Millions of people are diagnosed with a variety of malignant neoplastic lesions each year. Oral cancer, in which the primary malignancy arises within the oral cavity, is the 8th most common cancer in men and the 14th most common cancer in women. The common element among this diverse patient group are the problems encountered post-surgically when chemotherapy and or radiotherapy are used to destroy malignant cells, which can remain after the completion of surgery. Malignant lesions in the oral cavity are usually treated by surgical removal and several weeks of radiotherapy. The latter modality can cause severe changes in the mucosal tissues, bone, salivary glands, and the teeth, most of which are irreversible. Proper management before, during, and after both modes of therapy will have a positive impact on the quality of life and decrease the morbidity associated with these treatment regimens. This course will discuss the changes experienced within the oral environment during and after the treatment for oral and systemic cancers. Methods to mitigate these problems and to decrease the morbidity and the mortality which afflict these patients will be reviewed.
- INTRODUCTION
- ORAL CANCER
- DIAGNOSTIC PROCEDURES FOR ORAL CANCER
- LESION DIAGNOSIS
- CLASSIFICATION AND STAGING OF ORAL MALIGNANCIES
- TREATMENT FOR ORAL CANCER
- ORAL COMPLICATIONS FROM RADIOTHERAPY
- SURGERY AND RADIOTHERAPY: DENTAL CONSIDERATIONS
- ORAL COMPLICATIONS FROM CHEMOTHERAPY
- CHEMOTHERAPY: DENTAL CONSIDERATIONS
- CONSIDERATIONS FOR NON-ENGLISH-PROFICIENT PATIENTS
- CONCLUSION
- RESOURCES
- Works Cited
- Evidence-Based Practice Recommendations Citations
This course is designed for all physicians, including oncologists, surgeons, and radiologists, nurses, and speech, physical, and occupational therapists.
Problematic oral changes can affect more than oral health, and healthcare professionals should consider individuals' oral health in their overall patient care plans. The purpose of this course is to define oral cancer and briefly explain its diagnostic criteria as well as discuss the changes experienced within the oral environment after the treatments for oral and systemic cancers are initiated.
Upon completion of this course, you should be able to:
- Identify the most common etiologies of oral cancer and its incidence within the population.
- Review the basic histology of the oral mucosa and the changes that occur with premalignant and malignant lesions and their patterns of occurrence.
- Compare and contrast erythroplakic lesions and leukoplakic lesions.
- Distinguish among the varied diagnostic procedures for suspicious oral lesions and the classification and staging of those that are found to be malignant.
- Review the principles of and the complications from radiotherapy utilized postsurgically for patients with oral cancer.
- List dental procedures that should be completed before surgery and radiotherapy that can minimize oral complications after the completion of these treatment modalities.
- Explain the basic principles by which chemotherapeutic agents exert their cytotoxic effect.
- Discuss the serious chemotherapy-induced infections of oral origin that can be disseminated systemically.
- List other common oral effects of chemotherapy.
Mark J. Szarejko, DDS, FAGD, received his dental degree from the State University of New York at Buffalo in 1985. He received fellowship from the Academy of General Dentistry in 1994.
Contributing faculty, Mark J. Szarejko, DDS, FAGD, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
John M. Leonard, MD
Mary Franks, MSN, APRN, FNP-C
The division planners have disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#90684: Oral Cancer and Complications of Cancer Therapies
Few diagnosed medical conditions evoke as much fear and emotion as cancer. The incidence of cancer increases with age, and given the demographics of an aging population, more patients will be diagnosed with cancer annually[1]. The type of malignancy, its location, and the presence or absence of metastasis will dictate the options for medical intervention. In the last several decades, tremendous strides have been made in the prevention, diagnosis, and treatment of this group of diseases.
When chemotherapy is used to treat organic and systemic malignancies, alterations are commonplace in the cells of the oral epithelium, in those that form the cells necessary for immunocompetence, and in those that produce the formed elements of blood. The tissues within the oral cavity can undergo changes of such a deleterious nature that patients may require temporary respites from chemotherapy. Fortunately, these negative effects usually subside after chemotherapy ends.
In the United States in 2024, there will be approximately 58,500 new diagnoses of oral cancer and approximately 12,250 deaths; however, the number of deaths increases when complications of oncologic treatment are taken into consideration—nearly one death per hour [2,3]. This high mortality rate relates to the advanced metastatic stages at which these lesions are usually diagnosed. A challenge should be issued to healthcare professionals to reverse this trend with clinical procedures facilitating early detection. Surgical removal may be an option based on the extent of lesion size, its invasiveness into the proximate soft and hard tissues, and presence of metastasis into the regional lymph nodes. A postoperative course of radiotherapy may also have deleterious effects. As opposed to chemotherapy, the negative oral effects induced by radiotherapy are usually long-term or permanent.
The progression of cancer and the ensuing treatment will compromise the immune systems of most patients. Therefore, problematic oral changes can affect more than oral health. Debilitated and ulcerated oral mucous membranes can be a portal of entry for resident organisms of the oral microflora, with systemic dissemination and sepsis possible. A high degree of morbidity with potentially fatal consequences may ensue. It is imperative that all members of the allied healthcare team who treat these patients are aware of the etiology of these oral problems, available treatment modalities, and the consequences of delayed or inappropriate treatment.
Oral cancer, in which the primary malignancy arises within the oral cavity, is the eighth most common cancer in men, with incidence rates more than three times as high in men as in women [3]. Incidence has been declining since the 1970s, though it appears to be stable now in men, with women continuing to experience a 0.9% decline per year. The exception is of cases associated with human papillomavirus (HPV) infection, which are increasing in the White population.
Oral malignancies diagnosed in their initial stages can be treated more conservatively than their larger, metastatic counterparts. Unfortunately, the most common oral malignancy, squamous cell carcinoma, usually remains undetected until it is in its advanced stages. Pain, numbness, swelling, loss of function, and difficulty swallowing, which may appear later in disease progression, often do not accompany the beginnings of oral malignancies. The five-year survival rate of only 69% reflects the trend of late diagnosis [3].
The rich vascular and lymphatic network of the oral cavity, which extends beneath the tongue and into the floor of the mouth, facilitates local, regional, and distant metastasis. Early lesions may be difficult for the clinician to visualize and are often asymptomatic for the patient. Therefore, it is important for healthcare professionals to be familiar with the etiologies and risk factors associated with oral cancers.
Most patients with oral cancer have used tobacco products for prolonged periods of time [4]. Cigarettes, with their multitude of carcinogens, are the most frequent form of tobacco used. However, cigars, pipes, and smokeless tobacco also contain carcinogens; these should not be considered safe alternatives to cigarettes.
Although many more people smoke than develop oral cancer, the majority of oral cancers may be attributed to tobacco and/or alcohol use, either individually or together [4,5]. The use of alcoholic beverages by those who use tobacco products may enhance the negative effect upon the oral tissues [4]. The desiccating effects of alcohol provide a prolonged exposure of the carcinogens within tobacco on these tissues. This additional contact time increases the risk of the development of an oral malignancy, such as squamous cell carcinoma, 100 fold [4]. Factors such as immunosuppression and immunocompromise, a family history of cancer, nutritional considerations, alcohol abuse, systemic disease, and the duration and amount of tobacco used are possible reasons some tobacco users develop oral cancer and others do not. Because the majority of patients with oral cancer have a history of tobacco use, the implication of this product's carcinogens as agents that can cause malignant transformation in the oral tissues is strongly correlated.
Increasing age is another risk factor in the development of oral cancer, with a peak incidence in individuals 63 years of age; however, it is now occurring more frequently in younger individuals [2,6]. The exact causes for this are not yet clear, but there appear to be associations between young men and women who use conventional "smokeless" chewing or spit tobacco [2]. Historically, the incidence of oral cancer in the Black population has been twice that of the White population, but 2024 data from the National Cancer Institute indicates that the incidence in the White population has surpassed that of the Black population for both men and women [2,3,6]. Incidence of oral cancer is nearly as high in the American Indian/Alaska Native population as it is among the White population. A strong gender differentiation has also been noted historically, as men developed oral cancer with a frequency that was more than six times that of women. The ratio is now one woman to every three men, likely due to the increase in women who smoke since the 1950s [2]. It is thought that lifestyle choices (e.g., tobacco use, particularly in combination with the consumption of alcohol), rather than genetics, are responsible for these various disparities.
Chronic tissue trauma from ill-fitting prostheses, such as dentures or partial dentures, may predispose tissues to malignant change, though as a whole, there is no heightened risk for those with dentures [4]. However, patients who utilize these devices should be educated that any area of irritation should be examined and the corresponding adjustment should be made by a dentist. Sore spots that cannot be eliminated after adjustments, relines of the existing prosthesis, or the fabrication of a completely new prosthesis should be monitored very closely. If the prosthesis is not worn and the sore spot remains, a biopsy of the area is indicated.
In one study, HPV type 16 (HPV16) was found to account for approximately 55% of oral cancer cases in the absence of any other risk factors [7]. While HPV16 and HPV18 infections are widely recognized as a main cause of cervical cancers in women, they are also increasingly linked to oral cancer in those younger than 40 years of age [3,4]. The increase of oral cancer cases in this population is associated with the spread of HPV and is strongly correlated to having multiple oral sex partners [2,3,7]. Autoimmune factors, complex genetic mechanisms (individually or collectively), and other viral agents, such as herpes simplex virus, may also be etiologic risk factors in this group (Table 1).
Excessive, chronic ultraviolet light exposure has been linked to cancers of the lip, particularly in individuals who work outdoors [4]. Other documented or researched causes include poor nutrition (i.e., lack of fruits/vegetables), lichen planus, and graft-versus-host disease. Oral cancer may also develop in the absence of known risk factors. Approximately 25% of patients with oral cancer have no identified risk factors for the disease [10]. Most of these patients are younger than 40 years of age, well below the age distribution for this disease [2,11].
A discussion of the histologic basis for normal, healthy oral mucosa is required before an understanding of the stages that lead to the development of an oral malignancy can be appreciated. Also, some of the problems that develop after radiotherapy and chemotherapy have a cellular basis in these tissues.
The oral mucous membrane does not have the same surface consistency throughout the oral cavity. The oral mucosa is classified into three types:
Masticatory mucosa: It has a firm texture that comprises the hard palate and the gingiva. This tissue is bound to the bone and has a minimal capacity to stretch.
Specialized (sensory) mucosa: Located on the dorsum of the tongue, it contains the taste buds.
Lining (reflecting) mucosa: The vast majority of the oral mucosa is lining (reflecting) mucosa. It is easily flexible and distensible.
Common to all three mucosal types is an outermost cellular layer composed of stratified squamous epithelium. Some of the stratified squamous epithelium, specifically the masticatory mucosa, may be keratinized. All of these surface cells are produced from a deeper layer of cells called basal cells. This cellular layer consists of cells that are active in deoxyribonucleic acid (DNA) synthesis and undergo mitosis. The cells that replace the outer squamous layer every three to four days originate here. When radiotherapy or chemotherapy causes ulcerations anywhere in the oral mucosa, it is because the mitotic sequence of the basal cells has been interrupted. A small membrane beneath the basal cells, called the basement membrane, is what malignant cells perforate to invade the underlying tissue and begin the growth of a malignant lesion [12].
The earliest deviation from normal cellular arrangement is dysplasia. Dysplasia is characterized by atypical cellular formation and arrangement without any malignant transformation. Dysplastic cells can progress to carcinoma in situ, in which actual malignant transformation has occurred to one layer of cells. At this point, there is no invasion into the underlying tissue. The potential for continued growth and metastasis continues to be very high [13]. Both dysplasia and carcinoma in situ can only be diagnosed by histologic analysis. Lesions of varying sizes, shapes, colors, and surface textures cannot be discerned by visual means to possess any of these cellular alterations. Patients with premalignant lesions do not experience symptoms that would prompt them to seek medical or dental care.
There is no universal appearance of malignant lesions. It is recommended that an oral lesion of unknown origin that does not heal within two weeks should be submitted for an expedited referral [2]. Patients should be advised that lesions that appear harmless may be malignant, while those that appear aggressive may be benign. Whether benign or malignant, oral lesions span a remarkable array of clinical presentations.
The surface appearance of oral lesions may be flat, raised, smooth, ulcerated, invasive, pedunculated, or velvety, among many other descriptions. Some lesions may share two or more of these characteristics and may occur anywhere in the mouth.
Leukoplakic (white) lesions are much more common than their erythroplakic (red) counterparts. Clinically, the latter group of lesions is more difficult to see amidst oral mucous membranes of a similar color, especially in areas of tissue inflammation or hypertrophy. A prominent vascular supply causes erythroplakic lesions to appear red and to bleed easily upon palpation. These lesions occur with less frequency than leukoplakic lesions but have a 91% probability of being dysplastic or malignant [14]. Therefore, it is essential that any erythroplakic lesion is biopsied. Among leukoplakic lesions that have undergone histologic examination, 20% are found to be malignant or premalignant [14]. However, this rate is more than doubled for leukoplakic lesions that are found in the floor of the mouth [14]. Healthcare professionals should perform thorough oral soft tissue exams as these lesions may be difficult to detect and patients are usually asymptomatic. It is also important to remember that lesion color cannot be used as a feature to distinguish a malignant lesion from one that is innocuous.
Ultimately, histologic analysis is the only standard by which an oral lesion can be classified (Table 2) [8]. However, only 25% of intraoral leukoplakic lesions are submitted for histopathic examination via traditional biopsy procedures [15].
HISTOPATHOLOGY OF CANCER
| Classification | Cellular Activity | Malignancy | Status | Indication | ||||
|---|---|---|---|---|---|---|---|---|
| Hyperplasia |
| Noncancerous | Potentially reversible | Cause must be investigated | ||||
| Dysplasia |
| Noncancerous |
Potentially reversible, but may progress to cancer | Close monitoring is indicated | ||||
| Carcinoma in situ |
| Cancerous (very early) |
| Removal is indicated | ||||
| Invasive |
Cell structure is completely aberrant | Cancerous |
| Immediate therapy is indicated |
Traditional biopsy techniques are either incisional or excisional in nature. Larger lesions that cannot be removed completely usually undergo an incisional biopsy. This procedure features the removal of a small portion of the lesion along with a continuous band of healthy tissue. If a lesion plus some adjacent healthy tissue is small enough to be removed in its entirety, this process is essentially an excisional biopsy.
If a general dentist does not provide this service, the patient should be referred to an oral or maxillofacial surgeon or an otolaryngologist. Lesions located on the soft palate or the tonsillar pillar area may be difficult to biopsy due to a strong gag reflex. These patients may need sedation to accomplish the procedure.
Correspondence from any specialist to which the patient has been referred should be monitored closely for the diagnosis and the treatment plan. It should not be assumed that the patient will go to the specialist or follow his or her recommendations; a follow-up with the patient is necessary. In the event a malignancy is detected, the patient should be made aware of his or her treatment options, and those options should be pursued. Similarly, a patient's refusal to seek specialty care when it is recommended should be documented in the chart for medicolegal reasons. The patient should clearly be informed that the risks of refusing a biopsy procedure may allow for the formation of a malignant lesion that is capable of metastasizing with possible fatal consequences. Ideally, the patient should sign this informed refusal with at least two staff members witnessing it. Legal counsel may be necessary to prepare the appropriate forms.
Diagnostic tools that precede traditional biopsy procedures have been developed. Toluidine blue, ViziLite, and computer-assisted brush biopsy analysis are such adjunctive techniques. These screening tools do not replace the traditional biopsy procedures but provide an initial assessment of a questionable lesion [8].
The principle upon which ViziLite works is based on the cell physiology of abnormal cells. These cells have a nuclear content and mitochondrial matrix that is denser than normal cells. The patient rinses with a special ViziLite solution for 60 seconds and expectorates the excess. This acetic acid rinse removes the adherent mucosal glycoprotein layer and increases the nuclear/cytoplasmic ratio via osmosis. A disposable handheld ViziLite is then passed over the oral tissues. Normal cells will absorb the light and appear dark. Abnormal cells, given the increased density of the nucleus and the mitochondrial matrix, will reflect the light and appear bright [20]. This reflection pattern from ViziLite provides for the detection beneath the epithelial surface. If a suspicious lesion is detected at or below the epithelial surface, the clinician should perform a biopsy or refer the patient to a specialist who is able to perform this procedure. Further study is needed to determine what role, if any, this test should play in oral cancer screening [8]. The ultimate diagnosis of the lesion is still dependent on a biopsy procedure.
Toluidine blue is a metachromatic dye that stains abnormal DNA, thereby identifying appropriate tissue for biopsy. Studies have proven its efficacy as a diagnostic adjunct in detecting the presence of potential malignant lesions, particularly in the early stages [8,21,22]. A Taiwanese study found a 79% increase in the detection of oral submucous fibrosis when using the dye compared to standard visual screening [23].
Sections suspected of being malignant lesions should be deparaffinized and hydrated with distilled water. Then, the sections may be stained with toluidine blue solution for two to three minutes, after which the section should be thoroughly rinsed and dehydrated. Malignant cells will appear as violet or red purple against a blue background.
The Oral CDx brush biopsy system is another means of attaining an initial assessment for suspect oral lesions [8]. The Oral CDx kit contains a sterile brush biopsy instrument, a precoded glass slide, a tissue fixative pouch, a requisition form, and a pre-addressed container into which the slide and requisition form are placed [24]. The brush biopsy instrument is a small, circular wire brush that is rotated several times over the lesion surface until the tissue is slightly pink or is just beginning to bleed. This slight degree of lesion penetration is usually done without topical or local anesthesia. The tissue sample on the brush biopsy instrument is then applied to the precoded glass slide, which is bathed in the tissue fixative. This sample undergoes analysis by the Oral CDx computer.
One of four classifications is possible for all submitted samples. An inadequate category indicates that not enough of a tissue sample for a meaningful classification has been obtained. A negative classification means that no epithelial abnormality has been detected. An atypical sample is one that has some epithelial abnormalities whose diagnostic meaning is unclear. A positive classification indicates positive evidence of epithelial dysplasia or carcinoma [25]. Treatment from this point depends on the lesion classification. This is an expedient addition to the armamentarium of oral cancer screening devices. Of note, screening should be done by the clinician who has adequate illumination, visualization, and knowledge of how the tissues of the oral and maxillofacial complex appear in a healthy state.
The most common sites of oral cancers are the tongue, lip, and floor of the mouth [3]. However, oral cancers associated with HPV16 and HPV18 may appear at less common sites, such as the tonsils, tonsil pillar and crypt, base of the tongue, and the oropharynx [3]. Given the pleomorphic nature of oral cancers, clinicians should not ignore a lesion because it does not appear malignant or because it is on a site less frequently targeted by squamous cell lesions.
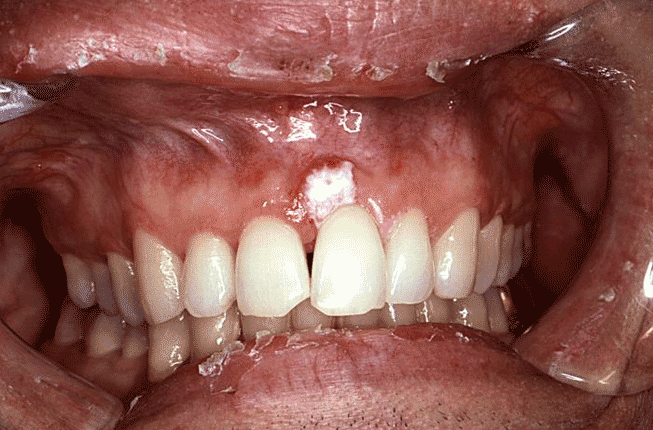
The oral malignancy responsible for more than 90% of the total cases of oral cancer is squamous cell carcinoma [26]. Squamous cell carcinoma is the result of uncontrolled differentiation of surface squamous cells of the oral mucosa into malignant cells. This is an aggressive lesion whose nests of malignant cells penetrate the basement membrane and the underlying connective tissue. Infiltration into the vascular and lymphatic circulation may occur early and facilitate metastasis. Continued proliferation can extend into the musculature and the supporting bone, with the capacity to destroy both. Upon histologic confirmation of a squamous cell carcinoma, surgery and radiotherapy should be scheduled as quickly as possible, because growth of the primary lesion and metastasis both occur rapidly; combined therapy may also include chemotherapy in later stages [26].
Squamous cell carcinoma can occur anywhere in the oral cavity. However, there are some areas of the mouth where these lesions occur more frequently than others. As noted, the most common sites of involvement are the tongue, lip, and floor of the mouth [21]. Many squamous cell carcinomas are located in areas that preclude visualization by the patient and can grow to larger sizes asymptomatically (Image 1).
The remaining types of oral malignancies affect tissues within the oral cavity or the adjacent salivary glands. Kaposi sarcoma, mainly associated with late-stage human immunodeficiency virus/acquired immune deficiency syndrome (HIV/AIDS), is one such malignancy. A rarity in the United States until the AIDS epidemic, Kaposi sarcoma has been identified as an AIDS-defining illness.
The initial presentation of these lesions is usually on the skin, but oral manifestations occur frequently. The palate, gingiva, and tongue are the primary sites of the appearance of these lesions; however, they may occur anywhere in the mouth. The human herpesvirus-8 (HHV-8) is considered to be the etiologic agent of this malignancy [9]. The lesions of Kaposi sarcoma may be red, violet, dark blue, or black-blue and usually begin asymptomatically. This vascular malignancy is typically flat at its onset but progresses to form nodules that develop a spongy consistency. Their growth can interfere with swallowing and eating, and larger lesions bleed easily. Treatment is usually a combination of surgery and radiation therapy, which is taxing for patients with an advanced stage of immunosuppression (Image 2).
Other types of cancers that may occur in the oral cavity include lymphomas, melanomas, and cancer of the minor salivary glands. These cancers are rare; nonetheless, they should be considered as a part of differential diagnosis when a patient presents with oral lesions of unknown etiology.
Before surgery and radiation therapy can begin, classifying and staging of the lesion must be completed. The internationally recognized system is the TNM classification (Table 3), which is based on assessment of primary tumor size (T), metastasis into regional lymph nodes (N), and the presence of distant metastasis (M) [27].
OVERVIEW OF TNM CLASSIFICATION OF ORAL CANCER
| Classification | Assessment |
|---|---|
| Primary Tumor (T) | |
| TX | Primary tumor unassessable |
| T0 | Primary tumor is not evident |
| Tis | Carcinoma in situ |
| T1, T2, T3 | Size of primary tumor may range from less than 2 cm to greater than 4 cm |
| T4a (lip or oral cavity) T4b (lip and oral cavity) | Primary tumor has invaded deeper and/or surrounding tissue, including nerve, cartilage, muscle, skin, sinus, bone, and skull |
| Regional Lymph Node (N) | |
| NX | Regional lymph node metastasis cannot be assessed |
| N0 | No metastasis to the regional lymph node(s) |
| N1 | Metastasis to only one lymph node 3 cm or less in greatest dimension |
| N2a | Metastasis of one ipsilateral lymph node greater than 3 cm but less than 6 cm |
| N2b | Metastasis to multiple ipsilateral lymph nodes less than 6 cm |
| N2c | Metastasis to bilateral lymph nodes less than 6 cm |
| N3 | Lymph node metastasis is greater than 6 cm |
| Distant Metastasis (M) | |
| MX | Distant metastasis unassessable |
| M0 | Distant metastasis is not evident |
| M1 | Distant metastasis is evident |
Primary tumor size ranges from TX, at which the tumor cannot be assessed, to a T4 level. The latter assessment indicates that the primary tumor size exceeds 4 cm and has extensive infiltration of the muscle, bone, cartilage, sinus, and/or skin. Lymph node metastasis features more complicated divisions and subdivisions. When the lymph nodes cannot be assessed, an NX designation is given, while N0 indicates a lack of lymph node involvement. The first designation of nodal involvement is N1, which indicates involvement of only one lymph node less than 3 cm in greatest dimension. Progressive nodal involvement in terms of number of lymph nodes, their distance from the primary tumor, and the nodal involvement of the same and/or opposite side, continues in this spectrum to a N3 level. Metastatic disease has only three levels of assessment. When distant metastasis cannot be assessed, an MX designation is assigned. No distant metastasis is an M0, while M1 indicates distant metastasis [30]. A chest radiograph is the current method by which metastasis is measured. With this system, lower numbers are equated with a better prognosis.
Staging is a system by which the individual components of the classification results are compiled together in stages (Table 4). Due to the asymptomatic nature of the lesions, diagnosis is often delayed [31,32,33].
CANCER STAGING CRITERIA
| Stage | General Description | Associated Classifications | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 0 | Carcinoma in situ; lesion affects only the epithelial tissue |
| ||||||||
| I | Tumor size is small; there is no metastasis to the regional lymph nodes or other organs | T1N0M0 | ||||||||
| II | Tumor size is larger; no metastasis to regional lymph nodes or other organs | T2N0M0 | ||||||||
| III | Any tumor concomitant with lymph node metastasis; there is no distant metastasis |
| ||||||||
| IV(A, B, C) |
|
|
When the diagnosis of oral squamous cell carcinoma is confirmed, plans for surgery and radiotherapy are initiated. Surgery includes the removal of the lesion and its extension into the neighboring hard and soft tissue. Surgical extension into the neck (neck dissection) is usually required to evaluate the extent of the tumor and its spread into local and regional lymph nodes. Areas where surgical deficits are created should be stabilized prior to surgical closure. Muscle from sites such as the pectoralis major muscle may be grafted to repair the surgical wound. Vascular grafts may also be needed to provide adequate circulation for the new muscle grafts. Larger lesions can intertwine around nerves of varying sizes. The removal of these lesions may cause permanent loss of sensation and loss of motor function for many structures in the oral cavity. The loss of hard and soft tissue is commensurate with the size of the lesion. Many patients require the use of maxillofacial prostheses to restore form, function, cosmetics, and self-esteem after these extensive surgical procedures. If a large portion of the tongue is removed, speaking, swallowing, eating, and drinking become arduous functions.
Surgery may not eliminate all squamous cell carcinoma cells. Radiotherapy is utilized to eliminate the cancer cells that may have persisted beyond surgical measures. A common modality used postsurgically, radiotherapy may be rarely used presurgically to decrease the size of larger lesions [34].
The current unit of absorbed radiation is the gray (Gy) or the centigray (cGy). Tumor size, location, and metastasis will determine the required cumulative dosage of radiation.
Radiation in adequate doses is cytotoxic to malignant cells because it causes free radical damage to the cellular components that are required for cell division and replication. Unfortunately, healthy tissues in the area of the radiation beam will undergo the same cellular damage. So, the goal is to destroy the malignant cells with as little damage to healthy cells as possible.
The amount of radiation required to destroy all affected cells is too large to be administered in only one dose. Modified fractionation is used to make doses smaller and more tolerable. Most patients receive the same dose of radiation five days a week, over a five-to seven-week period [35,36]. Because salivary glands are particularly radiosensitive, relatively small doses or irradiation may result in damage [37]. Most radiotherapy is given in fractionated doses of 150–200 cGy per day [35]. Once a cumulative dose of 4,500 cGy has been absorbed, long-term deleterious side effects are encountered. Because most radiotherapy regimens for squamous cell carcinoma patients range between 5,000 and 7,000 cGy, most patients will encounter undesirable side effects [38]. The area at which the radiation is targeted will influence the types of side effects experienced by the patient.
Concurrent antibody therapy with cetuximab, an epidermal growth factor receptor (EGFR) inhibitor, may be considered for patients in whom chemotherapy is contraindicated, as many oral squamous cell carcinomas show moderate to high levels of EGFR expression [39,40]. It has been suggested that side effects may be minimized if the agent is administered between the hours of 11 a.m. and 3 p.m., due to the circadian rhythm of the oral mucosa [41,42]. This time frame is hypothesized as being ideal for maximum therapeutic effect and reduced toxicity of both cetuximab and radiotherapy treatments.
For patients with oral cancer, chemotherapy is recommended only as an adjunct to radiation and/or surgical therapy [2]. Chemotherapy alone has not been shown to have the same efficacy against oral cancer as with other cancers. Chemotherapy is recommended as an adjunct in the treatment of oral cancer in order to [2,14]:
Reduce and/or inhibit distant metastasis
Reduce tumor size prior to surgery
Sensitize malignant tissue to radiotherapy
Additional research to determine the most effective use of chemotherapy as part of the overall treatment plan for oral cancer is necessary.
The earliest complication seen after radiotherapy is damage to the skin and hair follicles that lie in the direct path of radiation, known as the treatment portal. Hair follicles are highly radiosensitive, and hair will cease to grow and may fall out. This is a temporary loss that may take weeks or months to reverse. The skin in the portal area may become cracked, reddened, and ulcerated to the extent that radiation therapy should be postponed. This problem is also reversible upon cessation of radiotherapy. In addition, radiotherapy can result in negative effects on oral health.
Normal oral epithelium regenerates every three to four days. The outer squamous cells are replenished by cells made anew at the basal layer. The cellular regeneration corresponds with a high level of mitotic activity. Radiotherapy cannot distinguish the mitotic activity between malignant cells and those needed to replenish the oral epithelium; it is cytotoxic to both groups of cells, resulting in mucositis.
Oral mucositis is the most common intraoral side effect of radiotherapy and usually has an onset in the second week of therapy [43,44]. Mucositis affects nearly 80% of all patients who undergo head and neck radiotherapy and occurs in four phases [43]. The inflammatory phase is begun as ionizing radiation causes the generation of free radicals. The disruption of the normal sequence of turnover and stratification from the basal cell layer is a continuum into the epithelial phase. The ulcerative phase features ulcerations of varied dimensions on any mucosal surface. The consequent pain can be so intense that patients may have difficulty eating at a time when adequate nutrition is life sustaining. Patients with removable complete or partial dentures may be unable to wear them, further complicating their ability to masticate and swallow. The denuded mucosal surfaces also are a portal of entry for organisms of an altered oral microflora. This, coupled with a host whose immunocompetence is challenged, can lead to systemic bacterial or fungal infections that may be fatal. Severe mucositis mandates that radiotherapy be postponed until adequate healing of the epithelium occurs. The healing phase may take several weeks after the last radiotherapy treatment [45].
The National Cancer Institute has developed a Mucositis Scale to allow for the basic categorization of the mucositis lesions according to severity [46]. Grade 1 is defined as the absence of symptomatic mucositis or mild symptoms. Minimal mucositis, grade 2, involves moderate pain that does not greatly interfere with food intake but may necessitate a slightly altered diet. A grade 3 (severe) reaction is present when extreme pain causes feeding to become difficult. At this grade, the patient can only tolerate a liquid diet. When the mucosal ulcerations are deep or necrotic and bleed spontaneously, a grade 4 level has been attained. This level of mucositis is considered life-threatening. Patients with grade 4 mucositis may require intravenous fluids, analgesics, and antibiotics in a hospital setting until they are medically stabilized. Even if radiotherapy has been completed, the patient should still be followed closely to assure complete healing of all lesions. If radiotherapy has been interrupted because of the severity of mucositis, the cumulative dose of radiation that remains may be fractionated into smaller daily doses. Grade 5 is death [46].
Management of less severe grades of mucositis consist of palliative relief of pain, the monitoring and treatment of localized infections that may develop, and monitoring the patient's ability to maintain an oral care regimen and an adequate nutrition level. Liquid forms of systemic analgesics and antibiotics may be easier for the patient to swallow. Topical liquid anesthetics such as 2% viscous lidocaine may provide temporary analgesia. Because these patients may be taking medications for other conditions, care should be taken to avoid any adverse drug interactions. Prednisone, 40 mg to 80 mg per day prescribed for one week or less, may help to resolve some of the inflammation [47]. Varied rinses of sodium chloride and sodium bicarbonate may allow for tissue cleansing, moistening, and lubricating and are well tolerated. These rinses, along with proper oral hygiene and hydration, are mainstays of prevention and treatment. Chlorhexidine 0.12% rinses are useful but have a tendency to cause discomfort and nausea. Evidence supporting their use is generally inadequate and/or conflicting [48].
There is increasing evidence that severe oral mucositis due to radiotherapy may be pre-empted with palifermin, a recombinant human keratinocyte growth factor, though this use is an off-label use [49]. Palifermin is approved by the U.S. Food and Drug Administration for the treatment of severe oral mucositis in patients with hematologic malignancies undergoing total body irradiation, stem-cell transplantation, and chemotherapy [50]. Though the agent is expensive, oral mucositis is often reported to be the most torturous side effect of cancer treatment and may necessitate the cessation of radiotherapy even with advanced-stage malignancies. Evidence supporting the use of palifermin is conflicting [48].
The prophylactic palifermin regimen begins with one 60 mcg/kg IV dose three days prior to treatment and three days following treatment up to a maximum of six doses [51]. The most common side effect is skin rash/erythema [51,52]. A 2011 study examined its use in patients with head and neck cancer undergoing postoperative radiochemotherapy and found a modest reduction in the incidence of severe mucositis in those given palifermin (51%) versus placebo (67%), but the primary outcome was the reduction in duration of severe mucositis (4.5 days versus 22 days, respectively) [53]. A phase 3 clinical trial to determine safety and efficacy as an adjuvant treatment for those with head and neck cancers undergoing radiochemotherapy was completed in 2016, but the results of the study have not been published [54].
Palifermin use should be carefully considered for patients at increased risk of developing severe mucositis [51,52]. Pediatric patients and the elderly are at an increased risk; other risk factors include existing periodontal disease, poor diet, alcohol use, tobacco use, certain medications, oxygen therapy, and changes in breathing [55].
The Oral Assessment Guide (OAG), developed by Eilers, may be used in the staging of mucositis and when creating a management plan (Table 5) [56]. Using the OAG, the patient is assigned a number of points, from 1 to 3, in each of eight categories, with a total score of 8 indicating no change and a total score of 24 indicating severe mucositis. The OAG has been shown to be effective and reasonably easy to use in several studies [57,58]. It provides for objective assessment (as it omits pain as a measure of severity) and is able to identify subtle changes in status when used daily, thus ensuring rapid intervention. Another assessment tool is the World Health Organization scale, which despite its simplicity, is regarded as the most effective instrument used worldwide (followed by the OAG) [56,58]. Whichever tool is implemented, daily evaluation using a standardized assessment instrument is considered to be an integral part of oral mucositis management and should also be used at every patient contact [55,56,57,58]. Self-assessment using the OAG can also be taught for closer observations.
ORAL ASSESSMENT GUIDE (OAG)
| Category | Assessment | Finding | Score |
|---|---|---|---|
| Voice | Listen to the patient's voice | Normal | 1 |
| Deep or raspy | 2 | ||
| Unable to speak | 3 | ||
| Swallow | Ask the patient to swallow and test gag reflex with tongue depressor | Swallowing normally | 1 |
| Some pain while swallowing | 2 | ||
| Too painful to swallow | 3 | ||
| Lips | Observe and palpate | Smooth, pink, and moist | 1 |
| Cracked and/or dry | 2 | ||
| Ulcerated or bleeding | 3 | ||
| Tongue | Observe and palpate | Pink and moist, papillae present | 1 |
| Coated or papillae loss, shiny appearance with or without redness | 2 | ||
| Blistered or cracked | 3 | ||
| Saliva | Use depressor to assess the tongue and mucosa for saliva | Watery | 1 |
| Excessive amount of saliva, drooling | 2 | ||
| Thick, ropey, or absent | 3 | ||
| Mucous membranes | Observe | Pink and moist | 1 |
| Reddened or coated without ulcerations | 2 | ||
| Ulcerations with or without bleeding | 3 | ||
| Gingiva | Observe and gently scrape gingival tissue with depressor | Pink and firm | 1 |
| Oedematous | 2 | ||
| Spontaneous bleeding | 3 | ||
| Teeth or dentures | Observe and scrape teeth with depressor | Clean, no debris or plaque | 1 |
| Plaque or debris in some areas | 2 | ||
| Generalized plaque or debris along gum line | 3 |
While mucositis usually resolves after radiotherapy is completed, other radiotherapy-induced problems may be long-term or permanent. These include changes in the salivary glands, caries due to radiation, and osteoradionecrosis.
Saliva has several critical functions in the oral environment. Its chemical composition allows it to function as a lubricant, a buffer in the modulation of acidity (pH) levels, an initiator in the enzymatic process of digestion, and as part of the immune system. The immune function is not readily apparent but is critical in maintaining the delicate balance of the oral microflora. Certain salivary proteins inhibit microbial growth. Lysozyme, a salivary enzyme, can hydrolyze and thus destroy certain components of the bacterial cell wall. Immunoglobulin (Ig) is also secreted into saliva, with IgA being the predominant secretion. Small amounts of IgG and IgM are also secreted. These substances may exert their action by decreasing bacterial adherence to hard and soft tissue. The pH of saliva ranges from 6.7 (a weak acid) to 7.4 (a weak base) [59]. Alteration of this range toward either spectrum promotes certain forms of microbial growth over others. Lactobacillus and Streptococcus mutans, two cariogenic resident bacterial species, favor a more acidic environment. This situation occurs when salivary output decreases secondary to radiation therapy [60].
The parotid, submandibular, and sublingual glands compromise the major salivary glands. Scattered throughout the remainder of the oral mucosa are minor salivary glands. Location of the radiation portal will determine which gland or glands will be susceptible to damage. Because the secretory product of each gland varies, postradiation salivary composition will be determined by which gland or glands are damaged and which are spared.
The parotid gland is a purely serous gland (i.e., it releases a watery secretion without a mucous component). The submandibular gland has both a serous and a thicker mucus secretion, with the serous component being predominant. The sublingual salivary gland features secretions that are more mucus than serous. The minor salivary glands have secretions that are nearly all mucus in origin. Damage to one or both parotid glands will increase the viscosity of the saliva as the watery component of the saliva decreases. The saliva develops a thick, ropy consistency that decreases its function as a lubricating medium. The location of some malignant lesions is such that all of the major salivary glands are damaged. The cells that produce the serous secretions are extremely sensitive to ionizing radiation and can undergo a 50% decrease in output with a cumulative radiotherapy dose of only 1,000 cGy [61]. Salivary glands that are irradiated with a cumulative dose of 4,000 cGy usually have a permanent decrease in output [62].
The resultant condition of xerostomia will usually remain with patients for the remainder of their life. It is the most common persistent radiotherapy side effect [63]. Saliva substitutes and certain cholinergic drugs, such as pilocarpine, may decrease the severity of the xerostomia, but no treatment regimen will return salivary output to the levels prior to radiotherapy [64]. However, a 2011 multicenter randomized controlled trial found that intensity-modulated radiotherapy that spares the parotid glands is significantly less likely to cause severe xerostomia [63].
Xerostomia presents patients with a host of problems that they must confront on a daily basis. Patients who wear complete or partial dentures may have chronic sore spots because the lubrication that saliva produces to lessen the friction against the mucosal tissues is significantly decreased. These prostheses may be difficult to use for mastication and thus complicate the ability to eat. Because the perception of taste is partially dependent on food particles dissolved in a salivary medium, taste perception is altered. Patients often attempt to compensate for this by selecting foods that are very spicy or very sweet, which further compromises their medical and dental health. Swallowing food becomes more difficult as the bolus of food is less lubricated. Patients may need frequent sips of water during meals to alleviate this problem. The oral tissues can become subject to frequent irritation, tissue trauma, and opportunistic infection. The cleansing action that saliva provides for the teeth can be severely compromised. This can lead to a form of multiple caries that occurs after radiotherapy has damaged the salivary glands.
The changes that occur in the oral environment after radiotherapy portals have damaged the salivary glands may cause rapid and widespread destruction of teeth that previously had no dental pathology [65]. It is postulated that radiation alters the organic and inorganic matrix of enamel and the remaining tooth structure [47]. Decalcification may be favored over remineralization as an initiator of the carious process. The decrease in pH levels, which is commensurate with the amount of damage to the salivary glands, begins the creation of a caries-prone oral environment. When the serous component of saliva decreases and the viscosity increases, adherence of cariogenic bacteria to tooth structure increases. These organisms thrive in the more acidic oral environment that develops after radiotherapy.
These factors, coupled with the difficulty patients have with their oral hygiene maintenance amidst sensitive teeth and soft tissues, create a problem known as "radiation caries." This is an aggressive and rapid form of dental decay, targeting parts of the tooth that are usually not prone to decay. The smooth buccal (outer) and lingual (inner) walls of the tooth become involved with rapidly advancing carious lesions. The area of the tooth that is closest to the gingival tissues, the cervical area, is a frequent point of origin. The process can also affect the incisal edges of anterior teeth and the cusp tips of posterior teeth. Within weeks or months, the process renders teeth that were previously devoid of any dental pathology completely destroyed.
Extractions of the teeth should only be done after a consultation with the patient's primary care physician. Oral surgery procedures can produce extensive postsurgical complications, with significant morbidity and even death in patients who have undergone a full course of radiotherapy.
The most serious of the complications postradiotherapy is osteoradionecrosis (ORN), occurring in 3% to 10% of patients [66]. This is defined as necrosis of the bone in areas that have received radiotherapy. Patients who have received doses of radiation for head and neck malignancies in excess of 6,000 cGy have the highest risk of this pathologic entity [66,67]. The blood vessels that supply the bones with oxygen and nutrients become hyalinized, with a subsequent decrease in the ability to perfuse the tissue with enough oxygen-rich blood. Areas of bone supplied by these damaged vessels lack the oxygen and nutrients necessary to sustain the appropriate levels of metabolism. These areas of bone become ischemic and ultimately necrotic. The mandible is affected more frequently because it has less of a blood supply than the maxillary arch [66]. Necrotic pieces of bone may be small fragments or large sections whose loss undermines support for either arch. A pathologic fracture of the affected arch is a possible complication. Three grades of ORN have been categorized [67,68]. Grade I occurs in close proximity to the completion of surgery and radiotherapy. Exposed alveolar bone is observed [67]. Grade II designates ORN that does not respond to hyperbaric oxygen therapy and requires sequestrectomy/saucerization [67]. Grade III is demonstrated by full-thickness involvement and/or pathologic fracture. Patients may demonstrate grade I or III ORN at initial presentation [67].
Given the tumoricidal doses of radiation used, the 6,000 cGy threshold is easily reached for most patients with head and neck malignancies. Changes within the bone marrow include fibrous and fatty degeneration. The cells responsible for the production of bone, the osteocytes, are greatly diminished in number secondary to radiotherapy. The cells whose function is the resorption of bone, the osteoclasts, have fewer losses after radiotherapy. Thus, the dynamics of bone metabolism now favor bone resorption rather than bone apposition [60]. When this is combined with the damage to the blood vessels, the risk of ORN will be present for the remainder of the patient's life. Unfortunately, the passage of time does little to reverse the damage and the subsequent risk of ORN.
Treatment for ORN is variable. Small pieces of necrotic bone may migrate through the tissue and can be removed under local anesthesia. Larger segments of bone may require hospitalization for their removal. The risk of osteomyelitis, an infection of the bone, is increased in the patient who has undergone radiotherapy. The bony segments that perforate the mucosal tissues create a portal of entry for microbial organisms of the oral flora. Aggressive surgical and antibiotic treatment is needed to debride the area and resolve the infection. Hyperbaric oxygen treatments may help in the regeneration of new blood vessels with a resultant increase in the oxygen supply to the affected bone [69]. There is also evidence to suggest that hyperbaric oxygen treatments may be helpful as a therapy for soft tissue injury caused by radiation, as well as restoring tissues and cells damaged by chemotherapy and radiation treatments [66]. However, routine use is not recommended, and clinicians should assess any potential benefit to the patient on a case-by-case basis [67,70]. Any oral surgery procedure increases the risk of the development of spontaneous ORN, even if it is performed years after the last radiotherapy treatment. Trauma to the soft tissue by any means also causes a localized area of inflammation and infection that can extend to the bone and cause ORN. Bone that has been irradiated can undergo dire consequences from seemingly minor events.
Patients can experience a wide range of undesirable effects from any treatment modality, and radiotherapy is no exception. One such experience common to many patients undergoing radiotherapy is hypogeusia, the partial loss of the sensation of taste, or ageusia, the complete loss of this sensory function. Taste buds are very sensitive to ionizing radiation and begin to experience damage when a cumulative dosage of 1,000 cGy has been given. When the cumulative dose of 6,000 cGy has been reached, damage to the taste buds is usually permanent with the sensation of taste being lost [71]. Thus, if the oral malignancy being irradiated is in the area of the taste buds, the extent of damage and the ability to regain the sensation of taste will depend on the cumulative dose of radiation and the number of taste buds involved. The lower the dose and exposure, the better the chance that the sensation of taste will be restored. Patients should be counseled about the problems associated with the overcompensation of this loss by eating foods that are high in sugar content or excessively spicy.
A resident oral fungal organism with pathogenic capabilities, Candida albicans, causes a common opportunistic infection in the oral tissues of patients receiving radiotherapy. The normal competitive mechanisms among the microbial species of the oral environment and the immunocompetence of the host are usually sufficient to prevent infection of the mucosal tissues by this fungal organism. After radiotherapy, both of these protective mechanisms are altered, which can result in candidiasis in the oral tissues. This may be especially painful and even difficult to diagnose if it is superimposed on areas of mucositis.
The most significant concern is that a Candida infection superimposed over an area of mucositis could be a source of a regional or systemic fungal infection, which could have fatal consequences in a patient already weakened by illness, surgery, radiotherapy, and/or chemotherapy. Treatments for these infections consist of antifungal oral suspensions, such as nystatin, that follow a swish-and-swallow protocol (used with varying degrees of efficacy), or systemic fluconazole (highly effective for prophylaxis and treatment) [72]. Antifungal lozenges are difficult to use in patients whose salivary flow has diminished. Patients who wear complete or partial dentures, orthodontic retainers, or night guards should disinfect these appliances in accordance with the manufacturers' directions (e.g., soaking in antifungal solutions). The acrylic portions of these appliances have microscopic porosities in which C. albicans organisms thrive and re-infect oral tissues that have been cleared of the infection. Systemic fungal infections in these patients have a high mortality rate and should be treated with intravenous antifungal agents in a hospital setting.
Trismus, a condition in which the muscles that coordinate the functional range of jaw movements become spasmodic and contracted, can affect patients weeks or months after radiotherapy has been initiated [72]. Irradiation causes a thickening and scarring of the blood vessels that supply these muscles. The decreased oxygen and nutrient supply cause scars to form among the muscle fibers. This results in a state of relative contraction and a loss of range of motion. The onset of this problem is more gradual than that of mucositis because the muscle cells have a slower rate of mitosis. The prevalence of trismus increases with greater doses of radiation, and levels in excess of 60 Gy are more likely to cause the condition. Patients who have been previously irradiated and who are being treated for a recurrence appear to be at higher risk of trismus than those who are receiving their first treatment [72]. A physical therapist can recommend exercises for the facial musculature that minimize this problem. Preventive exercises should be employed before trismus becomes established, as it is difficult to regain muscle function and elasticity after this problem is firmly developed.
Oral complications secondary to surgery and radiotherapy for the treatment of malignancies may occur in patients with optimal oral health. These problems are exacerbated for those patients who have carious lesions, periodontal disease, problematic wisdom teeth, fractured teeth with sharp exposed edges, and prosthetic appliances that fit poorly and persistently traumatize the tissues.
A complete clinical and radiographic examination of the teeth and soft tissues should be completed as far in advance as possible from the surgical phase of oral cancer therapy. This will allow sufficient healing time for the extractions of teeth with unrestorable decay and advanced periodontal disease. Partially erupted wisdom teeth should be removed if they are in an area to be irradiated. Teeth with dental caries should be restored to optimal clinical condition. Teeth in which the carious process has extended into the pulp and has caused irreversible inflammation or necrosis should undergo root canal therapy or be extracted. Those teeth that cannot have deep periodontal pockets reduced to levels that will facilitate oral hygiene should be extracted. Prosthetic appliances should be adjusted so that their use will not promote tissue trauma. The goal is definitive treatment, avoiding a "watch and wait" approach. Patients should be informed that dental problems may exist without any symptoms and that lack of treatment will contribute to infections and even ORN after the completion of oral cancer therapy.
All patients should receive oral hygiene instruction and nutritional counseling. Manufacturers offer special sponge-like toothbrushes with toothpaste impregnated into the foamy material that may provide for an adequate means of cleansing the teeth without causing soft tissue trauma. The use of dental floss or dentotape for the interproximal areas should only be done if it can be accomplished atraumatically. Patients should demonstrate that proper flossing technique is within their capability.
Mouth rinses that contain alcohol may irritate the mucosal tissues and increase the dryness within the mouth. If an alcohol-based mouth rinse can be tolerated, 0.12% chlorhexidine gluconate is an excellent adjunct to the oral hygiene regimen [73]. This mouth rinse has substantivity, the ability to adhere to the tissues within the oral environment for several hours. This bactericidal formulation diminishes the number of bacteria associated with dental caries and periodontal disease. However, as discussed, chlorhexidine may cause additional discomfort for many patients [48].
All patients who will retain some or all of their natural teeth should have custom fluoride trays made before oral cancer treatment. These trays serve as reservoirs for a neutral formulation of 1.1% sodium fluoride or 0.4% stannous fluoride gels, depending on the composition of the patient's dental restorations [74]. These trays should be worn about 10 minutes daily, and patients should refrain from eating or drinking for 30 minutes after the fluoride treatment. Patients who do not want to use trays may brush the gels onto their teeth. Patients should brush their teeth after eating using a soft toothbrush and fluoride toothpaste [75]. This regimen should be a lifelong commitment for these patients in an attempt to minimize the risk of dental caries in a postsurgical oral environment that poses a high risk of dental caries.
Before surgery and radiotherapy for oral cancer is begun, patients should have an appointment for an oral assessment. The status of the teeth and the soft tissue should be scrutinized to minimize the chance of any condition that would lead to an infection necessitating oral surgery procedures, especially after radiotherapy. If a dental emergency develops that requires an extraction of a tooth, a 14-to 21-day window of healing should be allowed prior to radiotherapy to minimize the risk of ORN. Recall appointments should be frequent to allow for the examination of the oral tissues, as there is always a chance that an oral malignancy can recur at the original site or a new lesion can arise. These appointments also allow for an opportunity to evaluate oral hygiene status, presence of carious lesions, periodontal condition, and overall condition of the oral mucosa.
Rehabilitation of the patient with oral cancer is a challenging experience. The extent of necessary rehabilitation is proportionate to lesion size and the presence of metastasis. Larger squamous cell carcinoma lesions can engulf nerves, muscle, and bone. As noted, the removal of larger lesions adversely affects the ability to eat, speak, swallow, and enjoy the previous quality of life. Cosmetic disfigurement may not always be correctable to the patient's satisfaction. The team approach, involving the surgical and radiotherapy team, dentists, oral surgeons, oral and maxillofacial prosthodontists, nurses, nutritionists, occupational therapists, speech therapists, physical therapists, pharmacists, and plastic surgeons, may be needed. Counseling may be necessary to assist these patients as they face life from an entirely new perspective. Because most patients with oral cancer have a history of tobacco use, tobacco cessation education is an important aspect of patient recovery.
According to the Centers for Disease Control and Prevention, the death rate caused by cancers of all types is second only to heart disease [76]. During the 1990s, the incidence of cancer and death rates from this group of diseases actually declined. However, due to an increasing population, the actual number of deaths from cancer has increased [76].
Malignancies that involve individual organs, organ systems, or the bone marrow are usually treated by surgery, chemotherapy, and localized radiotherapy. When the primary lesion of squamous cell carcinoma arises within the oral cavity, chemotherapy is not typically a part of treatment. When chemotherapy is used postsurgically for organic or systemic malignancies, severe oral complications may also occur. When radiotherapy involves treatment of a malignant neoplasm that is distant from the oral and maxillofacial complex, oral complications rarely develop.
Because chemotherapy regimens are introduced intravenously, these drugs can interact with cells anywhere in the body. Chemotherapeutic agents exert their effects by interaction with the nuclei of malignant cells. Interference with DNA production, separation of the DNA helix, and disruption of protein synthesis are mechanisms by which the rapidly dividing and highly mitotic malignant cells are destroyed [77]. Normal cells, which undergo frequent turnover, can only be replaced if their successors also undergo frequent mitosis and cell division. Many chemotherapeutic agents exert their deleterious effect on normal cells as a result of the mitotic similarities between rapidly dividing malignant cells and those of normal cells. Because the cells of the oral mucosa undergo frequent turnover, they are subject to the nonspecific detrimental effects of chemotherapy.
The oral tissues are also subject to other problems, such as bleeding and infection, caused by the effects of chemotherapy on the cells from which the formed elements of human blood are produced. A review of these cells and their functions in the clotting mechanism and in appropriate immune function is necessary before the effects that chemotherapy has on these cellular elements, and ultimately the host, can be understood.
All blood cells are formed through the process of hematopoiesis, beginning with an undifferentiated cell, the hemocytoblast. Erythrocytes, platelets (thrombocytes), and the spectrum of the granular leukocytes (neutrophils, basophils, and eosinophils) are produced in the red bone marrow. This productive tissue is located in several bones, including the sternum, ribs, pelvis, and vertebrae. The agranular leukocytes are produced both in the red bone marrow and lymphoid tissue, such as the tonsils, spleen, and lymph nodes. Erythrocytes, containing their large hemoglobin molecules, are essential for carrying oxygen to the tissue. Platelets are a critical component of the blood clotting mechanism. The granular and agranular leukocytes serve different functions within the immune system. Any procedure or medication that interferes with the production of any of these components can cause systemic problems. Chemotherapy is a significant source of these problems.
When the number of platelets produced or the quality of those in existence are diminished, oral bleeding can occur. The normal range of platelets is 150,000–450,000 per mm3 of blood. Spontaneous bleeding occurs when the platelet count decreases to 20,000–50,000 per mm3 of blood [78]. When platelets contact a damaged blood vessel, they increase in size and adhesiveness and form a plug upon the damaged vessel. Some chemotherapeutic agents alter the ability of platelets to adhere to each other in the formation of a fibrous plug, which is required for hemostasis. Others may interfere with actual platelet production and decrease the number of platelets available. Regimens that use more than one chemotherapeutic agent may affect both platelet quality and production.
Interference with coagulation causes oral manifestations, including petechiae, ecchymoses, or oozing of blood [79]. The most common areas in which petechiae are found intraorally include the palate, gingiva, lips, and tongue. Petechiae are small areas of bleeding within the tissue that occur because of a decreased platelet count. Similarly, bleeding submucosally or subcutaneously due to platelet deficiencies in quality or quantity may produce ecchymoses. These lesions can occur anywhere within the oral tissues and appear as a dark red or reddish-blue area submucosally. They are exacerbated by accidental trauma or by prostheses that irritate the tissues. The most disconcerting problem for the patient is hemorrhage, which occurs spontaneously or with actions such as eating, brushing, or flossing. This problem is exacerbated in patients who have chronically inflamed gingival tissues characteristic of gingivitis and periodontal disease. Ideal depth of the gingival sulcus in health is 3 mm or less. As gingivitis and periodontal disease progress, destruction of the epithelial attachment causes this sulcus to become deeper. Cleansing the pocket depth becomes increasingly difficult, with a resultant state of chronic inflammation. As alveolar bone is lost during the progression of periodontal disease, the gingival tissues become poorly attached to the tooth and bone.
An environment of continually deepening periodontal pockets causes severe soft tissue inflammation. Despite this, tissues in this pathologic state often do not bleed spontaneously. Patients receiving chemotherapy, however, may have spontaneous gingival bleeding even if the depth of the gingival sulcus is not excessive. The clots usually appear as dark red and are friable, with slight bleeding evident when they are removed. Patients may experience this at any time, but it is most noticeable upon awakening in the morning. Dried blood from nocturnal bleeding can be encrusted on the lips, tongue, or anywhere in the oral mucosa. Sharp edges of fractured teeth or broken fillings, dental restorations that extend below the gingival crest, prostheses that cause tissue irritation, and partially erupted wisdom teeth are all potential sources that compromise tissue integrity and allow easy bleeding during chemotherapy. When bleeding is seen within the oral cavity, the patient should be referred to their physician, as internal bleeding in other areas of the body is possible.
The effect of chemotherapy on hemostasis subsides for most patients after the completion of the regimen. Even basic dental treatment, including prophylaxis, should not be performed until laboratory values ascertain that the platelet levels have returned to a range that is acceptable for hemostasis. Further diagnostic tests, such as a prothrombin time, may need to be done. The oncologist should be consulted before any invasive treatment is planned, as patients can have a wide interval of recovery times after chemotherapy ends. Emergency dental treatment that cannot be postponed, such as oral and maxillofacial trauma or painful exacerbations of dental problems, may need to be performed in a hospital setting.
Oral infections that are usually treated successfully with standard antibiotics can become a life-threatening problem for patients receiving chemotherapy. Oral infections may be bacterial, fungal, or viral in origin. Chemotherapy interferes with the production of the granular and agranular leukocytes, which are important components of the defense mechanism of the immune system. Oral infections in the aftermath of chemotherapy are common and may manifest into systemic conditions [80].
As mentioned, the normal host defense mechanisms and competitive inhibition among the oral microflora organisms are altered in many patients after chemotherapy. Any bacterial species have the potential to become a local or systemic pathogen. Pathologic dental conditions that preclude adequate cleansing, such as periodontal disease, necrotic pulps that have caused periapical infections, or partially erupted wisdom teeth, are potential sources of acute infections in patients receiving chemotherapy. The denuded, ulcerated areas of mucositis also facilitate a means of systemic bacterial dissemination. Antibacterials are indicated either as prophylaxis or as treatment if patients present with clinical signs of infection [81].
Oral infections of fungal origin (with the potential to spread systemically) occur in as many as 38% of patients receiving chemotherapy [80]. As mentioned, C. albicans is a resident fungal organism in the oral microflora. This opportunistic pathogen thrives in the oral environment of a host who is immunologically compromised. Oral candidiasis has different manifestations and degrees of severity. Angular cheilitis occurs when these organisms infect the commissures of the lips and the surrounding skin. The affected areas are sore and can crack and bleed easily. Treatment with a topical antifungal (such as miconazole) that is usually successful in the immunocompetent patient may not be successful in patients with cancer.
Pseudomembranous candidiasis features white to yellow-white raised plaques that may occur on any oral surface. These plaques may be wiped away from the underlying mucosal surface and an erythematous base will be revealed. This fungal infection can spread to the pharynx and esophagus by direct extension. Organisms that infect an area of mucositis have a portal for hematogenous dissemination and cause invasive candidiasis. Treatment with the swish-and-swallow regimen of nystatin may not work as well, or as quickly, in the immunocompromised patient [72]. Systemic antifungals, such as fluconazole, caspofungin, micafungin, anidulafungin, or lipid formulation of amphotericin B, may be necessary [82]. Another antifungal medication, voriconazole, is also available, but the side effects associated with its use are more severe and it offers little advantage over fluconazole as initial therapy [82]. The resistance of fungal organisms to these medications is becoming an increasing problem. Systemic antifungal medications should be prescribed with care, as they can interact with many other medications to produce serious side effects. Patients with impaired liver function may be unable to take these medications due to the risk for potentially fatal hepatotoxicity [51]. Prosthetic appliances that are made of acrylic should also be treated to destroy any inhabitant fungal organisms [82]. Some patients (e.g., neutropenic patients) benefit from a course of prophylactic antifungal medication (in recommended order: fluconazole, posaconazole, caspofungin) during chemotherapy [82]. Itraconazole is available for prophylaxis but is not recommended, except in the instance of fluconazole-refractory disease [82]. Isavuconazole, an expanded-spectrum antifungal approved in 2015, has excellent in vitro activity against Candida species [82,83].
The activation of herpes simplex virus or varicella zoster virus (shingles) is a common occurrence in immunocompromised patients [84]. These viruses reside and lie dormant in the ganglia of neurons until a triggering event or stressor stimulates their activation. In immunocompromised patients, these viral infections are more susceptible to systemic or organ dissemination [85]. Because they reside in the actual nerve, these viruses cannot be destroyed by any medical procedure.
Intraoral herpetic lesions may appear as large ulcerative areas and can resemble mucositis. Only a culture for this virus distinguishes between the two. When varicella zoster manifests facially, it follows the sensory distribution of either the right or left trigeminal nerve. The affected areas are much larger than those infected with the herpes simplex virus, and there is a commensurate increase in pain. The skin is most commonly involved, although the mandibular division of the trigeminal nerve may allow for an intraoral manifestation.
Analgesic and antiviral medications will decrease the symptoms associated with the outbreak. The ultimate goal of therapy in cases of post chemotherapy varicella zoster is to prevent or control systemic and/or organ dissemination, as the majority of mortalities related to varicella zoster are attributable to these complications [85]. Acyclovir is recommended, especially for immunosuppressed patients [85,86,87,88]. Valacyclovir or famciclovir may also be used [86,87,88]. Brivudin is contraindicated for patients receiving chemotherapy as the risk of fatal interaction with certain chemotherapeutic agents has been established [85,86,88]. Brivudin is not currently available in the United States [51]. Unlike the healing pattern for the herpes simplex virus, varicella zoster may leave scars upon healing and may have painful exacerbations of posthealing neuralgia. If the ophthalmic branch of the trigeminal nerve is involved, an ophthalmologist should be consulted as involvement of the cornea may lead to corneal scarring and blindness [85].
The use of large doses of IV bisphosphonates, as is common among patients with multiple myeloma or metastatic breast cancer, has been linked to the development of jaw osteonecrosis [89]. This phenomenon was previously referred to as bisphosphonate-related osteonecrosis of the jaw. However, the preferred term is now medication-related osteonecrosis of the jaw (MRONJ), which is favored due to the rise in osteonecrosis cases associated with other antiresorptive (denosumab) and antiangiogenic therapies [90,91]. MRONJ is diagnosed by the presence of three characteristics [90]:
Current or previous treatment with antiresorptive or antiangiogenic agents
Exposed bone or bone that can be probed through an intraoral or extraoral fistula(e) in the maxillofacial region that has persisted for more than eight weeks
No history of radiation to the jaws or obvious metastatic disease to the jaws
The risk of developing MRONJ increases with extended use of the medications. According to one meta-analysis, the majority of cases (60%) were precipitated by tooth extraction or oral surgery, which may involve trauma to the alveolar bone during the procedure as well as complications arising during recovery [89,92,93]. Among patients with jaw osteonecrosis who have not had oral surgery or tooth extraction, the use of dental prostheses or other oral problems are often present [94]. The results of one study suggest that the accurate diagnosis of MRONJ at the time of extraction is critical, and that an additional category of MRONJ that encompasses cases of bony necrosis found in the extraction socket during tooth extraction procedures may be needed. The study results also suggest that the routine discontinuation of bisphosphonates several months prior to the extraction procedure should be considered carefully [95]. All patients who are being treated with bisphosphonates or denosumab should be counseled regarding the possibility of MRONJ developing, including early signs, and the importance of good oral hygiene [90].
When MRONJ does develop, the stage of the disease should be determined, which will in turn guide the treatment plan. MRONJ is categorized as [90]:
Stage 0: No exposed/necrotic bone with non-specific symptoms or clinical and radiographic findings
Stage 1: Exposed/necrotic bone with no symptoms and no evidence of infection
Stage 2: Exposed/necrotic bone with pain and clinical evidence of infection
Stage 3: Exposed/necrotic bone with pain, infection, and one or more of the following:
Exposed necrotic bone extending beyond the alveolar region
Oral antral/oral nasal communication
Pathologic fracture
Extra-oral fistula
Osteolysis extending to the inferior border of the mandible or sinus floor
Patients with stage 1 MRONJ are usually treated conservatively, with oral antimicrobial rinses (e.g., chlorhexidine 0.12%) and no surgical intervention. Stage 2 MRONJ is treated with the use of antibiotic therapy in addition to oral antimicrobial rinses; certain cases may require surgical intervention to reduce the volume of colonized, necrotic bone. Stage 3 disease often impacts quality of life and requires more intensive intervention. These patients usually require surgical debridement/resection in combination with antibiotic therapy [90].
Systemic chemotherapy can have oral manifestations that are dependent on the agent(s) used, their dosage, and the duration of therapy. As with any medication, there is a considerable variability in the tolerance for a given pharmacotherapeutic regimen as well as any side effects. As noted, one such effect may be xerostomia. This problem is associated with some chemotherapeutic agents more than others. The parotid glands, with their serous secretions, are the glands most frequently affected. Because chemotherapeutic agents are administered as a systemic therapy, these substances course through all salivary glands. With the serous component reduced, the saliva develops a mucus-laden, ropey consistency. The decreased lubrication exacerbates the pain associated with concurrent areas of mucositis and makes it difficult to wear any dental prostheses. Eating, speaking, and swallowing may become difficult, and the taste of foods may be altered.
While radiotherapy-induced xerostomia and all of the problems associated with it are long-term or permanent, those associated with chemotherapy dissipate after the completion of the regimen. Chemotherapy is usually given in an incremental fashion, with several days or weeks separating the appointments. Xerostomia may be a continuous problem until enough time has elapsed after the last session. A 2015 Cochrane Review concluded that cryotherapy (i.e., holding ice chips or ice water in the mouth from 5 minutes prior to 30 minutes after treatment) is effective in reducing mucotoxicity [96]. A simple act to palliate the symptoms associated with this xerostomia and mucositis is to frequently suck on ice chips. Being that the cost and risks of this preventative measure are virtually nonexistent, cryotherapy should always be considered.
Neurologic effects may be seen in some patients on chemotherapy. Vincristine sulfate is the chemotherapeutic agent most commonly associated with this problem [51,97]. Chemotherapeutic agents exert varied effects on any nerve. The most commonly affected nerves that serve the oral and maxillofacial complex are the facial and trigeminal nerves. The facial nerve is the major source of motor innervation for the muscles of facial expression. Transient neural toxicity manifests as weakness of these muscles and decreased facial muscular coordination. The trigeminal nerve is another cranial nerve that provides sensory innervation to many portions of the face and for those structures within the oral cavity. Symptoms of neural toxicity present in a variety of ways. Pain that mimics that of dental origin may affect both the maxillary and the mandibular arches. There may be temporary paresthesia in the soft tissues or in the teeth. Pain in the temporomandibular joint (TMJ) may mimic TMJ problems. Patients should be reassured that these problems will regress after chemotherapy is completed.
Special considerations for the oral complications of chemotherapy include the pediatric population and those patients who receive bone marrow transplants. Unfortunately, many children must undergo the rigors of chemotherapy. This often affects tooth development and craniofacial growth in children younger than 12 years of age [98]. Effects are even more severe in children younger than 5 years of age [98]. Additionally, children are subject to all of the other chemotherapy-induced problems. Their immature immune systems are less capable of the provision of defense against oral infections. Any anticipated dental treatment should be cleared through the oncologist.
Patients who have received bone marrow transplants are particularly prone to infections [81]. Chemotherapy and radiation therapy are used to eliminate the normal and malignant cells within the bone marrow in anticipation of replacement marrow from a donor. As a result, the patient has virtually no immunocompetence. Patients are usually required to take immunosuppressive drugs for life and may be subject to life-threatening sepsis from dental infections that would be self-limiting in immunocompetent individuals. Any dental problem that has the potential to cause an infection should be eliminated before the patient begins therapy for the bone marrow transplant.
The guidelines established for dental pretreatment of patients who will receive radiotherapy should also be followed by those receiving chemotherapy. The major additional caveat is that these patients may have decreased defense mechanisms against oral infections for an extended period of time. Like bone marrow transplant patients, some patients receiving chemotherapy may be so immunocompromised that the cardinal signs of warmth, redness, and swelling may be completely lacking as a warning sign of an infection. It is imperative that within this patient population, any dental pathology related to the teeth, the periodontium, or the soft tissue is eliminated well in advance of chemotherapy [99].
Postchemotherapy dental treatment should include frequent recall appointments to examine the oral cavity and reinforce the need for meticulous oral hygiene. Antimicrobial prophylaxis may be required for any procedure in which bleeding is anticipated due to the increased risk for infection. Laboratory values for the formed elements of human blood may be necessary. The healthcare team, including dentists and oncologists, should be in communication regarding patient dental pretreatment and post-treatment [99,100].
As a result of the evolving racial and immigration demographics in the United States, interaction with patients for whom English is not a native language is inevitable. Because patient history and education are such vital aspects of the diagnosis of oral lesions and the prevention and treatment oral complications of systemic cancer therapies, it is each practitioner's responsibility to ensure that information and instructions are explained in such a way that allows for patient understanding. When there is an obvious disconnect in the communication process between the practitioner and patient due to the patient's lack of proficiency in the English language, an interpreter is required.
In this multicultural landscape, interpreters are a valuable resource to help bridge the communication and cultural gap between patients and practitioners. Interpreters are more than passive agents who translate and transmit information back and forth from party to party. When they are enlisted and treated as part of the interdisciplinary clinical team, they serve as cultural brokers who ultimately enhance the clinical encounter.
It has been suggested that most people know someone who has been afflicted with cancer. Whether it is a family member, friend, or relative, this group of diseases has been associated with high morbidity and high mortality rates. Medical science has made considerable breakthroughs in the prevention, diagnosis, and treatment of cancer. Prevention of any form of cancer remains the ideal. If this cannot be realized, then early diagnosis and prompt treatment are possibly life-saving measures.
Patients should be educated about the warning signs of cancer and encouraged to maintain yearly check-ups with their primary care physician. If treatment for cancer ensues, patients should be informed that the potential oral complications of cancer treatment may result in fatal consequences. Continued improvement of medical technology will be a medium through which patients can be treated more effectively when cancer strikes. All members of the healthcare team must commit to providing the highest level of care and compassion for these patients. Perhaps one day cancer will be spoken of in the past tense.
| American Cancer Society |
| 1-800-227-2345 |
| https://www.cancer.org |
| National Cancer Institute |
| 1-800-4-CANCER |
| https://www.cancer.gov |
| City of Hope |
| 1-866-843-7557 |
| https://www.cityofhope.org |
| The Oral Cancer Foundation |
| 1-949-723-4400 |
| https://oralcancerfoundation.org |
1. Starr JR. The relative contribution of oral cancer risk factors may differ in younger as compared to older adults. J Evid Based Dent Pract. 2005;5(2):78-79.
2. The Oral Cancer Foundation. Oral Cancer Facts. Available at https://oralcancerfoundation.org/facts. Last accessed December 17, 2024.
4. American Cancer Society. Risk Factors for Oral Cavity and Oropharyngeal Cancers. Available at https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/causes-risks-prevention/risk-factors.html. Last accessed December 17, 2024.
5. National Institutes of Health, National Institute of Dental and Craniofacial Research. Oral Cancer. Available at https://www.nidcr.nih.gov/health-info/oral-cancer. Last accessed December 17, 2024.
6. National Cancer Institute. Cancer Stat Facts: Oral Cavity and Pharynx Cancer. Available at https://seer.cancer.gov/statfacts/html/oralcav.html. Last accessed December 17, 2024.
7. D'Souza G, Kreimer AR, Viscidi R, et al. Case-control study of human papillomavirus and oropharyngeal cancer. N Engl J Med. 2007;19(356):1944-1986.
8. Lingen MW, Abt E, Agrawal N, et al. Evidence-based clinical practice guideline for the evaluation of potentially malignant disorders in the oral cavity: a report of the American Dental Association. J Am Dent Assoc. 2017;148(10):712-727.
9. Centers for Disease Control and Prevention, the National Institutes of Health, and the HIV Medicine Association/Infectious Diseases Society of America. Treating opportunistic infections among HIV-infected adults and adolescents. MMWR. 2004;53(RR15):1-112.
10. American Association of Oral and Maxillofacial Surgeons. Oral Cancer Fact Sheet. Available at https://aaoms.org/wp-content/uploads/2022/06/2017_oral_cancer_fact_sheet.pdf. Last accessed December 17, 2024.
11. National Collaborating Centre for Primary Care. Referral Guidelines for Suspected Cancer in Adults and Children. Available at https://www.ncbi.nlm.nih.gov/books/NBK45765. Last accessed December 17, 2024.
12. Wilson DF, De-Jun J, Pierce AM, Wiebkin OW. Oral cancer: role of the basement membrane in invasion. Aust Dent J. 1999;44(2):93-97.
13. Strassburg M, Knolle G. Diseases of the Oral Mucosa: A Color Atlas. 2nd ed. Carol Stream, IL: Quintessence Publishing Co., Inc.; 1994.
14. The Oral Cancer Foundation. CDC Oral Cancer Background Papers: Premalignant Lesions. Available at https://oralcancerfoundation.org/cdc. Last accessed December 17, 2024.
15. Sciubba JJ. Improving detection of precancerous and cancerous oral lesions: computer-assisted analysis of the oral brush biopsy. J Am Dent Assoc. 1999;130:1445-1457.
16. National Cancer Institute. What is Cancer? Available at https://www.cancer.gov/about-cancer/understanding/what-is-cancer. Last accessed December 17, 2024.
17. National Institutes of Health. Environment and Gene Interactions Cancer Module. Available at https://www.niehs.nih.gov/health/assets/docs_a_e/environment_and_gene_interactions_cancer_module_508.pdf. Last accessed December 17, 2024.
18. Perez-Ordonez B, Beauchemin M, Jordan RCK. Molecular biology of squamous cell carcinoma of the head and neck. J Clin Path. 2006;59(5):445-453.
19. Barnes L. Surgical Pathology of the Head and Neck. 3rd ed. New York, NY: Informa Healthcare; 2009.
21. Zhang L, Williams M, Poh CF, et al. Toluidine blue staining identifies high-risk primary oral premalignant lesions with poor outcome. Cancer Res. 2005;65(17):8017-8021.
22. Epstein JB, Sciubba J, Silverman S Jr, Sroussi HY. Utility of toluidine blue in oral premalignant lesions and squamous cell carcinoma: continuing research and implications for clinical practice. Head Neck. 2007;29(10):948-958.
23. Su WW, Yen AM, Chiu SY, Chen TH. A community-based RCT for oral cancer screening with toluidine blue. J Dent Res. 2010;89(9):933-937.
24. Sciubba JJ. Oral cancer and its detection: history-taking and the diagnostic phase of management. J Am Dent Assoc. 2001;132(Suppl 1):12s-17s.
25. 25. Svirsky JA, Burns JC, Carpenter WM, et al. Comparison of computer-assisted brush biopsy results with follow up scalpel biopsy and histology. Gen Dent. 2002;50(6):500-503.
26. National Institutes of Health, National Cancer Institute. Oral Cavity and Oropharyngeal Cancer Prevention: Incidence and Mortality. Available at https://www.cancer.gov/types/head-and-neck/hp/oral-prevention-pdq#section/all. Last accessed December 17, 2024.
27. Wiley InterScience. Reference Work: TNM Online. 8th ed. Available at https://onlinelibrary.wiley.com/doi/book/10.1002/9780471420194. Last accessed December 17, 2024.
28. National Institutes of Health, National Cancer Institute. Staging. Available at https://www.cancer.gov/about-cancer/diagnosis-staging/staging. Last accessed December 17, 2024.
29. World Health Organization. TNM Classification of Carcinomas of the Oral Cavity. Available at https://screening.iarc.fr/atlasoralclassiftnm.php. Last accessed December 17, 2024.
31. Scott SE, Grunfeld EA, McGurk M. The idiosyncratic relationship between diagnostic delay and stage of oral squamous cell carcinoma. Oral Oncol. 2005;41(4):396-403.
32. 32. Jensen A, Nolet PS, Diwan MA. Oral squamous cell carcinoma: an atypical presentation mimicking temporomandibular joint disorder. J Can Chiropr Assoc. 2004;48(4):266-272.
33. Carvalho AL, Pintos J, Schlecht NF, et al. Predictive factors for diagnosis of advanced-stage squamous cell carcinoma of the head and neck. Arch Otolaryngol Head Neck Surg. 2002;128(3):313-314.
34. Magge KT, Myers EN, Johson JT. Radiation following surgery for oral cancer: impact on local control. Laryngoscope. 2003;113(6):933-935.
35. De Crevoisier RMD, Bourhis J, Eschwege FMD. Modified fractionated radiotherapy in head and neck squamous cell carcinoma (HNSCC) re-irradiation in recurrent head and neck carcinomas. In: Brockstein B, Masters G (eds). Head and Neck Cancer. New York, NY: Springer; 2003.
36. Oral Cancer Foundation. Radiation. Available at https://oralcancerfoundation.org/treatment/radiation. Last accessed December 17, 2024.
37. Min YM, Lin YC, Wang YB, Wu DM. Dramatic and prolonged decrease of whole salivary secretion in nasopharyngeal carcinoma patients treated with radiotherapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):322-327.
38. Stanley J. Oral complications of radiation therapy and their management: a review. Detroit Dent Bull. 2000;69(7-8).
39. Ho C. Cetuximab in locally advanced head-and-neck cancer: defining the population. Curr Oncol. 2010;17(4):48-51.
40. Hiraishi Y, Wada T, Nakatani K, Negoro K, Fujita S. Immunohistochemical expression of EGFR and p-EGFR in oral squamous cell carcinomas. Pathol Oncol Res. 2006;12(2):87-91.
41. Goyal M, Shukla P, Gupta D, et al. Oral mucositis in morning vs. evening irradiated patients: a randomised prospective study. Int J Radiat Biol. 2009;85(6):504-509.
42. Shukla P, Gupta D, Munshi A, Agarwal JP. Cetuximab and cancers of the head and neck: tapping the circadian rhythm. Med Hypotheses. 2011;77(3):336-338.
43. Rubinstein EB, Peterson DE, Schubert M, et al. Clinical practice guidelines for the prevention and treatment of cancer therapy-induced oral and gastrointestinal mucositis.Cancer. 2004;100(9 Suppl):2026-2046.
44. Patni N, Patni S, Bapna N, Somani M, Gupta A, Ratnam BV. The role amifostine in prophylixis of radiotherapy induced mucositis and xerostomia in head and neck cancer. J Clin Onc. 2004;22(14S):5568.
45. Harrison JS, Dale RA, Haveman CW, Redding SW. Oral complications in radiation therapy. Gen Dent. 2003;51(6):552-560.
46. National Cancer Institute. Common Terminology Criteria for Adverse Events (CTCAE) Version 5.0. Available at https://ctep.cancer.gov/protocolDevelopment/electronic_applications/ctc.htm. Last accessed December 17, 2024.
47. Silverman S Jr. Oral cancer: complications of therapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(2):122-126.
48. 48. Elad S, Cheng KKF, Lalla RV, et al. MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Cancer. 2020;126(19):4423-4431.
49. Vadhan-Raj S, Goldberg JD, Perales MA, Berger DP, van den Brink MR. Clinical applications of palifermin: amelioration of oral mucositis and other potential indications. J Cell Mol Med. 2013;17(11):1371-1384.
50. National Cancer Institute. Palifermin. Available at https://www.cancer.gov/about-cancer/treatment/drugs/palifermin#:~:text=Palifermin%20is%20approved%20to%20prevent,followed%20by%20stem%20cell%20rescue. Last accessed December 17, 2024.
51. Wynn RL, Meiller TF, Crossley HL. Drug Information Handbook for Dentistry. 25th ed. Hudson, OH: Lexi-Comp, Inc.; 2020.
52. Hensley ML, Hagerty KL, Kewalramani T, American Society of Clinical Oncology. 2008 clinical practice guideline update: use of chemotherapy and radiation therapy protectants. J Clin Oncol. 2009;27(1):127-145.
53. Henke M, Alfonsi M, Foa P, et al. Palifermin decreases severe oral mucositis of patients undergoing postoperative radiochemotherapy for head and neck cancer: a randomized, placebo-controlled trial. J Clin Oncol. 2011;29(20):2815-2820.
54. ClinicaTrials.gov. A Study of Palifermin for the Reduction of Oral Mucositis in Subjects With Advanced Head and Neck Cancer. Available at https://clinicaltrials.gov/ct2/show/NCT00131638. Last accessed December 17, 2024.
55. Eilers J. Nursing interventions and supportive care for the prevention and treatment of oral mucositis associated with cancer treatment. Oncol Nurs Forum. 2004;31(4 Suppl):13-23.
56. Royal Children's Hospital Melbourne. Mouth Care: Oral Care of the Paediatric Oncology Patient and Haematopoieitic Stem Cell Transplant Patient. Available at https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/Mouth_Care_Oral_hygiene_for_HaematologyOncology_children. Last accessed December 17, 2024.
57. Farrington M, Cullen L, Dawson C. Assessment of oral mucositis in adult and pediatric oncology patients: an evidence-based approach. ORL Head Neck Nurs. 2010;28(3):8-15.
58. Potting C. Oral Mucositis: A Nurse's Perspective. Available at https://repository.ubn.ru.nl//bitstream/handle/2066/40148/40148_oralmu.pdf?sequence=1. Last accessed December 17, 2024.
59. Diaz-Arnold A. The impact of saliva on patient care: a literature review. J Prosthet Dent. 2002;88(3):337-343.
60. 60. Radke LM. Pre-radiation therapy dental evaluation. Greater Milwaukee Dent Assoc J. 1996;63(4):104-109.
61. Baharudin A, Khairuddin A, Nizam A, Samsuddin AR. Evaluation of irradiated salivary gland function in patients with head and neck tumours treated with radiotherapy. J Laryngol Otol. 2009;123(1):108-113.
62. Barker BF, Barker GJ. Oral management of the patient with cancer in the head and neck region. J Calif Dent Assoc. 2001;29(8): 619-623.
63. Nutting CM, Morden JP, Harrington KJ, et al. Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol. 2011;12(2):127-136.
64. Eisbruch A. Reducing radiation-induced xerostomia with highly conformal radiotherapy techniques. J Support Oncol. 2005;3(3):201-202.
65. 65. National Cancer Institute. Oral Complications of Chemotherapy and Head/Neck Radiation. Available at https://www.cancer.gov/about-cancer/treatment/side-effects/mouth-throat/oral-complications-hp-pdq#section/all. Last accessed December 17, 2024.
66. The Oral Cancer Foundation. Osteoradionecrosis. Available at https://oralcancerfoundation.org/complications/osteoradionecrosis. Last accessed December 17, 2024.
67. Blanchaert RH Jr. Osteoradionecrosis of the Mandible. Available at https://emedicine.medscape.com/article/851539-overview#a4. Last accessed December 17, 2024.
68. Marx RE, Johnson RP. Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol. 1987;64(4):379-390.
69. David LA, Sandor GKB, Evans AW, Brown DH. Hyperbaric oxygen therapy and mandibular osteoradionecrosis: a retrospective study and analysis of treatment outcomes. J Can Dent Assoc. 2001;67(7):384.
70. Sultan A, Hanna GJ, Margalit DN, et al. The use of hyperbaric oxygen for the prevention and management of osteoradionecrosis of the jaw: a Dana-Farber/Brigham and Women's Cancer Center multidisciplinary guideline.Oncologist. 2017;22(3):343-350.
71. Rankin KV, Jones DL (eds). Oral Health in Cancer Therapy: A Guide for Health Care Professionals. Austin, TX: DOEP, Texas Cancer Council; 1999.
72. National Cancer Institute. Oral Complications of Chemotherapy and Head/Neck Radiation: Infection. Available at https://www.cancer.gov/about-cancer/treatment/side-effects/mouth-throat/oral-complications-hp-pdq#_901. Last accessed December 17, 2024.
73. Pereira Pinto L, Batista de Souza L, Gordon-Nunez MA, et al. Prevention of oral lesions in children with acute lymphoblastic leukemia. Int J Pedatr Otor. 2006;70(11):1847-1851.
74. National Institute of Dental and Craniofacial Research. Oral Complications of Cancer Treatment: What the Dental Team Can Do. Available at https://www.nidcr.nih.gov/sites/default/files/2017-09/oral-complications-cancer-dental-team.pdf. Last accessed December 17, 2024.
75. Memorial Sloan Kettering Cancer Center. Mouth Care During Your Cancer Treatment. Available at https://www.mskcc.org/cancer-care/patient-education/mouth-care-during-your-treatment. Last accessed December 17, 2024.
76. Kochanek KD, Murphy SL, Xu J, Arias E. Deaths: final data for 2022. NCHS Data Brief. 2024;492:1-7.
77. Mealey BL, Semba SE, Hallmon WW. Dentistry and the cancer patient: part 1. Oral manifestations and complications of chemotherapy. Compendium. 1994;15(10):1252-1262.
78. Barker BF, Barker GJ. Oral complications and management of cancer chemotherapy. Northwest Dentistry. 1990;69(6):23-26.
79. Peterson DE, D'Ambrosio JA. Diagnosis and management of acute and chronic oral complications of nonsurgical cancer therapies. Dent Clin North Am. 1992;36(4):945-966.
80. Lalla RV, Latortue MC, Hong CH, et al. A systematic review of oral fungal infections in patients receiving cancer therapy. Support Care Cancer. 2010;18(8):985-992.
81. National Comprehensive Cancer Network. Clinical Practice Guidelines in Oncology: Prevention and Treatment of Cancer-Related Infections. Available at https://jnccn.org/view/journals/jnccn/14/7/article-p882.xml. Last accessed December 17, 2024.
82. Pappas PG, Kauffman CA, Andes D, et al. Clinical practice guidelines for the management of candidiasis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;62(4):e1-e50.
83. 83. U.S. Food and Drug Administration. News Release. FDA Approves New Antifungal Drug Cresemba [Archive]. Available at https://wayback.archive-it.org/7993/20171102201709/https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm437106.htm. Last accessed December 17, 2024.
84. American Cancer Society. Infections in People with Cancer. Available at https://www.cancer.org/treatment/treatments-and-side-effects/physical-side-effects/infections/infections-in-people-with-cancer.html. Last accessed December 17, 2024.
85. Dworkin RH, Johnson RW, Breuer J, et al. Recommendations for the management of herpes zoster. Clin Infect Dis. 2007;44(Suppl 1):S1-S26.
86. Janniger CK. Herpes Zoster Guidelines: Therapy and Prophylaxis Guidelines. Available at https://emedicine.medscape.com/article/1132465-guidelines#g2. Last accessed December 17, 2024.
87. Fashner J, Bell AL. Herpes zoster and postherpetic neuralgia: prevention and management. Am Fam Physician. 2011;83(12):1432-1437.
88. Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis. 2014;59(2):147-159.
89. Moore A, McQuay H, Derry S, Moore M. Bisphosphonates and jaw osteonecrosis. Bandolier. 2006;7:149-153.
90. American Association of Oral and Maxillofacial Surgeons. Position Paper: Medication-Related Osteonecrosis of the Jaw—2022 Update. Available at https://aaoms.org/wp-content/uploads/2024/03/mronj_position_paper.pdf. Last accessed December 17, 2024.
91. Goodell GG. Guidelines for Medication-Related Osteonecrosis Jaw: An Update. Available at https://www.aae.org/specialty/guidelines-for-medication-related-osteonecrosis-jaw-an-update/. Last accessed December 17, 2024.
92. Filleul O, Crompot E, Saussez S. Bisphosphonate-inducted osteonecrosis of the jaw: a review of 2,400 patient cases. J Cancer Res Clin Oncol. 2010;136(8):1117-1124.
93. Mozzati M, Arata V, Gallesio G, Carossa S. Tooth extraction and oral bisphosphonates: comparison of different surgical protocols. Joint Bone Spine. 2011;78(6):647-648.
94. Kim JW, Baik J, Jeon JH. Dental implant treatment after healing of bisphosphonate-related osteonecrosis of the jaw in the same region: a case report. J Korean Assoc Oral Maxillofac Surg. 2016;42(3):157-161.
95. Kang SH, Park SJ, Kim MK. The effect of bisphosphonate discontinuation on the incidence of postoperative medication-related osteonecrosis of the jaw after tooth extraction. J Korean Assoc Oral Maxillofac Surg. 2020;46(1):78-83.
96. Riley P, Glenny AM, Worthington HV, et al. Interventions for preventing oral mucositis in patients with cancer receiving treatment: oral cryotherapy. Cochrane Database Syst Rev. 2015;(12):CD0011552.
97. Sands S, Ladas EJ, Kelly KM, et al. Glutamine for the treatment of vincristine-induced neuropathy in children and adolescents with cancer. Support Care Cancer. 2017;25(3):701-708.
99. National Cancer Institute. Oral Complications of Chemotherapy and Head/Neck Radiation: Oral and Dental Management Before Cancer Therapy. Available at https://www.cancer.gov/about-cancer/treatment/side-effects/mouth-throat/oral-complications-hp-pdq#section/_28. Last accessed December 17, 2024.
1. National Collaborating Centre for Cancer. Suspected Cancer: Recognition and Referral. London: National Institute for Health and Care Excellence; 2023. Available at https://www.nice.org.uk/guidance/ng12. Last accessed December 20, 2024.
2. Lingen MW, Abt E, Agrawal N, et al. Evidence-based clinical practice guideline for the evaluation of potentially malignant disorders in the oral cavity: a report of the American Dental Association. J Am Dent Assoc. 2017;148(10):712-727. Available at https://jada.ada.org/article/S0002-8177(17)30701-8/fulltext. Last accessed December 20, 2024.
3. Riley P, Glenny A-M, Worthington HV, Littlewood A, Clarkson JE, McCabe MG. Interventions for preventing oral mucositis in patients with cancer receiving treatment: oral cryotherapy. Cochrane Database Syst Rev. 2015;(12):CD011552. Available at https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD011552.pub2/full. Last accessed December 20, 2024.
Mention of commercial products does not indicate endorsement.