoms is a critical tool for providers in office settings and urgent care or emergency room settings. How their losses are dealt with in these settings can set the tone for the remainder of the recovery process. There are many community and online resources available to individuals struggling with these issues (Appendix).
Finally, the availability of a properly trained physician who can promptly evacuate the uterus, respond to hemorrhage or ectopic pregnancy, or facilitate cesarean delivery when necessary is vital to the care for any pregnant patient. Early, timely consultations and referrals are essential.
Arcuate uterus: An abnormality of the uterus characterized by a mild concave indentation in the endometrial canal at the level of the fundus.
Bicornuate uterus: An abnormality in the uterus characterized by division into two lateral horns. The cervix may be single or double.
Blighted ovum: Fertilized egg that does not complete enough cell divisions to develop a fetus, probably due to chromosomal abnormality.
Cervical polyp: A soft, pedunculated growth extending from the cervical os, arising from the mucous membrane of the endocervix.
Chorionic villi: Structures described as finger-like projections formed as anchors from the embryonic sac to the endometrium. These eventually form the placenta.
D&C: Surgical dilatation of the uterine cervix and curettage (scraping) of the uterine wall for the purposes of emptying the uterus of its contents.
DES: Diethylstilbestrol, a hormone used in the mid-20th century for the treatment of recurrent pregnancy loss.
Ectopic pregnancy: A pregnancy implanted outside the uterus.
Endometritis: Infection of the lining of the uterus.
Gestational age: The estimated age of the pregnancy.
Gestational sac: The fluid filled chorionic/amniotic membranes developed from fertilization of the ovum.
Implantation bleeding: Light spotting thought to occur with implantation of a fertilized ovum into the endometrial lining, usually around the time of the first missed menses.
Parametritis: Infection of the structures adjacent to the uterus, connective tissue, tubal walls, lymphatics and blood vessels, or the peritoneal cavity.
Salpingitis: Infection of the fallopian tubes.
Septate uterus: An abnormality in the uterus characterized by a partial or complete septum dividing the uterus.
Subchorionic: Between the placenta and the membranes.
Succenturiate lobe or bilobed placenta: Two completely separate lobes, one usually more of an accessory lobe, of placenta with blood vessels extending between the two lobes.
Teratogen: Anything that, after exposure, results in fetal death or fetal abnormality.
Unicornuate uterus: An abnormality of the uterus characterized by a functional uterus accompanied by a rudimentary horn of the uterus, although there are many variations of this defect.
Uterine cornua: The very edge of the uterus as it attaches to the fallopian tube. Pregnancies implanting here are ectopic in nature, and their rupture can result in a profuse, rapidly fatal hemorrhage.
Uterine didelphys: An abnormality in the uterus characterized by the development of two entirely separate uteri. There are several variations.
Velamentous cord insertion: Umbilical vessels that branch and divide before reaching the placenta from the cord. The vessels are supported only by membrane and may result in significant hemorrhage if rupture occurs.
This section provides a partial listing of resources available to patients, families, or healthcare providers seeking support and/or information regarding pregnancy loss. Local support groups can be found in many medical centers and phone book listings.
| Centering Corporation |
| https://centering.org |
| (866) 218-0101 |
| A corporation providing books and workshops about grief. |
| The Compassionate Friends |
| https://www.compassionatefriends.org |
| (877) 969-0010 |
| National self-help organization offering support after the death of a child. |
| Hope After Loss |
| https://www.hopeafterloss.org |
| (203) 782-4330 |
| A global information source for perinatal health, loss, and bereavement. |
| March of Dimes |
| https://www.marchofdimes.org |
| Organization with references and support information on pregnancy and newborn loss. |
| SHARE Pregnancy and Infant Loss Support, Inc. |
| https://nationalshare.org |
| (800) 821-6819 |
| Nondenominational group offering support to those touched by the death of a child through pregnancy loss, stillbirth, or newborn death. More than 130 chapters worldwide. |
| Babies Remembered |
| Wintergreen Press |
| http://wintergreenpress.org |
| (952) 476-1303 |
| Published materials for grieving families. |
1. Griebel CP, Halvorsen J, Golemon TB, Day AA. Management of spontaneous abortion. Am Fam Physician. 2005;72(7):1243-1250.
2. American College of Obstetricians and Gynecologists. ACOG Practice Bulletin: management of recurrent pregnancy loss. Int J Gynaecol Obstet. 2002;78(2):179-190.
3. Windham GC, Von Behren J, Fenster L, Schaefer C, Swan SH. Moderate maternal alcohol consumption and risk of spontaneous abortion. Epidemiology. 1997;8(5):509-514.
4. Harville EW, Wilcox AJ, Baird DD, Weinberg CR. Vaginal bleeding in very early pregnancy. Hum Reprod. 2003;18(9):1944-1947.
5. Merck Manual. Spontaneous Abortion (Miscarriage). Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/abnormalities-of-pregnancy/spontaneous-abortion. Last accessed March 14, 2022.
6. Porter TF, Branch DW, Scott JR. Early pregnancy loss. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
7. Puscheck EE. Early Pregnancy Loss. Available at https://reference.medscape.com/article/266317-overview. Last accessed March 14, 2022.
8. Khan GQ, Heggen D. Recurrent Miscarriage: An Updated Appraisal. Available at https://search.proquest.com/openview/b92b70e79bf7486e5cbcd0074f76a362/1?pq-origsite=gscholar&cbl=47705. Last accessed March 14, 2022.
10. MedlinePlus. Miscarriage. Available at https://medlineplus.gov/miscarriage.html. Last accessed March 14, 2022.
11. Simpson JL, Jauniaux ERM. Complicated pregnancy: early pregnancy loss and stillbirth. In: Gabbe SG, Niebyl JR, Simpson JL, et al. (eds). Obstetrics: Normal and Problem Pregnancies. 7th ed. Philadelphia, PA: Elsevier Saunders; 2017: 578-594.
12. Hasan R, Baird DD, Herring AH, Olshan AF, Jonsson Funk ML, Hartmann KE. Association between first-trimester vaginal bleeding and miscarriage. Obstet Gynecol. 2009;114(4):860-867.
13. Gracia CR, Sammel MD, Chittams J, Hummel A, Shaunik AC, Barnhart KT. Risk factors for spontaneous abortion in early symptomatic first-trimester pregnancies. Obstet Gynecol. 2005;106(5 pt 1):993-999.
14. Shepard TH. Human teratogens: proven, possible, and unlikely. In: Shepard TH, Lemire RJ (eds). Catalog of Teratogenic Agents. 13th ed. Baltimore, MD: Johns Hopkins University Press; 2010.
15. Niebyl JR, Weber RJ, Briggs GG. Drugs and environmental agents in pregnancy and lactation: teratology, epidemiology. In: Gabbe SG, Niebyl JR, Simpson JL, et al. (eds). Obstetrics: Normal and Problem Pregnancies. 7th ed. Philadelphia, PA: Elsevier Saunders; 2017: 136-159.
16. American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 462: moderate caffeine consumption during pregnancy. Obstet Gynecol. 2010;116(2 Pt 1):467-468.
17. Dworzański W, Opielak G, Burdan F. Side effects of caffeine. Pol Merkur Lekarski. 2009;27(161):357-361.
18. Savitz DA, Chan RL, Herring AH, Howards PP, Hartmann KE. Caffeine and miscarriage risk. Epidemiology. 2008;19(1):55-62.
19. Gardella JR, Hill JA III. Environmental toxins associated with recurrent pregnancy loss. Semin Reprod Med. 2000;18(4):407-424.
20. Baba S, Noda H, Nakayama M, Waguri M, Mitsuda N, Iso H. Risk factors of early spontaneous abortions among Japanese: a matched case-control study. Hum Reprod. 2011;26(2):466-472.
21. Centers for Disease Control and Prevention. Smoking during pregnancy—United States, 1990–2002. MMWR. 2004;53(39):911-915.
22. Tong VT, Jones JR, Dietz PM, D'Angelo D, Bombard JM, Centers for Disease Control and Prevention. Trends in smoking before, during, and after pregnancy—Pregnancy Risk Assessment Monitoring System (PRAMS), United States, 31 sites, 2000–2005. MMWR. 2009;58(SS4):1-29.
23. American College of Obstetricians and Gynecologists. ACOG Committee Opinion Number 721: smoking cessation during pregnancy. Obstet Gynecol. 2017;130(4):e200-e204.
24. Wijesiriwardana A, Bhattacharya S, Shetty A, Smith N, Bhattacharya S. Obstetric outcome in women with threatened miscarriage in the first trimester. Obstet Gynecol. 2006;107(3):557-562.
25. Zhang BY, Wei YS, Niu JM, Li Y, Miao ZL, Wang ZN. Risk factors for unexplained recurrent spontaneous abortion in a population from southern China. Int J Gynaecol Obstet. 2010;108(2):135-138.
26. Centers for Disease Control and Prevention. E-Cigarettes and Pregnancy. Available at https://www.cdc.gov/reproductivehealth/maternalinfanthealth/tobaccousepregnancy/e-cigarettes-pregnancy.htm. Last accessed March 14, 2022.
27. Centers for Disease Control and Prevention. Alcohol Use During Pregnancy. Available at https://www.cdc.gov/ncbddd/fasd/alcohol-use.html. Last accessed March 14, 2022.
28. Henriksen TB, Hjollund NH, Jensen TK, et al. Alcohol consumption at the time of conception and spontaneous abortion. Am J Epidemiol. 2004;160(7):661-667.
29. Gauger VT, Voepel-Lewis T, Rubin P, Kostrzewa A, Tait AR. A survey of obstetric complications and pregnancy outcomes in paediatric and nonpaediatric anaesthesiologists. Paediatr Anaesth. 2003;13(6):490-495.
30. American Society of Anesthesiologists Task Force on Trace Anesthetic Gases. Waste Anesthetic Gases: Information for Management in Anesthetizing Areas and the Postanesthesia Care Unit (PACU). Available at https://www.cdc.gov/niosh/docket/archive/pdfs/niosh-064/0064-010199-mcgregor_ref2.pdf. Last accessed March 14, 2022.
31. Bell EM, Hertz-Picciotto I, Beaumont JJ. Case cohort analysis of agricultural pesticide applications near maternal residence and selected causes of fetal death. Am J Epidemiol. 2001;154(8):702-710.
32. Shirangi A, Fritschi L, Holman CD. Maternal occupational exposures and risk of spontaneous abortion in veterinary practice. Occup Environ Med. 2008;65(11):719-725.
33. Petrelli G, Figà-Talamanca I, Lauria L, Mantovani A. Spontaneous abortion in spouses of greenhouse workers exposed to pesticides. Environ Health Prev Med. 2003;8(3):77-81.
34. Brand T, van Haperen VW, van Vliet-Lachotzki EH, Steegers EA. Preconceptual care should include looking at the effect of working conditions on pregnancy. Ned Tijdschr Geneeskd. 2009;153:A363.
35. March of Dimes. Lead Poisoning. Available at https://www.marchofdimes.org/pregnancy/lead-poisoning.aspx. Last accessed March 14, 2022.
36. U.S. Department of Labor, Occupational Safety and Health Administration. Reproductive Hazards. Available at https://www.osha.gov/reproductive-hazards. Last accessed March 14, 2022.
37. Agency for Toxic Substances and Disease Registry. Toxic Substances Portal – Arsenic. Available at https://wwwn.cdc.gov/TSP/PHS/PHS.aspx?phsid=18&toxid=3. Last accessed March 14, 2022.
38. Malvasi A, Tinelli A, Buia A, De Luca GF. Possible long-term teratogenic effect of isotretinoin in pregnancy. Eur Rev Med Pharmacol Sci. 2009;13(5):393-396.
39. Lexicomp Online. Available at http://online.lexi.com. Last accessed March 14, 2022.
40. Imudia AN. Comprehensive Management Approach for Ectopic Pregnancy. Available at https://www.contemporaryobgyn.net/view/comprehensive-management-approach-ectopic-pregnancy. Last accessed March 14, 2022.
41. Li DK, Liu L, Odouli R. Exposure to non-steroidal anti-inflammatory drugs during pregnancy and risk of miscarriage: population-based cohort study. BMJ. 2003;327(7411):368.
43. Nakhai-Pour HR, Broy P, Sheehy O, Bérard A. Use of nonaspirin nonsteroidal anti-inflammatory drugs during pregnancy and the risk of spontaneous abortion. CMAJ. 2011;183(15):1713-1720.
45. Hahn KA, Hatch EE, Rothman KJ, et al. Body size and risk of spontaneous abortion among Danish pregnancy planners. Paediatr Perinat Epidemiol. 2014;28(5):412-423.
46. Nelson DB, Grisso JA, Joffe MM, Brensinger C, Shaw L, Datner E. Does stress influence early pregnancy loss? Ann Epidemiol. 2003;13(4):223-229.
47. Nepomnaschy PA, Welch KB, McConnell DS, Low BS, Strassmann BI, England BG. Cortisol levels and very early pregnancy loss in humans. Proc Natl Acad Sci U S A. 2006;103(10):3938-3942.
48. Qu F, Wu Y, Zhu YH, et al. The association between psychological stress and miscarriage: a systematic review and meta-analysis.Sci Rep. 2017;7(1):1731.
49. American College of Obstetricians and Gynecologists Committee on Practice Bulletins-Obstetrics. ACOG Practice Bulletin No. 118: antiphospholipid syndrome. Obstet Gynecol. 2011;117(1):192-199.
50. Berg TG. Antiphospholipid Syndrome and Pregnancy. Available at https://emedicine.medscape.com/article/261691-overview. Last accessed March 14, 2022.
51. Kovacs P. Effects of Fibroids on Women's Fertility. Available at https://www.medscape.com/viewarticle/701937. Last accessed March 14, 2022.
52. Devi Wold AS, Pham N, Arici A. Anatomic factors in recurrent pregnancy loss. Semin Reprod Med. 2006;24(1):25-32.
53. Lin PC. Reproductive Outcomes in Women with Uterine Anomalies. Available at https://www.medscape.com/viewarticle/471012_2. Last accessed March 14, 2022.
54. International Asherman's Association. What is Asherman's Syndrome? Available at https://www.ashermans.org. Last accessed March 14, 2022.
55. Centers for Disease Control and Prevention. DES Update Fact Sheet. Available at https://stacks.cdc.gov/view/cdc/26532. Last accessed March 14, 2022.
56. Norwitz ER, Conroy KE. Cervical Insufficiency Clinical Presentation. Available at https://emedicine.medscape.com/article/1979914-clinical. Last accessed March 14, 2022.
57. Blum J, Winikoff B, Gemzell-Danielsson K, Ho PC, Schiavon R, Weeks A. Treatment of incomplete abortion and miscarriage with misoprostol. Int J Gynaecol Obstet. 2007;99(Suppl 2):S186-S189.
58. American College of Obstetricians and Gynecologists. ACOG Committee Opinion Number 200: early pregnancy loss. Obstet Gynecol. 2018;132(5):e197-e207.
59. Emanuele MA, Emanuele N. Alcohol and the male reproductive system. Alcohol Res Health. 2001;25(4):282-287.
60. Centers for Disease Control and Prevention. Before Pregnancy: Information for Men. Available at https://www.cdc.gov/preconception/men.html. Last accessed March 14, 2022.
61. Fisch H. Older men are having children, but the reality of a male biological clock makes this trend worrisome. Geriatrics. 2009;64(1):14-17.
62. Rigby FB. Common Pregnancy Complaints and Questions. Available at https://emedicine.medscape.com/article/259724-overview. Last accessed March 14, 2022.
63. Dolan SM. Impact of parental age on the occurrence of chromosomal abnormalities. Medscape Ob/Gyn Women's Health. 2005;10(1).
64. Everett C. Incidence and outcome of bleeding before the 20th week of pregnancy: prospective study from general practice. BMJ. 1997;315(7099):32-34.
65. Snell BJ. Assessment and management of bleeding in the first trimester of pregnancy. J Midwifery Womens Health. 2009;54(6):483-491.
66. Dighe M, Cuevas C, Moshiri M, Dubinsky T, Dogra VS. Sonography in first trimester bleeding. J Clin Ultrasound. 2008;36(6):352-366.
67. American College of Obstetricians and Gynecologists. ACOG Committee Opinion Number 193: tubal ectopic pregnancy. Obstet Gynecol. 2018;131(3):e91-e103.
68. Williams MA, Mittendorf R, Lieberman E, Monson RR. Adverse infant outcomes associated with first-trimester vaginal bleeding. Obstet Gynecol. 1991;78(1):14-18.
69. Arafa M, Abdel-Fataah M, Zeid HA, el-Khouly A. Outcomes of pregnancies complicated by early vaginal bleeding. East Mediterr Health J. 2000;6(2-3):457-464.
70. The Merck Manuals Online Medical Library. Vaginal Bleeding During Early Pregnancy. Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/symptoms-during-pregnancy/vaginal-bleeding-during-early-pregnancy. Last accessed March 14, 2022.
71. Konrad G. First-trimester bleeding with falling HCG: don't assume miscarriage. Can Fam Physician. 2007;53(5):831-832.
72. Barnhart KT, Sammel MD, Rinaudo PF, Zhou L, Hummel AC, Guo W. Symptomatic patients with an early viable intrauterine pregnancy: hCG curves redefined. Obstet Gynecol. 2004;104(1):50-55.
73. MedlinePlus. Miscarriage: Threatened. Available at https://medlineplus.gov/ency/article/000907.htm. Last accessed March 14, 2022.
74. March of Dimes. Rh Disease. Available at https://www.marchofdimes.org/complications/rh-disease.aspx. Last accessed March 14, 2022.
75. American College of Obstetricians and Gynecologists. ACOG Committee Opinion Number 181: prevention of RhD alloimmunization. Obstet Gynecol. 2017;130(2):e57-e70.
76. Bernstein PS, Cole DS. Rh Alloimmunization. Available at https://www.medscape.com/viewarticle/442196. Last accessed March 14, 2022.
77. Testing.com. Progesterone. Available at https://www.testing.com/tests/progesterone. Last accessed March 14, 2022.
78. Fetal assessment during labor. In: King TL, Brucker MC, Osborne K, Jevitt CM (eds). Varney's Midwifery. 6th ed. Sudbury, MA: Jones and Bartlett Publishers, Inc.; 2019: 913-950.
79. Gaufberg SV. Early Pregnancy Loss in Emergency Medicine. Available at https://emedicine.medscape.com/article/795085-overview. Last accessed March 14, 2022.
80. Schauberger CW, Mathiason MA, Rooney BL. Ultrasound assessment of first-trimester bleeding. Obstet Gynecol. 2005;105(2):333-338.
81. The Miscarriage Association. Ultrasound Scans. Available at https://www.miscarriageassociation.org.uk/information/worried-about-pregnancy-loss/ultrasound-scans. Last accessed March 14, 2022.
82. Maso G, D'Ottavio G, De Seta F, Sartore A, Piccoli M, Mandruzzato G. First-trimester hematoma and outcome of pregnancy.Obstet Gynecol. 2005;105(2):339-344.
83. Chhabra A, Butehr CD, Batra K, et al. Subchorionic Hemorrhage Imaging. Available at https://emedicine.medscape.com/article/404971-overview. Last accessed March 14, 2022.
84. Aleman A, Althabe F, Belizán J, Bergel E. Bed rest during pregnancy for preventing miscarriage. Cochrane Database Syst Rev. 2005;(2):CD003576.
85. King TL, Leslie MS. Medical complications in pregnancy. In: King TL, Brucker MC, Kriebs JM, Fahey JO, Gegor CL, Varney H (eds). Varney's Midwifery. 6th ed. Sudbury, MA: Jones and Bartlett Publishers, Inc.; 2019: 819-858.
86. Medline Plus. Endometritis. Available at https://medlineplus.gov/ency/article/001484.htm. Last accessed March 14, 2022.
87. Testing.com. Pregnancy Test (hCG). Available at https://www.testing.com/tests/pregnancy-test-hcg. Last accessed March 14, 2022.
88. Patient.info. Miscarriage. Available at https://patient.info/doctor/miscarriage-pro. Last accessed March 14, 2022.
89. Schwerdtfeger KL, Shreffler KM. Trauma of pregnancy loss and infertility for mothers and involuntarily childless women in the contemporary United States. J Loss Trauma. 2009;14(3):211-227.
91. Schliep KC, Mitchell EM, Mumford SL, et al. Trying to conceive after an early pregnancy loss: an assessment on how long couples should wait. Obstet Gynecol. 2016;127(2):204-212.
92. Centers for Disease Control and Prevention. U.S. selected practice recommendations for contraceptive use, 2013: adapted from the World Health Organization Selected Practice Recommendations for Contraceptive Use, 2nd edition. MMWR. 2013;62(5):1-46.
93. Krakow D. Medical and surgical complications of pregnancy. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
94. Nanda K, Lopez LM, Grimes DA, Peloggia A, Nanda G. Expectant care versus surgical treatment for miscarriage. Cochrane Database Syst Rev. 2012;(3):CD003518.
95. Pauleta JR, Clode N, Graca LM. Expectant management of incomplete abortion in the first trimester. Int J Gynaecol Obstet. 2009;106(1):35-38.
96. Niinimäki M, Pouta A, Bloigu A, et al. Immediate complications after medical compared with surgical termination of pregnancy. Obstet Gynecol. 2009;114(4):795-804.
97. Kim C, Barnard S, Neilson JP, Hickey M, Vazquez JC, Dou L. Medical treatments for incomplete miscarriage. Cochrane Database Syst Rev. 2017;(1):CD007223.
98. Molnar AM, Oliver LM, Geyman JP. Patient preferences for management of first-trimester incomplete spontaneous abortion. J Am Board Fam Pract. 2000;13(5):333-337.
99. Molinaro TA, Barnhart KT. Ectopic pregnancies in unusual locations: interstitial (corneal) ectopic pregnancy. Semin Reprod Med. 2007;25(2):123-130.
100. Bui Q. Management options for early incomplete miscarriage. Am Fam Physician. 2011;83(3):258-260.
101. Borgatta L, Kapp N; Society of Family Planning. Clinical Guidelines: labor induction abortion in the second trimester. Contraception. 2011;84(1):4-18.
102. Lemmers M, Verschoor MA, Rengerink O, et al. MisoREST: surgical versus expectant management in women with an incomplete evacuation of the uterus after misoprostol treatment for miscarriage: a randomized controlled trial. Hum Reprod. 2016;31(11):2421-2427.
103. Tang OS, Ho PC. The use of misoprostol for early pregnancy failure. Curr Opin Obstet Gynecol. 2006;18(6):581-586.
104. Dempsey A, Davis A. Medical management of early pregnancy failure: how to treat and what to expect. Semin Reprod Med. 2008;26(5):401-410.
105. Zhang J, Gilles JM, Barnhart K, Creinin MD, Westhoff C, Frederick MM for the National Institute of Child Health Human Development (NICHD) Management of Early Pregnancy Failure Trial. A comparison of medical management with misoprostol and surgical management for early pregnancy failure. N Engl J Med. 2005;353(8):761-769.
106. Blandine T, Ouattara AZ, Coral A, et al. Oral misoprostol as first-line care for incomplete abortion in Burkina Faso. Int J Gynaecol Obstet. 2012;119(2):166-169.
107. Ning F, Hou H, Morse AN, Lash GE. Understanding and management of gestational trophoblastic disease. F1000Res. 2019;8:F1000.
108. U.S. Food and Drug Administration. Misoprostol (Marketed as Cytotec) Information. Available at https://www.fda.gov/drugs/postmarket-drug-safety-information-patients-and-providers/misoprostol-marketed-cytotec-information. Last accessed March 14, 2022.
109. March of Dimes. Dealing with Grief After the Death of Your Baby. Available at https://www.marchofdimes.org/complications/dealing-with-grief-after-the-death-of-your-baby.aspx. Last accessed March 14, 2022.
110. Blumenthal P, Clark S, Coyaji KJ, et al. Providing Medical Abortion in Low-Resource Settings: An Introductory Guidebook. 2nd ed. New York, NY: Gynuity; 2009.
111. Stöppler MC. Ectopic Pregnancy (Tubal Pregnancy). Available at https://www.medicinenet.com/ectopic_pregnancy/article.htm. Last accessed March 14, 2022.
112. Bourgon DR, Balmforth GJ, Outwater E. Ectopic Pregnancy Imaging. Available at https://emedicine.medscape.com/article/403062-overview. Last accessed March 14, 2022.
113. Seeber BE, Barnhart KT. Ectopic pregnancy. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
114. Sepilian VP, Wood E. Ectopic Pregnancy. Available at https://emedicine.medscape.com/article/2041923-overview. Last accessed March 14, 2022.
115. Clayton HB, Schieve LA, Peterson HB, Jamieson DJ, Reynolds MA, Wright VC. Ectopic pregnancy risk with assisted reproductive technology procedures. Obstet Gynecol. 2006;107(3):596-604.
116. Bayer HealthCare Pharmaceuticals, Inc. Mirena. Available at https://www.mirena-us.com. Last accessed March 14, 2022.
117. Bayer HealthCare Pharmaceuticals, Inc. Skyla. Available at https://www.skyla-us.com. Last accessed March 14, 2022.
118. Sunderam S, Kissin DM, Crawford SB, et al. Assisted reproductive technology surveillance—United States, 2013. MMWR. 2015;64(SS11):1-25.
119. Hughes E, Brown J, Collins JJ, Vanderkerchove P. Clomiphene citrate for unexplained subfertility in women. Cochrane Database Syst Rev. 2010;(1):CD000057.
120. Williams S, Peipert J, Buckel C, Zhao Q, Madden T, Secura G. Contraception and the risk of ectopic pregnancy. Contraception. 2014;90(3):326.
121. Jacobstein R. Long-acting and permanent contraception: progestin-containing subdermal implants. J Midwifery Womens Health. 2007;52(4):361-367.
122. Jazayeri A, Coussons HS. Surgical Management of Ectopic Pregnancy. Available at https://emedicine.medscape.com/article/267384-overview. Last accessed March 14, 2022.
123. Lozeau AM, Potter B. Diagnosis and management of ectopic pregnancy. Am Fam Physician. 2005;72(9):1707-1714.
124. King TL. Anatomy and physiology of pregnancy: maternal adaptations to pregnancy. In: King TL, Brucker MC, Kriebs JM, Fahey JO, Gegor CL, Varney H (eds). Varney's Midwifery. 6th ed. Sudbury, MA: Jones and Bartlett Publishers, Inc.; 2019: 633-662.
125. Bickell NA, Bodian C, Anderson RM, Kase N. Time and the risk of ruptured tubal pregnancy. Obstet Gynecol. 2004;104(4):789-794.
127. Sepilian VP, Wood E. Ectopic Pregnancy Workup. Available at https://emedicine.medscape.com/article/2041923-workup. Last accessed March 14, 2022.
128. Hajenius PJ, Mol F, Mol BW, Bossuyt PM, Ankum WM, van der Veen F. Interventions for tubal ectopic pregnancy. Cochrane Database Syst Rev. 2007;(1):CD000324.
129. ACOG Practice Bulletin No. 94: medical management of ectopic pregnancy. Obstet Gynecol. 2008;111:1479-1485.
130. Kelly H, Harvey D, Moll S. A cautionary tale: fatal outcome of methotrexate therapy given for management of ectopic pregnancy. Obstet Gynecol. 2006;107(2 pt 2):439-441.
131. Li AJ. Gestational trophoblastic neoplasms. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
132. Klatt TE, Franciosi, Cruikshank DP. Normal fetus with a twin presenting as both a complete hydatidiform mole and placenta previa. Obstet Gynecol. 2006;107(2 pt 2):527-530.
133. Shazly SAEM, Ali MK, Badee AYA, Alsokkary AA, Khodary MM, Mostafa NAE. Twin pregnancy with complete hydatidiform mole and coexisting fetus following ovulation induction with a non-prescribed clomiphene citrate regimen: as case report.J Med Case Rep. 2012;6:95.
134. Sekharan K. Gestational trophoblastic diseases. In: Ratnam SS, Rao KB, Arulkumaran S (eds). Obstetrics and Gynecology for Postgraduates. 3rd ed., vol. 2. India: Universities Press; 2010.
135. Soper JT, Mutch DG, Schink JC, American College of Obstetricians and Gynecologists. ACOG Practice Bulletin 53: diagnosis and treatment of gestational trophoblastic disease. Gynecol Oncol. 2004;93(3):575-585.
136. The Merck Manuals Online Medical Library. Gestational Trophoblastic Disease. Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/gynecologic-tumors/gestational-trophoblastic-disease. Last accessed March 14, 2022.
137. Salani R, Eisenhauer EL, Copeland LJ. Malignant diseases and pregnancy. In: Gabbe SG, Niebyl JR, Simpson JL, et al. (eds). Obstetrics: Normal and Problem Pregnancies. 6th ed. Philadelphia, PA: Elsevier Saunders; 2012.
138. National Cancer Institute. Gestational Trophoblastic Disease. Available at https://www.cancer.gov/types/gestational-trophoblastic/hp. Last accessed March 14, 2022.
139. Scott Ricci S, Kyle T, Carman S. Maternity and Pediatric Nursing. 3rd ed. Baltimore, MD: Lippincott Williams & Wilkins; 2017.
140. Royal College of Obstetricians and Gynaecologists. The Management of Gestational Trophoblastic Neoplasia. London: Royal College of Obstetricians and Gynaecologists; 2010.
141. Lurain JR. Hydatidiform Mole: Recognition and Management. Available at https://www.contemporaryobgyn.net/view/hydatidiform-mole-recognition-and-management. Last accessed March 14, 2022.
142. Oyelese Y, Smulian JC. Placenta previa, placenta accreta, and vasa previa. Obstet Gynecol. 2006;107(4):927-941.
143. Bakker R, Ramus RM. Placenta Previa. Available at https://emedicine.medscape.com/article/262063-overview. Last accessed March 14, 2022.
144. Kay HH. Placenta previa and abruption. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
145. Francois KE, Foley MR. Antepartum and postpartum hemorrhage. In: Gabbe SG, Niebyl JR, Simpson JL, et al. (eds). Obstetrics: Normal and Problem Pregnancies. 7th ed. Philadelphia, PA: Saunders; 2017: 395-424.
146. Mayo Clinic. Placenta Previa. Available at https://www.mayoclinic.org/diseases-conditions/placenta-previa/symptoms-causes/syc-20352768. Last accessed March 14, 2022.
147. Royal College of Obstetricians and Gynaecologists. Placenta Praevia, Placenta Praevia Accreta and Vasa Praevia: Diagnosis and Management. London: Royal College of Obstetricians and Gynaecologists; 2011.
148. Oppenheimer L, Society of Obstetricians and Gynaecologists of Canada. Diagnosis and management of placenta previa. J Obstet Gynaecol Can. 2007;29(3):261-273.
149. Eichelberger KY, Haeri S, Kessler DC, Swartz A, Herring A, Wolfe HM. Placenta previa in the second trimester: sonographic and clinical factors associated with its resolution. Am J Perinatol. 2011;28(9):735-740.
150. American College of Obstetricians and Gynecologists Committee on Obstetric Practice. Obstetric care consensus: placenta accreta spectrum. Obstet Gynecol. 2018;132(6):e259-e275.
151. Warshak CR, Ramos GA, Eskander R, et al. Effect of predelivery diagnosis in 99 consecutive cases of placenta accreta. Obstet Gynecol. 2010;115(1):65-69.
152. Wong HS, Hutton J, Zuccollo J, Tait J, Pringle KC. The maternal outcome in placenta accreta: the significance of antenatal diagnosis and non-separation of placenta at delivery. N Z Med J. 2008;121(1277):30-38.
153. Eller AG, Porter TF, Soisson P, Silver RM. Optimal management strategies for placenta accreta. BJOG. 2009;116(5):648-654.
154. Gagnon R, Morin L, Bly S, et al. Guidelines for the management of vasa previa. J Obstet Gynaecol Can. 2009;31(8):748-760.
155. The Merck Manuals Online Medical Library. Abruptio Placentae. Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/abnormalities-of-pregnancy/abruptio-placentae. Last accessed March 14, 2022.
156. Mayo Clinic. Placental Abruption: Symptoms. Available at https://www.mayoclinic.org/diseases-conditions/placental-abruption/symptoms-causes/syc-20376458. Last accessed March 14, 2022.
157. Gagnon A, Wilson RD, Audibert F, et al. Obstetrical complications associated with abnormal maternal serum markers analytes.J Obstet Gynaecol Can. 2008;30(10):918-949.
158. Krantz D, Hallahan T, Janik D, Carmichael J. Maternal serum screening markers and adverse outcome: a new perspective. J Clin Med. 2014;3(3):693-712.
159. Androutsopoulos G, Kkogkos P, Decavalas G. Mid-trimester maternal serum HCG and alpha fetal protein levels: clinical significance and prediction of adverse pregnancy outcome. Int J Endocrinol Metab. 2013;11(2):102-106.
160. Denney JM, Culhane JF, Goldenberg RL. Prevention of preterm birth. Womens Health. 2008;4(6):625-638.
161. Workowski KA, Bolan GA, Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2015. MMWR. 2010;64(RR3):1-137.
162. The Merck Manuals Online Medical Library. Cervical Polyps. Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/miscellaneous-gynecologic-disorders/cervical-polyps. Last accessed March 14, 2022.
163. MedlinePlus. Cervical Polyps. Available at https://medlineplus.gov/ency/article/001494.htm. Last accessed March 14, 2022.
164. Giuntoli RL II, Bristow RE. Cervical cancer. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
165. Morice P. Narducci F, Mathevet P, et al. French recommendations on the management of invasive cervical cancer during pregnancy. Int J Gynecol Cancer. 2009;19(9):1638-1641.
166. The Merck Manuals Online Medical Library. Cervical Cancer. Available at https://www.merckmanuals.com/professional/gynecology-and-obstetrics/gynecologic-tumors/cervical-cancer. Last accessed March 14, 2022.
167. National Cancer Institute. SEER Cancer Stat Facts: Cervical Cancer. Available at https://seer.cancer.gov/statfacts/html/cervix.html. Last accessed March 14, 2022.
168. Editors of The Johns Hopkins Medical Letter Health After 50, Margolis S. The Johns Hopkins Complete Home Guide to Symptoms and Remedies. New York, NY: Black Dog and Leventhal Publishers, Inc.; 2004.
169. Gould NS, Walker JL. Vulvar and vaginal cancer. In: Gibbs RS, Karlan BY, Haney AF, Nygaard I (eds). Danforth's Obstetrics and Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
171. Centers for Disease Control and Prevention. Vaginal and Vulvar Cancers. Available at https://www.cdc.gov/cancer/vagvulv. Last accessed March 14, 2022.
172. Johnson EK. Urinary Tract Infections in Pregnancy. Available at https://emedicine.medscape.com/article/452604-overview. Last accessed March 14, 2022.
173. Fulop T. Acute Pyelonephritis. Available at https://emedicine.medscape.com/article/245559-overview. Last accessed March 14, 2022.
174. Colombo DF. Renal disease in pregnancy. In: Gabbe SG, Niebyl JR, Simpson JL, et al. (eds). Obstetrics: Normal and Problem Pregnancies. 7th ed. Philadelphia, PA: Elsevier Saunders; 2017: 850-861.
175. MedlinePlus. Lithotripsy. Available at https://medlineplus.gov/ency/article/007113.htm. Last accessed March 14, 2022.
176. American College of Obstetricians and Gynecologists. ACOG Practice Bulletin 115: vaginal birth after previous cesarean. Obstet Gynecol. 2010;116(2 pt 1):450-463.
177. Nahum GG, Pham KQ. Uterine Rupture in Pregnancy. Available at https://reference.medscape.com/article/275854-overview. Last accessed March 14, 2022.
178. Magnus MC, Wilcox AJ, Morken NH, Weinberg CR, Håberg SE. Role of maternal age and pregnancy history in risk of miscarriage: prospective register based study. BMJ. 2019;364:l869.
179. 179. Şükür YE, Göç G, Köse O, et al. The effects of subchorionic hematoma on pregnancy outcome in patients with threatened abortion. J Turk Ger Gynecol Assoc. 2014;15(4):239-242.
180. Obstetric care consensus no. 7: placenta accreta spectrum. Obstet Gynecol. 2018;132(6):e259-e275.
181. Dimitriadis E, Menkhorst E, Saito S, Kutteh WH, Brosens JJ. Recurrent pregnancy loss. Nat Rev Dis Primers. 2020;6(98).
182. Young BK. A multidisciplinary approach to pregnancy loss: the pregnancy loss prevention center. J Perinat Med. 2019;47(1):41-44.
183. Coomarasamy A, Devall AJ, Cheed V, et al. A randomized trial of progesterone in women with bleeding in early pregnancy. N Eng J Med. 2019;380:1815-1824.
184. Hendriks E, MacNaughton H, MacKenzie MC. First trimester bleeding: evaluation and management. Am Fam Physician. 2019;99:166-174.
1. American College of Emergency Physicians Clinical Policies Subcommittee (Writing Committee) on Early Pregnancy, Hahn SA, Promes SB, Brown MD. Clinical policy: critical issues in the initial evaluation and management of patients presenting to the emergency department in early pregnancy. Ann Emerg Med. 2017;69(2):241-250. Available at https://www.acep.org/globalassets/new-pdfs/clinical-policies/cp-earlypregnancy-doc.pdf. Last accessed March 18, 2022.
2. American College of Obstetricians and Gynecologists. Medication Abortion Up to 70 Days of Gestation. Washington, DC: American College of Obstetricians and Gynecologists; 2020. Available at https://www.acog.org/clinical/clinical-guidance/practice-bulletin/articles/2020/10/medication-abortion-up-to-70-days-of-gestation. Last accessed March 18, 2022.
3. American College of Obstetricians and Gynecologists. Tubal Ectopic Pregnancy. Washington, DC: American College of Obstetricians and Gynecologists; 2018. Available at https://www.acog.org/Clinical-Guidance-and-Publications/Practice-Bulletins/Committee-on-Practice-Bulletins-Gynecology/Tubal-Ectopic-Pregnancy. Last accessed March 18, 2022.
4. Seckl MJ, Sebire NJ, Fisher RA, et al. Gestational trophoblastic disease: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2013;24(Suppl 6):vi39-vi50. Available at https://www.esmo.org/Guidelines/Gynaecological-Cancers/Gestational-Trophoblastic-Disease. Last accessed March 18, 2022.
5. Podrasky AE, Javitt MC, Glanc P, et al. ACR Appropriateness Criteria: Second and Third Trimester Bleeding. Reston, VA: American College of Radiology; 2020. Available at https://acsearch.acr.org/docs/69465/Narrative. Last accessed March 18, 2022.
Mention of commercial products does not indicate endorsement.