Healthcare professionals are an integral part of the transport system, stabilizing patients prior to transport, providing care in transport and ensuring the safety of the patient throughout the transport process. This course will provide information on the types of transport available, transport physiology (those stressors that impact the patient in transport), transport regulations, stabilization for transport, care in transport, and the general principles of transporting patients, including both safety and medical-legal issues. All healthcare professionals involved in caring for sick or injured patients must be aware of all of these concepts in order to provide optimal care.
- INTRODUCTION
- MODES OF TRANSPORT
- TRANSPORT PHYSIOLOGY
- THE TRANSPORT PROCESS
- STABILIZATION FOR TRANSPORT
- STABILIZATION OF SPECIFIC PATIENT POPULATIONS
- DETAILS INVOLVED IN THE TRANSPORT OF PATIENTS
- PRINCIPLES OF TRANSPORT
- MEDICAL-LEGAL ISSUES
- SUMMARY
- INTERNET RESOURCES
- Works Cited
- Works Consulted
- Evidence-Based Practice Recommendations Citations
This course is designed for all healthcare professionals involved in the transport of critically ill patients, including physicians, physician assistants, and nurses.
The purpose of this course is to provide information on the types of patient transport available, transport physiology, transport regulation, stabilization for transport, care in transport, and the general principles of transporting patients, including both safety and medical-legal issues, in order to facilitate better patient care.
Upon completion of this course, you should be able to:
- Compare the advantages and disadvantages of ground, fixed-wing, and helicopter transport.
- Evaluate physiologic changes that occur during transport and list interventions to limit patient compromise.
- Describe the current federal requirements and regulations in regard to transporting the ill or injured patient.
- List, in order, the appropriate steps in arranging an interfacility transport.
- Identify stabilization procedures to be undertaken for all patients requiring transport.
- Describe the emotional impact of transport on the patient and/or the family and list interventions to provide psychosocial support for these individuals, taking into consideration cultural and linguistic variables.
- List the baseline diagnostic studies to be performed prior to transport, if time and patient condition warrant their performance.
- Cite physiologic changes that occur during transport and impact the neurologic, respiratory, and cardiovascular systems.
- Summarize special considerations for transport of burn and multiple-trauma patients.
- Identify the problems that may occur during transport of the pediatric patient.
- Identify the stressors of transport that impact the elderly patient and cite how to best stabilize the patient to limit these complications.
- Describe the impact of transport on the pregnant patient and her fetus and how these problems can be managed.
- Describe the steps in caring for a patient in transport.
- Describe how transport impacts the choice and use of biomedical equipment.
- List actions to take to ensure the safety of the crew, the patient, and the personnel on the ground when performing both a helicopter and a fixed-wing transport.
- Cite the medical-legal requirements of providing care to a patient outside of a hospital system.
Susan Engman Lazear, RN, MN, received her undergraduate education at the Walter Reed Army Institute of Nursing in Washington, D.C. After completing her BSN, she served as an Army Nurse at Letterman Army Medical Center in San Francisco for four years. She then attended the University of Washington School of Nursing and received a Master’s in Nursing, specializing in Burn, Trauma and Emergency Nursing. After receiving her MN, she started Airlift Northwest, the air ambulance service based in Seattle which serves the entire Northwest region, including Alaska. Mrs. Lazear left the air ambulance service to start her own nursing education and consulting business, Specialists in Medical Education. For the past 20 years she has been teaching emergency nursing courses throughout the country. She lives in the Seattle area. Mrs. Lazear continues to teach and publish. She is both an editor and contributing author of Critical Care Nursing, published by W.B. Saunders Company, in June of 1992. She served as an author and reviewer of the Emergency Nursing Core Curriculum 6th Edition, published by W.B. Saunders Company in 2007. She has been named to the Who’s Who in American Healthcare list annually since 1992.
Contributing faculty, Susan Engman Lazear, RN, MN, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
John V. Jurica, MD, MPH
Jane C. Norman, RN, MSN, CNE, PhD
The division planners have disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#90744: Transport Methods for Critically Ill Patients
Stabilization and transporting patients when the needs of the patient surpass the available resources of a facility is now common occurrence. Legislation requires that patients receive the optimum care available to them, thus requiring the transport of patients to facilities that can provide this type of care. Healthcare professionals are an integral part of the transport system whether they are stabilizing patients prior to transport, providing care in transport, or ensuring the safety of the patient throughout the transport process. This course will provide information on the types of transport available, transport physiology (e.g., the stressors that impact the patient in transport), transport regulations, stabilization for transport, care in transport, and the general principles of transporting patients, including both safety and medical-legal issues. All healthcare professionals involved in caring for sick or injured patients should be aware of all of these concepts in order to provide optimal care.
Transport of the sick or injured patient from one location to another is not a new concept. For all of recorded history, patients have been moved so that they could receive medical treatment. Soldiers wounded on the battlefield have been transported in moving conveyances ranging from horse-drawn carts to purpose-built aircraft. The first soldiers transported by air were flown in hot air balloons during the Prussian siege of Paris in 1870. Throughout the 20th century, transport methods developed slowly and, at times, haphazardly. However, during the late 1960s and early 1970s, Congress enacted numerous pieces of legislation addressing emergency medical care and transport. These laws were the impetus to develop sophisticated transport systems. Since that time, transporting of patients has developed into a subspecialty of emergency medicine, involving physicians, nurses, paramedics, respiratory therapists, and other prehospital care providers. Transferring a patient in a safe and efficient manner is now considered essential in the provision of medical care.
Transport of patients occurs primarily in two distinct environments: on the ground by ambulance or in the air by either a rotor-wing vehicle (helicopter) or a fixed-wing vehicle (airplane). Air and ground transport each have advantages and disadvantages; the decision whether to use air or ground transport should be made on the basis of many factors. Consideration of out-of-hospital time, weather, terrain, work space, equipment, personnel, and proximity of a landing site will assist the transferring team in making an informed decision as to how to best meet each individual patient's needs.
Ground transport occurs most often in a modular type vehicle that can easily accommodate two supine patients and a full crew. Access to the patient is excellent and advanced life support measures can be easily performed. Larger ambulances can accommodate larger pieces of equipment including infant isolettes, ventilators, and intra-aortic balloon pumps. The level of care administered during the transport varies with the level of training of the transport personnel, varying from basic life support (BLS) to advanced life support (ALS). In choosing an appropriate transport vehicle, the referring physician is required to choose a vehicle in which the level of care does not diminish during the transport itself.
Ground transport is the cornerstone of the emergency response system in the United States. Ground ambulances are accessed by the public through the 911 system and provide rapid stabilization of ill or injured patients. In large urban areas with well-developed prehospital care systems, the time-to-patient is less than 10 minutes. However, as the population base expands into rural areas, the time-to-patient tends to lengthen, delaying access to medical care. To reduce the patient's out-of-hospital time, air ambulances have been developed to augment ground transport programs, providing rapid transfer.
Ground ambulance transport is an efficient and appropriate method of transport for most ill and injured patients in this country. The number of ground transports increases annually and the appropriateness of these transports is unquestioned. However, there are instances in which ground transport is at a disadvantage. Adverse weather conditions can impact the vehicle's ability to traverse certain terrain. At the same time, this adverse weather can prevent air ambulances from flying, leaving ground transport as the only viable option. Time-in-transit is another drawback of ground transport. Some critically ill or injured patients cannot withstand the stressors of transport and the shorter the out-of-hospital time, the better that patient's chance for survival. Finally, when choosing to utilize a ground ambulance, the needs of the community should be examined. Some isolated rural areas have only a single ground ambulance to service a largely scattered population base. If this vehicle is taken out of service for an interfacility transport, the people of the community are temporarily left without the medical coverage they have come to expect.
Air transport should be considered an adjunct to, not a replacement for, ground transport. There are inherent dangers in transporting by air, and it is an expensive alternative. Many third-party providers are withholding reimbursement for flights, which are considered nonemergent. The advantage of fixed-wing transport is the ability to travel long distances at speeds between 250 and 570 miles per hour. Care is usually provided in a pressurized cabin with sophisticated on-board medical equipment. Many aircraft utilized for air transport of patients have the capability of transporting multiple patients, and in some instances, family members are allowed to accompany the patient. All-weather navigational equipment allows for the transfer of patients during inclement weather. Many of the dedicated aircraft utilized in air transports have been referred to as "flying ICUs."
Fixed-wing transport requires suitable airfields to ensure the safety of the crew and patient. Accessibility to such fields may be a problem in isolated areas. Optimally, a 5,000-foot paved runway located near the site of the patient would erase the disadvantages of air transport. However, because hospitals are located a considerable distance from most airfields, ground transport is utilized at the beginning and the end of the air transport. (Note: A unique situation exists in Anchorage, Alaska, where a regional referral medical center is located on the edge of an appropriate airfield and the patient can be off-loaded from the plane and wheeled directly into the hospital. This is far from the norm.) The patient should be moved in and out of the aircraft to a waiting ground ambulance and then transported from the referring hospital or to the receiving hospital. This increases the likelihood of the dislodgment of tubes, lines, etc. There is an additional cost associated with this supplemental ground transport.
Rotor-wing vehicles provide rapid point-to-point transfers. Helicopters are capable of reaching most areas and can bypass difficult terrain. Landing zones can be made at or near the site of the patient to prevent lengthy ground transport times. Most helicopters operate within a 150-mile radius of their base station to allow for routine flights without refueling. The type of helicopter utilized by a transport program is determined by a number of factors. Most programs now rely on twin-engine helicopters for their enhanced performance and safety records. Certain helicopters perform better at altitude; they are utilized in areas of high terrain, such as in the Rocky Mountains or in the Swiss Alps. The highest helicopter rescue was performed in 2010 at 23,240 feet (density altitude) for injured climbers on the Kamet glacier in the Himalayas. In 2013, a simulated rescue was performed at 25,590 feet on Mt. Everest; however, the practical limit for safe rescue operations is generally agreed to be 23,000 feet [6].
The single largest disadvantage of helicopters is their dependence upon certain minimum weather conditions; if these conditions are not met, the weather can cause delay or cancellation of the flight. Helicopter cabin size often restricts access to the patient once the patient has been loaded into the helicopter. This limited access reduces the number of in-flight interventions possible. Weight limitations restrict the number of passengers and the amount of equipment on board. When transferring a patient by rotor-wing vehicle, comprehensive stabilization of the patient is required prior to departure.
As healthcare dollars become tighter and legislation mandates transport of patients to better-equipped facilities, those caring for patients who need transport should be cognizant of the advantages and disadvantages of the modes of transport. As air ambulance programs continue to proliferate in this country (although the number of programs has leveled off in the last few years), the preparation to choose between ground, helicopter, or fixed-wing transport will be important.
Exposure to environmental factors occurs during both ground and air transport. Some of the stressors are unique to air transport; for example, atmospheric changes occur when the aircraft's altitude changes. The problems that develop depend on vehicle design and configuration, motion of the transport vehicle, the patient's condition, or a combination of factors. Many of these stressors are detrimental to the patient's condition; however, with proper nursing care before and during the transport, these harmful effects can be minimized or eliminated.
Transport vehicles are designed according to different principles. These design specifics can impact the stressors that a patient encounters. Ground ambulances should travel as the road lies. This causes multiple forward, reverse, and lateral forces on the patient and the crew. These forces are greatly minimized in both fixed-wing and helicopter transports; however, the forward and reverse forces are momentarily much greater when an airplane is taking off or landing.
The following ten problems occur during transport. The first four are a result of changes in atmospheric pressure; therefore, these are only encountered in air transport.
Four types of hypoxia can occur to impact the oxygenation status of the patient transported by air. The physiology of these four types will be reviewed, followed by a discussion of the manifestations of hypoxia and interventions that can be instituted to minimize or prevent these harmful effects.
Hypoxic hypoxia, also known as altitude hypoxia, occurs when changes in atmospheric pressure are encountered. As an aircraft (both fixed-wing and rotor-wing) ascends in altitude, the partial pressure of oxygen (PO2) decreases, causing a decreased diffusion gradient for the oxygen molecule to cross the alveolar membrane. Table 1 shows the effects of altitude on the PO2.
EFFECTS OF ALTITUDE ON PARTIAL PRESSURE OF AMBIENT HUMIDIFIED OXYGEN
| Altitude (feet) | Atmospheric Pressure (mm Hg) | Partial Pressure of Oxygen (mm Hg) |
|---|---|---|
| 0 | 760 | 150 |
| 500 | 746 | 147 |
| 1,000 | 733 | 144 |
| 1,500 | 720 | 141 |
| 2,000 | 707 | 139 |
| 2,500 | 694 | 136 |
| 3,000 | 681 | 133 |
| 3,500 | 669 | 131 |
| 4,000 | 656 | 128 |
| 4,500 | 644 | 125 |
| 5,000 | 632 | 123 |
| 5,500 | 621 | 121 |
| 6,000 | 609 | 118 |
| 6,500 | 598 | 116 |
| 7,000 | 586 | 113 |
| 8,000 | 564 | 109 |
| 9,000 | 543 | 104 |
| 10,000 | 523 | 100 |
Simple calculation of the diffusion gradient is accomplished by utilizing the following formulas:
(Atmospheric Pressure - Water Pressure) x Oxygen Percentage = PO2
and
Alveolar PO2 - Venous PO2 = Diffusion Gradient
Assuming that the water pressure is equal to 47 mm Hg, the PO2 at sea level would be approximately 150 mm Hg [(760-47) x 0.21 = 150]. At an altitude of 6,000 feet the calculated PO2 would be 118 mm Hg [(609-47) x 0.21) = 118].
The decrease in PO2 that occurs in the respiratory tree is approximately 45 mm Hg. Therefore, at the alveolar level, the partial pressure of arterial oxygen (PaO2) at sea level would be approximately 105 mm Hg (150-45) and the PaO2 at 6,000 feet would be approximately 73 mm Hg (118-45). The PO2 of venous blood is approximately 40 mm Hg. Therefore, the diffusion gradient at sea level is equal to 65 mm Hg (105-40) and at 6,000 feet this gradient is 33 mm Hg (73-40). Patients with congestive heart failure and respiratory distress syndrome, among others, would be severely compromised when this drop in the diffusion gradient occurs.
Most fixed-wing aircraft utilized in air transport are pressurized, which allows for a comfortable cabin atmosphere when flying at higher altitudes. Generally, the lower the plane is flying, the lower the cabin altitude that can be achieved. This ability to maintain a physiologically comfortable environment within the aircraft minimizes the effects of altitude changes upon the patient. Rotor-wing vehicles are not pressurized, so these atmospheric changes impact the patient whenever the helicopter ascends. Therefore, the patient transported by helicopter may be at greater risk than those patients transported by fixed-wing aircraft. However, altitude gains are usually minimal and most patients are able to tolerate these changes [1].
Histologic hypoxia occurs in patients whose hemoglobin molecule is bound by molecules other than oxygen. There is an absence of oxygen at the tissue level leading to severe hypoxic events. Causes of histologic hypoxia include carbon monoxide poisoning, cyanide poisoning, as well as heavy smoking [2]. As an example, a burn patient who suffers from carbon monoxide poisoning requires air transport to a burn center. This patient is transported by air and encounters the effects of hypoxic hypoxia in addition to histologic hypoxia. The patient is at severe risk of sustaining life-threatening low PaO2 levels.
When a patient has an inadequate amount of circulating hemoglobin, he is said to have anemic, or hypemic, hypoxia [2]. Causes of anemic hypoxia include anemias and hemorrhage. A drop in hemoglobin to 10% or a hematocrit of less than 30 is most often associated with anemic hypoxia. These patients should be monitored for an adequate oxygen level to prevent further compromise in the patient's status. A commonly utilized monitoring technique is oxygen saturation. However, it is important to remember that oxygen saturation is only a measurement of the hemoglobin saturation. As an example, a patient with an oxygen content of 19 volume percent with a 20 volume percent capacity will have an oxygen saturation of 95%. This same patient could lose half of his blood volume so that the oxygen capacity would be 10 volume percent. If his oxygen content is 9.5 volume percent, his oxygen saturation is also 95%.
Stagnant hypoxia is caused by inadequate circulating hemoglobin. Different from other states, the patient with stagnant hypoxia has an adequate supply of oxygen and hemoglobin; however, it is not adequately circulated [2]. Examples of patients with a predisposition to stagnant hypoxia include those with low cardiac outputs (heart failure), hypothermic patients, and patients in hypovolemic shock. Additionally, the stressors of acceleration and deceleration forces (to be discussed at length later in this course) further compromise circulatory status in these patients.
Signs and symptoms of hypoxia include changes in vital signs, tachycardia, pupillary constriction, confusion, disorientation, and lethargy. Insidious and gradual in development, these signs may also be caused by a number of other illnesses and injuries, making the diagnosis of hypoxia more difficult. Astute observation of the patient is necessary to detect and correct the problems of hypoxia.
A great deal of research has been performed upon the effects of hypoxia on normal individuals. The military uses this information to establish guidelines for pilot performance. This research demonstrates what is referred to as time of useful consciousness (Table 2). This is the time in which a person subjected to a hypoxic environment can function to protect themselves from the harmful effects of hypoxia. Most commercial aircraft and aircraft utilized in air transport fly below 41,000 feet, indicating that the pilot will have a little less than 300 seconds to protect themselves from these detrimental effects in the event of cabin depressurization. Utilizing this information, the Federal Aviation Administration (FAA) has set requirements for oxygen use among pilots and occupants that state that oxygen use is mandatory for pilots when cabin pressure altitude is 12,500 to 14,000 feet for durations of more than 30 minutes or any duration at cabin pressure altitudes greater than 14,000 feet, and that oxygen must be available for all persons on board if the cabin pressure altitude is greater than 15,000 feet [3]. In a pressurized aircraft with two pilots at the controls, pilots must have their oxygen masks readily available to them in the cockpit (quick-donning type, ready within 5 seconds, and able to be placed on face with one hand) if flying at an altitude between 35,000 and 41,000 feet [3]. If at any time there is only one pilot at the aircraft controls and the altitude is above 35,000 feet, he or she must wear and use supplemental oxygen until the second pilot returns to his/her controls.
Prevention is the best approach to dealing with possible hypoxia development. Before transporting a patient by air, stabilization measures can be undertaken to help reduce the effects of hypoxia. Supplemental oxygen should be provided. If the patient has previously required oxygen, the oxygen percentage can be increased. This increase in oxygen delivery is performed as a prophylactic, temporary measure, and upon arrival at the receiving institution, the oxygen can be decreased or terminated as the patient's condition warrants.
Proper positioning of the patient combats the effects of hypoxia. The head of the stretcher may be elevated if not contraindicated by the patient's condition. However, in rotor-wing aircraft this elevation is often not possible due to the size of the cabin and placement of the patient within the helicopter.
Patients experiencing anemic hypoxia can be transfused to increase the hematocrit and improve the oxygen carrying capacity of the blood; however, this measure should not cause a delay in commencing the transport. Additional interventions include providing a calm environment while explaining all procedures and noises to the patient. Often, the patient's hypoxia worsens due to anxiety precipitated by the psychologic stressors associated with transport. Monitoring the patient's vital signs and observing for the signs associated with hypoxia will allow the transport personnel to monitor the patient's response to hypoxia. Portable arterial blood gas analysis may be available in certain transport programs; however, machinery does not replace assessment, and astute observation is paramount.
As an aircraft ascends, atmospheric pressure decreases and gas expands (Boyle's law). Gas expansion can be directly measured; 100 cubic centimeters (cc) of gas at sea level will expand to 130 cc at an altitude of 6,000 feet, to 200 cc at 18,000 feet, and to 400 cc at 34,000 feet. Gas expansion is a potential problem in all transports that ascend, but is especially harmful to patients transported in unpressurized aircraft flying above 12,000 feet.
Air can be present in many places in the body and in support equipment during patient transport, including the pleural space when a pneumothorax is present, air splints, and endotracheal tube cuffs. Pretransport stabilization measures can be instituted to prevent air expansion complications from hampering patient outcomes.
A pneumothorax that is recognized prior to transport should be treated with either a chest tube or, if chest tubes are impractical due to environmental limitations, a flutter valve attached to a one-way valve (Heimlich valve). Endotracheal tube cuffs should be monitored during transport as the air in the cuff will expand. The cuff may be partially deflated on ascent to prevent tracheal damage. (It is important to remember that gas can significantly expand during ascent and then decrease during descent. If air is removed, such as from an endotracheal tube cuff, it should be reinflated upon descent.)
Air splints should have air removed during ascent and replaced during descent. If this simple maneuver is overlooked, the splints become very tight, compromising the patient's circulatory status.
The gastrointestinal (GI) tract contains a great deal of gas. A nasogastric tube placed prior to transport will decrease gas expansion and reduce the risk of vomiting. A patient with a colostomy or ileostomy can have a rectal or nasogastric tube inserted into the stoma to reduce gas expansion in the lower bowel.
The patient may complain of dental pain from dental caries (tooth decay) that have not been managed appropriately. Little can be done during transport to ease the patient's pain except the administration of pain medication. The patient may also complain of ear pain (this is most common among the pediatric population). Expansion of gas trapped in the middle ear can be treated with vasoconstrictor nasal sprays and by assisting the patient with maneuvers to clear their ears. One useful procedure in the pediatric population is to have the child suck. A small child can suck on a pacifier, and if not contraindicated, an older child can have a small amount of liquid through a straw. The sucking motion helps relieve the pressure. Performing the Valsalva maneuver often assists with clearing the middle ear.
Finally, equipment can have gas inside that will expand. Glass intravenous (IV) bottles have air inside, and as the aircraft ascends, the gas expands and the rate of fluid delivery increases. The bottle should be vented in order to achieve proper functioning. However, a safer technique is to utilize plastic IV bags that do not contain air and also do not present a hazard during unexpected turbulence.
Most of the complications of gas expansion occur during fixed-wing transports as the altitude achieved is much higher. However, gas expansion can occur in helicopter and ground transports that traverse high mountain passes. It is essential to perform the interventions described above whenever the transport involves significant changes in altitudes.
A drop in ambient humidity also occurs with an increase in altitude. This loss of humidity is enhanced in a pressurized aircraft; cabin pressurization is achieved by introducing compressed air from the engines, recycling the air, and removing moisture to protect the aircraft and its electronic systems from corrosion. Ambient humidity in a pressurized aircraft after one hour of flying time is less than 5%.
Patients who are dehydrated or diaphoretic are at increased risk for dehydration, causing a further decrease in their circulating volume. A dry environment is also harmful to a patient's respiratory tract, as drying of the mucous membranes and loss of ciliary action can lead to an increased risk of respiratory tract infections.
Providing adequate hydration to the patient during transport can minimize the effects of dehydration. Ensuring adequate circulating volume prior to transport will ensure that the patient is stabilized appropriately. Adding humidification to the oxygen delivery system throughout transport will counter the drying effects of oxygen.
The standard lapse rate for temperature is that for each 1,000-foot gain in altitude there is a 2 degree centigrade drop in temperature, until the temperature reaches negative 55 degrees centigrade. The harmful effects of a decreasing temperature arise when the fuselage of the aircraft becomes cold. This cold is transmitted through the cabin walls causing the interior to cool. The coldest area in the aircraft is against the outside walls, where the patient stretcher is usually secured. An unconscious patient will not be able to report being cold and the effects of hypothermia may be subtle. An additional factor that impacts this concept is that the transport personnel are working and producing heat; their body temperature may actually feel warm and, therefore, they do not recognize that the environment has cooled significantly.
Although this problem is greatest during the colder winter months, the effects of the drop in temperature are experienced year-round. A drop in body temperature causes a decrease in the patient's level of consciousness and can produce shivering. The decrease in the patient's level of consciousness can be attributed to a number of factors, including hypoxia, dehydration leading to a decreased circulating volume, and a decreased temperature. Because the transport personnel have limited resources available to them to determine the cause of patient deterioration, they should assume that the problems of transport are compromising the patient and intervene to correct these problems.
Decreased temperature is not solely an altitude-induced problem. During a transport, a patient is subjected to a number of environmental changes. As an example, a patient may be injured at a scene of an accident and not found for a period of time. During this delay in receiving medical care, the patient becomes hypothermic. He is subsequently found, stabilized, and transported by ground ambulance to the nearest facility. During ground transport, the transport personnel heat the interior of the ambulance and work to maintain the patient's body temperature. Upon arrival at the hospital, the staff works to warm the patient. During evaluation of the patient's injuries, the determination is made to transport the patient to a trauma center, which is located 250 miles away. Arrangements for air transport are made and the patient is stabilized for transport. At this point the patient's temperature may be stabilizing; however, he is then transported from the hospital to an ambulance and transported from the ambulance to the aircraft. During air transport the patient again becomes hypothermic due to the decreased temperatures at altitude. Finally, before arriving at the Trauma Center, he is again transferred out of the plane and into another awaiting ambulance. The patient has been subjected to at least seven different environments, and if these transfers occurred in the middle of winter, it is obvious what this can do to impact the patient's condition.
Paramount to preventing temperature changes in patients is awareness of the ambient temperature. Minimizing the patient's exposure during transfer is of utmost importance. Maintaining an adequate supply of linens to warm the patient is helpful. Burn patients are at great risk from environmental changes and may benefit from the use of a rescue (Mylar) blanket. Pediatric and elderly patients are prone to hypothermia, and using a hat will help reduce up to 10% of radiated heat loss [4].
An additional complication that occurs with a decrease in temperature is that air molecules contract when cold. This is the opposite of the effects that occur with an increase in altitude as previously discussed. In a cold environment, air splints may deflate, thereby losing their effectiveness. This is most often encountered when a patient is in air splints and is removed from a warm hospital to the cold air outside. Each time the environmental conditions change, the effects on gas expansion or contraction should be compensated for.
Cold environments also impact IV solutions and medications, most notably those containing mannitol. Solutions stored in the aircraft are quite cool and should be warmed prior to administration. Mannitol may crystallize when cooled, rendering it useless. These solutions should be stored in the warmest spot in the cabin (usually the cockpit) and, if necessary, rewarmed. Warming of IV fluids can be done by utilizing a heat pack that is wrapped around the IV bag and part of the tubing. While this method will not assist in rewarming a hypothermic patient, it will prevent the administration of cold fluids. Mannitol is usually not stored in the aircraft in cold locales; it is considered to be one of the items that is loaded into the aircraft immediately prior to departure.
Time/temperature indicator (TTI) labels that can monitor mean kinetic temperatures, allowing for assessment of potential or real pharmacologic degradation, are used in clinical evaluations. With this type of measurement method, flight crews would be assured that the medications stored onboard the transport vehicle are safe and effective for patient care.
Acceleration and deceleration forces occur in all methods of transport; the severity and angle of these forces varies by vehicle type. Acceleration forces occur on takeoff, climb-out, or when a ground ambulance speeds up. These forces can produce what is known as positive G forces. These forces can be significant enough to cause fluid shifts in severely compromised patients. Blood pools in the dependent areas, most commonly the legs. The effects of positive G forces can produce what is known as "grey-out." This is a phenomenon that occurs when there is an inadequate circulating blood volume to the head, essentially causing the individual to faint momentarily. As soon as normal circulation is established the patient's level of consciousness returns to its previous state.
Deceleration forces occur upon slowing down, stopping, or during a rapid descent. As most patients are positioned in the transport vehicle with their head forward, these forces produce negative G forces, or "red-out," which is a rush of blood to the head. The term red-out was coined when this phenomenon was noted to produce a momentary reddening of the sclera in the eye as intraocular blood volume increased. Negative G forces are most harmful to the patient with increased intracranial pressure. This rush of blood to the cranial cavity causes a sudden, abrupt rise in intracranial pressure and subsequent deterioration in the patient's level of consciousness.
The effects of acceleration and deceleration forces vary with the speed, angle, and duration of the forces. Military pilots are subjected to these forces on a frequent basis and have developed a tolerance to them. These forces are most pronounced in a fixed-wing transport on either takeoff or landing. In certain situations; the pilots have some control over these factors, such as obtaining a slow rate of descent and having a longer landing roll. These issues are discussed with the pilots prior to departure and the pilots will work with the air traffic controllers to try to achieve the maximum benefit for the patients, while working within the constraints of the environment and vehicle performance.
Positioning the patient is crucial to limiting the effects of these forces. In most aircraft the stretcher should be secured with the head forward, requiring that the patient be placed in this position. If the patient can tolerate a head-elevated position, this will limit the abrupt rise in intracranial pressure that occurs during deceleration. Elevating the feet of the patient during takeoff can prevent fluid accumulation in the patient's feet during acceleration.
Lateral forces are a possibility, though rare, during helicopter transport. Usually, these lateral forces are of little consequence; many times the patient and crew are unaware of this type of movement. Lateral forces can also be experienced in ground transport while turning a corner. However, the driver of the vehicle should maneuver in such a manner that these forces do not harm the patient and crew.
Often patient transfers involve long distances and, therefore, long transport times. The patient who is immobilized on a stretcher throughout a transport (either by land or by air) is subjected to a number of factors, including pressure sore development and venous stasis. Space limitations and the inability to change the patient's position exacerbate this problem. Patients at increased risk for complications include trauma patients, the elderly, and any patient with previously compromised circulatory status.
The patient at greatest risk is the patient with a spinal cord injury requiring transport on a backboard. It is important to remember that the time of immobilization is not only the length of the transport; ground transport times, unexpected delays, and transfer times should also be considered. As an example, a patient is injured in a motor vehicle accident at a remote site and is secured to a backboard to protect the cervical spine. The patient is then transported to the local hospital for stabilization and evaluation. The decision is made that the patient requires the expertise only available at a trauma center and arrangements for transport are initiated. During the evaluation of the patient, the x-rays are inconclusive and the patient is to remain on the backboard until a definitive diagnosis can be reached. Subsequently, the patient is taken by ground ambulance to the local airfield, flown to the airfield near the trauma center, and is again transferred by ground ambulance to the trauma center. The length of time from the scene of the accident to the trauma center may exceed 5 to 6 hours, although flight time was less than 1.5 hours.
Signs of poor perfusion are often difficult to assess during transport. Lighting is less than optimal; therefore, assessment of extremity color and capillary refill are hampered. The patient may complain of tingling or numbness in a compromised area; however, the patient with a decreased level of consciousness would be unable to report these sensory changes. Doppler monitor ultrasound can be utilized to assess for the presence of pulses in distal extremities. The absence of pulses requires further investigation of the cause and interventions to improve circulation.
The patient who is secured to a backboard runs the risk of pressure sore development in a number of locations. The most common pressure areas include the coccyx and sacral areas. Additionally, the scapulae are prone to compromised circulation. A patient in a hard cervical collar for spinal cord immobilization should be monitored for pressure sore development at the angles of the jaw and at the occiput of the skull.
Before departure, all splints, casts, and pressure areas should be padded. The patient on a backboard can have a small towel or pad placed under their back and coccyx area without risking a change in spinal cord alignment. During transport, proper positioning should be accomplished and, if possible, range of motion within the constraints of the vehicle can be performed. Constant vigilance of the extremities and areas of high risk before, during, and after the transport is required to prevent pressure sore development.
Changes in inner ear equilibrium caused by unusual movements are the primary cause of motion sickness. However, other causes can include: hypoxia, excessive visual stimuli, stress, fear, unpleasant odors, heat, and poor diet. Gastric gas expansion that occurs on aircraft ascent can further potentiate the problem.
Nausea and vomiting are the two most common symptoms of motion sickness; other signs include chills and headache. In the transport environment, all persons are at risk of motion sickness, including the transport personnel. Those individuals who have a predisposition to motion sickness may prophylactically premedicate with transdermal patches. The problem that arises with the use of these patches is that, to be effective, they should be applied a half hour or more prior to departure; however, since these transports are generally not planned, this preventive measure may not be feasible.
To prevent or limit the effects of motion sickness, transport personnel should apply oxygen and ensure that the individual is in the supine position. Staring at a fixed object will help reduce the inner ear imbalance that precipitates the problem. Cooling the interior of the vehicle also will help reduce the symptoms. In severe cases, insertion of a nasogastric tube to suction will reduce gastric contents and vomiting.
Interestingly, transport personnel rarely, if ever, experience the symptoms of motion sickness while caring for a patient in transport. Most cases of crew motion sickness occur while on the way to pick up a patient. It appears that the concentration and work involved in caring for the patient helps overcome these complications.
All transport vehicles are noisy. Engine noises create a constant loud hum; sirens in a ground ambulance are very loud and of a harsh intensity. Constant noise can create a stressful environment as well as increased irritability in all persons in the transport vehicle. Patients who are exposed to this constant input experience changes in their vital signs, including tachycardia and hypertension.
Reduction of environmental noise can be accomplished in a number of ways. Flight crews in helicopters utilize headsets to reduce noise input, as well as to allow for communication with other crew members. Headsets can also be used for the patient; however, it should be remembered that when noise reduction techniques are utilized on the patient they cannot hear normal conversation. This may prevent the patient from appropriately answering questions, as well as increase their anxiety when they assume that the crew is talking about them and they cannot figure out what is being said.
Cotton balls are the simplest form of noise reduction. However, they are easily forgotten when the patient arrives at the receiving hospital and communication may be difficult for this very simple reason. Another method employed to help the staff with the noise is the use of Doppler monitor devices to assist in obtaining vital signs or to assess for air movement through the trachea. A stethoscope may be rendered useless in obtaining vital signs in a very noisy environment, but it can assist in communicating with the patient. By placing the ear pieces into the patient's ears and speaking at the diaphragm, the patient may be able to better communicate with the crew.
The noises heard in ambulances, helicopters, and airplanes may be familiar to the transport crew; however, these same noises may produce fear in the patient. It is essential that the crew communicates with the patient, explaining all noises and lights. A preflight briefing will help alleviate some of these fears.
Motion produces vibration. All transport vehicles are affected by vibration. However, this is most noticeable in a helicopter, especially during takeoff and landing. The biggest risk of vibration is the loosening of safety straps so that during a time of turbulence, equipment can come loose and pose a hazard to the safety of all. FAA regulations require that all equipment be secured for takeoff and landing in helicopters and airplanes; however, it is wise to keep all equipment secured at all times in the event of unexpected turbulence.
The patient should be secured onto the stretcher at all times. The safety straps used to secure the patient may be quite uncomfortable for them; during transport, these straps can be loosened slightly but should never be removed completely. The greatest risk comes to patients as they are being moved into and out of the transport vehicle.
Another problem with vibration is its effect upon equipment settings. Over time, constant vibration can cause a loosening of screws, so that equipment does not function properly. Mechanical ventilators are most prone to this complication; settings should be checked frequently during transport.
A rare and unexpected complication that can occur in a pressurized aircraft is the rapid loss of pressurization. This is an emergency situation in which the pilots of the aircraft will immediately put the aircraft into a steep descent to reduce the effects of atmospheric changes. When an aircraft loses its pressurization, the cabin pressure altitude immediately goes from its comfortable flying altitude (between 3,000–6,000 feet) to equilibrate with the altitude outside the aircraft (this can be up to 25,000–40,000 feet). The sudden decrease in cabin pressure produces all of the effects of altitude increase, including hypoxia, gas expansion, decreased temperature, and dehydration, with hypoxia causing the largest risk.
The immediate effects of a loss of pressurization depend upon the altitude of the aircraft at the time of the emergency; the higher the airplane, the greater the complications. The patient and crew could experience a number of problems including a ruptured eardrum, a drop in body temperature, and possibly wind burn, if the cause is due to a loss of a piece of the fuselage.
Decompression sickness is manifested by joint pain (the "bends"), paresthesias, central nervous system changes (e.g., headache, visual disturbances), and the "chokes" (a choking sensation). These symptoms are caused by the release of nitrogen bubbles into the blood stream.
Initially, when a loss of pressurization occurs, the crew is trained to put on their oxygen masks and protect themselves first. The pilots will don their oxygen masks and put the plane into an immediate descent. The crew should ensure that all equipment is secured and does not pose a hazard during this descent. The patient should have oxygen administered, or increased if he or she had previously been receiving oxygen. Symptoms of decompression sickness can be treated with oxygen therapy, or in severe cases, a decompression chamber with hyperbaric oxygen therapy.
Although rapid cabin decompressions rarely occur, transport personnel can now obtain training in handling of this type of emergency. The FAA and the U.S. Air Force have a joint training agreement to offer hypobaric chamber training to civilians at several U.S. Air Force Bases throughout the United States. This type of training allows the participants to experience the effects of decompression and the hypoxia associated with this untoward event, with the intent of being sufficiently trained in symptom recognition to protect themselves and their patients.
These ten stressors of transport are problems for all patients, some to a greater extent than others. Awareness of their probability and interventions to prevent their occurrence will limit the detrimental effects to the patient. Appropriate stabilization prior to transport will ensure that these effects will be minimized. Further stabilization measures will be discussed at length later in this course.
Local, state, and federal regulations all impact transport of patients, both in the air and on the ground. Healthcare providers who are facilitating a transport should be aware of how these regulations affect their choice of transport vehicle, as well as their legal responsibilities before, during, and at the end of the transport.
Ground ambulance regulations are developed at the state level by the Emergency Medical Services (EMS) office. These regulations can vary by state, but should meet the minimum standards as outlined in federal regulations. Most often these state regulations far exceed the minimum standards; however, they do vary significantly from state to state. Regulations are set for basic life support ambulances that are capable of providing advanced critical care measures. The equipment and training of the transport crew will vary depending on the services provided. Patient needs will dictate which type of transport vehicle is required for each transport.
Air ambulance operations are regulated by the FAA and should meet the requirements of a portion of the aviation regulation known as Part 135. These regulations stipulate the qualifications of the pilot-in-command and other flight crew members, maintenance requirements, and aviation management. Part 135 contains some of the most stringent of all the FAA regulations. Additionally, air transport crew members should be cognizant of the Federal Aviation Regulations (FARs) concerning in-flight safety and emergency procedures.
States may also regulate air ambulance operations within their state. To obtain licensure as an air ambulance, the transport program should meet certain minimum requirements. Although not required in all states, the legislative trend is to regulate the air ambulance operators to minimize the presence of those operating capricious services who believe they can make some extra money by transporting patients.
Accreditation is also available through the Commission on Accreditation of Medical Transport Systems (CAMTS). This is a voluntary review of an air transport program to ensure their compliance with patient care and safety standards. These standards are revised every two to three years. As of May 2022, there were 162 accredited medical air transport services in the United States [16].
Federal regulations also stipulate the requirements for the need to transport patients. These requirements were first introduced in 1985 as part of the Consolidated Omnibus Reconciliation Act (COBRA) and were subsequently amended in 1995 as a portion of the Medicare law, Emergency Medical Treatment and Labor Act (EMTALA). These laws state that all patients should have equal access to care and require the hospital to ensure that proper care is provided. If the hospital is incapable of providing care, arrangements should be made to transport the patient to a hospital with appropriate facilities. To ensure that the transport is performed in a safe and expeditious manner, the following conditions should be met [5]:
The transferring hospital has provided medical care within its capacity to minimize risk to the patient's health.
The receiving hospital has agreed to accept the patient and has the space and resources available for treatment.
The transferring hospital sends available medical records with the patient.
The transfer is affected through qualified personnel and transportation equipment.
It is the responsibility of all persons caring for patients to see that these regulations are followed.
The transfer of patients requires preplanning in order to ensure that both the medical needs of the patient and federal requirements are met. Referring facilities should first assess their capabilities and recognize their limitations for patient care. When a patient is admitted who exceeds these capabilities, an interfacility transport should be effected. Assessment should include, but not be limited to, staffing, equipment capabilities, advanced diagnostic techniques, and the availability of in-house specialty care. Most patients' needs are well within these capabilities; however, it is important to recognize those patients whose needs exceed the available resources.
The receiving facility should also be assessed as to their capabilities for caring for the needs of the patient. As an example, trauma patients are best cared for in facilities that are designated trauma centers as verified by the American College of Surgeons Committee on Trauma. It is important that each area of care be individually assessed as to how they will meet the individual patient's needs.
Transferring a patient from one facility to another must meet the federal mandates of COBRA. Each institution should have protocols established for the referral and acceptance of transported patients. Physician-to-physician contact should be initiated prior to departure of the patient to the receiving facility. These physicians jointly share in the legal responsibility for the transport and should establish guidelines for patient care.
The risks and benefits of the transfer should be explained to the patient (or patient's legal representative), and a consent form should be signed to indicate that the patient has been informed. In the event that a patient is unable to give consent due to their medical condition, and no family or next-of-kin can be located, the patient can be transferred under the implied consent law. The law assumes that the patient would give consent if able. However, it is imperative that a concentrated effort be undertaken to locate family members before this type of consent is invoked.
After the determination has been made that a patient requires transport, there are a number of steps to be taken to ensure safe transport. The referring facility should choose the appropriate transport vehicle, ground, helicopter, or fixed wing. When a dedicated transport program is available, this decision is usually made by general agreement between the referring physician and the transport program. Air transport cannot be chosen indiscriminately; many third-party payers will only cover the cost of air transport when it is deemed medically necessary. The following is a list of steps that comprise an interfacility transfer:
Physician-to-physician communication
Selection of the appropriate mode of transport and personnel to accompany the patient
Signed consent for transfer, signed by the patient or legal representative
Stabilization of the patient to limit the stressors of transport
Completed documentation
Development of a plan of care to be provided in transport
Communication with all involved personnel and family
Transfer of care is not complete until the staff on the receiving unit has received a full report of the patient's status, and has received the appropriate documentation. The verbal report should include the patient's history, current illnesses or injuries, care received during transport, patient's responses to the transport, and any known plans for care at the receiving facility. Additionally, the receiving staff should be informed of the status of the patient's family, where they are, how to locate them, and if they are planning on arriving at the receiving facility.
The transport crew should turn care of the patient over to the receiving hospital staff immediately upon arrival. The transport crew members should not be delegated to deliver care to the patient once they have arrived at the receiving unit.
Before transfer is complete, a transport team member should notify the transferring facility of the safe arrival of the patient. Also, the patient's family should be notified that the patient is safe at the receiving hospital. Once all parties are notified, the transfer of care is complete.
Airway patency during transport is of primary importance. Potential airway compromise should be anticipated before transport so that proper interventions can be undertaken to ensure that the airway is protected. Performing airway maneuvers in a transport vehicle are, at a minimum, challenging and often are unsuccessful.
Endotracheal intubation should be considered in any patient who has the potential to lose their airway due to aspiration, swelling, or edema. This may include patients with facial or neck burns, epiglottitis, facial fractures, or patients with an altered level of consciousness. Patients requiring mechanical ventilation and ventilatory support should be intubated in a controlled environment prior to departure. Examples of these patients include spinal cord injured patients, patients with chest wall injuries, or patients with other neurologic dysfunction.
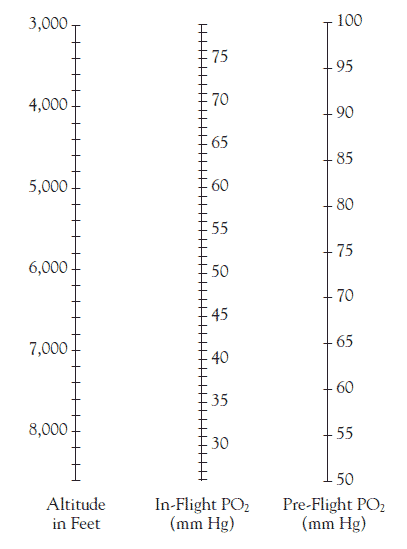
Supplemental oxygen should be contemplated and is usually considered to be standard therapy during transport. All patients transported by air are at risk for hypoxia, as previously discussed, and should be considered as candidates for oxygen therapy. Figure 1 shows the predicted in-flight PO2 for a patient, based upon his arterial blood gas results and the altitude at which the patient is to be transported (i.e., cabin altitude in a pressurized aircraft). You will note that a significant drop in the patient's oxygenation status occurs. As a general rule, it is estimated that inspired PO2 declines approximately 5 mm/Hg per 1,000 feet ascended [6]. Unfortunately, no consensus formula exists to accurately predict PO2 decline or how much the oxygen percentage should be increased to combat this drop in oxygenation [7,8]. Transport team members should rely on their astute assessment of the patient's color, capillary refill, and oxygen saturation results to determine how the patient is tolerating the transport.
Chest tube placement may be accomplished prior to transport to decompress a pneumothorax. The patient who is being transported by air will have expansion of the pneumothorax if it is not treated prior to departure. In cases of an undetected pneumothorax, a flutter valve attached to a one-way valve can be placed to prevent further decompensation in the patient. A closed drainage system should be attached to the chest tube and a one-way valve should be in place to prevent complications should an accidental disconnect occur.
Maintenance of normal vital signs and circulating status is the goal of hemodynamic stabilization. Initially, control of bleeding should be instituted followed by volume resuscitation. Depending on the patient's status, two large-bore IVs should be initiated prior to transport; insertion during transport is very difficult.
Control of bleeding can be accomplished by a number of methods. Pressure dressings can be applied; however, the transport team should ensure that their supply of dressings is adequate in the event that the dressings become saturated and require replacement.
IV fluid resuscitation can be accomplished with one or two IV lines. Murphy's Law applies in the transport environment: if you have only one IV line it will become dislodged, if you have two lines they will both stay in. As noted, plastic IV bags are recommended; the problems of gas expansion are negated and, in cases of significant motion, a glass bottle could easily break.
Blood products can be administered in transport. Care should be taken to prevent the spoilage of blood; a cooler is usually adequate to keep blood cool prior to administration.
Monitoring urine output is one of the best indicators of the patient's fluid status. Insertion of an indwelling catheter will assist the transport crew with frequent assessment of volume status. Additionally, an indwelling catheter will relieve patient discomfort during long transport times.
Cardiac rhythm status should be frequently assessed using a transportable cardiac monitor. Continuous monitoring should commence prior to transport and continue throughout the transfer.
Deterioration of the patient's level of consciousness should be avoided during transport. Many of the stressors of transport induce rises in intracranial pressure. The transport crew should intervene to prevent this occurrence.
Prior to departure, an assessment of the patient's neurologic status should be completed. Utilizing the Glasgow Coma Scale, or other neurologic assessment scales, can assist in providing continuous information regarding patient condition. Medications, such as cranial volume reducers, can be initiated and continued in transport.
Any patient experiencing seizures should receive antiseizure medication. One of the most common causes of prolonged seizure activity is hypoxia; this condition worsens during air transport.
Patients with spinal cord trauma and neurologic deficits need special attention during transport to prevent further deterioration in neurologic status. Spinal precautions should include the use of a backboard and hard cervical collar. As discussed, pressure sore development is a common complication during long transports and care should be taken to pad all bony prominences. Administration of methylprednisolone or similar medication for spinal cord injury is a requisite and should be initiated and subsequently continued throughout transport.
Care in transport of the patient with musculoskeletal injury should include immobilization of fractures, wound care, and the proper administration of medications as ordered or required.
Appropriate splints should be applied prior to departure. Throughout the transport, frequent assessment of distal pulses should be performed. Air splints and pneumatic antishock garments should be monitored for the effects of gas expansion and changes in atmospheric temperature. Traction splints can be utilized; the use of traction weights is generally avoided as the weights can pose a hazard during unanticipated movement.
Extensive wound care is not possible in the transport environment. The transport crew members should act to preserve the integrity of a wound and prevent further contamination. A wound should be dressed and the dressing reinforced as necessary.
Patients requiring transfer for limb reimplantation require special care. The amputated part should be preserved by wrapping it in slightly moistened gauze and placing it into a plastic bag. The plastic bag should then be placed into a plastic container, such as an emesis basin or urine collection cup. This container should then be placed on ice in a cooler. The amputated part should not be allowed to freeze, as tissue destruction can occur, preventing the reimplantation.
Burn wounds causing a disruption of tissue integrity need special attention. The risk of contamination is great and interventions should be undertaken to reduce this risk. Further discussion of the transport of burned patients can be found later in this course.
After the physical needs of the patient who is about to be transported have been met, the emotional and psychologic aspects of transport should be addressed. If the patient and his or her family have fears or questions, intervention prior to the start of the transport can alleviate many of their worries.
It is vital that any counseling or other interventions take into consideration patients' cultural or linguistic barriers. When there is an obvious disconnect in the communication process between the practitioner and patient due to the patient's lack of proficiency in the English language, an interpreter is required. Interpreters are more than passive agents who translate and transmit information back and forth from party to party. When they are enlisted and treated as part of the interdisciplinary clinical team, they serve as cultural brokers, who ultimately enhance the clinical encounter. In any case in which information regarding transport options or expectations during a procedure are being provided, the use of an interpreter should be considered.
Patients who are transported are moved away from their family, friends, and familiar medical care providers. The need to be transported can be interpreted by the patient and family to mean that the patient is dying. While often this is true, patients are transported for a number of reasons with a variety of illnesses and injuries, and most do survive after reaching a healthcare facility that is capable of meeting their needs. The fear of dying is very real to the patient and family and should be addressed immediately after the decision to transport has been made. Healthcare providers cannot overestimate the capabilities of the receiving hospital, but an honest, forthright approach is appreciated by all involved.
The fear of death is only one of many feelings that the patient and family may be experiencing. If the patient is to be transported by air, they may have a fear of flying. The patient and family may be afraid that they will never see their loved ones again, and sometimes the resulting anger and resentment is directed at the referring hospital and healthcare personnel. The patient and/or family may feel that if the transferring hospital was better equipped, the need for the transport would be negated. It is the responsibility of the transporting crew to help the patient rebuild trust in their hospital; if the patient survives, they will most likely return to that home community for further healthcare needs.
The fears that the patient and family feel increase anxiety, which in turn can cause changes in the patient's status. The patient may become tachycardic, hypertensive, and may hyperventilate, all of which will compromise their illness or injury. Another complicating factor is pain; the patient whose pain is not well-controlled is incapable of handling the emotional impact that is placed upon them. It is important that the referring personnel, as well as the transport crew, provide adequate pain relief. The complications of narcotic delivery, such as pupillary constriction, may mask or confuse the signs of hypoxia, but uncontrolled pain is unacceptable and should be managed appropriately.
Family of the patient may develop what has been referred to as "Mecca syndrome." This is an overinflated idea of what can be done for the patient at the receiving hospital. The family wants to believe that the receiving hospital is flawless and can save or cure anyone. While the receiving hospital has greater capabilities than the transferring hospital in terms of diagnostic tools, equipment, and personnel, not all patients can be saved. Again, it is important to openly and honestly discuss the patient's condition and outcome with the patient as well as the family.
A family member may wish to accompany the patient during the transport. While this may initially appear to be a good idea, the transport crew should consider a number of factors prior to giving the go-ahead for an accompanying member. First and foremost, safety should be considered. A family member should have his or her own seat and be able to be secured with approved straps in the transport vehicle. Accompaniment is almost always impossible in a helicopter. Not only is there no room in the cabin for the family, the additional weight may put the helicopter over its operating weight and balance capabilities.
Another important consideration is patient status. A critically ill or injured patient may decompensate during transport and the presence of a family member may be detrimental. The family member will not be able to leave the transport vehicle, and will be present while possibly unsuccessful interventions are performed. Some family members try to be helpful while in reality they are in the way. Another problem is the family member who may develop motion sickness during the transport. The members of the transport team are responsible to the patient who is being transported; they may not be able to assist the family member because they are busy caring for the patient.
If a family member is to accompany a patient, they should receive a complete safety briefing prior to departure. The expectation of what they can and cannot do should be addressed. If time permits, they should be told to gather a few personal items to take with them, as their stay at the receiving facility may be a long one. Family members can be of benefit and included in the transport once these issues have been addressed. A parent is often very beneficial in comforting the pediatric patient. Additionally, once the patient has arrived at the receiving hospital, the parent is immediately available for decision-making and consent. While care is generally not withheld if a parent is not present, their presence is often appreciated by the receiving hospital staff.
The final decision as to whether a family member may accompany a transport is at the discretion of the transport crew. Often, individuals at the referring hospital tell family members that they can, only to be told at the last minute that they cannot accompany the patient. In an air transport, the pilot-in-command has the final decision-making authority. The decision is based upon weather and aircraft performance capabilities. In a ground transport, the transport crew member in charge is responsible for making this decision.
If a family member chooses not to accompany the patient, or is told that they are not allowed to be part of the transport, time should be made available for the family to say their good-byes to the patient. This may be the last time that the family sees the patient alive; the few seconds that it takes to share a last kiss or hug may make a tremendous difference in the family's ability to recover from the death. Prior to departure, the family should receive as much information as possible about the receiving hospital. Maps, telephone numbers, and plans for patient admission should all be included in this information. Additionally, the family should be informed of the estimated time of the transport and when they can expect to be notified of the safe arrival of their loved one at the receiving facility. It is imperative that the transport crew takes into consideration the weather, unexpected delays, and time zone changes. When providing the family with the estimated arrival time, it is always better to overestimate the time rather than to underestimate it. A telephone call that comes 10 minutes later than expected may seem like a lifetime to the waiting family. During this time, the family has imagined all types of horrible things that may have gone wrong in the transport, adding needless stress to their lives.
Studies performed prior to transport depend upon a number of factors. Prehospital transports do not usually have the luxury of diagnostic tools. Patient stabilization is performed with consideration of the airway, breathing, and circulation (ABC), the mechanism of injury, and the history of the illness or injury. Interfacility transports have the time and more capabilities available to the patient.
The patient's illness or injury and current status will impact which studies are performed. The patient's airway should be examined and stabilized. Chest x-rays may be obtained to rule out any pulmonary complications that can compromise the patient during transport. Arterial blood gases will detect any abnormalities in oxygenation that the patient may be experiencing. Baseline blood studies, including hematocrit, will allow for determination of the patient's hematologic status. In emergent situations, only the basic studies that affect ABC should be performed, as time permits. Studies that should be performed if time permits include:
Radiographs of cervical spine, chest, pelvis, and extremities that may be injured
Laboratory tests, including hematocrit, hemoglobin content, arterial blood gas measurements, urinalysis, toxicology screens, blood alcohol measurements, and blood typing and crossmatching
Electrocardiogram
Copies of all laboratory results, electrocardiogram, and radiographs should accompany the patient. These should be well labeled with the patient's name, time of the test, and notation of abnormal results. Additionally, samples of the patient's blood, peridialysis fluid, and spinal fluid should accompany the patient so that further testing may be instituted on these samples at the receiving facility. Any information that is not readily available at the time of the patient's departure patient should be telephoned or electronically transmitted to the receiving facility.
Documentation for transport includes information obtained during the prehospital period, the hospital phase of care, and during all phases of transport. Prehospital transport documentation should include, but not be limited to:
Mechanism of injury or history
Time of injury or onset of symptoms
Time to arrival of EMS
Care provided in the field
Care provided en route
Protocols or orders used during transport
Documentation and information that should accompany the patient who is being transported from one healthcare facility to another should include:
Prehospital care record
Emergency department record of care
Medical history, if available
Results of laboratory and diagnostic studies, as previously described
Copies of radiographs (not just the radiologist's report)
Transfer record
Protocols or orders used in transport
Signed transfer consent form
Family information (name, address, telephone number for contact person)
Name and telephone number of contact individual at referring facility
Name of physician ordering transport and name of physician who has agreed to accept the patient at the receiving hospital
The following discussion will examine eight patient populations who commonly require transport. Each disease process or injury will be reviewed and the ways in which the stressors of transport can affect each patient type will be discussed. Finally, each section will end with a case study. It is important to remember that during transport the patient cannot be fully evaluated and stabilized. Thus, the transport team's goal is to prevent further injury or compromise in the patient. Once the patient arrives at the receiving facility, an advanced level of care is instituted.
The neurologically compromised patient is placed at great risk during transfer. Although there are many complications that can develop, the need to transfer the patient prevails, and the transport crew should intervene to limit these untoward problems.
Neurologically compromised patients are greatly impacted by the stressors of flight, including hypoxia, gas expansion, and decreased temperature. Hypoxia causes an increase in intracranial pressure and should be avoided by providing supplemental oxygen. A patient with an open skull fracture and air in the cranial cavity is at risk of herniation with gas expansion. Barotrauma within the ears, caused by gas expansion, will not be apparent in the unconscious patient. A decreased environmental temperature can cause shivering, which increases the patient's oxygen requirements up to 300% greater than normal. Obviously, in a previously compromised patient, this is to be avoided. Dehydration is generally not a problem, unless the patient has been placed under severe fluid restrictions in an effort to limit intracranial pressure. In this instance, the added effects of dehydration may be enough to cause cardiovascular collapse due to an inadequate circulating volume.
The effects of acceleration and deceleration forces on intracranial pressure have previously been presented. The transport crew should be cognizant of these forces and intervene to limit their effects. Patients with a decreased level of consciousness are not able to protect themselves by turning to avoid pressure sore development during long transports. Vomiting, associated with motion sickness, is generally not a problem; unconscious patients do not seem to experience the same responses as conscious patients. However, if the patient who is alert complains of nausea, measures should be taken to prevent the patient from vomiting, which increases intracranial pressure. Finally, noise and vibration increase anxiety and fear and have a detrimental effect on neurologic status.
Stabilization of the patient requires the use of supplemental oxygen, often at 100%. Intubation should be considered for all neurologically compromised patients, and oxygen saturations and end-tidal carbon dioxide levels should be monitored. Fluid status should be monitored to prevent dehydration. Guidelines for the management of cerebral trauma recommend maintaining the systolic blood pressure at 90 mm Hg [9]. Patients with suspected cervical spine injury should be transported on a hard backboard with spinal immobilization precautions. Positioning the patient with the head of the stretcher elevated, if tolerated, will reduce the effects of acceleration and deceleration forces. Prior to transport, pressure areas should be padded, and during transport, the patient's position should be changed within the confines of the transport vehicle. The use of cotton ear plugs can reduce extraneous noise; however, the effects of vibration are unavoidable. Neurotrauma patients receiving mannitol should have a Foley catheter placed for urine drainage and measurement of output volumes.
The use of paralytic agents in the transport environment has come under a great deal of scrutiny. The loss of respiratory drive accompanying neurologic compromise requires that the patient receive continuous ventilatory support. The beneficial effects of neuromuscular blocking agents on intracranial pressure often support their use. A patient who is comfortable and secure can be safely transported, while agitated patients who are out of control can be a danger to themselves as well as the other crew members. It is important to remember that paralysis can cause the patient to appear calm; however, their psychologic needs remain great. Patients who are chemically paralyzed should receive supplemental sedation and analgesia [10].
Patient A, 18 years of age, sustains cervical spinal trauma when diving into a river. He has no demonstrated motor or sensory function below C3 and has no respiratory drive. He is rescued by a local ambulance crew and transported to the nearest facility, a small rural hospital with limited resources. The emergency room physician appropriately requests air transport of this patient to the Level 1 Trauma Center, located 350 miles away.
While awaiting transfer, Patient A is stabilized by the referring hospital staff. He had been placed on a backboard and in a hard cervical collar at the scene, and the staff ensure that he is well-secured to the board. His ventilations are continually being assisted through an endotracheal tube. Admission laboratory results are obtained, and all are within normal limits. Head-to-toe evaluation identifies no further injuries. Subsequently, a Foley catheter is placed. His medical records are copied, and a copy of his cervical spine radiograph is made.
The transport crew arrives and performs an assessment of the patient. The referring hospital personnel have done an exceptional job in stabilizing Patient A; the only interventions that the team performs are to restart an IV that appears somewhat unstable and to place small towels under his coccyx and shoulder blades to prevent pressure injury development. Although Patient A appeared to be quite healthy prior to this accident and is in no current distress, arterial blood gases are obtained to ensure that no respiratory complications exist. After the results are obtained, he is placed on the transport stretcher and secured for transport.
Just prior to leaving the hospital, a person comes through the door in tears, stating she is Patient A's fiancée. She runs to the stretcher and throws herself over the top of him. At this point, the patient starts to cry, and it appears that the emotional impact of this devastating injury is beginning to be felt. The fiancée wants to accompany the patient but is told that there is no room for her. The transport team allows Patient A and his fiancée a few moments together prior to departure.
During transport, a flight crew member notes that Patient A's body is quite cool. The cabin of the helicopter is air-conditioned, and the fan is blowing on the patient. Assuming that the spinal cord trauma disrupted his temperature regulating mechanisms, the team works to maintain an adequate body temperature.
Upon arrival at the trauma center, Patient A is evaluated in the emergency department. His core body temperature is 93 degrees and measures are undertaken to warm him. After further stabilization measures are performed, he is transferred to a spinal cord center, where he remains for four months, learning to use a portable ventilator and a wheelchair.
Discussion
The patient was well stabilized prior to the arrival of the transport team. The interventions the team performed could have been performed prior to their arrival if better communication had occurred. Advice on stabilization measures is always appreciated by the referring hospital staff and would have saved time at the referring hospital.
The psychologic aspects of Patient A's care were not fully evaluated prior to the arrival of the fiancée. Had the emergency department staff performed more in-depth evaluation of the impact of this injury, they would have learned of the fiancée's existence and could have called her earlier in his care. A tearful scene just prior to departure did not help the patient cope with the devastating injury.
In transport, the patient should have been kept warm. Allowing the patient's body temperature to drop to 93 degrees was an oversight on the part of the transport crew. In all transports, the crew should evaluate the patient for complications of the illness or injury sustained, not just how the patient will tolerate the stressors of transport.
Because many of the stressors of flight directly impact the respiratory system, the patient with respiratory compromise can be difficult to care for during transport. The predisposition to oxygen desaturation and respiratory failure is high.
Hypoxia is an enormous problem for the respiratory patient. The illness or injury may have caused the patient to experience the four types of hypoxia: hypoxic, histologic, anemic, and stagnant. Coupled with anxiety, fear, and pain that the patient may be experiencing, the patient is at risk for further respiratory insufficiency. Hypoxic hypoxia that occurs during air transport reduces the diffusion gradient for the oxygen molecules. The patient with fluid in his or her alveoli has a greater distance for diffusion, and the patient becomes more hypoxic at altitude. Increasing the oxygen percentage that the patient is receiving will increase the oxygen diffusion gradient, thereby minimizing the effects of atmospheric changes.
Gas expansion within the pleural and abdominal cavities compromises ventilatory effort. Undetected or untreated, pneumothoraces will expand at altitude, leading to worsening respiratory status. Gas expansion in the stomach causes pressure on the diaphragm, limiting respiratory excursion effort and subsequent ventilatory limitations.
Pulmonary secretions increase in tenacity in a low humidity environment. If the patient is prone to developing plugs in the respiratory tree, transport at altitude will enhance plug formation. Patients who hyperventilate lose additional insensible water through their respiratory tree, increasing the risk for volume depletion. This is an additional problem for the patient with a decreased body temperature whose compensatory response to cold stress is to hyperventilate. A decrease in body temperature of 2 degrees centigrade causes oxygen consumption to double. Therefore, the problems of decreased temperature and hypoxia potentiate one another.
If the patient's volume status is compromised, acceleration and deceleration forces can reduce venous return to the heart. This leads to a subsequent decrease in pulmonary circulation, further hampering oxygen diffusion. Additionally, deceleration forces can precipitate pulmonary venous pooling and pulmonary stasis.
Patients transported on stretchers should be secured with safety straps, usually placed over the chest. If these straps are too tight, full lung expansion is prevented. This immobilization also promotes atelectasis and pulmonary stasis.
Motion sickness can be avoided by the insertion of a nasogastric tube. Vomiting, if it occurs, can lead to shortness of breath and respiratory compromise. Both noise and vibration affect the respiratory patient; increased anxiety can increase respiratory rate, leading to further hypoxia and insensible water losses. Noise also limits the ability to fully auscultate breath sounds. An important part of assessment is lost in the transport environment, but efforts at assessment can include monitoring for chest expansion and placing the patient on a pulse oximeter to monitor for signs of oxygen desaturation.
In long transports, respiratory patients may require mechanical ventilator support. During air transport, a ventilator should be continually checked. Tidal volumes can be affected by gas expansion; commonly, the tidal volumes delivered will increase incrementally. For most patients, this increase in tidal volume is tolerable. However, there are some patients who cannot tolerate these minor changes in volume and they subsequently develop pneumothoraces. Additionally, ventilators require up to 15 liters/minute of air flow to function properly. This high flow rate rapidly depletes oxygen supplies, which, if not closely monitored, can be life-threatening to the patient.
Sickle cell patients are at increased risk during air transport as hypoxia predisposes the patient to a crisis. This patient's oxygenation status should be maximized to prevent this occurrence.
Stabilization interventions require that the patient with respiratory compromise be administered supplemental oxygen with an increased oxygen percentage. Restoring optimum circulating blood volume with blood products, if needed, will improve the oxygen-carrying capacity of the blood. The patient should be positioned for best oxygenation and gas exchange. If tolerated and feasible, the head of the stretcher should be elevated. This will allow for improved lung expansion and prevent pulmonary stasis. A pneumothorax should be treated with either a flutter valve, or preferably, a chest tube attached to a one-way (Heimlich) valve. Humidification of the delivered oxygen will reduce the incidence of plug formation; sterile saline can be instilled through the endotracheal tube prior to suctioning. Methods should be employed to limit heat loss in patients, including warming the oxygen, covering the patient with an adequate supply of linen, and maintaining an ambient temperature that is comfortable for the patient instead of the crew.
Patient B is 5 years of age and is found at the bottom of her grandmother's pool on a cold winter day. She is pulled from the water by the paramedics, and resuscitation efforts are initiated. She is found to have an agonal rhythm and intermittent spontaneous respirations. Cardiopulmonary resuscitation (CPR) is continued, and she is transported to the local children's hospital, approximately 55 minutes away by ambulance.
Prior to transport, the paramedics intubate the patient with a 5.0 endotracheal tube and start one IV line in her antecubital fossa. She is continually hand ventilated with 100% oxygen at an approximate rate of 30 breaths per minute. Her wet clothing is removed, and she is covered with a rescue blanket.
During transport, Patient B develops a bradycardic rhythm with occasional ventricular ectopy. She is given a weight-appropriate dose of atropine, and her heart rate remains between 90 and 100 beats per minute. Standing orders prescribe the administration of sodium bicarbonate, and she receives this dose 30 minutes before arrival at the children's hospital.
Upon arrival, Patient B's vital signs are: pulse 90 beats per minute; blood pressure 86/52 mm Hg; assisted ventilations at 30 per minute; and temperature of 91 degrees. Immediate interventions include rechecking her ABCs and obtaining a chest x-ray to confirm endotracheal tube placement. A set of arterial blood gases are obtained, and the results are: PO2 65; partial pressure of carbon dioxide (PCO2) 53; pH 7.23. Efforts are initiated to warm her, and after two hours, her body temperature is 96 degrees.
She is admitted to the pediatric intensive care unit (ICU), where she can be closely monitored. During the first 24 hours, an intracranial pressure monitor is inserted and signs of increased intracranial pressure are evident. The diagnosis of severe anoxic brain injury is made, and Patient B remains in a vegetative state.
Discussion
This case presents some of the dilemmas that are present in the prehospital care environment. One may ask why the paramedics chose to drive this child by ambulance rather than request helicopter transfer, the answer being quite simple; the helicopter was out-of-service at the time and the crew had no other options available to them.
In the prehospital environment, preparation for transport includes stabilization of the ABCs. Few diagnostic measures can be undertaken; the crew must rely on its initial assessment findings. Patient B was intubated, was ventilated with 100% oxygen, and had an IV line started, thus managing the ABCs. Her wet clothing was removed, but she was quite hypothermic upon arrival at the children's hospital. It would have helped to wrap the patient's head with a towel in transport and then replace this towel after it was water saturated to conserve body heat, as every body surface is equally susceptible to heat loss.
The patient also was predisposed to the problems previously discussed in the neurologically compromised patient. Her anoxic injury caused an increased intracranial pressure and the noise and vibrations experienced during the ambulance ride may have worsened this condition. Another measure that was not undertaken, but that should have at least been considered, is the placement of a nasogastric tube. The moving vehicle could have predisposed this child to vomiting and the risk of aspiration. If circumstances were different, other interventions may have been undertaken, including placement of a Foley catheter.
Cardiovascular patients requiring transport generally fall into two categories: those who are experiencing acute myocardial infarction or acute coronary syndrome, or patients with rhythm disturbances. The stressors of transport are debilitating to these patients if interventions are not performed to minimize the harmful effects.
Hypoxia is a significant complication to these patients due to a compromised myocardium. The compensatory response to hypoxia is tachycardia, which will lead to an increased cardiac oxygen demand. This demand is further enhanced by fear, anxiety, and pain, and supplemental oxygen is a requirement for these patients. Stagnant hypoxia caused by a damaged myocardium further intensifies the damage sustained. Continual real-time cardiac and respiratory monitoring to detect further hypoxic complications should be employed at all times throughout the course of care.
The altitude-induced problems of gas expansion, decreased temperature, and dehydration may or may not impact the patient. Gas expansion within the stomach can lead to vomiting, and this can limit blood flow back to the heart. The insertion of a nasogastric tube would solve this problem. However, the insertion of the tube may be more stressful and harmful to the patient than the risk of vomiting. Patients in severe cardiogenic shock with poor peripheral perfusion may exhibit cool and clammy extremities; core temperature would worsen in this state. During transport, most cardiovascular patients are placed on fluid restrictions. If the patient's condition is severe, the dehydrating environment that occurs in air transport could restrict their fluid status to the point of experiencing cardiovascular collapse.
The effects of acceleration and deceleration forces are prominent in this patient population. Compromised circulation is worsened in the presence of these forces. It is critical that these patients be positioned for maximum cardiac return and function. Cardiac congestion is common with both acceleration and deceleration forces and should be avoided if at all possible.
Patients with a lengthy cardiac history are predisposed to circulatory complications, both centrally and peripherally. The peripheral venous congestion that occurs enhances the risk of pressure sore development during long transports. The application of antiembolism stockings or other types of devices can limit thrombophlebitis formation in the lower extremities.
Cardiac patients require continuous monitoring and cardiac support. The transport team should utilize a cardiac monitor that is not affected by radio transmissions. Pacemakers should be functional in all environments and shielded from emissions. Defibrillators should be used with caution so that damage does not occur to the vehicle or other medical equipment.
In severe cases of cardiac failure, a patient may require an intra-aortic balloon pump. There are transportable pumps now available that have been used with great success. The most important parameter to assess when using a balloon in a patient during air transport is the balloon itself, as the balloon can be affected by gas expansion. Another device utilized in transport to stabilize the critically ill cardiovascular patient is the biventricular assist device, which requires extensive pretransport training and expertise on behalf of the transport crew.
Patients requiring continuous infusions of cardiac support medications are often transported. It is imperative that the crew be aware of this requirement prior to the transport to ensure that an adequate supply of medication is available. This supply should take into account unexpected delays. Transportable infusion devices are useful in delivering the prescribed amount of medication required. One of the classes of medication for which these concepts are critical are thrombolytic agents. Should the team be delayed, additional medication should be available, or, if the supply of the primary medication is exhausted, alternative drugs should be administered according to protocol.
Stabilization of the cardiac patient requires efforts to maximize cardiac function without compromising cardiac reserve. These patients have a fine line under which they can function and all interventions should be instituted to stabilize the patient prior to transport.
Patient C is a man, 62 years of age, who is complaining of chest pain upon his arrival at the local hospital. Evaluation of his complaints, laboratory studies, and chest pain demonstrate a massive anterolateral myocardial infarction. Thirty minutes after arrival in the emergency department, the patient sustains a cardiac arrest secondary to ventricular fibrillation. He is successfully resuscitated utilizing advanced life support measures. After the cardiac arrest, he remains quite unstable, having multiple runs of ventricular tachycardia despite multiple antiarrhythmics. The emergency physician consults with the cardiac care center at the referral hospital, and the patient is accepted into their care. Arrangements for air transport are made and Patient C is stabilized according to the instructions of the consulting cardiologist.
While awaiting the arrival of the air transport team, the referring personnel obtain a set of arterial blood gases for measurement. The patient's PO2 remains at 72 despite increasing the oxygen percentage delivered. A second IV line is started per instructions. It is decided not to insert a nasogastric tube, as it has been more than six hours since Patient C last ate and he states he has never experienced motion sickness.
Upon arrival of the transport team, the patient is moved to the transport stretcher. While moving the patient, increased ventricular ectopy is noted. The dosage of antiarrhythmic medication is increased and the oxygen face mask is replaced with a non-rebreather mask, which is capable of a higher oxygen concentration delivery. The patient is transferred to the waiting helicopter, and the team takes off.
During the initial moments of the transport, Patient C is very alert and interested in his surroundings, asking many questions about the helicopter. Within fifteen minutes, the patient becomes quiet and appears to be dozing. However, at the same time, the crew notice another increase in ventricular ectopy. While another IV drip is being mixed, the patient sustains a cardiac arrest in the helicopter. CPR is initiated, and attempts at intubation are made. Finally, after the fourth attempt, an endotracheal tube is successfully placed, and the patient is ventilated with 100% oxygen. The crew suspects that the cause of the arrest is a hypoxic myocardium secondary to the hypoxia associated with altitude. After 15 minutes of CPR and resuscitation efforts, Patient C again regains a cardiac rhythm and is stabilized. His condition remains critical; he remains comatose after cardiac arrest in the helicopter and is admitted to the cardiac care center in a severe cardiogenic shock. He has an intra-aortic balloon inserted and is supported on the pump for two weeks. After that time, without improvement in his condition, his family chooses to discontinue the balloon pump, and the patient dies shortly thereafter.
Discussion
Patient C's critical condition was not fully recognized by the individuals caring for him. He was alert and awake and this may have caused the healthcare providers to be complacent in their evaluation of him. He had no previous cardiac history and he was not considered to be a high risk individual. The ectopy that he sustained in the emergency department is common after a large myocardial infarction and should have alerted the physicians and nurses to his tenuous condition.
The stabilization measures undertaken by the staff were appropriate and thorough. With a PO2 of 72 and a cardiac arrest, Patient C was a candidate for endotracheal intubation. The flight crew should have been aware of the risks inherent in transporting this patient, and he should have been intubated prior to departure. Multiple intubation attempts in the helicopter are not uncommon; it is a difficult environment, with poor lighting and poor patient access.
This patient's outcome may or may not have been affected by the omissions of the referring personnel and the flight team members. However, they should have better assessed the severity of the patient's condition and intervened as necessary.
Burn patients require transport to a burn center whenever they have large, deep burns or burns that involve the face, hands, feet, or joints. The American Burn Association/American College of Surgeons Committee on Trauma published classifications of patients requiring treatment at a burn center, including [11]:
Partial thickness burns over more than 10% of the total body surface area (TBSA)
Burns involving the face, hands, feet, genitalia, perineum, or major joints
Third-degree burns in any age group
Electrical burns, including lightning injuries
Chemical burns
Inhalation injuries
Burn injury in patients with significant pre-existing medical disorders that could complicate management, prolong recovery, or affect mortality
Patients with burns and concomitant trauma when the burn injury poses the highest risk of morbidity or mortality
Burn injury in pediatric patients (transfer to burn center for the care of children)
Burn injury in patients who will require special social, emotional, and/or long-term rehabilitative intervention(s)
Burn patients are transferred daily from the scene of a fire (or injury) to the local medical care facility. Prehospital care of the burned individual should include:
Removing constrictive clothing and jewelry
Covering the patient with a clean sheet or blanket
Maintaining the patient in a position of comfort, usually flat
Avoiding application of ice or ointments to the wound
Flushing chemical injuries continuously
Initiating IV fluid resuscitation in major burn victims to maintain blood pressure and heart rate
Airway management is critical in the early moments following a burn injury. Airway edema develops rapidly and early intubation is recommended in patients with signs of impending airway compromise. If intubation is delayed, airway swelling will prevent placement of an appropriate size endotracheal tube and a smaller diameter tube must then be utilized. It is difficult to ventilate a patient through a smaller size tube, thus hindering ventilatory assistance. Patients should be administered 100% oxygen. Oxygen will break the chemical bond between carbon monoxide molecules and hemoglobin, thus improving the patient's oxygenation status.
Patient stabilization also includes circulatory support with either oral or IV fluids. Utilizing IV fluids in burns of greater than 20% TBSA is usually recommended because large volumes of oral fluids are neither tolerated nor absorbed. The 20% TBSA recommendation is simply a guideline. Interventions should be based on each patient's individual needs. Starting IV fluids in the prehospital care environment offers two advantages. First, IV line placement may be more easily obtained as peripheral swelling has not had sufficient time to develop. Secondly, the formulas for fluid resuscitation utilize the time of the burn injury as the starting point for resuscitation; delay in placing the line will make resuscitation efforts more difficult.
Lactated Ringer's solution remains the fluid of choice for fluid resuscitation, although other solutions are utilized in some parts of the country [12]. Fluid needs are based on the patient's weight in kilograms and the percentage of body surface area injured.
The fluid resuscitation formula most commonly utilized for adults with severe burns is the Parkland formula [12]:
4 cc x weight in kilograms x % BSA injured
Half of this calculated amount should be delivered in the first eight hours after the injury, the remainder over the subsequent sixteen hours. As an example, an 80-kilogram man with a 40% TBSA burn would require 12,800 cc during the first 24 hours (4 x 80 x 40). To receive half of this volume in the first eight hours, the patient should receive fluids at a rate of 800 cc/hr. During the second sixteen hours, the fluids would be infused at 400 cc/hr. It is important to calculate this volume correctly and ensure that adequate fluids are available throughout the transport of the patient. Monitoring blood pressure and weight-based urine output should ultimately guide fluid volume administration.
After evaluation of the burn injury, the decision to transport the injured patient to a burn center should be made. Based upon the criteria listed above, referral to the physicians at the facility should be initiated. Further stabilization of the patient, prior to transport to a burn center, should take into consideration the stressors of transport. Interventions should be instituted to limit these problems.
Air transport of burn patients is common as burn centers are often located many miles from the scene of the injury. Inhalation burns and burns of the face, head, and neck all predispose the patient to significant hypoxia. The hypoxia experienced in air transport potentiates this problem significantly. It is crucial that the patient have a secure airway. If the patient is intubated, the tube should be well secured. Burns of the face will weep fluid and render standard adhesive tape ineffective, leading to easy dislodgment of the endotracheal tube. Trach tape is often used to tie the tube in place, preventing this devastating complication.
The patient's head should be elevated as much as possible to limit edema formation. Supplemental oxygen should be continued with 100% oxygen, and cooling and humidifying the oxygen will help prevent airway edema formation. A patient who does not require intubation should be monitored continuously for ventilatory compromise, which may be developing secondary to smoke inhalation. This patient should always have an intubation set readily available at the bedside.
Gas expansion in the abdominal cavity is complicated by the development of an ileus. Ileus formation is quite common following a burn injury and will prevent the passage of gastric contents. A nasogastric tube and suctioning will help limit these effects, reducing the risk of vomiting and aspiration.
Hypovolemia is one of the most common problems occurring after a burn injury. Patients with partial thickness burns are at greatest risk of significant fluid loss. This loss of fluid, coupled with the dehydration that occurs in air transport, further compromises the patient's volume status. Evaporative losses are enhanced in the dry cabin environment, further increasing the patient's need for hydration. Prior to transport, a patient should be stabilized with IV fluids and all wounds should be covered with absorbent dressings. The transport team should be aware of the patient's fluid requirements. When determining how much fluid to take in transport, the patient's needs are calculated and that amount is increased again by half. A Foley catheter should be placed to monitor urine output, as this is the best indicator of the patient's response to fluid resuscitation efforts [13].
One of the biggest problems for the burn patient that occurs in all modes of transport is a subnormal temperature. With the loss of skin from the burn injury, the patient has lost his or her temperature regulating mechanism. In the best of situations, most burn patients become hypothermic, and the transport environment is not considered to be optimal for these patients. It is important that efforts be undertaken to keep the patient warm. This includes covering the wounds with dry dressings. When these dressings become saturated they should be reinforced with additional dry dressings. The patient can be wrapped in a rescue blanket; however, there are reported cases of patients becoming overheated in these blankets when wrapped too tightly. Additional blankets and linen will also help keep the patient warm. Covering the head with a hat is beneficial, especially in children and the elderly.
The hypovolemic shock that develops after a severe burn predisposes the patient to complications of acceleration and deceleration forces. The patient should be adequately fluid resuscitated to assist in combating these forces. Positioning the patient with the feet elevated will prevent blood from pooling in this region.
Immobilization of the burned individual enhances edema formation and can cause the extent and depth of the burn to increase. Lying on burn wounds is not only uncomfortable for the patient but limits circulation to the injured area. All wounds should be dressed prior to transport; these dressings need to be checked periodically to ensure that they have not become too tight from increased edema formation. Elevation of dependent limbs will limit edema formation, and it is important to check that all rings, necklaces, and other constricting devices were removed in the prehospital environment.
As noted, ileus formation promotes nausea and vomiting; however, a nasogastric tube to suction will limit these effects. The noise and vibration from the transport may increase the patient's stress level and efforts should be made to limit as much environmental input as possible.
Additional considerations in the transport of burn patients include pain control and the prevention of infection. Burn patients have a significant amount of pain, coupled with the devastating psychosocial and emotional impact of being burned. Small frequent intravenous doses of narcotics are useful in controlling some of the pain the patient is experiencing. Burn patients have very high metabolic rates that increase the metabolism of the narcotics, causing their length of action to decrease dramatically. Administering doses every 15 to 20 minutes is not uncommon. Therefore, it is important to have an adequate supply of narcotics available for the estimated length of transport. Most transport programs carry a limited supply of narcotics, so securing additional narcotics from the transferring hospital may be necessary. Additionally, the patient may be administered sedative agents to decrease awareness of the environmental input.
The transport environment is not a clean, sterile environment. Meticulous care should be provided to limit contamination of the patient's wounds. Applying topical antibiotics has the advantage of limiting the risk of wound contamination; however, these topical agents should be removed upon arrival at the burn center, delaying other interventions. In determining if topical agents should be used, each individual case should be considered and recommendations from the burn center should be utilized.
Transporting the burn patient requires a significant amount of preplanning and stabilization, as well as a great deal of work during transport. With proper stabilization and interventions, most burn patients tolerate the transport without complications.
Patient D is a man, 23 years of age, who was burned when a propane heater exploded while he was sleeping in his camper. He was able to escape from the camper prior to the entire truck exploding into flames. However, he sustained more than 60% partial- and full-thickness burns, mostly of the lower torso, back, and legs. He is treated at the scene by a volunteer ambulance crew that is only trained in basic life support measures. They apply an oxygen face mask, cover the patient with blankets, and transport him to the nearest facility 90 minutes away. The facility is a rural hospital, staffed by nurse practitioners and physician assistants, with a physician on-call 45 minutes away.
Upon arrival at this facility, placement of an IV line is attempted. After 45 minutes of unsuccessful attempts, the physician arrives and places a brachial cutdown. Lactated Ringer's solution is started, and initially the fluid was run wide open. Evaluation of Patient D's injuries includes calculating body surface area involvement, which is determined to be approximately 60%. He weighs 70 kilograms, and according to the fluid resuscitation formulas, his fluid requirements for the first 24 hours are 16,800 cc. Based on this calculation, the calculated fluid infusion rate is 1,050 cc/hour for the first eight hours. However, it is important to remember that this formula is based upon starting the IV fluids at the time of injury. By the time the line is placed, more than 2.5 hours have passed. This means that the patient is more than 2 liters behind (if utilizing the Parkland formula). Depending on the patient's condition, fluids can be increased so that the calculated amount is given in the first eight hours, or fluids can be administered according to the calculated formula and the patient monitored for response to these fluids. Patient D is an active, healthy young male without pre-existing medical diseases, and the decision is made to increase the fluid infusion rate to catch him up to these calculated needs. He tolerates this without problems, maintaining a normal blood pressure and an adequate urine output.
In assessing this patient, it is noted that he has singed hair on his head and mustache. No burns are noted on his head, and his airway appears clear. The oxygen delivery system is switched to a non-rebreather mask, capable of delivering approximately 95% to 100% oxygen. The decision to intubate is delayed at this time. Other interventions include cleaning and dressing his wounds and placement of a Foley catheter. He is administered 100 mg of intramuscular meperidine for pain. Arrangements for air transport to the burn center are initiated.
Upon arrival of the helicopter, the transport crew performs an assessment of Patient D. His airway remains clear without evidence of swelling, and the team chooses not to intubate him. The Lactated Ringer's solution had continued wide open, and he has received 5 liters of fluid up to this point. The team slows the infusion to a rate of 900 cc/hour with the knowledge that the patient's urine output had been greater than 50 cc/hour during the last hour.
The patient's dressings are reinforced with dry dressings, and the extremities are elevated to decrease edema formation. Throughout their assessment, the patient continually complains of pain. He is given 10 mg of morphine sulfate IV, with some relief of pain. The meperidine that he received intramuscularly was most likely sitting at the site of injection as his circulation was poor and was, therefore, not helping to relieve his pain.
The patient is transferred to the transport stretcher, and efforts are made to keep him as comfortable as possible. Due to the location of his burns, it is impossible to keep him from lying on his wounds; the team works to make subtle position changes as often as possible. The helicopter trip to pick up the patient is turbulent. The team wants to reduce the risk of motion sickness and vomiting on the return trip, so prior to departure, they place a nasogastric tube.
In transport, Patient D continues to complain of pain and is given frequent small doses of IV morphine sulfate. Upon arrival at the burn center, it is noted that he had received more than 50 mg of IV morphine sulfate, without compromise to his ventilatory status. In fact, the patient continues to complain of pain, although he does note some relief of its severity.
The patient remains stable during the transport. Upon arrival, his vital signs are stable, urine output remains more than 50 cc/hour, and his core body temperature is 96 degrees. He is admitted to the burn center, and the next morning has grafting over 35% of his wounds. After a lengthy stay at the facility, he is released with appointments for rehabilitation.
The multiple trauma patient has many problems that impact most body systems, thereby increasing the chance that the stressors of transport will be harmful to the patient. Transporting the patient by air is often required due to the large distances between trauma centers. This mode of transport increases the risk of compromise, and interventions need to be performed to reduce these risks.
Hypoxia is common in any patient sustaining chest trauma. Pneumothorax will compromise ventilatory effort and the patient should be decompressed with either a flutter valve or chest tube. Patients with chest wall injuries will have a decreased chest excursion effort and will need to be positioned for maximal ventilatory function. Dyspnea may be a sign of increasing hypoxia, but the transport team should also rule out the possibility of a pulmonary embolus as the cause of the hypoxia.
It is important to remember that gas expansion can compromise physiologic functioning of the patient, but it can also impact equipment such as air splints. During transport, these pieces of equipment should be continually checked for an increase in pressure on the involved extremity, which may harm neurovascular function. Wounds (e.g., bowel rupture) that lead to the formation of free air within the body cavities should be decompressed as the free air will expand causing further damage. Gas expansion within the stomach will predispose the patient to vomiting associated with motion sickness.
Hypovolemia, secondary to blood loss, is a common complication of trauma. Additional fluid loss in the form of evaporative losses in a pressurized aircraft will further jeopardize circulatory function. Patients in hypovolemic shock are also predisposed to the complications of acceleration and deceleration forces. Ensuring adequate fluid replacement prior to departure will prevent this complication.
Patients with traumatic injury to the central nervous system may have lost their thermoregulatory capabilities, enhancing the risk of hypothermia in transport. IV fluids should be warmed prior to administration and patients should be adequately protected from evaporative and radiated heat losses. Removing any wet or saturated clothing or linen should be done prior to departure.
Trauma to the musculoskeletal system requires the placement of splints and other stabilizing devices. Casts should be bivalved to prevent edematous compromise and traction devices should be monitored for causing circulatory impairment. As mentioned, traction weights should not be utilized in the transport environment, as these become a hazard during turbulence and motion.
Most trauma patients will have a nasogastric tube inserted during initial resuscitation. This tube should remain in place for transport to limit the risk of vomiting with motion. Any trauma patient who has had their jaw wired shut should be transported with a pair of wire cutters at the head of the stretcher.
With a multitude of equipment, lines, and interventions, multiple trauma patients require a tremendous amount of care during transport. Administering fluid, blood, and medications is time-consuming. When coupled with frequent vital sign checks and checks of equipment function, the transport crew is constantly working to stabilize the patient. To have a family member accompany the patient in this situation can be a benefit and a detriment. On the positive side, the family member can assist with the emotional needs of the patient, while on the negative side, they may be in the way of the crew, preventing their attention from being focused completely on the patient.
Transport crews will often say that the most challenging and the most rewarding transport is the trauma patient. The time in transport goes quickly and a number of interventions are performed. Being involved in a transport that can mean the difference between life and death of a patient is a very exhilarating experience and one on which many transport crew members thrive.
Patient E is a man, 33 years of age, working in a logging camp during the summer months. He is a well-conditioned, active male with a love of the outdoors. While at work one day, a log falls from the logging truck, crushing him beneath the weight. An emergency medical technician (EMT) who works at the logging camp rushes to the scene and directs the care of the patient while the log is being lifted off him.
Patient E sustains significant trauma to his chest, abdomen, and lower extremities. He is awake, talking, and in a tremendous amount of pain. The EMT is only trained in basic life support measures; he applies an oxygen mask to Patient E and directs an associate to call for helicopter transport to the local trauma center. While awaiting the arrival of the helicopter, the EMT places the patient in air splints to stabilize his suspected fractures.
When the helicopter crew arrives, the team immediately chooses to intubate the patient. Although he is maintaining his airway at present, he continues to lose blood and his condition is becoming more serious. Two large bore IV lines are started, one on each upper extremity. Lactated Ringer's solution is infused wide open until the patient has received two liters of fluid. The air splints on his lower extremities limit the ability of the team to examine the injuries to Patient E's lower extremities. By the EMT's report, Patient E has sustained multiple bruises to the lower abdomen, a displaced pelvis, and an obvious fracture to the left femur. The crew is able to palpate distal pulses on the right and left feet, the left pulse being slightly weaker than the right. As the transport is relatively short (25 minutes), the patient is loaded into the helicopter.
During transport, the patient's neurologic status appears to decompensate. The patient is no longer awake and responding to the transport crew. At this point the crew increases the oxygen percentage to 100% and obtains another set of vital signs. The patient's systolic blood pressure drops by 20 points, and fluids are again run at a wide open rate. A check of his peripheral pulses shows a diminished pulse of the right foot, with no change noted in the pulse on the left foot.
The patient is attached to a pulse oximeter for the transport and at this point it is noted that his oxygen saturation has dropped from 94% to 80%. Placement of the endotracheal tube is checked and the oxygen system is evaluated for proper functioning. When all components are evaluated and found to be functioning properly, it is assumed that the patient has developed a complication secondary to the chest trauma. The most obvious complication would be the development of a pneumothorax, and a flutter valve is placed. Immediately after placement, the patient's oxygen saturation increases to 88% and subsequently rises to 90%.
Upon arrival at the trauma center, the trauma team evaluates the patient and performs a head-to-toe assessment. A chest x-ray is obtained and confirms the development of a pneumothorax, as suspected by the transport team. During the assessment of the patient, it is noted that he has a cold, pulseless right foot. The mechanisms of injury and patient history are again evaluated in an effort to determine the cause of this complication. The femur fracture noted by the EMT at the logging camp is on the left side; it is suspected that an undiagnosed fracture has also occurred on the right side.
As the air splints are being slowly deflated, it is noted that color is returning to the patient's right foot and pulses again become palpable. When the splints are finally removed, a large ring of keys is found in the front pocket of the patient's jeans. It is suspected that the warm air in the emergency department increased gas expansion within the air splints, causing increased pressure on this key ring. The pressure increase was enough to put pressure on the patient's femoral artery, cutting off circulation to his right leg. If the splints had been left inflated for any longer, the patient ran the risk of losing his right leg.
The injuries this patient sustained included fractured ribs of the right chest (causing the pneumothorax), a fractured pelvis, a ruptured spleen, a small liver laceration, fractured left femur, and a closed fracture of the right tibia and fibula. He is taken to the operating room for repair of the splenic and hepatic injuries and orthopedic stabilization and subsequently transferred to the trauma ICU. During his ICU stay, he develops respiratory distress syndrome but is eventually removed from the ventilator and extubated after six days. His other injuries are stabilized and the patient does well.
Discussion
This patient required astute assessment by the transport crew to safely transport him to the trauma center. The conditions at the logging camp did not allow for a complete assessment of the patient and interventions had to be based on the mechanism of injury and the history taken by the EMT at the scene. During transport, the patient's blood pressure dropped, a sign of significant blood loss. As no blood products were available, the team could only support his volume with crystalloid solution. Due to the short length of the trip, this was adequate for this patient.
The other significant complication that could have been devastating to this patient's long-term functioning was the loss of pulse in his right foot. If the pressure on his femoral artery lasted longer, he may have lost his leg to amputation. Equipment should be checked continually for proper functioning to prevent these untoward complications from developing during transport.
Transporting the pediatric patient offers a unique set of challenges for the transport crew. Patient size is an advantage, as children weigh less and are more easily moved from one place to another. However, because they are small, children are at risk for more rapid decompensation, without the reserves to help them tolerate the stressors of transport.
Hypoxia develops more rapidly in the pediatric patient. Children have smaller vital capacities and a smaller surface area for gas exchange. An additional complicating factor can be that the child will refuse to utilize an oxygen mask. This potentiates the hypoxia as well as increases the risk of combativeness that is precipitated by hypoxia. If a child refuses a mask, oxygen tubing can be held in front of the child's face and oxygen blown at his oral and nasal airways.
The child's gastric cavity is relatively small; therefore, the child is more prone to complications of gastric gas expansion. Gastric and bowel function are irregular, and it may take a long period of time for food to pass into the bowel, increasing the risk of aspiration. Most pediatric nasogastric tubes available do not have a sump attached; these tubes can clog and suction is more difficult to apply. Occasionally flushing the tube with a small amount of water will assist with emptying the gastric cavity.
Pediatric patients are mouth breathers, which predisposes them to dry mucous membranes. The dry environment in a pressurized aircraft will potentiate this problem. For example, a child with respiratory syncytial virus who has thick tenacious mucous will have increasing difficulty in clearing secretions in this type of transport. Instilling saline into the nasal and pharyngeal passages will assist in thinning the secretions and opening the airways.
Children have a large body surface area to body mass ratio. This predisposes the child to increased evaporative heat losses and subsequent hypothermia. Transporting a child in a cool environment will enhance hypothermia development, and it is crucial that efforts are made to keep the child warm. With the large surface area of the head, placement of a stocking cap is quite successful in keeping the child warm. Rescue-type blankets can be utilized. However, with the large radiated heat loss a child produces, it is easy for the child to become overheated while wrapped in such a blanket. If a rescue blanket is used, it should be placed over the blankets that cover the child, and the edges should not be tucked in around the child.
Children are prone to the same effects of acceleration and deceleration forces as adults. The advantage of transporting a child is that their position can be more easily changed within the confines of the transport vehicle, including elevating the head of the child during landing (deceleration) to limit these forces on intracranial pressure.
Immobilizing the pediatric patient is often challenging, as the child may be too small to fit within the approved stretcher securing belts. Therefore, the crew members should be inventive in their immobilization of the child. Restraining devices need to be secure enough to provide for the safety of the child, while at the same time, not compromising the child's cardiovascular function. Restraining devices that are too tight across the chest of a child can hinder respiratory function and should be avoided. One method of transporting the very small child is to utilize a child's car seat. This offers two advantages. First and foremost is that the child is well secured and safe in the car seat. Secondly, most children feel comfortable in their car seat and may be more cooperative with this increased sense of security.
Noise, vibration, and motion sickness present the same complications in the pediatric patient as are found with adults. Providing diversionary activities to a child may help remove some of these stressors. Fully explaining all noises and procedures to a child may also reduce their fear and anxiety.
Ensuring adequate oxygenation of the child may require that the patient be intubated prior to departure. The challenge of intubating children in a controlled environment is increased many times in the transport environment and should be avoided at all costs. Insertion of a nasogastric tube may be at the discretion of the transport crew; consideration of the child's condition and time since the last meal can be included in the decision-making process. Ensuring that the child has at least one good IV line should be undertaken. Providing the young child with dextrose-containing maintenance fluids will prevent hypoglycemia from developing in transport. Keeping the child warm with hats and blankets will often provide comfort to the child. Transporting with the child's own blanket can also help keep the child warm and provide a sense of security. When placing the child on the transport stretcher, location of the safety straps should be double-checked to prevent placement over the child's chest wall.
Neonates often require transport when born prematurely or when diagnosed with congenital abnormalities. These small individuals are predisposed to hypoxia, hypothermia, and fluid overload states. Specialty-trained neonatal nurses are commonly utilized in these transports as their expertise allows them to carefully monitor the child and the effects of transport on that child. The use of a transport isolette unit provides the child with a safe, warm environment that can limit the harmful effects of transport.
Transporting children requires that the transport personnel be aware of the unique anatomic and physiologic variances of children. With consideration of these special needs, children can be safely transported long distances with minor impact upon their condition.
Patient F is a boy, 5 years of age, who was found unconscious by his mother after an undetermined amount of time. At his side were an empty bottle of children's acetaminophen tablets and an empty bottle of children's vitamins. EMS responds and transports the patient to the local hospital. He is intubated and placed on a ventilator with 100% oxygen; an IV line is started and blood is drawn for toxicology screen. His mother estimates that there were about 20 acetaminophen tablets and 25 vitamins ingested. The emergency department staff evaluates the bottles, and concern arises because the vitamins contained iron, increasing the risk of iron overdose.
While further efforts are underway to stabilize Patient F, arrangements are made to transport him to the referral medical center, which subspecializes in pediatrics. While awaiting the transport team, gastric lavage is performed, and when completed, the patient receives acetylcysteine down the lavage tube. Throughout the interventions, he remains comatose with occasional weak gasping breaths.
When the transport team arrives, they ask for a chest x-ray and a set of arterial blood gas (ABG) measurements. The chest x-ray shows no evidence of aspiration; the ABG results on 100% oxygen are pH 7.21; PO2 of 85; and PCO2 of 54. Based on these results, the team continues the oxygen at 100% but increases the rate of ventilations to 40 (from 30) breaths per minute. The lavage tube is left in place and a Foley catheter is inserted. Patient F's vital signs remain stable, although his blood pressure is on the low side of normal at 88/62 mm Hg.
Prior to departing, the team allows the mother and father to spend time with the patient. The mother asks repeatedly if she can accompany the team. However, due to the confines of the helicopter, this is not possible. The team provides her with as much information as possible about the receiving hospital, including telephone numbers, maps, and plans for admission. As the team leaves, the mother becomes distraught and has to be held back by her husband and other members of the emergency department.
In transport, Patient F's systolic blood pressure drops to 76/42 mm Hg. The team suspects that he is beginning to suffer an acute GI bleed secondary to the iron overdose. However, because this cannot be confirmed, they intervene within the capabilities of the transport, which involves increasing fluid administration. No blood products are available to the team at this time. After three fluid challenges, the patient's blood pressure drops to a palpable level of 50 mm Hg. The fluids are run wide open, and albumin is administered.
During the last few minutes of the flight, the pilot is in contact with the receiving hospital and is able to pass along a message that the patient is in acute need of blood products. Within minutes, the helicopter lands and Patient F is admitted to the emergency department, where the waiting blood is infused. After four units of blood, his blood pressure increases to 78/54 mm Hg.
As the patient is being stabilized in the emergency department, an additional set of ABGs are obtained, and the results are pH 7.15; PO2 of 76; and PCO2 of 46. Sodium bicarbonate is administered on a per kilogram basis. Shortly thereafter, Patient F sustains a tonic-clonic seizure. The seizure lasts approximately five minutes after receiving doses of both diazepam and phenobarbital. He is stabilized and transferred to the pediatric ICU.
After four days, his neurologic status improves and he is arousable. He is eventually discharged; however, he continues with neurologic deficits. With intensive rehabilitation, his long-term outcome is hopeful.
Discussion
During the transport of Patient F, his condition worsened, but not because of the stressors of transport. He tolerated the transport complications well, his oxygenation status had been optimized prior to his departure, and he was well-prepared for the transport. However, one of the life-threatening sequelae of iron overdose is GI bleed, and it was suspected that this was the cause of his hypotension in the transport. As this is a well-known complication of iron ingestion, it may have been worthwhile to obtain two or three units of typed, cross-matched blood prior to departure to accompany the patient in transit. However, this was not considered, and the team was able to support Patient F with fluids during the transport. Fortunately, the transport was not a lengthy one; a longer transport may have seen this patient arrest due to significant blood loss.
The increased incidence of acute and chronic illnesses in the elderly makes them frequent candidates for transport. For many years, when the elderly became sick, they remained at their local healthcare facility. However, as more sophisticated medical therapies have been developed and are being utilized in the elderly population, these patients are being transported. The multitude of health problems in this population increases their risk for developing complications during transport.
With advanced age comes an increase in underlying disease processes, which should be considered when assessing the elderly patient. A decrease in pulmonary compliance and total lung surface area enhances the risk of hypoxia. Coupled with pre-existing poor respiratory function, elderly patients need aggressive therapies to prevent the problems of hypoxia. Confusion, a sign of developing hypoxia, is often misinterpreted as senile dementia and therefore determined to be acceptable. The transport team has a short interaction with the patient and is not able to fully assess the patient's neurologic status. An accurate history regarding the patient's status from the referring hospital staff will assist the transport members in precisely assessing changes in the patient's condition.
The problems of gastric gas expansion are commonly not reported by the elderly patient, as abnormal bowel function and increased gastric gas are common to this population. Dehydration can potentiate a pre-existing contracted fluid volume state in the patient. It is imperative that adequate fluids are provided, while avoiding fluid overload states. Often fluid status is difficult to assess in the elderly patient, and this difficult assessment is increased in the transport environment. If the ability to assess heart and lung sounds is lost, other parameters, such as skin turgor, blood pressure, and urine output, can be utilized as indicators of fluid status.
The loss of subcutaneous tissue that occurs with aging predisposes the patient to hypothermia. The patient should be kept warm with blankets, clothing, and hats. Limiting out-of-hospital time will decrease the environmental changes that a patient experiences in transport. The better stabilized the patient is prior to transport, the more efficient the transport process.
As the vascular system stiffens, cardiac return and output become compromised. Peripheral circulation decreases, and the ability to withstand acceleration and deceleration forces is diminished. Significant fluid shifts can compromise both cardiac and respiratory function. Additionally, the patient's protective mechanisms are less adaptive, preventing self-protection measures. Positioning the patient to diminish these effects is beneficial. The head of the stretcher should be elevated if possible, and during acceleration, the feet can be placed on pillows.
A unique challenge in the elderly patient with pronounced curvature of the spine is immobilizing the patient on a backboard, should a spinal column injury be suspected. This increased curvature prevents the patient from being secured in a position of good cervical alignment. Additionally, this curvature increases the risk of pressure sore development in areas that are not normally at risk for this complication.
Immobilizing the elderly patient also increases the risk of the patient developing poor venous return and edema formation. Stabilization measures can include the application of antiembolism stockings to assist with circulatory support in this patient population.
While it may seem that diminished hearing and eyesight may be an advantage in reducing noise and vibration input, the opposite is true. A patient who cannot fully comprehend the environment will become increasingly confused and disoriented. The patient may not have heard the briefing offered by the transport crew. Elderly patients' pride may prevent them from admitting to this deficiency. Continual reorientation and explanation can help lessen this confusion.
Elderly patients also have a decrease in both the primary response and cellular immunity that acts to protect them from infection. While this is not a significant problem in transport, it should be considered and all interventions should be performed with this concept in mind. Minimizing the risk of infection is formidable in the transport environment, as handwashing is not feasible and the disposal of contaminated items is not possible. Limiting the patient's exposure to potentially infectious situations should be considered at all times.
Stabilizing the elderly patient for transport is quite similar to that for other patients. Supplemental oxygen should be administered, IV lines should be started and well-secured, and Foley catheter and nasogastric tube placement should be considered. Keeping the patient warm and in a position of comfort will improve the patient's ability to withstand complications as well as provide a sense of security. Optimum long-term outcomes of the elderly are less frequent than in younger populations; therefore, it is crucial that the family members be allowed time with the elderly individual prior to transport. The referring hospital personnel can include these individuals in preparations for transport to provide the family members with a sense of being able to do something for their loved one.
Transporting the elderly patient is not tremendously difficult. However, when the patient does decompensate in transport, it is important that the transport crew be aware of the medical-legal aspects of their care when determining what interventions will be utilized to further stabilize the patient. Awareness of the patient's wishes and advance directives should be an important part of the medical report given by the referring hospital personnel to the transport crew.
Patient G is a man, 70 years of age, who requires transport to a hospital with ventilator capabilities. He is treated at the local 32-bed hospital in his home community for recurrent pneumonia. On his third return trip to the emergency department, he sustains a respiratory arrest and is resuscitated. However, this hospital does not have an ICU, nor are the staff trained in caring for a patient on a ventilator. Therefore, arrangements for transport are made.
The nurses caring for Patient G have previously prepared many patients for transport. They make sure that Patient G has a nasogastric tube and a Foley catheter inserted, and they keep him well-covered with blankets from the warmer. An IV line placed during the resuscitation appears to be functioning without difficulty, and fluids are infused at a to-keep-open (TKO) rate. Patient G continues to be ventilated by the respiratory therapist with 100% oxygen. Finally, the patient's chart, x-rays, and laboratory results are compiled to give to the transporting team.
The transporting team arrives to find Patient G obtunded but responsive to painful stimuli. Arterial blood gas measurements are obtained and reveal a pH of 7.5, PO2 of 88, and PCO2 of 24. Based upon these results, the respiratory therapist is instructed to slow the rate of ventilations to 20 per minute. The patient's history is reviewed and includes diabetes mellitus, controlled with 20 units of neutral protamine Hagedorn (NPH) insulin every day, an anterior wall myocardial infarction sustained four years ago, and a history of hypertension, controlled with antihypertensives (although his wife reports that the patient is noncompliant with these medications as he feels "draggy" all the time). At the present time, the patient's blood pressure is reported to be 110/62 mm Hg.
The patient's chest x-ray is reviewed and reveals a large consolidation in the left lower lobe. No other abnormalities are reported. Oral antibiotics had been ordered five days previously, and a single intravenous dose is administered before the arrival of the transport team.
The transport team compliments the referring hospital staff on their stabilization measures and prepares to depart with the patient. The patient's wife is allowed in to see her husband and she begins to cry at his bedside. One of the referring hospital staff remains with her throughout her visit and continually provides psychosocial support. The transport team promises to notify her of his safe arrival and estimates the length of transport to be approximately one hour.
After take-off in the airplane, the patient develops ventricular ectopy as noted on the cardiac monitor. The team assumes that this is caused by increasing hypoxia, enhanced by the previous myocardial infarction. As the patient is on the ventilator on 100% oxygen, the hypoxia can only be managed by changing the patient's position to maximize gas exchange. He is turned onto his right side to improve his ventilation and perfusion ratio. However, the ectopy continues and the patient is started on an amiodarone drip.
During the ectopy, the patient's blood pressure drops to a systolic pressure of 88 mm Hg. The team increases the IV fluid rate, and immediately the IV becomes nonfunctional. As the patient only has one IV line, this means that the amiodarone (Cordarone) is also discontinued. While numerous attempts are being made at IV line placement, the frequency of the ectopy increases. IV line placement is unsuccessful up to this point, secondary to the patient's contracted fluid status and the multiple attempts that had previously been made during his arrest at the referring hospital.
While the second crew member attempts to start an IV line, the patient sustains a cardiopulmonary arrest. The team begins resuscitation efforts per advanced cardiac life support protocols, including administering medications via the endotracheal tube. The patient continues in ventricular fibrillation for the remainder of the flight and the transport team chooses to discontinue resuscitation efforts after 45 minutes. The difficulty in making this decision to discontinue treatment is that the team has no diagnostic capabilities available to them to determine the cause of the arrest. While it is assumed that this was caused by hypoxia secondary to the pneumonia and enhanced by the previous myocardial infarction, the team cannot be sure. However, after 45 minutes, all efforts available to them have been undertaken and the team has no further interventions at their disposal. Shortly after this, the airplane lands at the airport and the medical examiner is notified of the patient's death.
The final task required of the transport team is notification of the patient's wife of his death in transport. She is assured that all efforts were performed to prevent his death and that he did not suffer during these efforts. She thanks the team for their efforts to save her husband's life and hangs up the telephone.
Discussion
This case presented the difficulties in transporting a patient with a multitude of health problems in an environment with limited resources. The patient's outcome was tenuous before the transport, and was further compromised in the transport environment. However, his condition at the time of the transport was such that he could not have remained at the referring hospital due to their limited resources. Therefore, the transport needed to take place, the risks being an inherent part of the transport.
The transport team did not take the time to start another IV line; had they done so, the patient may have survived the transport, as the arrest may have been avoided. Any patient who has previously arrested and requires transport should have at least two IV lines in place. The patient's IV line had appeared to be functioning; however, it was at a TKO rate, which is not a true test of a line's patency.
The decision to not place a second IV line may have been based on the fact that the referral hospital had been working hard at stabilizing the patient and the transport team did not want to offend them. While this line of thinking is polite, the error of their judgment is obvious. Placing a second line could have been performed without offending the staff by simply explaining the need for a second line, should the first one malfunction. The referral hospital staff seemed interested in helping to stabilize the patient and would most likely have viewed this explanation as a learning experience. Hopefully, the transport team will never make this mistake again. And while the transport team's interventions may be questioned, the death of this patient cannot be blamed on their error in judgment.
Transporting the high-risk obstetrical patient involves the stabilization and transport of two patients, the mother and the fetus. The sudden, precipitous delivery of the fetus is always a possibility and should be prepared for. If possible, delaying the delivery would be preferable to all individuals involved in the transport. Contraindications to transport, including acute fetal distress, uncontrolled maternal bleeding, and imminent delivery, may postpone the transport until such time that both the mother and fetus (or newborn) are stabilized.
During pregnancy, increased oxygen consumption occurs, predisposing the woman to hypoxia during times of stress. Hypoxia causes uterine irritability and predisposes the patient to premature labor. For the patient being transported for premature labor, this is a significant consideration. Providing supplemental oxygen throughout the transport and positioning the patient in the left lateral decubitus position will enhance the patient's oxygenation status. If exposed to hypoxia for a short duration, the fetus will experience minimal effects. However, as maternal hypoxia increases, fetal distress will develop as evidenced by a decrease or increase in fetal heart tones.
Gastric gas expansion causes pressure on the diaphragm, which is elevated during the third trimester. This leads to the development of dyspnea, and further increases the risk of hypoxia development. Gastric gas expansion can also place pressure on the uterus, increasing uterine irritability. Insertion of a nasogastric tube to suction will help relieve this development as well as reduce the risk of vomiting during turbulence.
During pregnancy a woman develops a 40% to 50% increase in circulating blood volume, although this is mostly an increase in plasma. Dehydration can cause a woman to become volume depleted rapidly, and volume depletion predisposes the uterus to preterm labor. Increased fluid volumes are required during pregnancy, and this volume should be increased even further during transport.
Of all patient types transported, the one who prefers the decrease in ambient temperature is the pregnant patient. Massive vasodilation occurs during pregnancy so the woman is continually complaining of being warm. This cool environment has little effect upon her physiologic functioning and will increase patient comfort. However, should the fetus be delivered, this cool environment can be harmful to the neonate's outcome. The neonate should be immediately dried and wrapped in blankets to help maintain body temperature.
Fluid volume shifts associated with acceleration and deceleration forces can lead to a decrease in uterine blood flow. Physiologically, the uterus is considered a nonessential organ in the body's response to shock and low-flow states, thereby leading to fetal distress when circulating volume is shifted towards the core circulation and away from the uterus. Placing the patient in the left lateral decubitus position will improve venous return and the ability to withstand these forces.
Most stretcher securing devices are designed to function properly when the patient is in the supine position. The pregnant patient who is transported in the left lateral decubitus position is more difficult to safely secure to the stretcher. Additionally, if the stretcher is located on the right side of the transport vehicle, the patient will be facing away from the transport crew during the transport. This obviously presents difficulties in assessing the patient. Turning the patient may seem the obvious answer; however, this is nearly impossible in many helicopters and airplanes used in air transport. Therefore, immobilizing and securing the pregnant patient presents one of the more challenging problems in transport.
A decrease in gastric motility that occurs during pregnancy predisposes the patient to vomiting with motion. This can be avoided with the insertion of a nasogastric tube, as previously discussed. Patients with pregnancy-induced hypertension (toxemia of pregnancy) are at increased risk of experiencing nausea and vomiting with motion. Hypertension, which can accompany vomiting, is to be avoided in these patients, and efforts to reduce this untoward complication should be considered a high priority.
Noise and vibration also can compromise the patient with toxemia of pregnancy. The patient may be increasingly sensitive to environmental input, predisposing her to seizure development. Reduction of noise with ear plugs can help reduce this input and limit her exposure to increased risk. Dimming the cabin lighting will also help in reducing the risk of seizure activity, although this may hamper the transport team's capabilities in accurately assessing patient color.
Stabilization prior to transport requires accurate assessment of the patient's status and interventions to maximize her physiologic functioning. High-flow oxygen, preferably by non-rebreather mask, and appropriate management of her fluid status will heighten her ability to withstand these stressors. Medications to control preterm labor can be instituted and continued throughout the transport. Seizure precautions should be initiated prior to transport and antiseizure medications should be readily available.
Delivery of an infant is also a consideration. The transport crew should have sufficient training in the delivery of an infant, as well as training in stabilization measures necessary to support the life of the child. Delivery of a child requires that the transport be diverted to a closer facility if additional stabilization measures are required for the infant. Knowledge of the resources available en route is imperative during the pretransport planning. Appropriate size equipment for airway and circulatory management should be easily accessible in the transport environment; this should include, but not be limited to, infant size laryngoscope blades, infant endotracheal tubes and suction catheters, infant intravenous catheters, and intravenous fluids used for neonates. Methods of maintaining the child's body temperature should be available, including rescue blankets and stocking hats.
The emotional impact of transport on the high-risk obstetrical patient is extreme. Time for interactions with other family members should be made available. The woman's original birth plan is no longer a reality and the patient and her family should be assisted in understanding the necessity of transport. While most individuals want the transport to occur because they believe that it is best for the outcome of the child, removing the patient from her loved ones remains difficult. The family that is left behind needs assurance that they will be notified immediately upon the patient's arrival at the receiving facility. If the patient's condition warrants, she can be the one to place this important telephone call.
During the transport itself, it is difficult to fully assess the patient. As mentioned earlier, she may be facing away from the transport crew. The ability to hear fetal heart tones with a fetoscope is negated by the noise inherent in the transport vehicle. An obstetrical Doppler monitor should be considered an essential piece of equipment to allow for the monitoring of fetal heart tones. Fetal heart tones are the only indication of fetal status available and are crucial to ascertain, at a minimum of 15-minute intervals.
Preparing for a high-risk obstetrical transport requires a great deal of planning. Equipment should be readily available, training should be current, and the transport crew should be prepared to deal with all consequences. Fortunately, the majority of obstetrical transports occur without utilizing all of this preparation. When the patient is stabilized appropriately and thoroughly, the majority of transports occur smoothly.
Patient H is 38 years of age and has developed preterm labor at 31 weeks' gestation. Tocolytic therapy has been unsuccessful at discontinuing her labor, and she is to be transported by air to a high-risk obstetrical center with the capabilities for delivery of a high-risk neonate. Patient H's history includes a previous cesarean delivery two years ago for uterine atony. She has a two-year-old girl and a husband who is very involved in the child's care.
In preparing the patient for transport, the referring hospital personnel start Patient H on oxygen by face mask. Magnesium sulfate is infusing at a rate of 3 g/minute in an effort to control or stop her labor; a new drip is made so that there will be a sufficient amount of medication to last the length of the transport. Additionally, Patient H is receiving lactated Ringer's solution at a rate of 75 cc/hour. Her husband remains with her throughout the preparation, offering her emotional support.
When the transport team arrives, they review Patient H's history with her and with the referring hospital staff. Patient H is well-informed of the reason for the transport and wants to get to a facility that can provide intensive neonatal support, if needed. Prior to departing the hospital, the transport team places Patient H on a non-rebreather mask to increase her oxygen concentration delivery. She is placed on the stretcher in the left lateral decubitus position and fetal heart tones are monitored prior to departure from the hospital. Fetal heart tones remain at 120 to 130 beats per minute.
During transport Patient H's vital signs remain stable, a Doppler monitor is utilized to monitor the fetus, and after 20 minutes, the patient appears to fall asleep. Thirty minutes into the flight, the transport crew notices that Patient H's respiratory rate has dropped to a rate of 6 breaths per minute. They immediately start assisting her ventilations with a bag-valve-mask device. Her vital signs are obtained; her systolic blood pressure has dropped 20 points. Fetal heart tones are initially not heard; after repositioning the patient, they are measured at 100 beats per minute. At this point, it is apparent that both the mother and fetus are in acute distress and a decision regarding interventions has to be made.
The team continues to hand ventilate the patient with 100% oxygen; after seven to eight minutes, the fetal heart tones increase to a rate of 118 beats per minute. The patient's respiratory rate remains at 6 breaths per minute, and the team continues to ventilate her at a rate of 25 per minute with 100% oxygen.
The team is now 20 minutes from the receiving hospital and the transport continues to its original destination. The patient requires continuous ventilatory support during the remainder of the transport. Fetal heart tones continue to fluctuate between 110 and 120 beats per minute.
Immediately upon arrival at the receiving hospital, Patient H is intubated and placed on a ventilator. She is arousable at this point, and showing signs of acute apprehension. Further studies reveal that her magnesium level is toxic, which caused her ventilatory failure. The magnesium drip is discontinued and she remains on the ventilator until her magnesium level is within normal limits, at which time she is successfully weaned from the ventilator.
When the magnesium drip is discontinued, her contractions increase in frequency and intensity. Other therapies are unsuccessful at controlling her contractions, and her membranes rupture. Within two hours of arriving at the receiving hospital, Patient H delivers a 1,000-gram baby boy. The infant is immediately resuscitated by the neonatal team and transferred to the neonatal intensive care unit (NICU). The baby boy does well and is released when weighing slightly more than 4 pounds.
Discussion
The referring hospital had well stabilized Patient H for the transport, with the exception of obtaining a magnesium level. The transport team neglected to look for this result in the patient's chart, and this set up the course of events leading to the patient's ventilatory failure. Additionally, the healthcare providers should have been monitoring the patient's deep tendon reflexes, as weakened reflexes indicate impending magnesium toxicity. Although this would have been difficult to perform in transport, the team should have attempted to obtain this assessment parameter.
Fortunately, the outcome of this transport was excellent. The patient was successfully ventilated when the need arose, and the fetus responded to this ventilatory support. Had the transport been longer, the team may have elected to attempt an intubation in the aircraft. Successfully mask ventilating a patient for a long period of time is difficult within the confines of the transport vehicle and tiring for the transport crew; however, intubation is also a challenge in this environment.
The transport team appeared not to consider that the patient may have been magnesium toxic. Had this been considered, they could have discontinued the drip and switched to another tocolytic agent. The most serious consequence of this action would have been an earlier delivery of the fetus, possibly during the transport itself. While other tocolytic agents may have been unsuccessful in terminating the preterm labor, the need to discontinue or slow the rate of the magnesium infusion was indisputable.
The successful outcome demonstrates the appropriateness of this transport. Without accessing such a facility prior to delivery, the infant would have been subjected to the stressors of transport as a neonate requiring NICU care and may not have tolerated the transport as well as he did while remaining in utero.
These case studies have demonstrated a number of developments that can occur in the transport environment. While some of the complications may have been avoided with more intensive stabilization, the outcomes of the patients presented most likely would not have changed. Appropriately stabilizing the patient should be considered one of the most important steps in transporting the sick or injured patient.
As discussed, continual assessment and interventions during transports are performed to keep the patient as stable as possible. The transport crew's responsibilities are performed with limited resources in a less-than-optimal environment. The advantage of transport is that there are usually no other distractions, and the patient is the crew's sole medical responsibility.
To maintain patient stability, the transport crew functions under standing transport protocols as well as physician orders. The interventions that can be undertaken include, but are not limited to, airway stability, suctioning, fluid management, performing advanced life support measures, administering medications, and either chest tube or flutter valve insertion. Monitoring the patient involves the utilization of a cardiac monitor, pulse oximeter, and capnography. Doppler monitors are employed to assess pulses when auscultation is difficult. Analysis of blood results is possible utilizing transportable bedside testing devices.
Vital sign assessment should be completed at frequent intervals to allow for early detection of patient deterioration. The patient's level of consciousness should be frequently monitored; hypoxia is a common cause of neurologic decline. Fluid intake and output should be frequently checked, as gas expansion occurring in air transport can cause changes in the fluid infusion rates.
The transport team is involved in the stabilization of the patient as previously discussed. The stressors of transport are reviewed and the patient stabilized to minimize these effects. During transport, the team should continually assess for the effects of these stressors and intervene as necessary. Releasing a small amount of air from the air splints during ascent in air transport will need to be followed with inflation during descent. Prevention of these untoward complications is the goal the crew works to attain.
All care during transport should be documented. The transport form should become a permanent part of the patient's chart at the receiving facility. The receiving staff should be familiar with its design in order to obtain information regarding the patient's response to transport. Any unusual events should be noted and the patient's response to these events recorded.
Throughout the transport, the team should be prepared to deal with the worst possible outcome. Without ancillary help or extra equipment available to the crew, they should be able to act and intervene rapidly and efficiently within the confines of their working environment. In unforeseen emergencies, when sophisticated medical equipment and personnel are critical, diversion to a closer facility may be necessary. It is important that the crew knows the location of these facilities to prevent unnecessary delays.
The communication loop begins when the transport is initiated. It is complete when the report has been given at the receiving hospital and the documented paperwork is integrated into the patient's chart. This process includes a number of individuals, and effective communication at each level is imperative. A break in this process can increase the risk of complications.
When a call for transport is placed to a transport program, whether it be air or ground transport, information regarding the patient's status is shared and should be based on physician-to-physician contact. Although direct physician communication may take place at a later time, the medical control individual responsible for the transport is taking on the legal ramifications mandated by law. Once the patient's status has been provided, the requirements for pretransport stabilization should be communicated to the care providers. The transport team should be informed of any special needs that the patient will require. This may include the use of specialized equipment, which is not normally carried in the transport vehicle. The transport team should receive a complete report from those individuals who are providing the initial stabilization measures to the patient. During transport, the transport team may or may not be in direct contact with their base station. The team is directed to function under standing orders and written protocols. Should the team need to deviate from these protocols, accepted standards of practice and safe and reasonable actions should be employed.
Upon arrival at the receiving facility, the transport crew should provide information about the patient's condition from the time of the initiating event to the time of arrival of the patient at the receiving hospital. Much of this information is secondhand, so the communication process should be flawless to ensure that important pieces of information are not lost. Finally, all information should be fully documented as a permanent form of communication.
As noted, before this process is complete, the patient's family and the referring facility should be notified of the safe arrival of the patient. Only after all involved persons are notified is this loop considered complete.
Communication techniques and technology are too extensive to be covered here; the reader is referred to a number of excellent references if more in-depth information is desired. Regardless of the technology utilized, every effort should be undertaken to protect the patient's confidentiality based upon the Health Insurance Portability and Accountability Act (HIPAA) requirements. The patient's name should not be used, and other identifying features should be avoided. This is especially difficult during an incident with a high-profile patient or during a media event.
All transport programs have a medical control officer. The organization of this control varies from system to system. On-line medical control is the direct communication between the transport personnel and the physician (or physician-surrogate) via radio or telephone for the purpose of providing orders for patient care.
Off-line medical control includes those administrative functions that are necessary to ensure the quality of care. Each medical control officer is a physician who is directly responsible for the transport crew and their actions. It is the medical control officer's responsibility to ensure proper training, orientation, development of protocols, and ongoing continuing education.
Most transport programs have recurring "run reviews" in which the transport is reviewed for appropriateness, timeliness, and care delivered in transport. These run reviews are directed by the medical control officer and assist in providing ongoing education for the crew members. Additionally, this review allows for a critique of current protocols and can provide the impetus for change that may be necessary to meet the changing technology of medical care.
Ground transports are unique in that they can be initiated by the general public through emergency medical care systems, such as the 911 system. Air transports are generally initiated by healthcare providers after initial evaluation of the patient's status. Public request for medical care often puts the transport crew members at a disadvantage, as the information they receive may be inaccurate and/or incomplete. Therefore, ground transport crew members should perform astute assessments while under the watchful eye of the patient's family, friends, and the general public. To work in this type of job, the individual should be self-assured about their abilities and confident of their responsibilities.
Emergency medical care systems are well developed in the United States. Patients are often within minutes of being treated by individuals trained in basic life support measures. A tiered layer of response is generally utilized; if the patient's condition warrants more intensive treatment, individuals trained in advanced life support measures are rapidly called to the scene. This system maximizes healthcare resources without wasting limited healthcare dollars. In 2019, the Centers for Medicare and Medicare Services (CMS) introduced the Emergency Triage, Treat, and Transport (ET3) model, a voluntary program in which Medicare will pay participating ambulance suppliers to either transport Medicare beneficiaries to the emergency department, transport to a primary care or urgent care clinic, or provide care at the location. This model is intended to give ground transport and local 911 dispatches greater ability to triage patients, and is designed to prevent unnecessary emergency department admissions, thereby improving quality of care and lower costs [17].
Ground transport may also be utilized in transporting a patient from a small facility to a larger hospital with more sophisticated resources. These transports require personnel with a more advanced level of training; it is important to remember that a patient cannot legally be transported in an environment that does not provide the same level of care as the patient had been previously receiving.
While ground transports do not have to contend with the stressors of altitude changes that occur in air transport, the other stressors (e.g., acceleration, deceleration, prolonged immobilization) remain factors throughout the transport. It is the feeling of many seasoned transport personnel that caring for a patient while going across town in a ground ambulance is equally as difficult as caring for a patient in a helicopter. The constant forward, backward, and lateral movements of both environments make caring for the patient a true challenge.
Most established transport programs utilize pressurized aircraft for the transport of patients. This pressurization system allows for the maintenance of a reasonable cabin pressure altitude, minimizing the effects of altitude-induced changes on the patient. However, there are still patients who are transported in unpressurized aircraft, and it is these patients who are greatly impacted by altitude changes.
If a patient is to be transported by a fixed-wing aircraft, the patient should be stabilized with consideration of the stressors of altitude. The length of the transport is also an important consideration; the longer the transport time, the longer the exposure to the stressors of altitude and the greater the risk of complications. It is also generally true that the longer the transport, the higher the altitude at which the aircraft will travel, increasing the risks of hypoxia and gas expansion. Each patient should be continually assessed for these risks as they can develop insidiously.
Caring for the patient in a fixed-wing transport is often easier than in other transport environments. The cabin space is larger than in a helicopter, allowing for additional equipment and increased room to maneuver. Many fixed-wing aircraft dedicated to air transport are retrofitted with mechanical ventilators, large oxygen and air tanks, hospital-grade suction, and alternating current (AC) power sources. These aircraft are often referred to as flying ICUs. This sophisticated environment demands that the transport crew has additional training in the use and care of the equipment on board. Many transport programs utilizing mechanical ventilators include a respiratory therapist as a part of the transport crew. This individual is responsible to care for the patient's airway and ventilatory status.
Fixed-wing transports require the use of ground ambulances to transport the patient from the hospital to the airfield and back to the hospital at the receiving end. This system requires good communication with ground-based personnel to prevent unwarranted delays in the arrival of these ground units. Time is of the essence and the ground ambulance should be present to assist with moving the patient in an expeditious manner.
One of the most important aspects of helicopter transports is the safety of the individuals on the ground when the helicopter is landing and taking off, which is discussed later in this course. Transporting the patient in a helicopter is a challenging and difficult responsibility. Access to the patient is limited; often only the patient's upper torso and head are accessible. Thorough pretransport stabilization is critical if the patient is to be transported safely. While the length of transport is generally short (as compared to fixed-wing or ground transports), the patient is at risk during the entire transport.
The effects of altitude on the patient can be minimal to extensive. As mentioned, helicopters are not pressurized. Therefore, if the helicopter must ascend in altitude to clear mountain passes or other obstacles, the patient will experience both hypoxia and gas expansion. Generally, the pilot of the helicopter will choose a flight path that has minimal altitude changes, thereby limiting patient complications. However, care in transport requires that the transport crew be aware of these risks and intervene as necessary should they become a factor.
With restricted access to the patient, in-flight care is limited, requiring the crew to perform frequent assessments. Care in-flight is often limited to ABC support, as well as medication administration. Changing patient position and other comfort measures may need to be withheld. However, the crew should remember, as in all transports, that if the patient is anxious and frightened, measures to calm the patient should be performed as part of routine care.
Statutory law regulates the equipment required in ground transports. In many states these statutes also regulate the operation of air ambulances. The minimum equipment needed for maintaining the stability of the ill or injured patient is listed in Table 3. Additional items can and should be included as the patient's condition and needs dictate. Equipment utilized in the transport environment should meet specific criteria, including but not limited to being: lightweight; portable; easy to secure; easy to clean; able to be utilized with battery backup; able to be used both in and outside the transport vehicle; and able to withstand the stressors of altitude and movement.
TRANSPORT EQUIPMENT
| Vehicle Equipment | |||||||||
| |||||||||
| Medical Equipment | |||||||||
| |||||||||
| Equipment Packs | |||||||||
|
Medical crew members should be familiar with the operation of the equipment in the transport vehicle, as well as be able to repair the equipment should it fail. The crew members should ensure that an adequate supply of disposable equipment is available to last for the length of the transport, with consideration of possible delays that may extend the projected transport time.
All equipment utilized in the transport environment should be easily secured. Equipment packs made of soft material are generally utilized for disposable equipment. If the equipment requires a power source, a backup battery source should be available if the power fails. The team could utilize hand-powered devices, such as resuscitation bags for ventilating the patient, if a ventilator failure were to occur. All equipment should be protected from electromagnetic interference. If not, radio transmissions may render the equipment nonfunctional.
In air transport, equipment weight is also an important factor. Placement of heavy items is at the discretion of the pilot-in-command; the weight and balance of the aircraft should be maintained for safe performance. Equipment that is permanently secured to the aircraft (e.g., ventilators, suction units, oxygen tanks) are placed in a position offering the crew some leeway in the placement of other disposable equipment packs.
It is important that the oxygen source in the transport vehicle be operating appropriately. The volume remaining in the tanks should be checked prior to each departure. These tanks can be replaced with full tanks to ensure an adequate oxygen supply throughout the transport. Attachments for the humidification and warming of the oxygen are available and should be utilized as the patient's condition warrants.
Altitude impacts flow rates of oxygen cylinders. Table 4 demonstrates this effect on flow rates. If transporting the patient by air, it is important that the crew utilize this information when calculating oxygen supply. If standard sea level flow rates were utilized, the oxygen supply would run out before the calculated time, putting the patient at significant risk.
Other transport equipment that may be utilized includes infusion pumps, Doppler monitors, pulse oximeters, and cardiac monitors. Monitoring of oxygen saturations and end-tidal carbon dioxide levels is critical when auditory cues are diminished. The crew should know the limitations of each piece of equipment and not depend solely on the equipment but rather on their assessment of the patient when making decisions regarding interventions.
When equipment packs are prepared, the crew generally packages items together to maximize the efficiency of their actions. For example, a nasogastric tube is packaged with an aspirating syringe, gel for insertion, adapters for connecting the tube to the suction source, as well as tape. When a nasogastric tube is to be inserted, the team has everything together in one package and does not need to open numerous packs in search of a piece of equipment.
Medications are usually removed from their standard packaging. The boxes that most medications come in are bulky and, in the event of a respiratory or cardiac arrest, make a large mess in a small place. It is important for the crew to check the medication labels closely, as should be done for any patient anywhere.
Transport packs are usually developed for individual patient needs. Many programs have developed a pack for burn patients, neonates, obstetrical patients, and pediatric patients. Knowing that the patient is 8 years of age alerts the transport crew to the need for the pediatric pack, and this can be loaded on the transport vehicle prior to departure. This limits the amount of excess equipment transported on each and every transport. Additionally, equipment is commonly placed in a backpack style pack so it can be easily carried into and out of remote locations.
Safety in transport should be the primary concern of all individuals at all times. Most accidents occur during helicopter transfers; however, a high level of risk is associated with all types of transports. Safety concerns should focus on all aspects of the transport, including both patient and crew safety issues. It is imperative that all personnel develop a strict policy to ensure their safety and the safety of others.
Safety restraints should be utilized at all times. This means that the patient should have restraining straps secured throughout the transport and that the crew wears seat belts at all times. Crew members often become complacent about seat belt use, removing the belt during the transport to allow for more movement around the transport vehicle. In an aircraft, the pilot should always ensure that everyone is secured prior to takeoff and landing; it is during the transport when these measures are neglected. Clear air turbulence can cause significant injury to unrestrained individuals at any time during a flight.
All equipment should be secured, and securing devices should be double-checked throughout the transport. Equipment that can present danger to the patient or crew should be placed away from individuals' heads, placing it either near the patient's feet or, preferably, on the floor. Disposable equipment in soft packs will limit the dangers inherent in hard objects.
The crew should brief everyone prior to each departure. The pilot should be informed of the patient's condition, and the patient should be informed of his or her responsibilities in the event of an emergency. Family members who accompany a transport should be briefed as to the location and function of emergency exits and the need to utilize safety restraints throughout the transport.
No smoking should be allowed in or around a transport vehicle. The team should know where fire extinguishers are located and how they work. Crew members should avoid flammable clothing such as nylon and polyester, which, if ignited, can cause deep, full-thickness burns.
The crew should be trained in the proper functioning of emergency exits and emergency procedures. The emergency exits should be clearly marked and should be kept clear of extraneous equipment. Emergency procedures should be practiced on a regular basis as part of continuing education.
The transport crew's first responsibility in an emergency is to themselves and then to the patient. The crew should remain safety conscious at all times. It is worth mentioning that the occupational injury rate for EMS workers in the United States is the highest of any reported to the Department of Labor [14,15].
Helicopter transports create a large amount of interest. Many people assemble to watch a helicopter take off and land. These bystanders should be kept away from danger. A safe landing zone should be established in a clearing that measures at least 75 feet by 75 feet, although most pilots prefer a landing area of a minimum of 100 feet by 100 feet. The landing surface should be solid; sand and gravel should be avoided. The slope of the landing site should be no greater than 8 degrees, otherwise the tail rotor is at risk of contacting the ground. All wires, trees, and other possible hazards should be marked and verbally described to the pilot. Smoke flares are used to assist the pilot in locating the landing zone, but it is imperative that these be removed prior to the helicopter's approach as they may obscure the landing zone and can be blown away, possibly causing a fire. All loose items should be removed from or secured to the landing zone.
When the helicopter is making its final approach, the patient, ground crew, and bystanders should be at least 500 feet from the site and should be directed to turn their backs to the helicopter. This is the hardest rule for bystanders to comply with; they came to watch and they will watch. The rotor wash, created by the rotating blades, causes swirling dust and gravel, posing a hazard to all individuals. Landing in the snow poses a real hazard, as the rotor wash produces a momentary whiteout condition. Additional hazards are created when the rotor wash blows loose items up and around. This can include stethoscopes hanging around a team member's neck, sheets covering the patient, or transport forms.
Helicopters should always be approached from the front, in the line of sight of the pilot. Never approach a helicopter from the uphill side. As rotor blades slow, they drop closer to the ground, possibly causing the decapitation of an unsuspecting person. Finally, approach should only be done once the pilot has indicated that it is safe to do so.
On rare occasions, a "hot" loading or unloading may be performed. This is when the patient is loaded or off-loaded with the rotor blades turning at idle speed. In these instances, all personnel should approach the helicopter in a crouched position. This is only done in cases of extreme emergency; some transport programs prohibit this action in all instances, citing the high risk of injury.
Other hazards of a helicopter include noise, which is measured at 90 to 100 decibels, and wind, which is up to 50 miles per hour. Engine exhaust that is routed out of the back of the helicopter measures 750 degrees Fahrenheit. Most individuals are aware of the main rotor blades that rotate above the fuselage of the helicopter, but the tail rotor at the back of the helicopter is difficult to see when spinning. Injuries commonly occur when individuals approach the helicopter from the rear.
Fixed-wing safety requirements in air transport should meet the same stringent requirements of the FAA regulations under which commercial aircraft function. These requirements specify that all equipment should be secured to ensure that passengers and crew are not injured by flying objects during turbulence or in the event of a crash. Equipment that is not secured to the airframe should be in soft packs and placed on the floor away from the patient and crew. Emergency exits should never be blocked by equipment or extraneous items.
The aircraft should always be approached in a safe manner. Although the hazards are not as great as with helicopters, the exhaust from a jet engine can reach 900 to 1,100 degrees Fahrenheit, causing a significant burn if contact is made with the exhaust or the cowling over the exhaust vent. Propeller aircraft should always be approached from behind the wing to prevent injury from the propeller. Ground personnel who are assisting with the loading and unloading of the aircraft should be trained and briefed regarding safety issues. Weight distribution is critical in aircraft and the ground personnel may not be aware of these requirements.
The pilot-in-command is responsible for the safety of the aircraft at all times. The pilot has the authority to determine that it is unsafe to fly a particular mission in certain weather conditions. This also holds true for rotor-wing transports. In most transport programs, the pilot is not informed of the patient's condition at the time a transport is requested. This relieves some of the stress that may cloud judgment when a life-or-death transport is being requested. The pilot should be free to decline a mission based upon weather or other factors, without feeling guilty for this refusal.
In the event of an emergency landing of an aircraft, all electrical equipment and oxygen must be turned off. If the patient is attached to a ventilator, the patient should be hand ventilated and the ventilator shut down. If time allows, the patient should be protected with extra linen and pillows. The crew should ensure that emergency exits are not blocked and the rapid egress is possible once the aircraft has landed. Once the aircraft has come to a complete stop, the crew should make a rapid assessment of the condition of the patient and other crew members. All personnel should immediately exit the aircraft and move to a safe spot, at least 500 feet away from the aircraft. One of the biggest risks in an emergency landing of this nature is the rupture of a fuel tank, causing an explosion and fire. The team should be well away from the aircraft in the event that this occurs. Once all individuals are safe, a plan should be formulated on how to care for those injured in the crash. The crew should remain with the aircraft unless a road or other public area is easily accessed. It is much easier for rescue teams to locate a downed aircraft rather than a lone individual walking to get help.
In any emergency situation, keeping a clear head and maximizing available resources will assist with a successful rescue. Knowledge of radio codes and emergency broadcast frequencies will help the search and rescue teams find the location of the aircraft in an expeditious manner.
Providing patient care in the transport environment encompasses a number of medical-legal issues. Responsibility for the care of the patient is often shared among a number of individuals and institutions, requiring that each one is aware of the other's function and capabilities. Both the transport personnel and those individuals who are facilitating patient transfer should be aware of these requirements to ensure that the patient is transferred in a safe and legal manner.
As previously discussed, in 1985 the transport of patients was addressed in the Consolidated Omnibus Reconciliation Act (COBRA). Subsequently, in 1995, these regulations were amended as a part of the EMTALA to clarify specific aspects of patient care.
The most significant impact from these regulations is that ever more patients are being transferred to facilities that can provide specialized care. This has increased the number of transports, which has caused a proliferation of transport programs. As these transport programs were developed, the expertise of transport personnel has improved and patients are now safely transported both on the ground and in the air.
Responsibility to provide care is shared among the physicians who are directly involved in caring for the patient. When an interfacility transport is being conducted, the referring and receiving physicians share in the patient's care. This responsibility may also be shared with the medical control officer of the transport program who is directly responsible for the actions of the transport team.
The concept of shared responsibility was developed to prevent referring physicians from transferring patients in a manner that is not suitable to providing care. Prior to joint responsibility, some physicians would order a patient to be transported out of their facility, and arrangements for this transport were made as quickly as possible. The patient would be loaded in whatever transport vehicle was available (in some cases this was a taxi) to ferry a patient across town. Once the patient left the referring hospital, the physician's responsibility was complete. This yielded a situation in which the patient arrived at the receiving facility in worse condition or even possibly dead.
Therefore, to ensure that patients are transferred safely, the responsibility is shared. This requires that the referring physician utilize the most appropriate mode of transport, employing trained transport personnel. The receiving physician should ensure that the patient arrives in as good condition as possible, withstanding the stressors of transport.
The shared responsibility ends when the patient arrives safely at the receiving facility. A notation of their safe arrival should be made in the copy of the patient's chart, which was left at the referring facility. This closes the patient's case for the referring hospital.
While this shared responsibility is apparent in the interfacility transfer of patients, it also is a factor in the prehospital transfer of patients. When a patient or family member accesses emergency medical care by the 911 system, a trained medical team will respond and transfer the patient to a hospital, if appropriate. The medical director of the emergency medical care system is responsible for the care of the patient in transport. This responsibility is shared by all individuals and facilities that support the emergency medical care system. Although this shared responsibility is subtle, it does exist in the prehospital environment.
Regardless of the environment, when an individual is employed and on duty, he or she has a responsibility to provide health care within the limits of their licensure. Nursing practice acts and emergency medical system guidelines outline the responsibilities of nurses, paramedics, and emergency medical care technicians. When transporting patients, these transport crew members should function within the guidelines of their state administrative codes, as well as within the protocols for care as outlined by the medical control officer.
If a patient is pronounced dead during transport, the transport crew must notify the local medical examiner in the county in which the patient died. This holds true in air transport as well if the patient's death occurs in the county over which the aircraft is flying at that time.
In everyday practice, patients are usually not pronounced dead during transport due to these legal entanglements. Many transport programs utilize nurses as the transport crew members, and, in most states, nurses are not legally allowed to pronounce a patient's death. Additionally, the transport environment does not lend itself to allowing the transport crew to make an informed decision regarding the outcome of the patient. The limited assessment tools available to the transport crew put them at a disadvantage in making an informed decision. Resuscitation efforts are usually continued until the final destination is reached and the patient can be assessed in a more sophisticated environment.
If a transport is requested for an extremely unstable patient, a decision regarding the final disposition of the patient should be made prior to departure. Patient wishes and family requests should be included in this decision-making process. If a patient experiences an arrest in transport, the team has two options: either return to the referring hospital or continue on to the receiving facility. If the transport continues on to the receiving facility and the patient expires in that hospital, the family should make arrangements to retrieve the body for burial. This is costly and often involves a large amount of paperwork.
On the other hand, the family may be in transit to the receiving facility, and if the patient is returned to the referring hospital, the family is left to wonder where their loved one is and why he or she has not yet arrived. This also creates a dilemma for the family who must return to the referring facility and who may be distraught and incapable of driving back home safely.
There is no easy answer to dealing with the death of the patient. It is a risk that is increased in transport; the transport environment puts additional stressors on the patient and patients who are transported are generally unstable to begin with. The transport team should be aware of the legal ramifications as well as the family's wishes and should try to choose a course of action that will be appropriate for all involved.
Additional issues facing the transport team include transport delays, traversing time zones, traversing international borders, and infection control. While these issues are not a part of everyday transports, they do arise on occasion and should be prepared for prior to departure.
Transport delays can be caused by a number of factors, including weather, mechanical breakdown, fueling requirements, and missed connections. Pretrip planning should include an assessment of current and future weather conditions, yet this does not guarantee that the weather will not change for the worse during the transport itself.
Weather problems can cause the delay of the transfer, diversion of the transport to an alternate facility, or cancellation of a transport. The transport team should be alert to these possibilities and make arrangements prior to departure. Having an adequate supply of equipment on board to care for the patient during a delay is a necessity. While it would be convenient to have a large amount of IV fluids and dressings, it is neither practical nor safe (in air transport weight is an important issue). The team should always be aware of their situation and the availability of backup supplies. When it appears that the supplies are running low, an alternate plan should be instituted. The team cannot wait to make a decision after their supplies are exhausted.
Mechanical breakdowns are never intended, but do occur (e.g., a flat tire on a ground ambulance is always a possibility and should be prepared for). Mechanical breakdowns in aircraft are usually slower to be repaired; parts are not readily available and an alternative mode of transport should be sought.
Missed connections should never occur with proper pretransport planning, but nonetheless, they do happen. This is most often a problem of fixed-wing transports, when a number of crew members are involved. The aircraft should notify the ground ambulance of their estimated time of arrival so that the airplane can be met immediately upon arrival. However, if transport delays do occur, the ground ambulance may not be notified and the team has to wait at the airfield for the ambulance. It is best to assign one individual on the ground who can be notified of any delays; it is then this individual's responsibility to notify others. Many transport programs now employ a communications specialist, or transport team dispatcher, who is responsible for all communications beginning with the first call requesting transport until the transport is completed and all appropriate individuals have been notified. This individual is critical to a smooth running operation.
It is also important to keep the family informed of delays. If the family has been told that the patient will arrive in one hour, and a delay occurs causing the length of transport to increase to one and one-half hours, the family will spend the last half hour in a state of worry. Fear that an accident has occurred will escalate until the family is convinced that a catastrophe has occurred and everyone has been killed. The family is already anxious due to the nature of the transport; they do not need any additional stressors.
Whenever a transport is delayed, the team should be resourceful and, if necessary, institute an alternate plan. However, this too may have to be changed. Individuals who are obsessively tied to standing protocols and unable to deal with change should not be in the transport environment.
The problems encountered when traversing time zones include changes to the times of medication administration, disruption of meal times, disruption of sleep patterns, and arrival and departure after hours. When traversing only one or two time zones with only an hour or two time change, these problems are not significant. However, when transporting the patient long distances over many time zones, these issues become more important.
Times of medication administration generally remain on the schedule initiated at the referral facility. In transport, the crew can continue with this schedule to ensure that the patient is receiving the appropriate medication in a timely manner. Upon arrival at the receiving facility, these times can be adjusted to meet the needs of the patient and staff.
Disruption of meal times can be avoided when preplanning occurs. If a patient is on a set meal schedule and is scheduled to be in transport during that time, a bag lunch can be prepared for the patient. Not only is this important to consider during the transport, but the time of arrival at the receiving facility should also be considered. If arrival is after hours and no food service is available, the patient should be able to have a source of nourishment.
Disruption of the circadian rhythms is a common consequence of hospitalization. A number of research studies have shown this to be harmful for the patient; however, it is something that is often unavoidable. During transport, the patient can be allowed, and should be encouraged, to sleep. The number of interventions is limited and it is a perfect time to rest. However, the transport crew becomes concerned when the patient experiences somnolence that accompanies hypoxia. Utilizing a pulse oximeter in this situation can prevent unnecessary arousal of the patient.
After-hours arrivals and departures can also produce delays in transport. As an example, a patient arrives in the middle of the night at the receiving facility and the number of staff is inadequate to care for this additional patient, or the patient needs an x-ray, but the x-ray technician is not in-house during the night shift. All of these problems can be eliminated with pretransport planning. If the patient is to arrive in the middle of the night, the staff should be informed well ahead of time and additional staff should be awaiting the patient's arrival.
Avoiding the problems associated with transport delays is easily accomplished with preplanning. Communication between all involved parties will minimize a number of these complications, expediting the patient's arrival.
Patients injured or taken ill while traveling abroad are those who usually require transfer across international borders; this is commonly referred to as aeromedical repatriation. This may include either individuals who are citizens of the United States and want to return to their home facility or foreigners to the United States who are transferred to their home country. Regardless of the direction of the transport, international borders must be crossed.
Care in international transport is no different than care in other transports. The transport times may be long and the team should make arrangements for adequate supplies and equipment. Transport delays commonly occur when crossing a border, and the team should take the possible delay into consideration.
Immigration and customs requirements vary depending on the country, the citizenship of the individuals in the transport, and the country in which the transport started. In emergency situations, most immigration and customs offices are very helpful in expediting the arrival process. Early notification of these government officials will allow for arrangements to be made ahead of time. Usually these officials will be readily available when the transport arrives at the border offices so that the transport can be rapidly continued. One of the biggest concerns of these officials is the transporting of controlled substances (narcotics) over the border. Most programs that perform these transports on a regular basis have an established document citing the type and amount of narcotics on board. The officials can then quickly check these counts and clear the vehicle and crew.
Another complication that occurs with international transport is communication difficulties. The services of a translator may be required, and arrangements for these services should be made prior to departure. Additionally, the patient and his or her family may not speak English, complicating communication between the transport crew and the patient and family. Bilingual crew members are an added resource in these situations. As in any healthcare situation, cultural differences should also be considered and addressed.
The risk of infectious disease in the transport environment is high. The patient is at increased risk for two reasons: their disease or injury may predispose them to infection; and the transport environment is not sterile, although cleanliness is always a goal of transport crew members. The number of environmental changes that the patient experiences in transport can increase their exposure to contaminants. Ensuring that the patient is covered and protected should always be a consideration.
Crew members are also at risk. The incidence of Mycobacterium tuberculosis, HIV, and hepatitis infection has become prevalent in the prehospital environment. This, coupled with the increased number of multi-drug resistant and virulent bacterial strains, indicates a necessity for much caution. Crew members need to reduce their risk of exposure; therefore, the use of barrier protection should be instituted at all times.
During transport, there is no access to hand-washing, although alcohol-based hand sanitizers can be useful. Gloves should be utilized and changed to reduce contamination. Wrapping and sealing contaminated dressings and linen should be performed to prevent exposure to those individuals who may be assisting with cleaning the vehicle at the termination of the transport.
Recognition of potential hazards should alert the transport crew to take appropriate precautions. Once the patient arrives at their destination, the covering over the patient should be replaced to reduce bringing outside contaminants into the hospital.
As health management continues to expand and develop, more patients will require and/or desire access to new therapies. It will be necessary for those involved in transporting patients to keep abreast of these therapies in order to provide advanced care during transport. Education and training programs dealing exclusively with aspects of transport care are being developed. Case Western University offers an educational program, the Dorothy Ebersbach Academic Center for Flight Nursing, specifically for those nurses involved in patient air transport. Programs such as this are coming to the forefront of education of transport nurses. Emergency department physicians are also being trained and made more aware of the parameters associated with patient transport.
Transporting the ill or injured patient is a challenging and exciting part of health care. Transport programs have been developed to provide patients whose medical needs surpass available resources with a variety of modes of transport, including ground and air transport. The transport environment introduces the patient to a number of stressors, which can occur in all modes of transport.
Transport regulations ensure that all patients who are in need of transport are transported in a safe and timely manner. The legal steps in arranging a transport are well delineated, and it is every individual's responsibility in caring for the patient to ensure that these steps are met.
Patients need to be stabilized appropriately to limit the stressors occurring in the transport environment. Stabilization of the airway, ventilatory system, and circulatory system is crucial prior to moving a patient from one locale to another. Additional stabilization measures should be undertaken depending on the patient's problems and condition at the time of transport. Each individual patient should be evaluated for the effects of the stressors of transport and stabilized appropriately.
Transporting patients is recognized as an integral part of their care; guarding their safety should be foremost in each individual's mind. The medical-legal aspects of transport should be met, ensuring that professional standards are maintained.
Only a small population of healthcare providers are actually involved in transporting patients, but all individuals caring for patients who are to be transported, or who have been transported, should be aware of these principles of care in transport.
Many organizations and associations offer additional information regarding emergency medical transport. A list of organizations and their Web sites is provided here as a resource, to allow for further research.
| Air and Surface Transport Nurses Association (ASTNA) |
| https://www.astna.org |
| American Academy of Pediatrics Section on Transport Medicine |
| https://www.aap.org/en/community/aap-sections/transport-medicine |
| Association of Air Medical Services |
| https://www.aams.org |
| Commission on Accreditation of Medical Transport Systems |
| https://www.camts.org |
| CONCERN Network |
| http://www.concern-network.org |
| International Academy of Aviation and Space Medicine |
| https://www.iaasm.org |
| MedEvac Foundation International |
| http://medevacfoundation.org |
| National EMS Pilots Association (NEMSPA) |
| http://www.nemspa.org |
| The Dorothy Ebersbach Academic Center for Flight Nursing, Case Western Reserve University |
| https://case.edu/nursing/research/centers-excellence/emergency-and-critical-care-transport |
1. Wilson WC, Grande CM, Hoyt DB (eds). Trauma: Emergency Resuscitation Perioperative Anesthesia Surgical Management. Vol 1. New York, NY: Informa Healthcare USA; 2007.
2. Pittman RN. Regulation of Tissue Oxygenation. San Rafael, CA: Morgan and Claypool Life Sciences; 2011.
3. Federal Aviation Administration. Federal Aviation Regulations: Part 91.211. Available at https://drs.faa.gov/browse/cfrPart/externalWindow/8/Part%2091%20-%20GENERAL%20OPERATING%20AND%20FLIGHT%20RULES/current/default. Last accessed June 27, 2022.
4. Pretorius T, Bristow GK, Steinman AM, Giesbrecht GG. Thermal effects of whole head submersion in cold water on nonshivering humans. J Appl Physiol. 2006;101(2):669-675.
5. Insoft RM, Schwartz HP (eds). Guidelines for Air and Ground Transport of Neonatal and Pediatric Patients. 4th ed. Elk Grove Village, IL: American Academy of Pediatrics; 2015.
6. Wilkinson F. Nepal's High-Risk Helicopter Rescue Unit. Available at https://www.mensjournal.com/adventure/nepals-high-risk-helicopter-rescue-unit-20150113. Last accessed June 27, 2022.
7. Ergan B, Akgun M, Pacilli AMG, Nava S. Should I stay or should I go? COPD and air travel. Eur Respir Rev. 2018;27(148).
8. Bradi AC, Faughnan ME, Stanbrook MB, Deschenes-Leek E, Chapman KR. Predicting the need for supplemental oxygen during airline flight in patients with chronic pulmonary disease: a comparison of predictive equations and altitude simulation. Can Respir J. 2009;16(4):119-124.
9. Brain Trauma Foundation. Guidelines for the management of severe traumatic brain injury; 4th edition. J Neurotrauma. 2017;80(1):1-244.
10. Warren J, Fromm RE Jr, Orr RA, Rotello LC, Horst HM. Guidelines for the inter- and intrahospital transport of critically ill patients. Crit Care Med. 2004;32(1):256-262.
11. American Burn Association/American College of Surgeons. Burn Center Referral Criteria. Available at https://ameriburn.org/wp-content/uploads/2017/05/burncenterreferralcriteria.pdf. Last accessed June 27, 2022.
12. U.S. Department of Health and Human Services. Burn Triage and Treatment: Thermal Injuries. Available at https://chemm.hhs.gov/burns.htm. Last accessed June 27, 2022.
13. Blumetti J, Hunt JL, Arnoldo BD, Parks JK, Purdue GF. The Parkland formula under fire: is the criticism justified? J Burn Care Res. 2008;29(1):180-186.
14. Centers for Disease Control and Prevention. Emergency Medical Services Workers: Injury Data, 2020. Available at https://www.cdc.gov/niosh/topics/ems/data.html. Last accessed June 27, 2022.
15. U.S. Department of Transportation, National Highway Traffic Safety Administration. Feasibility for an EMS Workforce Safety and Health Surveillance System. Bedford, MA: Bedford Research; 2007.
16. Commission on Accreditation of Medical Transport Systems. Accredited Services. Available at https://www.camts.org/services. Last accessed June 27, 2022.
17. Centers for Medicare and Medicaid Services. Emergency Triage, Treat, and Transport (ET3) Model. Available at https://innovation.cms.gov/initiatives/et3/. Last accessed June 27, 2022.
1. Moyle J. Medical guidelines for airline travel. Aviat Space Environ Med. 2003;74(5 suppl):A1-A19.
2. Blumen IJ, Rinnert KJ. Altitude physiology and the stresses of flight. Air Med J. 1995;14(2):87-100.
3. Brown J, Tompkins K, Chaney E, Donovan R. Family member ride-alongs during interfacility transport. Air Med J. 1998;17(4):169-173.
4. Commission on Accreditation of Medical Transport Systems. 11th Edition Accreditation Standards. Available https://www.camts.org/wp-content/uploads/2017/05/CAMTS-11th-Standards-DIGITAL-FREE.pdf. Last accessed June 27, 2022.
1. Theodore N, Hadley MN, Aarabi B, et al. Prehospital cervical spinal immobilization after trauma. In: Guidelines for the management of acute cervical spine and spinal cord injuries. Neurosurgery. 2013;72(Suppl 2):22-34. Available at https://www.cns.org/guidelines/browse-guidelines-detail/2-prehospital-cervical-spinal-immobilization-after. Last accessed July 22, 2022.
2. Mayglothling J, Duane TM, Gibbs M, et al. Emergency tracheal intubation immediately following traumatic injury: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012;73(5 Suppl 4):S333-S340. Available at https://www.east.org/education/practice-management-guidelines/endotracheal-intubation-following-trauma. Last accessed July 22, 2022.
3. Theodore N, Aarabi B, Dhall SS, et al. Transportation of patients with acute traumatic cervical spine injuries. In: Guidelines for the management of acute cervical spine and spinal cord injuries. Neurosurgery. 2013;72(Suppl 2):35-39. Available at https://www.cns.org/guidelines/browse-guidelines-detail/3-transportation-of-patients-with-acute-traumatic-. Last accessed July 22, 2022.
4. Sasser SM, Hunt RC, Faul M, et al. Guidelines for field triage of injured patients: recommendations of the National Expert Panel on Field Triage, 2011. MMWR. 2012;61(RR1):1-20. Available at https://www.cdc.gov/mmwr/preview/mmwrhtml/rr6101a1.htm. Last accessed July 22, 2022.
Mention of commercial products does not indicate endorsement.