The term "novel psychoactive substance" (or synthetic drug) refers to a new category of drugs on the market that have been created to circumvent existing laws on illicit drugs. This course will provide the most up-to-date information available on novel psychoactive substances, including the evolution of synthetic drug use; demographic characteristics of novel psychoactive substance users; the pharmacology, mechanism of action, and acute effects of novel psychoactive substances; approaches to reverse or manage acute toxicity; possible long-term effects; and prevention or treatment of novel psychoactive substance abuse.
- INTRODUCTION
- BACKGROUND OF NOVEL PSYCHOACTIVE SUBSTANCES
- NPS EMERGENCE AND EXPANSION
- EPIDEMIOLOGY
- PHENETHYLAMINE DERIVATIVES
- SYNTHETIC CATHINONES AND AMPHETAMINE/MDMA DERIVATIVES
- CANNABIMIMETICS
- TRYPTAMINES
- ARYLCYCLOHEXYLAMINE DISSOCIATIVE ANESTHETICS
- OPIOIDS
- BOTANICAL PRODUCTS
- ASSESSMENT, DIAGNOSIS, AND TREATMENT OF NPS TOXICITY
- NPS USE DISORDERS
- HARM REDUCTION
- PREVENTION
- CONSIDERATIONS FOR NON-ENGLISH-PROFICIENT PATIENTS
- CONCLUSION
- Works Cited
This course is designed for mental health professionals who are involved in the evaluation or treatment of persons who use novel psychoactive substances or whose past use has resulted in untoward effects.
The purpose of this course is to allow mental and behavioral health professionals to effectively identify, diagnose, treat, and provide appropriate referrals for patients who use novel psychoactive substances.
Upon completion of this course, you should be able to:
- Recall the history and epidemiology of the use of novel drugs of abuse.
- Analyze the effects and management of synthetic cathinones and other amphetamine analogs.
- Outline the pharmacology and effects of synthetic cannabinoids.
- Identify other synthetic drugs of abuse and emerging botanical products.
- Discuss strategies for the prevention and treatment of novel drug abuse and/or dependence.
Mark Rose, BS, MA, LP, is a licensed psychologist in the State of Minnesota with a private consulting practice and a medical research analyst with a biomedical communications firm. Earlier healthcare technology assessment work led to medical device and pharmaceutical sector experience in new product development involving cancer ablative devices and pain therapeutics. Along with substantial experience in addiction research, Mr. Rose has contributed to the authorship of numerous papers on CNS, oncology, and other medical disorders. He is the lead author of papers published in peer-reviewed addiction, psychiatry, and pain medicine journals and has written books on prescription opioids and alcoholism published by the Hazelden Foundation. He also serves as an Expert Advisor and Expert Witness to law firms that represent disability claimants or criminal defendants on cases related to chronic pain, psychiatric/substance use disorders, and acute pharmacologic/toxicologic effects. Mr. Rose is on the Board of Directors of the Minneapolis-based International Institute of Anti-Aging Medicine and is a member of several professional organizations.
Contributing faculty, Mark Rose, BS, MA, LP, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Alice Yick Flanagan, PhD, MSW
James Trent, PhD
The division planners have disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#76912: Novel Psychoactive Substances: Trends in Drug Abuse
A unique trend in recreational and problematic drug use began to emerge in the United States around 2008, with the introduction and proliferation of previously unknown psychoactive substances. By 2015, this trend became an established element of domestic and global recreational drug cultures. Novel psychoactive substances (NPS) describe a diverse range of emerging recreational drugs with molecular structures intended to circumvent existing drug laws. Unique to this group of NPS is their Internet and retail promotion, sales, and use as "legal high" substitutes for the standard illicit drugs cannabis, cocaine, amphetamines, 3,4-methylenedioxy-methamphetamine (MDMA), and lysergic acid diethylamide (LSD). This marketing approach has had some factual basis, as many NPS molecules have been derivatives, or have been designed to mimic the effects, of banned drugs [1]. Although the rates of NPS use peaked in 2011–2012 and have been steadily declining, education regarding NPS for healthcare professionals is necessary due to the substantially greater risks of adverse effects and toxicity syndromes than the illegal drugs whose prohibition spurred their introduction.
Users of NPS are attracted by the low cost, easy Internet and retail access, and the lack of legal risk (until banned) [2,29]. People on probation/parole or in certain vocations may gravitate to NPS to evade urine drug testing. The NPS phenomenon is characterized by an evolutionary arms race. Novel drugs are introduced, become banned, and are rapidly replaced by unregulated substances that become banned and rapidly replaced. Earlier NPS (2008–2012) were originally synthesized in academic or pharmaceutical laboratories for research or clinical use, and some briefly entered clinical practice. Post-2012, NPS generations are more likely to be unknown molecular entities that may be more toxic than previous NPS. Potential substances are introduced if the drug shows interesting market potential, has not been banned under a controlled substance act, and/or there is increasing scarcity of an established drug [3].
Synthetic cathinones and cannabimimetics remain the most widely used NPS classes and are sold under numerous product and brand names. NPS market turnover is high, but many NPS resemble their banned parent compound molecularly and pharmacologically [29].
Understanding the molecular structures and pharmacology of NPS classes can help clinicians predict their clinical effects and toxicity. NPS are undetected by drug toxicology screening, but NPS toxicity/overdose is readily managed by identifying the characteristic toxicity syndrome. This helps link substance to clinical effect, and understanding the pharmacologic profiles of the underlying molecular group can facilitate effective patient care [4,30]. Following emergency department care for NPS toxicity/overdose, many patients experience persistent neuropsychiatric symptoms. These can be effectively managed in the primary care setting but require clinician knowledge and education.
The American Academy of Family Physicians (AAFP) identified substantial knowledge gaps between published research evidence and clinical care of patients using NPS [5]. The AAFP also states these knowledge deficits can be remedied by continuing education that provides primary care providers with the information necessary to understand the clinical effects of NPS and the assessment, differential diagnosis, and management of medical and neuropsychiatric problems from NPS use [5].
This course will provide the most up-to-date information available on NPS while avoiding the more time-sensitive aspects of this "moving target." Discussion will include the evolution of their use; demographic characteristics of users; the pharmacology, mechanism of action, and acute effects of NPS; signs and symptoms of NPS intoxication; differential diagnosis and clinical management of severe adverse effects and toxicity from NPS use; possible long-term adverse effects; and prevention and treatment of NPS abuse and addiction. The bulk of this course addresses synthetic cathinones and cannabimimetics. These broad substance categories have been the most widely used NPS. As synthetic cathinones carry the potential for severe and fatal toxicity, assessment, diagnosis, and management of toxicity syndromes following their use is detailed.
NPS represents a broadly diverse category of novel substances, primarily those synthesized from phenethylamines, amphetamines, cathinones, aminoindanes, benzofurans, tryptamines, opioids, and arylcyclohexylamines; however, cannabimimetics and natural botanical products are also included. The molecular structure of common drugs is altered to produce a novel drug agent with shared pharmacologic and clinical properties of the parent drug that, owing to the novel molecular structure, falls outside of legal and regulatory control. This allows for their distribution and sales as "legal" alternatives to the established but banned drugs [6,7,8].
NPS are marketed as purportedly non-ingestible consumer products, most commonly legal highs, herbal incense (cannabimimetics), bath salts (synthetic cathinones), and also as potpourri, plant food, room deodorizer, and electronic-device cleaner [9,10]. All NPS are labeled by distributors "not for human consumption" in order to evade controlled substance analogue statutes for which prosecution requires the intent for human consumption. NPS purchased on the Internet are often labeled "research chemicals" (or RC), "intended for scientific research only," and "not for human consumption" [8,10]. Cannabimimetics now appear in liquid form for use in electronic cigarettes and vaporizer devices [12].
The brand names given to these products become associated with the drug effect; for example, Spice and K2 are popular brand names of cannabimimetic products packaged and sold as herbal incense and are purchased with the expectation of attaining a cannabis-like drug effect. Despite numerous product and brand names, "bath salts" and "Spice" have stuck and are generic terms for synthetic cathinones and cannabimimetics, respectively [9,10]. The popularity of NPS as "legal highs" has been propagated by online marketing, media coverage, and availability (without age restriction) in gas stations, convenience stores, "head shops," and on the Internet [9].
Since early humans first experienced euphoria with psychotropic plants more than 6,000 years ago, creative individuals have explored new ways of achieving drug-induced euphoria without getting in trouble with the law or dying [13]. These same human tendencies—the quest for novel yet legal psychoactive experiences—are driving the NPS phenomenon.
Although NPS emerged domestically in 2008, use has been widespread in Europe for years, prompted by recreational drug scarcity. Banned in 1985, MDMA (also referred to as Ecstasy) has remained very popular for its mild stimulant, euphoric, and entactogenic/empathogenic effects. The standard MDMA chemical precursor, safrole, is extracted from camphor trees (Cinnamomum camphora) in Southeast Asia. During the 1990s and 2000s, interdiction of safrole shipments into Europe and safrole oil at extraction sites limited precursor supplies for MDMA production, decreasing MDMA purity and availability in Europe. Another precursor, piperonyl methyl ketone (PMK), is banned, but in 2012, Chinese chemists introduced PMK-glycidate, a precursor easily converted to PMK. This reversed long-term scarcity, and from 2013 to 2015, Europe was flooded with high-potency MDMA pills produced by labs in the Netherlands and Belgium, with reports in 2016 indicating that seizures and stopped shipments were being seen in France, Bulgaria, and Spain, suggesting diversifying trafficking routes [14,15]. The MDMA resurgence continues, with the 2018 European Drug Report indicating 1 kg of piperonal, 1,077 liters of PMK, 63 liters of safrole, 5,905 kg PMK-glycidate, and 123 kg of N-tert-butoxycarbonyl-MDMA (Nt-BOC-MDMA) seized in 2016. Additionally, stopped shipment of 7,700 kg of piperonal and 1,000 kg of PMK-glycidate occurred in Europe in 2016 [14]. The European Drug Report indicates increased rates of seizure for both PMK and non-scheduled chemicals (PMK-glycidate and Nt-BOC-MDMA) for MDMA production [14].
Concurrently, the interception of cocaine shipments into Europe from South America made cocaine scarce and poor in quality. The European emergence of cathinones in the early to mid-2000s filled the void of MDMA and cocaine by promising users a legal-high substitute. Cathinones began replacing MDMA in Ecstasy and were introduced as over-the-counter "bath salt" products. The decreasing MDMA content in Ecstasy coincided with the 2009 emergence of cathinones in the United States, which were promoted as less expensive "legal high" Ecstasy and cocaine alternatives [3].
The 2021 European Drug Report indicates that the drug with the most increase of quantity being seized was methamphetamine (0.6 tons in 2018 versus 2.9 tons in 2019), when comparing a two-year period. This has also been proven to be the case when using a 10-year comparison (2009–2019). Increases in the quantity of drug seized within the decade are as follows [11]:
Methamphetamine (+931%)
MDMA (+456 %)
Cocaine (+279 %).
Herbal Cannabis (+226%)
Amphetamine (+180%)
Heroin (+17 %)
Cannabis resin (-19%)
The Internet has emerged as the new marketplace for NPS and plays an essential role in the NPS phenomenon through a variety of mechanisms. Most users and manufacturers obtain information from the Internet for acquisition, synthesis, extraction, identification, and use of NPS and other substances. The Internet also serves as the marketplace that connects manufacturers, suppliers, retailers, and end users. It is increasingly common that manufacturers, suppliers, retailers, web-hosting, and payment processing services are based in different countries, and this decentralization of the online drug markets adds to the difficulty for law enforcement control [14,15,16].
Information and transactions occur on the surface web as well as the "deep web." The "deep web" is a part of the Internet not accessible to traditional search engines, and the "dark web" is a small portion of the deep web intentionally hidden and inaccessible through standard web browsers, typically to evade detection of illicit activities. The dark web hosts drug cryptomarkets, which are only accessible through encryption software that provides a high level of anonymity. Cryptomarkets resemble online marketplaces such as eBay and provide sellers and buyers with an infrastructure to conduct transactions and services, including seller and buyer ratings and discussion forums. Cryptocurrencies like Bitcoin are used as the medium of exchange to facilitate anonymous transactions, and stealth packaging is used to facilitate transportation of small quantities of drugs through established commercial channels. Evidence suggests that many illicit drug purchases made on the deep web are intended for resale [14,15].
Internet facilitation of NPS began in the 2000s. 4-Methylmethcathinone (mephedrone) was "rediscovered" in the early 2000s and marketed as a "legal cocaine" and MDMA substitute and became the most widely used NPS in the European Union by 2009. Internet centrality in seller and user information exchange led to mephedrone being dubbed "the first Internet drug" [17]. Today, NPS Internet information-sharing and transactions are usually referred to as the "research chemical market."
The profit potential is also fueling the pace of NPS expansion. In 2010, a store in Missouri was selling the cannabimimetic product K2 for $20 per 3-gram packet. The owner stated he was making $7,000 per day in K2 sales [18].
A more recent example of the fast pace of NPS expansion and change is the potent synthetic cathinone alpha-pyrrolidinovalerophenone (alpha-PVP) or "flakka." Emerging in Florida and other U.S. regions in 2014 and 2015, "flakka" was sold to users in quantities as small as 100 mg for as little as $5. Bulk alpha-PVP was being purchased from China (via the Internet) for around $1,500/kg and shipped by worldwide express to local mid-level dealers. One kilogram provides 10,000 doses, which can yield $50,000 in sales—$48,500 in profit. This profit margin required a high sales volume. However, the $5 retail price means it is affordable for most users, and the high abuse/addiction potential of alpha-PVP assures repeat business. Younger and poorer populations are increasingly targeted as customers, and alpha-PVP is actively sold to, and by, homeless people [19]. However, since 2015, alpha-PVP was given attention through many law enforcement agencies and legislation, and other similar NPS that can circumvent legal action have become developed, illustrating the rapid growth and decline of many synthesized drugs [160,161]. In 2016, China banned 116 NPS, including "flakka," resulting in a dramatic reduction in the drug in the United States, especially Florida [21].
Non-chemists can synthesize NPS compounds with readily available raw materials or directly obtain the synthetic compounds. Most NPS chemicals are produced in China, in suburban laboratories near Chinese port cities for easy and rapid shipment to North America and Europe using ordinary commercial delivery services. Bulk quantities are also available and may be shipped to wholesalers in the United States and packaged for retail distribution [20].
The number of recently emergent NPS is unprecedented. In the United States between 2009 and 2014, 233 new synthetic compounds were identified, including 95 cannabimimetics, 51 synthetic cathinones, and 87 other NPS compounds [12]. The United Nations reported that 803 NPS were identified by member nations between 2009 and 2017, including cannabimimetics (31%), synthetic cathinones (18%), and phenethylamines (17%) [47]. As of late 2020, the European Union was tracking approximately 830 psychoactive substances, 46 of which were first reported in 2020, and almost all of which are NPS [11,14]. These figures are constantly becoming outdated and staying abreast of rapid changes in the NPS market is difficult [11,13].
The term "generation" is used to demarcate the time points before and after successive legislation actions and resultant bans of NPS, as reflected by specific NPS prevalence [23]. This generational turnover in market presence was more evident between 2009 and 2012. After 2012, some NPS have begun to maintain market presence or vanish and later reappear with widespread regional use after their ban.
Record of chemical name by year was once an effective way to track changes in cathinone and amphetamine derivative generations [23]. However, the quick pace at which chemicals structures are altered to create newer versions of drugs in order to circumvent drug laws eventually made it reasonable to change the system of classification of these derivatives.
Because of the rapid changes to this class of synthetic drug and because several drugs are no longer prevalent, today many researchers and law enforcement personnel refer to the chemical makeup rather than year to track changes in NSP. Although there is no standard international nomenclature among different agencies, cathinone derivatives have been categorized into four groups by chemical structure, with novel drugs being created by slightly altering each structure [163]:
Group 1: N-alkyl compounds or those with an alkyl or halogen substituent at any possible position of the aromatic ring. First synthetic cathinones, including ethcathinone, ephedrone, mephedrone, flephedrone, buphedrone, and pentedrone, are part of group 1.
Group 2: Methylenedioxy-substituted compounds with substituents at any given position of aromatic ring, such as methylone, pentylone, and butylone. In terms of their structure and pharmacologic effect, these compounds are quite similar to MDMA.
Group 3: Analogs of natural cathinone with an N-pyrrolidinyl substituent. Most frequently encountered in the designer drug market.
Group 4: Compounds with both methylenedioxyl and N-pyrrolidinyl substituents.
Through mid-2011: JWH-018, JWH-073, JWH-200, CP47,497
July 2011 to July 2012: AM-2201, JWH-019, JWH-081, JWH-122, JWH-203, JWH-210, JWH-250, RCS-8
August 2012 to early 2013: UR-144, XLR-11, AKB-48, STS-135, MAM-2201
2013: PB-22, 5-fluoro AKB-48, 5-fluoro-PB-22, BB-22
2013 to 2014: AB-PINACA, AB-FUBINACA, ADB-PINACA
2014 to early 2015: THJ-018, FUB-PB-22
2015: MAB-CHMINACA, ADB-CHMINACA
2016: 5F-ADB, 5FMDMB-PINACA, 5F-AMB, 5F-APINACA, 5F-AKB48, ADB-FUBINACA, MDMB-CHMICA, MMB-CHMINACA, MDMB-FUBINACA
2018 to 2019: 5FEDMB-PINACA, 5F-MDMB-PICA, FUB-AKB48, FUB-APINACA, AKB48, 5F-CUMYLPINACA, SGT-25), FUB-144
2020 to July 2021: NM2201 or CBL2201, 5F-ABPINACA, 4-CN-CUMYL-BUTINACA, 4-cyano-CUMYL-BUTINACA; 4-CN-CUMYL BINACA, CUMYL-4CN-BINACA, SGT-78, MMB-CHMICA, AMB-CHMICA, 5F-CUMYL-P7AICA
As noted, the NPS arena is characterized by an evolutionary "arms race" between manufacturers and regulators. The U.S. Drug Enforcement Administration (DEA) broadens prohibition of NPS agents and structures, with manufacturers introducing NPS that circumvent these legislative actions. The hazard from this process is that manufacturer efforts to circumvent new drug laws will lead to NPS entry with greater toxicity and morbidity risk, as already observed with fluorinated cannabimimetics and likely with synthetic cathinones and other NPS [25,28].
A predictable pattern, termed a drug epidemic cycle, has long been observed with some recreational drugs. The cycle begins when the drug first becomes used by a narrow population segment, followed by dramatic increases in its use, possibly fueled by accounts of highly desired effect, perceived safety, or legality. With widespread use come initial reports of addiction or adverse effects from its use, followed by medical and public health alarm, extensive and sometimes sensationalized media reporting, rushed legislation criminalizing its use or possession, and then declining prevalence of its use [17]. This pattern unfolded in the United Kingdom (UK) during the 2000s with the NPS mephedrone and MDPV, and in 2012 the United States followed trend with the enactment of the Synthetic Drug Abuse Prevention Act and subsequent decline in use [17,24].
Schedule I is the most restrictive category under the Controlled Substances Act (CSA) and is reserved for drugs with no recognized medical use and a high abuse liability (e.g., heroin, LSD). The DEA has placed numerous NPS into Schedule I [26]. This is an ongoing process, and the most recent list of temporary and permanent NPS placed in Schedule I is found on the DEA website at https://www.deadiversion.usdoj.gov/schedules.
Other attempts at regulating NPS are still being developed. The UK responded to emerging NPS by enacting the European Psychoactive Substances Act of 2016, making it illegal to produce or supply many drugs including NPS. Though more research is needed, one survey showed a modest put positive reduction in the online availability of MDMB-CHMICA (from 47 to 38 websites offering the substance) one month after implementation of the Act. Some websites removed information indicating they were based in the UK, three stated that they could no longer supply customers in the UK, and two websites specifically referred to the Act [162]. In the United States, House Bill 1732: Synthetic Drug Control Act of 2017 was introduced to amend the Controlled Substances Act to include several NPS as Schedule I drugs; the HB was not passed. In 2019, the Stop Importation and Manufacturing of Synthetic Analogues (SIMSA) Act was introduced, but no action was taken. As noted, in July 2021, HB 4459: SIMSA Act of 2021 was reintroduced as a result of increased drug overdoses in 2019 and 2020 [33,89]. In addition, many individual states have enacted legislation to regulate the distribution and use of NPS [54].
Although patterns of use are rapidly changing, the information in this section helps show the direction of movement in NPS use, distribution, and associated public health concerns. It is believed that the NPS climate in Europe reliably forecasts emerging domestic trends by roughly two years, as illustrated by 2014–2015 European Union data suggesting use patterns in the following few years in the United States [27]. It should be noted that 2014–2015 was the year that NPS began receiving more attention and drugs were rapidly produced; therefore, much information and studies regarding NPS occurred during these years. More current information is provided when available.
The DEA produces an annual Emerging Threat Report that compiles seizure and drug analysis information to provide a snapshot of new psychoactive substances in the United States [38]. Results from the Emerging Threat Report analyzed in 2020 produced roughly 5,550 records (Table 1) [38].
MOST COMMON NPS TESTED IN THE UNITED STATES, 2020
| Chemical Class | Psychoactive Substances |
|---|---|
| Substituted amphetamines | 2F-deschloroketamine, 2-methoxymethamphetamine and mitragynine |
| Cathinones | Eutylone,α-Pi HP |
| Benzodiazepines | Flualprazolam, etizolam |
| Tryptamines | 5-MeO-DBT, AcO-DMT |
| Fentanyl analogs | Fentanyl, 4-ANPP, Acetylfentanyl |
| Synthetic cannabanoids | 5F-MDMB-PICA, MDMB-4en-PINACA, 4F-MDMB-BUTINACA |
These results suggest a fair number of non-cannabimimetic/cathinone NPS in use, with the DEA's Emerging Trends Program reporting nearly 88% of NPS tested being comprised of opioids, most commonly fentanyl (90% of all opioids) compared with 5.3% of benzodiazepines, 3.6% of cathinones, and 2.4% cannabimimetics identified [38]. According to data from these sources, a high proportion (53%) of samples purchased as fentanyl contained only fentanyl and no other substance and 31% of fentanyl identifications contained fentanyl and heroin [38].
In 2020, the United States indicated a 30% increase in overall drug overdoses (including non-synthetic drugs), the largest increase in nearly three decades. The National Center for Health Statistics notes that the increase is likely higher; however, concrete data are not yet available. The catalyst behind the sharp increase is likely due to the coronavirus pandemic (COVID-19), with reasons of poor mental health due to stress and isolation, in combination with more lethal variations of synthetic drugs, such as fentanyl [34].
There is a rapidly changing landscape of synthetic drug us that is occurring with the ongoing COVID-19 pandemic. While there is lack of statistics thus far, it is postulated that there has been a lower rate of "social drugs" such as MDMA, and a higher rate of cannabinoid and dissociative drugs as individuals adjust to socially distanced environments and greater time in the home. The highest rate is consistent with the opioid epidemic that has become prevalent in the past several years. Early data from the 2021 European Drug Report indicate that individuals are consuming alcohol more regularly as a "socially acceptable" alternative to drugs. In addition, it was noted that there is likely a decline or cease of drug use in individuals that only occasionally used, while there is likely an increase in those that used them regularly prior to COVID-19 [11].
Rapidly spreading local/regional outbreaks of NPS use, toxicity/overdose requiring emergency medical services (EMS), and fatalities all increased through 2014 and 2015 (Table 2). Especially hard-hit were Broward County, Florida, with county hospitals averaging 20 emergency department admits per day for alpha-PVP overdose or excited delirium, and Washington, DC, where cannabimimetic toxicity led to 439 emergency department admits in one month. Many DC toxicities were excited delirium; two homicides were committed during cannabimimetic-induced excited delirium, with one victim stabbed 40 times on a subway [19,31].
OUTBREAKS OF NPS USE, MORBIDITY, AND MORTALITY
| Timeframe | Locality | Patient Admits | Deaths | Confirmed NPS | ||
|---|---|---|---|---|---|---|
| Cathinones | ||||||
| March to June 2015 | Broward County, Florida | 20 ED admits per day average | — | Alpha-PVP | ||
| Late 2014 to May 2015 | Unknown | 30 | Alpha-PVP, ethylone | |||
| Cannabimimetics | ||||||
| February to April 2018 | Chicago and surrounding area, Illinois, extending to eight other states | >150 ED admits in Chicago area; 38 in other states | 4 | Unknown, but cannabinoid users all tested positive for brodifacoum, a long-acting vitamin K antagonist used in rodenticides, suggesting contamination | ||
| October 2017 to January 2018 | Utah | 52 admits | — | 4-cyano CUMYL-BUTINACA (4-CCB) | ||
| March to May 2015 | Mississippi | >1,200 ED admits | 17 | MAB-CHMINACA | ||
| Alabama | >1,000 ED admits | 5 | Unknown | |||
| May to September 2015 | Austin, Texas | 873 ED admits | — | Unknown | ||
| May to June 2015 | Washington, DC | 439 ED admits | — | Unknown | ||
| 2 weeks in April 2015 | New York City | >160 hospital admits | — | Unknown | ||
| October 2014 | Baton Rouge and Lafayette, Louisiana | >150 hospital admits | — | MAB-CHMINACA, ADB-CHMINACAa | ||
| Late 2013 (one month) | Colorado | 221 ED admits | — | ADB-PINACA | ||
| ||||||
The brief lifecycle of many NPS, under-detection and under-reporting of NPS morbidity and mortality, and polysubstance presence in many suspected cases makes accurate epidemiologic capture of current NPS use difficult. Time delays in data reporting often render epidemiologic sources and peer-reviewed publications outdated at their publication. However, NPS use has appeared to decline since the 2011–2012 peak, with the only exception being a notable increase and subsequent decrease in cannabimimetics reported in 2015. Data collected since 2014 have illustrated growing frequency and size of local/regional outbreaks of severe toxicity and death from specific NPS, although it is unclear how recent events (e.g., ongoing opioid epidemic, COVID-19 pandemic) [11].
Reports to the network of 55 poison control centers in the United States provide valuable information on population-level trends in the abuse of specific and class-wide substances. According to the American Association of Poison Control Centers, use of synthetic cathinones resulting in toxic effects peaked in 2012 and cannabimimetics reached highest rates in 2015, although 2011 shows the highest rates combined for the two categories (Table 3) [36].
TOXIC EXPOSURES TO SYNTHETIC CATHINONES AND CANNABIMIMETICS REPORTED TO THE AMERICAN ASSOCIATION OF POISON CONTROL CENTERS
| Year | Exposure | ||
|---|---|---|---|
| Synthetic Cathinones | Cannabimimetics | Total | |
| 2010 | — | — | — |
| 2011 | 6,137 | 6,968 | 13,105 |
| 2012 | 2,691 | 5,230 | 7,921 |
| 2013 | 995 | 2,668 | 3,663 |
| 2014 | 582 | 3,682 | 4,264 |
| 2015 | 522 | 7,797 | 8,319 |
| 2016 | 107 | 2,706 | 2,813 |
| 2017 | 7 | 1,959 | 1,966 |
| 2018 | 290 | 1,993 | 2,283 |
| 2019 | 268 | 1,163 | 1,431 |
It should be noted, beginning in 2013, poison control call counts are lower than actual NPS toxicities, as emergency department staff has become increasingly adept in identifying and managing NPS toxicity [19].
Current NPS exposure report data are available at https://www.poison.org/poison-statistics-national.
From the peak of past-year use in 2011–2012, cannabimimetic use has declined among adolescents and young adults (Table 4). For example, among 12th graders, 11.3% used synthetic marijuana, decreasing to 3.3% in 2020 [36]. The same trends have followed among 10th and 8th grade students [39]. This decline likely reflects the greater numbers of identified and banned NPS and/or an increase in the perception of harm [39,47]. High school and college students and adults 19 to 30 years of age have indicated an increased perception of risk of trying synthetic marijuana once or twice, with an average of 29.5% in 2012 to 43.9% in 2020. In both years, the perceived risk was higher if using synthetic marijuana occasionally (versus once or twice), with 37.4% in 2012 and 52.4% in 2020 [39].
PAST-YEAR CANNABIMIMETIC USE: ADOLESCENTS AND YOUNG ADULTS
| Grade Level/Age | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | 2020 |
|---|---|---|---|---|---|---|---|---|---|---|
| 8th grade | — | 4.4% | 4.0% | 3.3% | 3.1% | 2.7% | 2.0% | 1.6% | 2.7% | 2.7% |
| 10th grade | — | 8.8% | 7.4% | 5.4% | 4.3% | 3.3% | 2.7% | 2.9% | 2.6% | 2.6% |
| 12th grade | 11.4% | 11.3% | 7.9% | 5.8% | 5.2% | 3.5% | 3.7% | 3.5% | 3.3% | 3.3% |
| College | 7.4% | 5.3% | 2.3% | 0.9% | 1.5% | 1.3% | 0.5% | 1.6% | 1.8% | 0.5% |
| 19 to 30 years | 7.4% | 5.3% | 2.3% | 1.3% | 1.5% | 1.0% | 0.9% | 1.3% | 1.1% | 1.2% |
Cathinone use has also declined since 2012, although not as dramatically as users of cannabimimetics, given the overall lower usage rate (>1% annually). Very high rates of perceived danger from even single-use synthetic cathinones may explain the lower rates, with rates of perceived risk of 45% to 49% in 2012, compared with 68% to 72% in 2017 [39]. As of 2019, questions regarding cathinones has been removed from the annual National Survey Results on Drug Use study to study other emerging drugs [36].
NPS users are defined as those who research, discuss, and share NPS information in Internet forums and websites and who purchase NPS online or offline. Those who discuss and obtain the substances online appear to be distinct from NPS users making retail or street purchases.
A study of cannabimimetic users found the majority used these substances to avoid drug-testing detection due to probation/parole, seeking employment, residing in a sober facility, or joining the military. Most report using cannabimimetics as a cannabis substitute during drug-testing periods and resuming cannabis when drug testing has ended. In one study, nearly all learned of cannabimimetics from someone using the substances to avoid drug-testing detection [40].
Military Personnel
The difficulty in detecting cannabimimetics and cathinones by urine drug screens has made their use attractive to active U.S. Armed Forces members. Beginning in early 2011, the extent these drugs were used became evident, with reports of numerous incidents involving the detection and subsequent discharge of large numbers of service members from individual military bases or deployments. Among these reports was an event in 2011 in which an Army combat medic with two deployments to Iraq asphyxiated his young son and then shot and killed his wife and himself during synthetic cathinone intoxication [1]. Increasingly, soldiers have begun requiring emergency department admission or police intervention for medical and behavioral toxicity from these agents. These cases raised sufficient alarm for the military to enact regulations banning the use, possession, or sales of cannabimimetics and cathinones in 2011 [41].
Persons on Probation/Parole
Hard data are difficult to find, but persons on parole and/or probation have been mentioned as among the most likely groups to use NPS for escaping detection by urine drug testing. Considering the number on probation/parole with untreated addiction and limited resources and the availability of a low-cost street purchase sufficient for intoxication, this may represent a sizeable number of NPS users [19,31].
Music and club subcultures and recreational drug preferences have evolved in tandem. Cocaine was favored in the 1970s and 1980s disco scene. Underground raves started appearing in the late 1980s and early 1990s, and MDMA (sold and referred to as Ecstasy) was the favored psychoactive at these events. MDMA remained favored by participants in the domestic rave, club, and warehouse party scenes during the 1990s to early 2000s, along with gamma-hydroxybutyrate (GHB) and ketamine. Other growing scenes were gay nightclubs and circuit parties, with methamphetamine the preferred circuit party drug [25]. Efforts to improve safety through harm-reduction approaches (e.g., testing pills, information dissemination) developed during this period.
In the 2000s, electronic dance music grew out of rave culture, with indoor club or warehouse productions and outdoor festivals. Outdoor electronic dance music events are often large, with tens of thousands of participants and corporate sponsorships. These events have been plagued by NPS-related emergency department admissions and fatalities among participants. Independent harm-reduction groups began offering free drug sample testing to inform participants about the true contents of what was sold to them as MDMA or LSD. However, event promoters and venue owners have banned drug testing groups from admission, concerned that allowing their entrance would appear to condone drug use. This stance is a consequence of the 2003 Reducing Americans' Vulnerability to Ecstasy (RAVE) Act, which holds promoters legally responsible for drug dealing at their events. Some law enforcement members began misinterpreting the harm-reduction services and conflating them with drug promotion [42]. Drug testing groups have begun to sneak equipment past security to provide services, but violent retaliation by drug dealers is an ongoing concern [25].
Polysubstance ingestion before, during, and after NPS use is common and can occur without intent by the frequent addition of multiple NPS and other psychoactives to NPS products. NPS users often co-ingest cocaine, amphetamines, MDMA, caffeine, hallucinogens, Mitragyna speciosa (kratom), and/or cathinones to enhance stimulant and entactogen effects; alcohol and beta-blockers to suppress tachycardia; zopiclone to produce visual hallucinations; pregabalin, omeprazole, and domperidone to counteract stomach pain; and cannabis and benzodiazepines to counteract anxiety [43]. Self-administration of the second-generation antipsychotic drug olanzapine has become widely endorsed on Internet forums as the "ideal" molecule to terminate NPS-related psychotic crises/"bad trips," typically at a dosage range of 5–50 mg/day [44].
A 2010 survey of mephedrone users in London found that use of this drug was intended to augment, but not replace, pre-established use patterns of cocaine, Ecstasy, and MDMA. This pattern increases the risks of drug interaction toxicities in users [45].
Importantly, data suggest polysubstance use may be more or less prevalent in users of specific NPS, rather than endemic. Several studies found significantly higher rates of mono-substance use in cannabimimetic-related emergency department admissions than in patients with synthetic cathinone-related admissions. This may importantly influence management of patients with acute NPS toxicity [40].
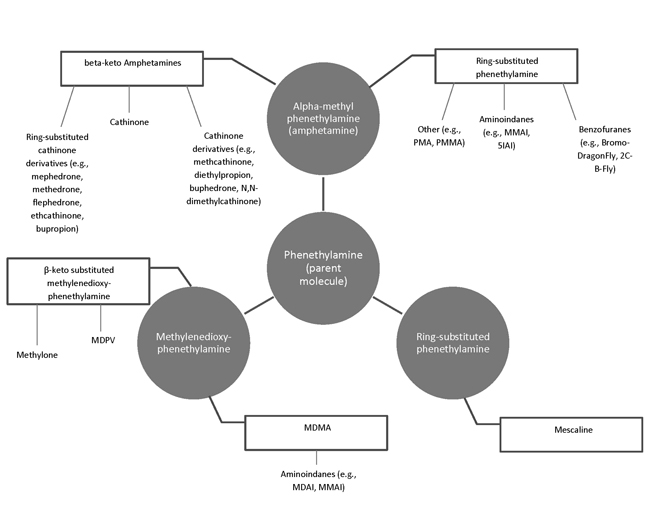
An astonishing diversity of structural families and subgroups of NPS and psychoactive drugs have been synthesized from the single parent molecule phenethylamine [46]. Phenethylamines are a broad molecular class that includes amphetamine, methamphetamine, MDMA, and their beta-keto analogs; mescaline; ring-substituted phenethylamines, such as the 2C series and their NBOMe analogs; benzodifurans; aminoindanes; and others (e.g., p-methoxymethamphetamine [PMMA]) [47]. For the purposes of this course, phenethylamines (plural) refers to phenethylamine derivatives as a class.
Phenethylamine, or phenylethylamine, is the parent molecule of many psychoactive substances, including synthetic cathinones, benzofurans and benzodifurans, the 2C and NBOMe series, aminoindanes, mescaline, and the classic recreational drugs amphetamine, methamphetamine, and MDMA (Figure 1). The structural similarity of phenethylamine to the neurotransmitter dopamine is readily apparent.
Phenethylamine contains a phenyl ring joined to an amino group via an ethyl sidechain. In substituted phenethylamines, the phenyl ring, sidechain, and/or amino group is modified by substituting another group for one of the hydrogen atoms [8,48]. Manipulation of the phenethylamine structure forms new compounds with stimulant, empathogenic, or hallucinogenic effects or their combination, influenced by the location and molecular make-up of the substitution.
Amphetamine is a substituted phenethylamine, formed by adding an alpha-methyl group to yield alpha-methyl-phenylethylamine. Amphetamine is modified to produce substituted amphetamines. Methylation of the terminal amine forms methamphetamine. A methylenedioxy substitution on the phenyl ring forms MDMA. Adding a ketone oxygen group at the beta position of the side-chain forms cathinone, termed beta-keto-amphetamine. Amphetamine, cathinone, and MDMA are likewise parent structures of numerous stimulant and empathogenic (MDMA-like) NPS; cathinone is the parent of most "bath salts" NPS [49].
All phenethylamines produce their stimulant, entactogenic, and/or hallucinogenic effects by increasing synaptic monoamine levels. Dopamine, serotonin (5-hydroxytryptamine or 5-HT), and norepinephrine are the monoamine neurotransmitters. Normally, dopamine, serotonin, or norepinephrine is released into the synaptic cleft, and then cleared from the synapse through uptake by their respective transporter. The last step involves vesicular monoamine transporter-2 (VMAT-2) located on the vesicular membrane. VMAT-2 uptakes the monoamines retrieved from the synapse and packages and stores them in synaptic vesicles for later release [48,71].
Phenethylamines increase synaptic monoamine levels by acting as inhibitors (blockers) or substrate releasers. Blockers inhibit monoamine transporter (re)uptake by competing with monoamine for binding sites on reuptake transporters to reduce synaptic clearance [72]. Releasers induce the release of newly synthesized monoamine pools and release monoamines from pre-synaptic vesicle stores. The drug molecule permeates the intracellular space to inhibit vesicular reuptake of monoamines within the cell, induce transporter-mediated sodium currents (i.e., depolarization), and initiate transporter-mediated monoamine efflux (i.e., reverse transport or release). Outflow of cytoplasmic monoamines into the synaptic cleft is increased [48,71,73].
The net result of increased synaptic monoamine concentration is greater activation of post-synaptic dopamine, norepinephrine, or serotonin receptors, which transmit the amplified electrochemical signaling downstream for relay through various pathways to produce clinical effects of the phenethylamine derivative. Phenethylamines differ by monoamines targeted, relative monoamine activating potencies, and mechanism of monoamine increase (i.e., blockers, releasers, or both). Differences in potency, duration of effect, desired and adverse effects, abuse potential, acute toxicity syndromes, and neurotoxicity potential result from these varied interactions with monoamine systems and from interaction with non-monoamine transmitter systems [71].
Substrate releaser-induced depolarization puts neurons at risk, as seen with methamphetamine-associated dopamine neuron dysfunction and serotonin neuronal depletion from the use of fenfluramines [71]. Releasers also disrupt vesicular storage to induce monoamine release, potentially contributing to persistent functional deficit in monoamine neurons through neurotransmitter depletion and loss of functional transporters. These potential neurotoxic mechanisms are not found in inhibitors [74,75].
Ring-substituted phenethylamines comprise many NPS groups with hallucinogenic properties. For example, addition of methoxy-groups at the 2 and 5 positions of phenethylamine, with any hydrophobic substitution at the 4 position, confers hallucinogenic activity and produces the 2C series. Adding a 2-methoxybenzyl (MeOB) unit onto the nitrogen molecule of 2C drugs confers substantially greater potency and forms the NBOMe series. The primarily stimulant-substituted phenethylamines—MDMA, mephedrone, and methcathinone—also co-activate psychedelic pathways through serotonin receptor activation [8,48].
Ring-substituted, or hallucinogenic, phenethylamines include the 2C series and their NBOMe analogs; the 2D series; benzofurans and benzodifurans; aminoindanes; and the para-(4)-phenyl-substituted amphetamines paramethoxyamphetamine (PMA) and paramethoxy-methamphetamine [8,47]. The phenethylamines are distinct from the indoleamines and piperazines [23,50].
The hallucinogenic properties of 2C drugs are further enhanced by a methyl-group at the alpha-carbon, forming the D-Series or ring-substituted (hallucinogenic) amphetamines produced decades ago such as 2,5-dimethoxy-4-methylamphetamine (DOM). All ring-substituted phenethylamines are potent serotonin (5-HT2A) receptor agonists, and many have strong activity in other receptor complexes [8].
There are 27 known 2C compounds, all originally produced by Alexander Shulgin. The powerful hallucinogen 2C-B was the first 2C synthesized, in 1974, by simple alterations to the natural phenylethylamine molecule mescaline [47]. The more commonly encountered 2Cs in the United States are 2C-B, 2C-I, and 2C-T-7, known by the street names Nexus, Bromo, Blue Mystic, and T7.
The effect following oral use in the lower dose range (<8 mg for 2C-B, 3–25 mg for 2C-I, and 10–50 mg for 2C-T-7) lasts six to eight hours and is often described as relaxation, awareness of integration between sensory perception and emotional state, and euphoria with increased body awareness and enhanced receptiveness of visual, auditory, olfactory, and tactile sensation. Dosing in the upper limits results in greater stimulant effects and a state of substantially greater intoxication. Even higher dosing produces LSD-like visual and auditory effects and potentially extremely fearful hallucinations and morbid delusions. User reports of 2C drug effects describe a blend of MDMA-like empathy and entactogenic effects with LSD-like psychedelic effects. 2C-B is used primarily as a club drug in the rave culture and circuit party scene, where some users ingest 2C-B in combination with LSD (a "banana split") or MDMA (a "party pack"). Several fatalities have been reported from co-ingestion of 2C-T-7 and MDMA [51,52,53].
Possible adverse effects include nausea, vomiting, agitation, tachycardia, hypertension, respiratory depression, seizures, psychosis, and suicidal thoughts. Excited delirium with agitation and violent behavior, hyperactivity, hyperthermia, and cardiopulmonary arrest have been documented following 2C use [23]. Several fatalities have resulted from co-ingesting 2C-T-7 and MDMA. Treatment of 2C toxicity is supportive, but immediate action is required with excited delirium, hyperthermia, and seizure activity, because presence of vomiting, agitated behavior, and seizures are risk factors for fatal 2C toxicity [18,55].
The NBOMe series was first developed in the early to mid-2000s for the purpose of researching mammalian serotonin receptor distribution. Initial Internet discussion and law enforcement attention both occurred in 2010 [56]. They are commonly known by the street names N-Bomb, Smiles, 25I, 25C, and 25B.
As noted, the NBOMes are synthesized from 2C phenethylamines by the addition of a 2-methoxybenzyl (MeOB) unit onto the nitrogen molecule. This molecular appendage confers greater potency than its 2C counterpart; for example, the dose of 2C-I is roughly 20 mg versus 50–100 mcg with 25I-NBOMe. The hallucinogenic effects are mediated by highly potent and selective agonist activity at 5-HT2A receptors [56].
The NBOMe series is sold as powder, liquid solution, or soaked into blotter paper. NBOMe appears in products sold as LSD, a widespread counterfeiting practice that is encouraged by the cheaper cost of NBOMe [57,58]. This poses a potentially serious health risk to the user, who instead of ingesting the physiologically benign LSD, unsuspectingly ingests NBOMe and risks potentially severe and fatal adverse effects [59].
The effects of NBOMe last 6 to 10 hours with sublingual ingestion. Users report desired effects of euphoria, mental/physical stimulation, feelings of love/empathy, altered consciousness, and unusual body sensations. Negative effects include confusion, shaking, nausea, insomnia, paranoia, and intense negative emotions. Users with severe NBOMe toxicity show violent, severely agitated, and hallucinating presentations and require hospitalization, as hyperthermia, tachycardia, hypertension, seizures, metabolic acidosis, elevated creatine kinase, and acute renal injury are usually present [56]. Even small amounts can cause seizures, cardiac and respiratory arrest, and death [57]. Many fatalities have occurred following NBOMe use, typically preceded by excited delirium [60,61].
Benzofurans include 1-(benzofuran-5-yl)-propan-2-amine (5-APB), 6-APB, and their dihydro-derivatives 5-APDB and 6-APDB. Benzofurans are analogs of MDMA and MDA, first synthesized in the 1990s at Purdue University for researching structure-activity relationships of MDMA-like molecules. In 2010, 5/6-APB entered the UK market as an MDMA replacement "legal high" under the brand name Benzofury (derived from benzofuran) and became very popular. Other benzofurans include IAP and 5-APDI, which replace both oxygen atoms of MDA with methylene groups; 5- and 6-API, which replace the oxygen atom in the heterocyclic rings of 5/6-APB with a nitrogen atom; and 5-MAPB, an N-methyl analogue of 5-APB [62].
Benzofurans are dopamine, norepinephrine, and serotonin inhibitors, with greatest potency at dopamine and norepinephrine receptors. As full 5-HT2B agonists, 5/6-APB may be cardiotoxic with long-term use. User reports describe an empathogenic and stimulant effect, with 5-APB more potent than 6-APB. Several fatalities have been attributed to benzofurans, with hyperpyrexia noted in several cases. Emergency department admissions for benzofuran toxicity have noted tachycardia, elevated blood pressure, and fever [62].
Benzodifurans are termed the "fly" drugs in reference to their insect-resembling molecular structure. They include tetrahydrobenzodifuranyl (Fly), 2C-B-Fly, 3C-B-Fly, and the most potent and widely used drug of this category, benzodifuranyl aminoalkane (Bromo-Dragonfly or B-Fly). The phenyl ring bound between two dihydrofuran rings in B-Fly produces much greater potency and duration of action than most phenethylamine derivatives. B-Fly mechanism of action is mediated primarily by agonist activity at 5-HT2A receptors and, to some degree, 5-HT1 and 5-HT2C receptors [63].
Recreational use of B-Fly was first noted in 2001 and became widespread in 2008, primarily through Internet mediation [63]. B-Fly is sold for oral use in blotter paper or liquid. Following a typical 200–800 mcg dose, the onset of effects can take six hours. Many users assume the initial dose ineffective and ingest another dose or other substances. The drug effect commonly lasts two to three days and is described as profound hallucinations (mainly visual, with geometric patterns and lights), sound alterations, a sense of connection/belonging with other realities, a sense of peace and well-being, emotional stimulation, and meeting with metaphysical entities. Commonly reported adverse effects include nausea and vomiting, headache, tachycardia, elevated blood pressure, lung collapse, gastrointestinal disturbances, muscle tension, tremor, anxiety, panic attacks, arrhythmias, heart murmurs, convulsions, flashbacks, memory disturbances, confusion, and paranoid ideation. Several fatalities have been reported in Europe, but attribution is unclear, as polysubstance use (particularly with ketamine) is common with B-Fly [63].
Aminoindanes were first synthesized in the 1970s and investigated for their significant bronchodilating and analgesic properties, though they were later found to produce psychoactive effects. Aminoindanes are amphetamine analogs, with their molecule characterized by a closed five-membered ring system next to the parent six-membered system. This configuration bestows minimal to no neurotoxicity (in preclinical studies) and higher serotonin than dopamine activation (which dampens drug craving). Together with Internet availability as "research chemicals," these actions form the basis of predictions that aminoindanes will become the next wave of NPS [64,65].
2-Aminoindane (2-AI) produces a stimulant effect similar to amphetamine but at one-sixth the potency. It also induces an analgesic effect that, in contrast to morphine, does not depress the brain respiratory center and is not counteracted by nalorphine. In contrast to amphetamines, 2-AI does not increase motor activity but does decrease food consumption. 5-Methoxy-6-methyl-2-aminoindane (MMAI) is a potent serotonin releaser but minimally inhibits dopamine uptake. By stimulating serotonergic neurotransmission, it can increase secretion of hormones such as adrenocorticotropic hormone. Compared with MDMA, 5-IAI is a greater serotonin and dopamine releaser and minimally inhibits their reuptake. Both are non-neurotoxic [66,67]. Some 1-AIs are promising candidates for psychosis treatment, and the substituted derivative rasagiline is used in the treatment for Parkinson disease [64,68]. The finding of potent 5-HT2B receptor full agonist activity with 5-IAI suggests cardiotoxic potential with long-term use, as this mechanism is shared by all drugs that induce heart valvular disease in humans, including fenfluramine, MDMA, and various ergolines [69].
Following oral ingestion of powder or crystals, aminoindanes produce empathogenic and entactogenic effects similar to other serotonin-releasing drugs (such as MDMA) and a mild stimulant effect similar to amphetamine [70].
The pipradrol derivatives diphenylprolinol (D2PM) and desoxypipradrol (2-DPMP) are selective and very potent monoamine transporter inhibitors without substrate-releasing properties. This pharmacologic profile closely resembles MDPV and alpha-PVP and predicts high risk of abuse potential and psychiatric morbidity. First appearing in 2010 as "Ivory Wave," clinical toxicity from 2-DPMP/D2PM is long-lasting (24 to 72 hours), with sympathomimetic symptoms of hypertension, agitation, and hallucinations [8].
In plural, cathinones and amphetamines refer to all synthetics/derivatives of the respective parent. Most stimulant NPS are cathinones, but NPS amphetamines have also begun to emerge as significant drugs of abuse.
More than 120 years ago, cathinone, the parent compound of this drug class, was isolated from Catha edulis (khat), a plant cultivated and chewed as a recreational and stimulant drug in Africa and the Arabian Peninsula for centuries [1]. Beginning with the synthesis of methcathinone in 1928 and mephedrone in 1929, many cathinone derivatives and analogs were synthesized and investigated or introduced into clinical use as anorectics, CNS stimulants, or antidepressants. Overall, problems with abuse and dependence have limited their clinical utility. Methcathinone was used in the former Soviet Union as an antidepressant in the 1930s and 1940s but was removed from clinical use due to problems with its abuse. It has been most widely used as a drug of abuse in countries formerly part of the Soviet Union [73]. Another derivative, pyrovalerone, is a stimulant first synthesized in 1964. It was investigated for use in treating chronic fatigue, lethargy, and obesity but was withdrawn due to abuse and dependency in users [73,77]. Methylone was created and patented by Jacob Peyton and Alexander Shulgin in 1996 as an antidepressant but never entered clinical use [78]. MDPV was developed by Boehringer Ingelheim in 1969 and subsequently prescribed for chronic fatigue and lethargy before its abuse liability became apparent [79].
As of 2021, only two cathinones are in clinical use in the United States. Diethylpropion is used as an anorectic but is infrequently prescribed due to abuse and dependence liability. It has also shown neurotoxicity in preclinical studies. The most successful cathinone derivative is bupropion, a ring-substituted cathinone widely used in the United States and Europe as an antidepressant and smoking-cessation aid under the brand names Wellbutrin and Zyban. This drug has no abuse liability [80].
The first documented large-scale abuse of synthetic cathinones occurred with methcathinone in the former Soviet Union in the 1970s and 1980s. Clandestine methcathinone manufacture first appeared in the United States in Michigan in 1991, followed by significant problems with abuse in the early 1990s [80]. In Europe, novel cathinone compounds emerged later in the 1990s, immediately followed by the rising prominence of "bath salts," which began appearing in the United States in 2009 [1].
Cathinone and its derivatives are closely related to phenethylamine, MDMA, and the classic stimulants amphetamine and methamphetamine in use in various settings since the 1930s. Cathinone, amphetamine, and MDMA are parent molecules of all known synthetic cathinones on the NPS market sold through the Internet, retailers, or street dealers [8].
As discussed, adding an alpha-methyl group to phenethylamine forms amphetamine. Methylation of the terminal amine then forms methamphetamine and greater CNS potency. Some cathinones are beta-ketone analogs of amphetamines. The parent cathinone is formed by adding a ketone oxygen group at the beta-carbon position on the amino side-chain of amphetamine, making cathinone its beta-keto analog (or bk-amphetamine). A ketone group added to methamphetamine forms methcathinone and the N-methyl derivative of cathinone [8].
MDMA is formed by a methylenedioxy substitution on the phenyl ring of amphetamine. Other cathinones are formed from MDMA and derivatives by adding a ketone group; thus, MDMA forms methylone or bk-MDMA; methylenedioxyethylamphetamine (MDEA or "Eve") forms ethylone or bk-MDEA; and N-methyl-1,3-benzodioxolylbutanamine (MBDB) forms butylone or bk-MBDB [46,81].
The molecular structure of cathinone is modified to form new cathinones through N-alkylation, which is achieved by substitutions in the phenyl (aromatic) ring or at the alpha-carbon position [17,82]. Cathinones without ring substitution produce mainly stimulant effects. Ring substitution with a secondary or cyclic amino group (usually alkyl, alkoxy, or methylenedioxy) confers varying degrees of entactogenic and other effects similar to MDMA. All cathinones, whether or not ring substituted, possess primary stimulant properties [8,82].
As with amphetamines and MDMA, the subjective and physiologic effects of cathinones result from increased synaptic concentrations of the monoamines dopamine, norepinephrine, and serotonin. In addition to those discussed for phenethylamines, cathinones inhibit monoamine oxidase (MAO), especially MAO-B, reducing the breakdown of dopamine and phenethylamine [48].
Several cathinones and amphetamine derivatives are now pharmacologically characterized in humans, allowing their grouping by mechanisms of action resembling classic stimulants, which can help in the understanding of their clinical effects [46,83].
Similar to cocaine, cocaine-MDMA-mixed cathinones show a ratio of dopamine versus serotonin inhibition ranging from 1 to 5 (dopamine>serotonin). With methylone, ethylone, and butylone, their corresponding non-beta-keto analog entactogens MDMA, MDEA ("Eve"), and MBDB are 10-fold more selective for serotonin compared with dopamine. These cathinones are more dopaminergic in monoamine transporter inhibition activity than their serotonergic entactogen analogs. Overall, the cocaine-MDMA-mixed cathinones are comparable to MDMA in monoamine-releasing activity, although the overall pharmacologic effects of mephedrone and methylone share the dopamine system-stimulating properties of amphetamine and methamphetamine [46,83].
Mephedrone is equally potent at dopamine and serotonin inhibition. It is a more potent releaser of dopamine than MDMA and produces a rapid and pronounced increase in nucleus accumbens dopamine levels, similar to amphetamine and unlike MDMA. However, mephedrone produces strong increases in extracellular serotonin similar to MDMA and unlike amphetamine.
Methylone is a slightly more potent dopamine inhibitor than a serotonin inhibitor. It has been found to elevate extracellular monoamine levels in the nucleus accumbens, similar to MDMA. Ethylone is an equipotent dopamine, serotonin, and norepinephrine inhibitor and releases serotonin. Butylone also releases serotonin, but it is a slightly more potent dopamine than serotonin inhibitor.
Naphyrone shows a monoamine uptake transporter inhibition profile similar to cocaine, with equal potency at all three transporters and no monoamine releaser activity. Naphyrone is structurally related to pyrovalerone and its derivative MDPV, but it is functionally distinct due to its greater absolute and relative serotonin-inhibiting potency [84].
This group of NPS includes mephedrone, 4-ethylmethcathinone (4-EMC), 4-FMC, 4-bromomethcathinone (4-BMC or brephedrone), 4-FA, and 4-fluoromethamphetamine (4-FMA). Substances in this group are more serotonergic (i.e., have a lower dopamine/serotonin ratio) than their amphetamine, methamphetamine, and methcathinone analogs [85].
The 4-methyl, 4-ethyl, and 4-bromo groups show enhanced serotonergic properties versus the 4-fluoro group. The para-substituted amphetamines release norepinephrine and dopamine; 4-FA, 4-FMA, 4-MEC, and 4-EMC also release serotonin (similar to MDMA). Most para-substituted amphetamines show 5-HT2A receptor affinity, without relevant 5-HT2B receptor activation. The enhanced direct and indirect serotonergic agonist properties of para-substituted amphetamines/cathinones are associated with greater MDMA-like effects [85].
Cathinone and methcathinone show pharmacologic profiles highly similar to their non-beta-keto analogs amphetamine and methamphetamine, including their relative monoamine transporter inhibition profiles with high inhibitory potencies at dopamine and low potencies at serotonin. They are potent releasers of dopamine but not of serotonin [46,83].
Flephedrone inhibits dopamine but not serotonin, similar to its analog 4-FA. It has a dopamine/serotonin selectivity profile equal to the methamphetamine-like cathinones, but with higher 5-HT2A receptor binding and agonism, similar to mephedrone and MDMA [46,83].
Pyrovalerone and its derivative MDPV are very potent dopamine inhibitors—at least 10-fold more potent than cocaine and methamphetamine. They are weak serotonin inhibitors and thus show dopamine/serotonin inhibition ratios greater than 100. MDPV and pyrovalerone are also highly potent norepinephrine inhibitors. Pyrovalerone and MDPV do not produce dopamine efflux, and the activity of pyrovalerone-derivative cathinones is purely transporter uptake inhibition [46,83,85].
PMA and PMMA are potent norepinephrine and serotonin transporter inhibitors and releasers and have been sold as MDMA. However, they are substantially more toxic. In 2014, PMA/PMMA sold as MDMA led to 29 deaths in the UK [8,14].
4-MTA, the methyl-thio analog of PMA, has dominant serotonergic action and a high risk of serotonin toxicity. Methedrone is the beta-keto analog of PMMA, and whether this cathinone carries the toxicity of its parent compound is not known [8].
Mephedrone can produce the sought-after entactogenic effects of MDMA, particularly the feeling of enhanced emotional and physical connection to others. Other desired effects include intense stimulation, alertness, euphoria, sociability and talkativeness, moderate sexual arousal, perceptual distortions, and intensification of sensory experiences. The numerous unwanted effects are common to all cathinones and result from hyper-dopaminergic, hyper-adrenergic, and hyper-serotonergic output [1]. The effects are often followed by intense compulsion to re-dose. Tolerance develops quickly, and brief drug effect and urge to re-dose can lead users to ingest successive doses, often in excess of 1 g [86,87,88].
Following single-dose mephedrone, brain dopamine peaks in 20 minutes and returns to baseline within two hours, 10 times faster than MDMA and two times faster than amphetamine [73]. Dopamine levels increase 496% following a single dose of mephedrone, compared with 412% with amphetamine and 235% with MDMA. Serotonin levels increase by 941% with mephedrone, 165% with amphetamine, and 911% with MDMA [1]. An intranasal dose of 25–75 mg or an oral dose of 150–250 mg can induce intense craving and compulsion to re-dose—stronger than that experienced with MDMA. Intranasal users rate mephedrone as more addictive than cocaine. Mephedrone alone is not neurotoxic to dopamine neuron terminals, but its co-administration with MDMA, amphetamine, and methamphetamine enhances neurotoxicity [88].
Relative to MDMA, 100–200 mg oral methylone produces calm euphoria, alertness, restlessness, a strong feeling of empathy, and milder stimulation. Unlike methamphetamine, methylone is a weak motor stimulant, and unlike MDMA, methylone induces minimal hyperthermia and little long-term cortical or striatal amines alteration. It has shown antidepressant effects and demonstrates little long-term cortical or striatal amine alteration. The side effect profile primarily reflects sympathomimetic activity. Fatalities attributed to methylone often involve polysubstance use [9,16,73].
Entering the domestic NPS market in late 2010, MDPV quickly rose in prominence and notoriety [77]. Its pharmacologic actions closely resemble pyrovalerone and alpha-PVP. Rapid blood-brain barrier penetration confers high potency. Full effects peak at 90 minutes and last three hours. Relative to cocaine, MDPV shows 50-fold greater dopamine potency and 10-fold greater norepinephrine potency, predictive of pronounced sympathomimetic stimulation and euphoria [48,74].
MDPV imposes risks from the slim dose-response margin between desired (2–10 mg oral) and adverse (>10 mg oral) effects. Effects include physical and mental stimulation, increased sociability, euphoria, and potentially severe prolonged panic attacks, agitation, anhedonia, confusion, intense paranoia, and depression. An unpleasant comedown, significant craving, compulsion to re-dose, and rapid tolerance are often reported [90]. Users have repeatedly re-dosed from intense craving and to counteract unpleasant comedown symptoms, increasing the risks of overdose and toxicity. More than other cathinones, MDPV is linked to excited delirium syndrome [16,91].
4-MEC is a methcathinone derivative that produces stimulant, euphoric, and empathogenic effects. 4-MEC users frequently report multiple re-dosing and difficulty refraining from re-dosing if more 4-MEC is available. Tolerance quickly develops [16].
As noted, mephedrone can be nasally ingested (snorted), but most cathinones are orally ingested. They cannot be smoked because their free bases are highly labile. Mephedrone, MDPV, 4-MEC, and pentedrone are water soluble, allowing injection. Mephedrone has been injected with heroin to simulate IV heroin/cocaine effects ("speedball") [48,80]. Other ingestion approaches are "bombing," with mephedrone powder wrapped in cigarette paper and swallowed, and "keying," an approach to get a crude dose estimate by dipping a car or house key into powder and then ingesting nasally. It is thought the powder from five to eight "keys" amounts to 1 gram [73].
The side effect profile of cathinones reflects relative contribution from dopamine, serotonin, and/or norepinephrine activation. Sympathomimetic effects common to all cathinones include tachycardia, tremor, sweating, hypertension, mydriasis, or hyperthermia. Excessive dopamine release can induce psychosis and confusion, while excessive serotonin release can induce myoclonus, nausea and vomiting, and agitation [6,80,92]. Additional possible side effects include seizures, bruxism, prolonged panic attacks, insomnia, headache, tinnitus, vertigo, muscle twitching, dizziness, altered vision, short-term memory problems, anhedonia, depression, and suicidal thoughts [42]. Cathinones closely resemble amphetamines in molecular structure, but differ by greater potential for severe and protracted adverse effects, potentially even from a single dose [92].
Excited delirium syndrome is a life-threatening and potentially fatal state of agitated delirium and autonomic dysregulation. It is the most severe manifestation of toxicity/overdose with cathinones use. Cannabimimetics and other NPS can also induce excited delirium, but cathinones-induced excited delirium is the most documented in the scientific literature and the lay media.
Cathinones-induced agitated delirium or psychosis may persist for weeks, even from a single dose. Close to 80% of patients presenting for emergency medical care following cathinone use exhibit agitation ranging from mild to severe psychosis requiring chemical and physical restraint [50,73]. With severe agitation, the patient may require restraint and transport to a medical setting by law enforcement personnel. Agitation can be exacerbated by concurrent use of alcohol or other drugs, such as cocaine. Dramatic cases of disorganized and agitated behavior manifesting in severe aggression, violence, homicidal combative behavior, self-mutilation, or suicide have received media coverage due to injury and loss of life. Delusions of persecution and auditory hallucinations during binge use have been described in users with a negative history of psychosis [93,94,95,96].
The bizarre, aberrant behavior during cathinone-induced psychosis encountered by poison control and emergency medical experts led to their description as embodying the combined worst attributes of methamphetamine, cocaine, phencyclidine, LSD, and MDMA [97]. In a case series, poison control experts in Kentucky and Louisiana described their encounters with individuals displaying "aggressive violent behavior, hallucinations, and paranoia in higher percentages than previously reported" following synthetic cathinone use [98]. Behavioral descriptions included those who were found "jumping out of a window to flee from non-existent pursuers; requiring electrical shock (Taser) and eight responders to initially subdue the patient; repeatedly firing guns out of the house windows at 'strangers' who were not there; walking into a river in January to look for a friend who was not there; leaving a 2-year-old daughter in the middle of a highway because she had demons; climbing into the attic of the home with a gun to kill demons that were hiding there; and breaking all the windows in a house and wandering barefoot through the broken glass" [98]. Also described was a patient fatality from a self-inflicted gunshot wound while delusional. Investigation into possible causality in each of these cases found that MDPV was present in every case and that MDPV was the sole cause of the behavioral toxicity [98].
MDPV has been the primary cathinone detected in patients hospitalized for synthetic cathinone toxicity and overdose in the United States and has become the cathinone most responsible for excited delirium [74,98]. MDPV cross-reacts with the phencyclidine (PCP) immunoassay used in hospitals, suggesting some cases of severe neuropsychiatric toxicity following MDPV use may have been falsely attributed to PCP [74]. In addition to paranoia, psychosis, and agitation associated with all cathinones, high-dose MDPV use can induce extreme anxiety and intense prolonged panic attacks, aggressive behavior, "superhuman" strength, combativeness, and potentially terrifying hallucinations [94].
The first case report of fatality following acute MDPV toxicity described a sequence beginning with arrival to the emergency department, where the patient went into cardiac arrest with pulseless electrical activity. Despite rapid aggressive intervention that restored spontaneous circulation, the patient subsequently developed coagulopathy, rhabdomyolysis, renal failure, hepatic failure, and anoxic brain injury and ultimately died [77].
Numerous cases of organ damage and other life-threatening sequelae have been documented following cathinone use, including acute tubular necrosis and renal failure resulting from severe renal tubular vasospasm and elevated creatine kinase [99]. Seizure activity or anion gap metabolic acidosis has resulted from excessive anaerobic metabolism induced by excessive systemic monoamine elevation. Several fatalities following mephedrone use were linked to severe hyponatremia and cerebral edema [73]. MDPV exposure in one patient led to fulminant hepatic failure and disseminated intravascular coagulation. Most fatalities following cathinone use have resulted from aggression/self-harm in the context of severe agitation and psychosis [77,100].
Cannabis refers to the natural cannabis plant, primarily Cannabis sativa or C. indica. Cannabinoids are any natural or synthetic compounds with pharmacologic activity resembling the primary psychoactive effects of cannabis plants (via delta-9-tetrahydrocannabinol or THC) through cannabinoid receptor (CB)-1 or CB2 activity. Cannabimimetics have been called "synthetic marijuana," which can be misleading because while these substances functionally resemble THC, they also produce a range of pharmacologic and clinical effects uncharacteristic of cannabis [7,18,48].
The psychoactive components of cannabimimetics are primarily manufactured in China. These bulk chemicals are shipped as powder or dissolved in acetone or other solvents to U.S. distributors, who spray or coat the compound onto dried herbs and package the product for retail sales as herbal incense or potpourri. Of the numerous brands cannabimimetics have sold under, "Spice" has the highest name recognition and has become synonymous with cannabimimetic products. Herbal products saturated with cannabimimetics were introduced in Europe in 2004 and the United States in 2008, marketed as legal-high alternatives to cannabis [6,7,101]. Spice products were smoked until the entrance of oral/e-liquid/injectable cannabimimetic formulations for use in e-cigarettes or "vaping." Identically labeled products vary by cannabimimetic dosage, composition, and concentration. Some contain multiple cannabimimetic agents and other substances identified in samples as psychoactive herbs and plants, benzodiazepines, tryptamines, phenethylamines, NBOMe compounds, cathinones, and opioids [26,102].
The actual herbal plant materials in cannabimimetic products are listed on the packaging, typically a combination of purportedly psychoactive plants such as Indian warrior (Pedicularis densiflora) and Lion's tail (Leonotis leonurus). Some of the plants may have been chosen because of their actual historical use as cannabis substitutes, but little is known of their pharmacology and toxicology and concern has been raised over potential heavy-metal residue content. When these products first appeared in Europe, it was thought the mixture of legal herbs produced the "high." However, laboratory analysis revealed cannabimimetics as the psychoactive constituent [41,86]. Identification of the true psychoactive drug was delayed by several plausible factors, including psychoactivity from the labeled botanical products, the complex evaluation methods necessary, the addition of large amounts of masking agents such as vitamin E (tocopherol) to conceal the active substance, and distribution through legal Internet or retail establishments instead of clandestine production and illegal distribution that would have led to law enforcement interception and analysis [86]. Consumer perception in the United States that herbal smoking blends were safe, legal cannabis alternatives with the "high" produced by the proprietary herbal combinations persisted as their use became widespread [6].
Cannabimimetics entering domestic NPS markets between 2009 and 2012 were "rediscovered" molecules originally developed for research or clinical use. Following the discovery of THC in the 1960s, researchers synthesized numerous cannabimimetics during concerted efforts to isolate the psychoactive effects from desired therapeutic properties by modifying the THC structure. Their synthesis was described in scientific publications and later replicated for NPS market entry. Earlier cannabimimetic molecules bear a prefix denoting their origin. The first THC analogs were synthesized at Hebrew University, and these molecules are designated HU- (e.g., HU-210). The best known, nabilone and dronabinol, received U.S. Food and Drug Administration (FDA) approval in 1985 for the treatment of chemotherapy-induced nausea and vomiting. In the 1970s, Pfizer developed the cyclohexylphenols (CP) series and their N-alkyl homologues [1,103]. John W. Huffman and his team at Clemson University synthesized more than 450 cannabinoids during the 1990s to study interactions between molecular structure, receptor activity, and physiologic response. Their structural groups are indoles, pyrroles, and indenes [104,105]. These substances bear the prefix JWH- (e.g., JWH-018).
Newer cannabimimetics fluorinate the aliphatic side chain of older indole-based substances to strongly increase potency; this may also enhance blood-brain barrier penetration [7,23]. For example, fluorinated JWH-018 forms AM-2201, and fluorinated UR-144 forms XLR-11. AB-FUBINACA, AB-CHMINACA, and similar substituted indazole compounds have been introduced using this method. Many indazole compounds are fluorinated, and all are very potent, with high CB1 binding affinity. Receptor binding affinity is one potency test, with a lower affinity constant value indicating increased potency (Table 5) [18,48].
COMPARISON OF THC AND CANNABIMIMETICS CB1 BINDING POTENCY
| Origin | Examples | Structure | Potency and Selectivity | CB1 Binding Affinity |
|---|---|---|---|---|
| Delta-9-THC | Cannabis | Dibenzopyran | CB1 partial agonist | 35–80 nM |
| Hebrew University | HU-210 | Dibenzopyran ring, THC analog | Full CB1/CB2 agonist | 0.06 nM |
| Pfizer | CP47,497 | Cyclohexylphenol | Potent selective CB1 agonist | 9.54 nM |
| John W. Huffman, Clemson University | JWH-018 | Naphthoylindole | Potent CB1 agonist | 9 nM |
| JWH-122 | Naphthoylindole | Potent CB1 agonist | 0.69 nM | |
| NPS | AM-2201 | Fluorinated JWH-018 analog | CB1 agonist | 1 nM |
THC and cannabimimetics bind and activate CB1 receptors to produce their euphoric effects. Compared to the partial CB1 agonist THC, full agonist cannabimimetics have greater potency, with toxicity and overdose potential uncharacteristic of cannabis [106]. As a partial agonist, THC is limited in the extent it activates CB1 and shows a direct dose-response effect until a plateau is reached, with further dose escalation failing to increase drug effect. This partial agonist property contributes to the infrequent toxicity from cannabis use and the perception of cannabis as a "safe" drug. In contrast, the full CB1 agonist cannabimimetics do not possess a dose-response plateau and further use increases overdose and toxicity risk [103].
Cannabimimetics produce a substantially greater drug effect than THC, with CB1 receptor binding affinities 5 to 10,000 times greater and significantly higher dose-response efficacy. CB1 agonists inhibit GABAergic neurons that project to the nucleus accumbens, which disinhibits nucleus accumbens dopaminergic neurons that activate the mesolimbic dopaminergic pathways and contribute to the rewarding properties and abuse potential of cannabinoids. Because cannabimimetics more powerfully activate CB1, they produce more intense euphoria and reward. This greater inhibition of GABA-mediated neurotransmission also disrupts the balance of GABA/glutamate release in neuronal projections from the prefrontal cortex, which over-activates dopaminergic systems in the prefrontal cortex and striatum, inducing paranoia, agitation, anxiety, psychoses, and convulsions [18,102].
Importantly, evidence and growing consensus indicates that absence of cannabidiol (CBD) in the presence of THC strongly contributes to more frequent, severe toxicity. Cannabidiol is a cannabinoid and natural constituent of cannabis with demonstrated anxiolytic, antipsychotic, and anticraving effects. The presence of cannabidiol in cannabis is thought to counter the psychotomimetic and anxiogenic properties of THC in a concentration-dependent manner. Cannabidiol is absent in cannabimimetics, which may increase the risks of acute psychosis [7,8,18,47,48,102].
Many cannabimimetics possess indole-derived structures similar to serotonin, which may facilitate 5-HT2A receptor dysfunction associated with hallucinations, psychosis, and serotonin syndrome [7,107]. Some cannabimimetics show additional activity as N-methyl-D-aspartate (NMDA) receptor antagonists and/or MAO inhibitors. This may increase the risk of serious drug interaction toxicity [102]. Cannabimimetic products are often contaminated with clenbuterol, a beta2-adrenergic receptor agonist that potentiates sympathomimetic effects and may result in hypertension, tachycardia, nausea/vomiting, chest pain, and myocardial infarction [106].
Natural cannabis and cannabimimetics overlap mechanistically through CB1 receptor binding and activation to produce the shared subjective effects of relaxation, euphoria, perceptual changes (e.g., altered sense of time, intensified sensory experiences), cognitive impairment (e.g., amnestic symptoms, slowed reaction time), and the physiologic effects of xerostomia, conjunctival injection, and tachycardia [50]. Acute changes in mood, anxiety, perception, thinking, memory, and attention are common to both. Agitation, aggression, paranoia, anxiety, and psychoses are common with cannabimimetic use and less common or rare with cannabis use. As discussed, the more frequent and severe psychosis, agitation, and sympathomimetic effects with cannabimimetic use reflect greater potency, full CB1 agonist action, and absence of CBD [102,108].
The quality and intensity of adverse effects also differ. Unlike cannabis, cannabimimetics can induce severe agitation, psychosis, and paranoid delusions; command hallucinations are more likely with prolonged, heavy use. The greatest safety concern is psychosis, which can occur in persons without previous history and persist five months or longer [109]. Young and first-time users may be particularly vulnerable to cannabimimetic-induced psychoses [110]. The severity of distress during panic attacks and other psychologic effects has driven some cannabimimetic users to suicide [50].
Cannabimimetic use has repeatedly led to excited delirium, and some users die before reaching an emergency department [32]. Others may seek emergent care for paranoia, hallucinations, or physical violence emergencies. Increased activity from severe agitation and struggle can lead to rhabdomyolysis and the risk of renal failure. Seizures can induce anoxia, hyperthermia, acidosis, and long-term end-organ damage; these are fatal in 2% of cases [32,106].
Tryptamines are monoamine alkaloids synthesized by decarboxylation of tryptophan and are quite varied. They include natural neurotransmitters (e.g., serotonin, melatonin); hallucinogens found in plants, fungi, and animals (dimethyltryptamine [DMT], 5-MeO-DMT, bufotenin); synthetic pharmaceutical products (e.g., sumatriptan and zolmitriptan to treat migraine); and various synthetic hallucinogenic compounds, such as alpha-methyltryptamine (AMT), diisopropyltryptamine (DiPT), 5-MeO-DiPT, 5-MeO-AMT, diethyltryptamine (DET), and 5-MeO-DET [47]. Use of tryptamines for psychoactive effect began in the late 1950s with psilocybin, the natural ingredient in certain mushroom species. Synthetic tryptamines appeared on the illicit drug market in the United States during the 1990s [8; 111]. The use of tryptamines as an NPS has declined in recent years, as indicated by the DEA's 2018 Emerging Threat Report and 2020 National Drug Threat Assessment, which classifies tryptamines under the category of "other" [38]. However, due to the rise-and-fall nature of NPS drugs over short periods of time, there is a potential for tryptamines to make a comeback.
Tryptamines have an indole ring structure (a fused pyrrole and benzene double-ring) joined to an amino group by a 2-carbon side chain. Psychoactive effects are closely related to their structural influence on receptor affinity. Tryptamines produce dominant hallucinogenic/psychedelic effects as 5-HT2A/1A/2C receptor agonists. Alpha methylation leads to stimulant activity, as with AMT and 5-MeO-AMT. Many synthetic tryptamines are monoamine releasers, increasing the risks of serotonin syndrome and sympathomimetic toxicity. With primarily serotonergic action, tryptamines lack reinforcement and abuse liability [8,112]. Tryptamines are grouped by structure as indole ring-unsubstituted tryptamines, 4-position ring-substituted tryptamines (e.g., psilocybin), 5-position ring-substituted tryptamines, and ergolines (or complex tryptamines) (e.g., LSD, lysergic acid amide). Of these groups, the indole ring-unsubstituted and the 5-position ring-substituted tryptamines are considered NPS.
Indole ring-unsubstituted tryptamines include AMT (banned in 2004), alpha-ethyltryptamine (AET), DMT, DET, dipropyltryptamine (DPT), and DiPT. AMT and AET were developed as antidepressants in the 1960s by Upjohn but were withdrawn from brief clinical use due to the risk for psychoses and other adverse effects. With a 15–40 mg oral dose of AMT, effects have onset in three to four hours. Visual hallucinations, altered sensory perception, and euphoria persist for 12 to 24 hours. Frequently reported adverse effects include anxiety, nausea, moderately severe dysphoria, and next-day depression. AET produces psychedelic, stimulant, and entactogenic effects but may induce serotonin neurotoxicity [112].
DPT was synthesized in the 1950s and was first used in 1973 as an adjunct to psychotherapy in the treatment of alcoholism. An oral dose of 100–250 mg induces psychedelic effects, with increased music and color intensity, flashes of light and sparkles, ego loss, and seeing apparitions of faces. These effects last two to four hours [112].
All 5-position ring-substituted tryptamines inhibit monoamine reuptake but have few monoamine releasing effects. 5-MeO-AMT is a psychedelic tryptamine with structural similarity to amphetamines. Oral use of 2.5–4.5 mg produces effects lasting 12 to 18 hours. Excessive dosing can induce sympathomimetic effects and has led to several hospitalizations and fatalities.
5-MeO-DiPT, termed Foxy or Foxy Methoxy, was first synthesized by Andrew Shulgin and emerged as a drug of abuse in 1999. The effects resemble 2C-B, with a psychoactive threshold of 4 mg. Doses of 6–20 mg produce full-blown effects that peak at 60 to 90 minutes and last three to six hours. The initial nausea and muscular hyper-reflexia are followed by euphoria, relaxation with emotional enhancement, talkativeness, and behavioral disinhibition. Higher doses can produce abstract closed-eye imagery [113]. Adverse effects include restlessness, agitation, gastrointestinal distress, muscle tension, and rhabdomyolysis. Fatalities have been associated with 5-MeO-DiPT [47].
5-MeO-MiPT or "Moxy" is an analog of 5-MeO-DiPT. Following an oral dose of 4–6 mg, this drug produces euphoria, increased tactile sensations, relaxation, and visual distortions that dissipate by 10 hours, followed by difficulty sleeping.
Phencyclidine or PCP was discovered in 1956 by Parke-Davis. Initially showing great promise as a potent anesthetic, evidence of the alarming adverse effects delirium, hallucinations, and violent behavior led to PCP being declared "clinically unacceptable," halting clinical trials in 1965. However, recreational use of PCP was widespread in the late 1970s. Efforts to isolate useful from undesirable properties produced more than 300 PCP analogs, including ketamine. Aside from PCP and ketamine, PCP-like pharmacology was found in 22 phenylcyclohexylamine (PCA) and PCP analogs, with eight later appearing as abused drugs [114].
PCP and ketamine are arylcyclohexylamines with an aryl group attached to a cyclohexane ring and a basic amine function. The first arylcyclohexylamine NPS sold online was the low-potency PCP analogue methoxydine (4-MeO-PCP) in 2008 [48]. The ketamine analog methoxetamine (MXE) or 2-(3-methoxyphenyl)-2-(ethylamino)-cyclohexanone was developed as an alternative free of urinary tract morbidity. After its 2010 Internet entrance, it became the most popular dissociative NPS. Compared with ketamine, the 3-methox substituent provides higher serotonin transporter affinity and euphoria and greater duration/potency from the N-ethyl group [48].
MXE and ketamine both produce dissociative anesthetic effects and act as NMDA receptor antagonists and dopamine reuptake inhibitors. MXE is also an agonist at dopamine D2, 5-HT2, muscarinic cholinergic, sigma-1, and opioid mu and kappa receptors. Ketamine has shown efficacy in alleviating severe, treatment-resistant depression, and the mechanistic profile of MXE suggests comparable clinical use [115,116]. MXE is ingested through numerous routes, and a 15–40 mg oral dose can produce euphoria, a sense of calm and serenity, and distortion or loss of sensory perception. Adverse effects include severe dissociation, depersonalization, anxiety, paranoia, loss of consciousness, and nausea and vomiting [117]. MXE users report compulsive re-dosing and ingesting more than intended [18].
2-Methoxyphenidine (2-MXP or MXP) is an NPS dissociative and structural analog of diphenidine, introduced to meet growing demand for alternatives to the arylcyclohexylamines and to replace banned MXE. Aside from anecdotal reports suggesting greater potency than MXE, with dissociation, visual effects, and seizures at higher doses, little is known of this drug. Use of 2-MXP has led to three confirmed fatalities [118].
Analogs of fentanyl and meperidine, members of the piperidine class of opioids, comprise most opioid NPS. Fentanyl analogs first appeared in California in the late 1970s and early 1980s and were dubbed "designer drugs," the origin of this term. MPPP, a reverse ester of meperidine, emerged during this period but contained MPTP, an impurity converted in the body to the neurotoxin MPP+. Most who used the distributed MPPP developed an irreversible parkinsonian-like syndrome [114].
Fentanyl is used in surgical anesthesia and chronic pain analgesia. With potency roughly 100 times greater than morphine and 30 to 50 times greater than heroin, as little as 0.25 mg can be fatal. Fentanyl and its analogs are often laced in heroin, making their resurgence deadly; fentanyl distribution in Detroit and Cleveland between 2005 and 2007 contributed to more than 1,000 deaths [119]. Acetyl fentanyl, with one-third the potency of fentanyl, has appeared sporadically in the United States during 2014 and 2015 and resulted in at least 60 fatalities, a probable underestimate, suggesting, and correctly predicting, a fentanyl analog resurgence that began during the opioid crisis [38,119]. The DEA identified 15 novel fentanyl analogs during 2013–2014; in 2017, they identified 2,825 new fentanyl analogs [12]. A rapid rise in fentanyl use occurred between 2015 to 2017, and fentanyl and fentanyl analogs now account for the majority of tested and seized NPS, with the 2017 Emerging Threat Report showing a 116% increase in identification from 2016 alone [35,38]. Of the almost 3,000 identified substances, fentanyl accounted for 66% of identifications, followed by furanylfentanyl (10%) and U-47700 (7%) [38]. As of the 2020 report, fentanyl accounted for 89% of the identifications, followed by 4-ANPP at 5% [38].
AH-7921 is an atypical opioid synthesized in the 1970s to structurally and pharmacologically resemble fentanyl and phencyclidine. Its addiction potential and online availability have generated concern [48]. Shortly after initial detection in Europe, AH-7921 and MT-45, another novel opioid, contributed to more than 40 deaths [22].
Catha edulis is a flowering shrub native to East Africa and the Arabian Peninsula. Its leaves are chewed for psychoactive effect and are referred to as khat (or alternatively, qat, kat, Chat, Miraa, or Quaadka). Khat has been widely used since the thirteenth century as a recreational drug in Africa and the Middle East [120]. The acute effects of khat include euphoria, increased alertness and energy, hyperactivity, anorexia, and decreased fatigue; many users report feeling relaxed and talkative. The sympathomimetic effects mimic those of amphetamines. Following the 90- to 180-minute effect, users report diminished concentration, numbness, and insomnia [120]. Widespread khat use in the United States is unlikely [43].
Salvia divinorum is a member of the mint family native to Oaxaca, Mexico, and has been used by Mazatec shamans for divination and spiritual healing for more than 500 years [121]. It is used in the United States for its intense hallucinogenic effects, sometimes under the street names Sally-D, Diviner's Sage, Magic Mint, and Mystic Sage [122]. Salvinorin A, the primary psychoactive constituent, is a potent and selective kappa opioid receptor agonist that, unlike LSD, psilocybin, and DMT, lacks serotonin receptor activity [122]. Salvinorin A is the most highly potent known hallucinogen found in nature.
Salvia is usually taken by smoking the dried leaves, which produces a rapid onset with peak effect within two minutes and dissipation by 20 to 30 minutes. User reports describe intense, highly unusual experiences of changes in spatial orientation, sensations of energy or pressure on different areas of the body, revisiting childhood memories, cartoon-like imagery, and contact with entities. Other descriptions include dysphoria, uncontrolled laughter, a sense of bodily loss, overlapping realities, hallucinations, bright lights, vivid colors and shapes, and body or object distortions [121,122]. Adverse effects can include incoordination, dizziness, and slurred speech. No clinically meaningful changes occur in cardiovascular parameters [50,121,123]. Salvia divinorum and salvinorin A are not currently DEA scheduled, but several states have enacted regulatory controls for either or both agents [122].
Kratom (Mitragyna speciosa korth) is a tree indigenous to Southeast Asia, used by natives for its therapeutic and recreational effects (as an opium substitute) and to manage opioid withdrawal symptoms. In the United States, kratom has been promoted as a legal psychoactive product [124]. However, in 2016, the DEA announced it would be placing the active compounds in kratom into Schedule I [159].
Mitragynine is the primary active alkaloid of kratom. Kratom leaves are ingested by chewing or boiling into tea. The effects last two to five hours. Low doses produce increased alertness, physical energy, talkativeness, and sociable behavior. High doses produce an opioid-like effect with sedation and euphoria. Undesired effects include nausea, itching, sweating, dry mouth, constipation, increased urination, and loss of appetite [124].
Addiction to kratom has been documented and is associated with anorexia, weight loss, insomnia, skin darkening, dry mouth, frequent urination, and constipation. Isolated cases of psychosis have occurred from chronic use. A withdrawal syndrome is also characterized, with hostility, aggression, emotional lability, muscle and bone ache, and jerky movement of the limbs.
Patients presenting for medical attention following NPS use may exhibit intact or altered mental status. Mentally lucid patients may be intensely distressed with anxiety or panic, highly concerned with physical symptoms, or both. Symptoms are typically isolated and not systemic. If possible, information from patient history-taking and interview, together with patient signs and symptoms, directs management. However, patient presentations with altered mental status are not amenable to history-taking or interview, in which case management is directed by identifying the specific toxicity syndrome. Most toxicity/overdose symptoms are expressed through common pathways that allow markedly similar interventions despite pharmacologic diversity of causal NPS agent(s). This is fortunate, as toxicology confirmation of ingested NPS is rarely possible [7].
An attempt should be made to obtain information from all patients, with added information from lucid, coherent patients. The initial approach to assessing NPS intoxication and toxicity is evaluation of presenting signs and symptoms [61]. With cathinone use, this may include mydriasis, excited delirium syndrome, and sympathomimetic toxidromes. Cannabimimetic intoxication may present with conjunctival injection, signs/symptoms of cannabis intoxication with THC-negative urine drug screen, and sudden-onset psychosis not otherwise explained. Being subject to urine drug testing (e.g., active military duty, probation/parole) should be considered a risk factor for cannabimimetic use. A standard toxicology screening of illicit drugs should be obtained to anticipate drug interaction toxicities or the need for closer/prolonged monitoring.
Clinicians should have a working knowledge of NPS and other substances common to their region to facilitate recognition of toxicities. Knowledge of NPS street names can improve patient communication/rapport. Patients should be directly asked about recent NPS use, especially younger patients with signs/symptoms of possible substance-related toxicity. Inconsistencies between observed and expected presentations from self-reported or screen-detected drug class may indicate NPS use. If the patient and/or friend or family member has additional unused NPS and/or the package, the brand and possible NPS should be identified. Any unused NPS may be sent for laboratory analysis.
If severe muscle spasms, swelling and pain in the extremities, or seizures are present, a laboratory workup should be obtained, including complete blood count, metabolic panel, cardiac enzymes, and creatine kinase for suspected rhabdomyolysis. Very high lactic acid concentration, very low pH, and high creatinine/creatine kinase suggests rhabdomyolysis, metabolic acidosis, and potential renal failure.
The constellation of signs and symptoms in severe NPS toxicities reflects dysregulation of autonomic, sympathetic, dopaminergic, and/or serotonergic systems. These are termed syndromes or toxidromes.
As discussed, excited delirium syndrome, the most serious NPS-induced toxicity, is a severe, life-threatening state of agitated delirium and autonomic dysregulation. This syndrome is characterized by sympathetic hyperarousal (e.g., hyperthermia, vital sign abnormalities, metabolic acidosis), delirium (altered consciousness with diminished awareness of one's environment), rhabdomyolysis, and agitated or violent behavior. Patients with excited delirium are incoherent and combative; emergency department arrival is often by EMS transport or police escort in physical restraints. Many sustain traumatic injuries before first responder contact and intensely struggle even when struggle is futile, resulting in self-harm. Some patients may strip naked, reflecting the combined hyperthermia and altered mental status [125,126].
Stimulant toxicity resulting in excited delirium syndrome has been described with MDMA, cocaine, amphetamine, and more recently, NPS such as cathinones and cannabimimetics. The hyper-dopaminergic state associated with intoxication with these drugs overloads dopamine circuitry with electrochemical signaling, triggering a surge in extreme motor hyperactivity, delirium, agitation, and violent behavior. Action pathways lead to peripheral sympathomimetic stimulation that predisposes to cardiac arrhythmia and cardiomyopathy, and with sufficient activation of the neurocardiac axis, sudden death [127,128]. Autopsy results have shown a diminished concentration of D3 dopamine receptors relative to controls, suggesting a deficit in normal compensatory measures in response to rapid changes in dopamine levels [129,130].
Hyperthermia contributes to excited delirium-associated morbidity and mortality and primarily results from agitation that drives muscular hyperactivity, rhabdomyolysis, and renal failure. Even with patient survival of an initial cardiac arrest, persistent hyperthermia contributes to the developing coagulopathy, rhabdomyolysis, and multisystem organ failure [77,131].
Effective Calming of Patients with Excited Delirium Syndrome
The ability of EMS or emergency department staff to safely subdue patients with excited delirium has been elusive. Delays in medical treatment and the use of conventional restraints can be fatal. The behavioral symptoms of excited delirium impose a serious safety hazard to EMS, emergency department staff, and the patient [19]. TASER and physical restraints are standard control measures but produce further destruction of muscle tissue, exacerbating the risks of subsequent renal failure and cardiopulmonary collapse [127]. Benzodiazepines and haloperidol are used by some EMS to calm patients with excited delirium before attempting emergency transport. In this setting, IV administration is usually impossible, intramuscular administration delays the onset, and the dose required to sedate violent patients risks adverse hemodynamic and respiratory complications. Antipsychotic drugs interfere with already-compromised dopamine function [132].
Intramuscular ketamine has rapid onset and efficacy, a wide therapeutic window, and favorable side effect profile. It is becoming favored by EMS for calming patients with excited delirium before emergency transport with support from several studies [132,133]. However, some patients develop laryngospasm and hypoxia, resolved by endotracheal intubation. In one study of 52 patients receiving ketamine 4 mg/kg IM, effective sedation and medical control was achieved within 150 seconds in 96% of cases; all remained sedated following emergency department arrival (mean: 19 minutes) [132]. In another study of 35 agitated, combative patients with possible excited delirium, 91% were successfully sedated by ketamine IM (mean dose: 324 mg), 17% required additional post-ketamine sedation by EMS or emergency department staff, and 23% required post-ketamine intubation [133]. Emergence reactions, well described with ketamine, also developed but were resolved with benzodiazepines [134,135]. Rapid calming from ketamine reduces extreme physiologic stress from extended struggles with police and continued agitation with physical restraints. Excited delirium syndrome requires IV initiation to begin end-organ, life-preserving treatment, which is nearly impossible until severely agitated, combative patients are sedated [132,133,134].
Sympathomimetic toxidrome resembles excited delirium, differing by dominant hyperadrenergic symptoms of tachycardia, hypertension, nausea/vomiting, and diaphoresis and a lack of violent agitation. Excited delirium syndrome and sympathomimetic toxidrome can co-occur. The presumed underlying hyperdopaminergic and hyperadrenergic states of excited delirium and sympathomimetic toxidrome, respectively, are intertwined. As such, co-occurrence in NPS toxicity is probably frequent, and management is highly similar [18].
Serotonin syndrome is a state of excess serotonin activity from serotonergic agent overdose or synergistic toxicity. Serotonin syndrome shares some features with excited delirium and sympathomimetic toxidrome, but patients are rarely aggressive and violent. Patients typically present with psychomotor agitation, and cognitive (e.g., confusion, delirium), neuromuscular (e.g., akathisia, ataxia, myoclonus, hyper-reflexia), and autonomic (e.g., dizziness, nausea/vomiting, tachycardia, sweating) symptoms. It can be differentiated from sympathomimetic toxidrome by the presence of shivering, rigidity, myoclonus, and hyper-reflexia. Serotonin syndrome is characterized by a rapid onset of neuromuscular symptoms with markedly increased muscle tone, along with shivering, tremors, hyper-reflexia, akathisia, ataxia, and myoclonus. Sweating may decrease and contraction of opposing muscle groups generates heat more rapidly than vasodilatation, leading to hyperpyrexia and cardiovascular instability. The mortality rate is 10% to 15% [48,136].
Acute Hyponatremia
Acute hyponatremia has led to numerous MDMA fatalities. These deaths usually result from prolonged (8 to 12 hours) dancing to electronic dance music (e.g., techno, house). Indoor settings with poor ventilation and high ambient temperature contribute further. Hyperthermic complications from MDMA stem from exertional hyperpyrexia, hyponatremia, and serotonin syndrome [136].
Rapid identification of NPS-induced toxicity is essential in patients who present with agitation, altered mental status, hyperthermia, and autonomic dysregulation. Conditions that resemble NPS toxicity should be ruled out first (Table 6) [93]. This narrows the field to identify the NPS toxicity syndrome or toxidrome.
POSSIBLE CONDITIONS ACCOUNTING FOR AGITATION, FEVER, ALTERED MENTAL STATUS, AND HYPERDYNAMIC VITAL SIGNS
| Medical | Substance-Induced | Toxidromes | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
| ||||||||||||||||
| GABA = gamma-aminobutyric acid. | ||||||||||||||||||
A GABA agonist withdrawal syndrome from substances such as alcohol or benzodiazepines is a common medical condition that shares autonomic hyperarousal, agitation, and altered mental status with NPS toxicity [93,137,138]. Neurologic trauma or disease, including traumatic brain injury, hydrocephalus, brain tumor, and subarachnoid or intracerebral hemorrhage, can produce an intense autonomic dysregulation syndrome similar to that seen with NPS use. These patients may also display hypertension, fever, tachycardia, tachypnea, and pupillary dilation [139,140,141].
Some psychiatric disorders may have similar presentations to acute NPS toxicity, including bipolar disorder and paranoid schizophrenia. Patients may display an emotional rage reaction in response to acute psychologic stressors. In addition, psychotropic drug withdrawal and emergent symptoms from medication noncompliance may precipitate symptoms similar to an excited delirium or serotonin syndrome.
Systemic inflammatory response syndrome (SIRS) is related to systemic inflammation, organ dysfunction, or organ failure and is broadly classified as infectious or noninfectious. With infection, the condition is termed sepsis. Noninfectious SIRS origins include trauma, burns, pancreatitis, ischemia, and hemorrhage, and dysregulated and uninhibited pro-inflammatory pathways result in altered mental status, fever, or hyperdynamic vital signs [93,142].
Encephalitis of viral, bacterial, fungal, or autoimmune origin can manifest in neuropsychiatric disturbances and altered mental status with severe headache, fever, confusion, agitation, personality changes, seizures, hallucinations, or impairment in speech or hearing. Limbic encephalitis of paraneoplastic origin can produce severe neuropsychiatric symptoms, marked agitation, and autonomic dysfunction [93,143].
Malignant catatonia is a neuropsychiatric syndrome seldom seen clinically, is highly lethal, and initially presents as nonspecific insomnia and mood changes, progressing to severe anxiety, delusions, hallucinations, and agitation. Other symptoms can include severe, nonpurposeful hyperkinetic movements, high fever, tachycardia, and labile blood pressure [93,144].
Endocrine system disorders can appear as agitation, autonomic instability, and fever. In thyrotoxic crisis, cardiac failure, arrhythmia, or hyperthermia can result from a massive surge in thyroid hormone. Tumors of the sympathetic ganglia can produce hypertension, tachycardia, sweating, and panic attacks from increased sympathetic tone. Less commonly, fever and delirious agitation may be noted [93]. In patients with diabetes, hypoglycemia may precipitate violent outbursts and an appearance of intoxication. Hypoglycemia may be diagnosed rapidly and conclusively via blood glucose testing and glucose response.
Anticholinergic toxidromes can resemble NPS toxicity, with altered consciousness, agitation, confusion, disorientation, delirium, hallucinations, tachycardia, tachypnea, and hyperthermia [145]. Sympathomimetic toxidrome may be differentiated from anticholinergic toxidromes by presence of marked diaphoresis (instead of dry skin) and lack of bowel sounds [145]. The presence of neuromuscular abnormalities is specific to serotonin syndrome and is not seen in patients with anticholinergic toxidromes.
Most nonpsychiatric symptoms of NPS toxicity appear self-limited and resolve within one to several days with supportive treatment. Panic attacks, intense anxiety, agitation, or paranoia can be treated with benzodiazepines. Antipsychotics are second-line agents for more severe agitation or paranoia because they increase the risk of seizure if cathinones or phenethylamines were taken [61].
The similar core features of NPS toxicities allow symptom-directed management independent of (presumed) causal substance. Management of common core features and those specific to excited delirium, sympathomimetic toxidrome, and serotonin syndrome is discussed in this section.
If treatment of excited delirium or sympathomimetic toxidrome is neglected, delayed, or inadequate, the outcome is often multiple end-organ damage or death [94]. The most essential aspect of the management of cathinone toxicity is rapid, aggressive sedation with benzodiazepines. Benzodiazepines are the agents of choice because they decrease excessive heart rate, blood pressure, neural stimulation, and muscular activity; prevent seizures; protect against physical violence; and reduce muscular hyperactivity that drives fever, rhabdomyolysis, and renal failure. Benzodiazepines have a wide safety margin and, contrary to common belief, do not dangerously decrease cardiovascular or respiratory parameters unless used with potent sedatives. Immediate calming may require IM lorazepam, midazolam, or ketamine to allow for safe placement of IV access. With access in place, IV diazepam may be initiated, the preferred agent for effective rapid titration because full onset of each dose occurs within five minutes, allowing repeat dosing without the "overshooting" risk with slower-onset lorazepam. Patients may require very high doses for effective sedation. Propofol or barbiturates in those appearing refractory to high-dose benzodiazepine [18,93,94,146,147,148]. Antipsychotic drugs interfere with already-compromised systemic dopaminergic function and should be avoided in patients with suspected excited delirium [127].
Management of serotonin syndrome targets agitation, hyperthermia, and autonomic dysfunction. Benzodiazepines are preferred to induce sedation and reduce muscle rigidity. With causal substance(s) typically unidentified and benzodiazepine efficacy across NPS toxicity syndromes, benzodiazepines should be used instead of serotonin antagonists [149].
All toxicities with hyperpyrexia require aggressive cooling through high-rate IV fluids and external cooling measures. The combination of sedation, fluids, and cooling reverses hyperthermia and metabolic acidosis and prevents further muscular and hepatorenal injury. Enteral or parenteral vasodilators should be used for persistent hypertension, while beta-blockers should be avoided because unopposed alpha-receptor stimulation can induce systemic vasoconstriction. Sodium bicarbonate may be considered for rhabdomyolysis and acidosis [106]. Antipyretics are ineffective for hyperthermia because the origin is increased muscular activity, not hypothalamic temperature dysregulation [149].
Following resolution of the autonomic storm and return to normal reflexes and muscle tone, clinicians should be aware that psychosis, dysphoria, and irritable unrest can persist in patients hospitalized for NPS toxicity after medical stability is achieved. These lingering psychiatric symptoms best respond to dopamine blockade with neuroleptics. This aspect of persistent cathinone toxicity makes post-hospital care challenging and heightens the importance of care providers in multiple specialties to understand this toxidrome and the associated phases of illness [93]. Fatalities following cannabimimetic use have occurred in patients discharged home with lingering paranoia and depression [50].
Multiple lines of evidence have captured the abuse and addiction potential of cathinones. These data have primarily involved mephedrone, but it is reasonable to extrapolate the findings to other cathinones with similar pharmacologic, clinical, and behavioral properties [93].
The abuse potential of synthetic cathinones can be predicted by pharmacologic activity. The ratio of dopamine to serotonin increase influences episodic (i.e., recreational) versus compulsive (i.e., addictive) use patterns [9]. Cathinones release more dopamine than serotonin (similar to methamphetamine and cocaine), which predicts drug craving, urge to re-dose, and addiction liability [76]. Drugs that release higher serotonin than dopamine levels (e.g., MDMA) tend to have a dampening effect on craving and urge to re-dose and a lower abuse potential [74,75].
A survey of 1,500 mephedrone users found more than 50% considered it addictive [150]. Of 1,006 students older than 21 years of age in Scotland, 4.4% were daily mephedrone users and 17.5% of users reported addiction/dependence symptoms [151]. In a study of 100 British mephedrone users, 47% had binged on mephedrone, 30% met Diagnostic and Statistical Manual of Mental Disorders 4th edition (DSM-IV) criteria for mephedrone dependence, and 44% described mephedrone as at least as addictive as cocaine [92]. More than 50% developed tolerance after continued use and described withdrawal symptoms of tiredness, difficulty concentrating, depression/anxiety, irritability, and ongoing cravings for mephedrone [92]. Another study found that 22.4% of mephedrone users experienced intense cravings when they stopped [152].
Frequent high-dose methcathinone, mephedrone, and MDPV use induces tolerance, dependence, craving, and a withdrawal syndrome with cessation characterized by depression, anxiety, sleep disorders, and fatigue, with craving, anhedonia, and anergia that can last several weeks [153]. Class-wide, cathinone withdrawal symptoms include depression, impulsivity, anhedonia, and cognitive complaints of poor concentration and attention [18].
A survey found that 36% of cannabimimetic users experienced tolerance and 12% developed dependence [102]. Long-term cannabimimetic use has been associated with a severe withdrawal syndrome with drug craving, tachycardia, tremor, profuse sweating, nightmares/insomnia, headache, anxiety, irritability, feelings of emptiness, depressive symptoms, and somatic complaints [102]. However, little has been published on the prevalence or natural history of cannabimimetic use disorder [154].
The abuse liability of many other NPS is anecdotal, and while pharmacologic profiles can help predict risks of craving and compulsive use (as discussed), little is known of the prevalence, natural history, or withdrawal syndromes in patients with heavy/prolonged use [3].
Helping motivate and empower patients with NPS use disorder to seek help is a challenge. Research suggests many patients with NPS use disorder do not identify as needing conventional drug treatment, with many stating they will not enroll in such services [25]. However, specialized NPS treatment programs in the UK report high demand and offer specialist assessments, detoxification, psychologic and psychosocial treatment, and support/referral for drug-related health problems [25,155].
Hospitalization for NPS overdose/toxicity presents an excellent window of opportunity (the "teachable moment") for advising patients to decrease their substance use or to engage them in treatment. Provider awareness and patient education are cornerstones of public health initiatives to confront the new challenges from NPS. Simple admonitions are insufficient, and adolescents/younger adults are wary of any communication with a judgmental, heavy-handed abstinence tone [25,61]. Patients identified with NPS use disorder in the emergency department or inpatient setting should be linked to information on local addiction treatment resources (Table 7) [61].
RESOURCES FOR PATIENTS WITH NPS USE DISORDER
|
Because patients with problematic NPS use may be ambivalent about changing behavior, clinicians should demonstrate respect for patient autonomy by expressing empathy without confrontation. Providing appropriate, accurate information on the relative risks and unknown harms of NPS empowers patients in making informed decisions to continue NPS use, attempt to quit, or seek treatment [61].
In the primary care setting, patients with NPS-related problems may present with concerns over their NPS use or with problems they suspect are NPS-related. Alternatively, patients may describe an NPS-related problem without linking it to NPS use. Motivational interviewing is suggested because this technique is proven useful in resolving patient ambivalence over change with numerous clinical conditions. This approach involves first appreciating and addressing patient concerns and withholding advice until greater clarity emerges. This empowers active patient participation and facilitates positive behavioral change. To begin this process, gain patient permission before questioning about substance use [156]. If granted, mention confidentiality. If concern is from a family member, explore further, ask about their coping, and provide info on relevant support if needed. With assessment of patients acknowledging drug use-related problems, invite active patient contribution by asking open-ended questions, such as:
"Tell me about your drug use."
"What is your drug use during an average week?"
"What concerns do you have?"
"You mentioned discomfort when urinating—how might that be related to your drug use?" (e.g., ketamine abuse associated with urinary complications)
To help build rapport, ask about drug jargon and drug effects. Giving feedback with specific reference to patient concerns can help patients re-frame their drug use and consequences.
After the basic situation and clinical picture has been established, the next steps should be determined. Further questions may include:
"Where would you like to go with this next?"
"Is there anything I can specifically help with?"
This can involve further information about the presenting problem or drug use, harm-reduction advice, guidance on managing physical or psychiatric problems, exploration of abstinence, or specialist referral.
Patients who clearly link drug use with a problem are likely to ask questions and be receptive to expert input. Apply a circular process to engage patient interest:
"Would you like to know some more about how MDPV can affect your mood?"
"When people use stimulants over a weekend and don't get any sleep, it can reduce chemicals in the brain that help keep our mood stable and feeling happy."
"How does that fit with your experience?"
Avoid assuming the patient wants to change or needs expert help to change. Instead, introduce the concept of change by asking:
"We've discussed some concerns you have, and how they might be related to your drug use. Where do we go from here?"
"Would you like to do something about your drug use?"
If a patient expresses the wish to change, ask how he or she might do this and whether professional support is needed. In patients unsure about what they should do, consider harm-reduction advice. As little is known about NPS, give general harm reduction advice such as limiting use, a period of cessation to observe improvement in health concerns, and total avoidance in high-risk patients (e.g., those with a history of psychiatric illness, addiction). The appointment should end with permission to revisit the subject in the future [156].
Patients in treatment for NPS use disorder may need to address premorbid or NPS-induced psychiatric or medical conditions or symptoms. As with other patients, those recovering from NPS use disorder probably require long-term support, professional contact, and possibly multiple short-term acute treatment episodes. Treatment typically involves components similar to those in general use, including individual and group counseling, cognitive-behavioral therapy, motivational enhancement therapy, and 12-step facilitation. Family members should be considered for involvement in the treatment program, especially with adolescent or young adult patients. Little data are available to guide pharmacologic management of acute and post-acute NPS withdrawal symptoms and ongoing NPS craving. Treatment is more complex for patients with backgrounds of polysubstance abuse, young age at initiation of regular drug use, lingering neuropsychologic impairment, or psychiatric disorders. Patients with intermittent NPS use in social settings may perceive they have less of a problem [61]. Encouragement of 12-step program involvement, such as Narcotics Anonymous, can provide patients the means for support, a non-substance-using social network, and other benefits conducive to recovery.
Bupropion
Bupropion is a ring-substituted cathinone and a dopamine and norepinephrine reuptake inhibitor. Its close structural and functional similarity with psychoactive cathinones suggests it may be beneficial in the treatment of cathinone addiction and craving. There is some evidence of benefit in treating selected methamphetamine-dependent patients with bupropion, although effectiveness has not been consistently shown [157,158].
Harm reduction neither condones nor condemns drug use, but recognizes that some risks from recreational NPS use can be mitigated. DanceSafe is the largest harm-reduction organization for North American nightlife/electronic dance music communities. Efforts by DanceSafe are directed at non-addicted recreational users, who comprise the largest number of drug users but are underserved by conventional harm reduction that targets addicted users. DanceSafe objectives include reducing drug misuse and empowering users to make informed decisions about their health and safety by providing unbiased educational literature on the effects/risks of specific drugs; remote and, when possible, on-site adulterant screening (drug testing); on-site free water and electrolytes to help prevent hyperthermia; free ear plugs; free safe sex tools to avoid pregnancy and sexually transmitted infections; and first point of contact for adverse drug effects [91]. Many other American and European harm-reduction groups use common objectives and methods.
The most effective measure against problems from NPS use is preventive, especially in educating and informing adolescents, young adults, and the general public. Helpful educational materials are available that target specific age groups, educators, parents, healthcare workers, and the public and that address health and medical consequences and the legal status of NPS [17].
As a result of the evolving racial and immigration demographics in the United States, interaction with patients for whom English is not a native language is inevitable. Because specific details about the patient's history are crucial to diagnosing NPS toxicity, effective communication is required. Communicating effectively is more challenging when the patient's primary language differs from that of the practitioner. When there is an obvious disconnect in the communication process between the practitioner and patient due to the patient's lack of proficiency in the English language, an interpreter is required.
NPS are broadly diverse in molecular structure and pharmacology. Many carry potential risks of serious adverse psychiatric effects or life-threatening toxicity. Frequent inclusion of multiple psychoactive substances in NPS products increases the risk of toxic drug interaction. Although past-year NPS use appears to have been declining since 2013–2014, intermittent regional resurgences in synthetic cathinone and cannabimimetic use, and a rapid increase in opioid and fentanyl analog use and spikes in hospital admissions and overdose/toxicity fatalities have been noted through 2021. Intrinsic NPS properties, their frequent adulteration with other substances, and highly prevalent polysubstance ingestion heighten risks of overdose and toxicity reactions urgently requiring medical care. NPS market growth is likely to continue in the near future, making it essential for primary care providers to understand the spectrum of emerging drugs in order to identify and manage potential acute and persistent effects.
1. Loeffler G, Hurst D, Penn A, Yung K. Spice, bath salts, and the U.S. military: the emergence of synthetic cannabinoid receptor agonists and cathinones in the U.S. armed forces. Mil Med. 2012;177(9):1041-1048.
2. Cottencin O, Rolland B, Karila L. New designer drugs (synthetic cannabinoids and synthetic cathinones): review of literature.Curr Pharm Des. 2014;20(25):4106-4111.
3. Brunt TM, Poortman A, Niesink RJM, van den Brink W. Instability of the ecstasy market and a new kid on the block: mephedrone. J Psychopharmacol. 2011;25(11):1543-1547.
5. American Academy of Family Physicians. 2019 Scientific Assembly Needs Assessment: Substance Use and Misuse. Available at https://www.aafp.org/dam/AAFP/documents/events/fmx/needs/fmx19-na-psy-substance-use-and-misuse.pdf. Last accessed October 26, 2021.
6. Jerry J, Collins G, Streem D. Synthetic legal intoxicating drugs: the emerging "incense" and "bath salt" phenomenon.Cleve Clin J Med. 2012;79(4):258-264.
7. Schifano F, Orsolini L, Papanti GD, Corkery JM. Novel psychoactive substances of interest for psychiatry. World Psychiatry. 2015;14(1):15-26.
8. Liechti ME. Novel psychoactive substances (designer drugs): overview and pharmacology of modulators of monoamine signaling. Swiss Med Wkly. 2015;145:w14043.
9. Watterson LR, Hood L, Sewalia K, et al. The reinforcing and rewarding effects of methylone, a synthetic cathinone commonly found in "bath salts." J Addict Res Ther. 2012;Suppl 9.
10. United Nations Office on Drugs and Crime. UNODC Early Warning Advisory on New Psychoactive Substances. Available at https://www.unodc.org/LSS/Page/NPS. Last accessed October 26, 2021.
11. European Monitoring Centre for Drugs and Drug Addiction. European Drug Report 2021: Trends and Development. Available at https://www.emcdda.europa.eu/system/files/publications/13838/TDAT21001ENN.pdf. accessed November 8, 2021.
12. Guzman AR. United States Encounters and Efforts against Synthetic Designer Drugs. Presentation at the 22nd National Conference on Pharmaceutical and Chemical Diversion. Available at https://www.deadiversion.usdoj.gov/mtgs/drug_chemical/2014/guzman.pdf. Last accessed November 8, 2021.
13. Mycyk MB. Emerging drugs of abuse: what was new yesterday is new today. J Med Toxicol. 2012;8(1):1-2.
14. European Monitoring Centre for Drugs and Drug Addiction. European Drug Report 2018: Trends and Development. Available at https://www.emcdda.europa.eu/system/files/publications/8585/20181816_TDAT18001ENN_PDF.pdf. accessed October 26, 2021.
15. European Monitoring Centre for Drugs and Drug Addiction. European Drug Report 2015. Available at https://www.emcdda.europa.eu/system/files/publications/974/TDAT15001ENN.pdf. Last accessed November 8, 2021.
16. Karila L, Megarbane B, Cottencin O, Lejoyeux M. Synthetic cathinones: a new public health problem. Curr Neuropharmacol. 2015;13(1):12-20.
17. Biliński P, Holownia P, Kapka-Skrzypczak L, Wojtyla A. Designer drug (DD) abuse in Poland: a review of the psychoactive and toxic properties of substances found during seizures of illegal drug products and resulting legal consequences thereof. Part I: cannabinoids and cathinones. Ann Agric Environ Med. 2012;19(4):857-870.
18. Scalzo AJ. Synthetic Drugs: Cannabinoids and Cathinones, Amphetamines, 2C Drugs Toxicology and Case Studies. Presented at: 2015 Midwest Pediatric Trauma Conference; May 15, 2015; St. Charles, MO.
19. United Way of Broward County Commission on Substance Abuse. Drug Abuse Trends in Broward County, Florida Annual Report: June 2015. Available at http://cdn.trustedpartner.com/docs/library/UWBCCommissionSubstanceAbuse2011/Content/Documents/Data%20Central/June%202015%20Broward%20Annual%20Trends%20Report.pdf. Last accessed November 8, 2021.
20. Carpenter TG, Cato Institute. Designer Drugs. A New, Futile Front in the War on Illegal Drugs. Policy Analysis Number 774. Available at https://www.cato.org/sites/cato.org/files/pubs/pdf/pa774_1.pdf. Last accessed November 8, 2021.
21. United Way of Broward County Commission on Substance Abuse. Drug Abuse Trends in Broward County, Florida Annual Report: June 2017. Available at https://www.unitedwaybroward.org/sites/default/files/images/Commission%20on%20Behavioral%20Health%20%26%20Drug%20Prevention/Prevention%20Resource%20Center/June-2017-Broward-Substance-Abuse-Trends-Report.pdf. Last accessed November 8, 2021.
22. European Monitoring Centre for Drugs and Drug Addiction. New Psychoactive Substances in Europe: An Update from the EU Early Warning System. Available at https://www.emcdda.europa.eu/publications/rapid-communications/2015/new-psychoactive-substances_en. Last November 18, 2021.
23. National Institute of Standards and Technology, U.S. Drug Enforcement Administration. Emerging Trends in Synthetic Drugs Workshop. Available at https://www.nist.gov/news-events/events/2013/04/emerging-trends-synthetic-drugs-workshop. Last accessed November 8, 2021.
24. Weinstein AM, Rosca P, Fattore L, London ED. Synthetic cathinone and cannabinoid designer drugs pose a major risk for public health. Front Psychiatry. 2017;8:156.
25. Boyce N. Novel Psychoactive Substances. Presented at: Third Annual Addictions and Mental Health Conference; May 25, 2015; Ontario. Available at https://www.slideshare.net/OHSUTP/novel-psychoactive-substances-an-analyis-of-the-2015-psa-cookin-with-molly. Last accessed November 8, 2021.
26. Federal Register. Health and Public Welfare. Available at https://www.federalregister.gov. Last accessed November 8, 2021.
27. Engebretsen KM. Clinical Professor, University of Minnesota, and President-elect, American Board of Applied Toxicology. Personal communication with the author, September 14, 2015.
28. Howlett AC, Thomas BF, Huffman JW. The spicy story of cannabimimetic indoles. Molecules. 2021;26(6190):1-30.
29. Weinstein AM, Rosca P, Fattore L, London ED. Synthetic cathinone and cannabinoid designer drugs pose a major risk for public health. Front Psychiatry. 2017;8:156.
30. Liu L, Wheeler SE, Venkataramanan, et al. Newly emerging drugs of abuse and their detection methods: an ACLPS critical review. Am J Clin Pathol. 2018;149(2):105-116.
31. NDEWS. National Drug Early Warning System. Available at https://ndews.org. Last accessed November 15, 2021.
32. Trecki J, Gerona RR, Schwartz MD. Synthetic cannabinoid-related illnesses and deaths. N Engl J Med. 2015;373(2):103-107.
33. U.S. Congress. HR.4459: Stop the Importation and Manufacturing of Synthetic Analogues Act of 2021 Available at https://www.congress.gov/bill/117th-congress/house-bill/4459. Last accessed November 14, 2021.
34. Centers for Disease Control and Prevention. Vital Statistics Rapid Release: Provisional Drug Overdose Death Counts. Available at https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm. Last accessed November 13, 2021.
35. Zawilska JB. An expanding world of novel psychoactive substances: opioids. Front Psychiatry. 2017;8:110.
36. American Association of Poison Control Centers. National Poison Data System. Available at https://aapcc.org/national-poison-data-system. Last accessed November 15, 2021.
37. Sacco LN, Finklea K, Congressional Research Service. Synthetic Drugs: Overview and Issues for Congress. Available at https://sgp.fas.org/crs/misc/R42066.pdf. Last accessed November 15, 2021.
38. U.S. Drug Enforcement Administration. National Drug Threat Assessment, 2020. Available at https://cesar.umd.edu/sites/cesar.umd.edu/files/pubs/DEA-Emerging-Threat-Report-2020-Annual.pdf. Last accessed November 14, 2021.
39. Schulenberg JE, Patrick ME, Johnston LD, et al. Monitoring the Future National Survey Results on Drug Use, 1975–2020: Volume II, College Students and Adults Ages 19–60. Available at http://www.monitoringthefuture.org/pubs/monographs/mtf-vol2_2020.pdf. Last accessed November 15, 2021.
40. University of Maryland Center for Substance Abuse Research. CESAR FAX Synthetic Cannabinoid Series May 9, 2011 to October 12, 2015 (updated October 13, 2015). Available at http://www.cesar.umd.edu/cesar/pubs/SyntheticCannabinoidCESARFAX.pdf. Last accessed November 15, 2021.
41. Berry-Cabán CS, Kleinschmidt PE, Rao DS, Jenkins J. Synthetic cannabinoid and cathinone use among U.S. soldiers. US Army Med Dep J. 2012;Oct-Dec:19-24.
42. Gardiner R. Banning Raves in California Won't Save Lives. Available at https://mixmag.net/feature/banning-raves-in-california-wont-save-lives. Last accessed November 16, 2021.
43. Coppola M, Mondola R. Synthetic cathinones: chemistry, pharmacology and toxicology of a new class of designer drugs of abuse marketed as "bath salts" or "plant food." Toxicol Lett. 2012;211(2):144-149.
44. Valeriani G, Corazza O, Bersani FS, et al. Olanzapine as the ideal "trip terminator"? Analysis of online reports relating to antipsychotics' use and misuse following occurrence of novel psychoactive substance-related psychotic symptoms. Hum Psychopharmacol. 2015;30(4):249-254.
45. Moore K, Dargan PI, Wood DM, Measham F. Do novel psychoactive substances displace established club drugs, supplement them or act as drugs of initiation? The relationship between mephedrone, ecstasy and cocaine. Eur Addict Res. 2013;19(5): 276-282.
46. Hohmann N, Mikus G, Czock D. Effects and risks associated with novel psychoactive substances: mislabeling and sale as bath salts, spice, and research chemicals. Dtsch Arztebl Int. 2014;111(9):139-147.
47. United Nations Office on Drugs and Crime. World Drug Report 2021. Available at https://www.unodc.org/unodc/en/data-and-analysis/wdr2021.html. Last accessed November 16, 2021.
48. Baumeister D, Tojo LM, Tracy DK. Legal highs: staying on top of the flood of novel psychoactive substances. Ther Adv Psychopharmacol. 2015;5(2):97-132.
49. United Nations Office on Drugs and Crime. Recommended Methods for the Identification and Analysis of Amphetamine, Methamphetamine and Their Ring-Substituted Analogues in Seized Materials. Available at https://www.unodc.org/pdf/scientific/stnar34.pdf. Last accessed November 16, 2021.
50. Wilson B, Tavakoli H, DeCecchis D, Mahadev V. Synthetic cannabinoids, synthetic cathinones, and other emerging drugs of abuse. Psychiatr Ann. 2013;43(12):558-564.
51. U.S. Drug Enforcement Administration. 4-Bromo-2,5-dimethoxyphenethylamine. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/bromo_dmp.pdf. Last accessed November 17, 2021.
52. U.S. Drug Enforcement Administration. 2C-I, 4-Iodo-2,5-dimethoxyphenethylamine. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/2c_i.pdf. Last accessed November 17, 2021.
53. U.S. Drug Enforcement Administration. 2,5-Dimethoxy-4-(n)-propylthiophenethylamine. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/2ct7.pdf. Last accessed November 17, 2021.
54. National Alliance for Model State Drug Laws. Novel Psychoactive Substances and Analogues: Summary of State Laws. Available at https://namsdl.org/wp-content/uploads/Novel-Psychoactive-Substances-and-Analogues-Summary-of-State-Laws.pdf. Last accessed November 21, 2021.
55. Dean BV, Stellpflug SJ, Burnett AM, Engebretsen KM. 2C or not 2C: phenethylamine designer drug review. J Med Toxicol. 2013;9(2):172-178.
56. Advisory Council on the Misuse of Drugs. NBOMe Compounds: A Review of the Evidence of Use and Harm. Available at https://www.gov.uk/government/publications/nbome-compounds-a-review-of-the-evidence-of-use-and-harm. Last accessed November 15, 2021.
57. U.S. Drug Enforcement Administration. 25-NBOMe. 25I-NBOMe, 25C-NBOMe, and 25B-NBOMe. Available at http://www.deadiversion.usdoj.gov/drug_chem_info/nbome.pdf. Last accessed November 15, 2021.
58. Erowid E, Erowid F. LSD Field Tests Differentiate LSD from 25I-NBOMe. Available at https://www.erowid.org/chemicals/lsd/lsd_testing3.shtml. Last accessed November 17, 2021.
59. Ninnemann A, Stuart GL. The NBOMe series: a novel, dangerous group of hallucinogenic drugs. J Stud Alcohol Drugs. 2013;74(6):977-978.
60. Hill SL, Doris T, Gurung S, et al. Severe clinical toxicity associated with analytically confirmed recreational use of 25I-NBOMe: case series. Clin Toxicol. 2013;51(6)487-492.
61. Weaver MF, Hopper JA, Gunderson EW. Designer drugs 2015: assessment and management. Addict Sci Clin Pract. 2015;10:8.
62. Advisory Council on the Misuse of Drugs. Benzofurans: A Review of the Evidence of Use and Harm. Available at https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/261783/Benzofuran_compounds_report.pdf. Last accessed November 17, 2018.
63. Corazza O, Schifano F, Farre M, et al. Designer drugs on the Internet: a phenomenon out-of-control? Analysis of anecdotal online reports relating to the hallucinogenic drug Bromo-Dragonfly. Curr Clin Pharmacol. 2011;6(2):125-129.
64. Biliński P, Holownia P, Kapka-Skrzypczak L, Wojtyla A. Designer drug (DD) abuse in Poland: a review of the psychoactive and toxic properties of substances found during seizures of illegal drug products and resulting legal consequences thereof. Part II: piperazines/piperidines, phenylethylamines, tryptamines and miscellaneous "others." Ann Agric Environ Med. 2012;19(4): 871-882.
65. Sainsbury PD, Kicman AT, Archer RP, King LA, Braithwaite RA. Aminoindanes: the next wave of "legal highs?" Drug Test Anal. 2011;3(7-8):479-482.
66. Nichols DE, Johnson MP, Oberlender R. 5-Iodo-2-aminoindan, a nonneurotoxic analogue of p-iodoamphetamine. Pharmacol Biochem Behav. 1991;38(1):135-139.
67. Rudnick G, Wall SC. Non-neurotoxic amphetamine derivatives release serotonin through serotonin transporters. Mol Pharmacol. 1993;43(2):271-276.
68. Graham JM, Coughenour LL, Barr BM, Rock DL, Nikam SS. 1-Aminoindanes as novel motif with potential atypical antipsychotic properties. Bioorg Med Chem Lett. 2008;18(2):489-493.
69. Iversen L, Gibbons S, Treble R, Setola V, Huang XP, Roth BL. Neurochemical profiles of some novel psychoactive substances. Eur J Pharmacol. 2013;700(1-3):147-151.
70. United Nations Office on Drugs and Crime. Details for Aminoindanes. Available at https://www.unodc.org/LSS/SubstanceGroup/Details/8fd64573-c567-4734-a258-76d1d95dca25. Last accessed November 15, 2021.
71. Sitte HH, Freissmuth M. Amphetamines, new psychoactive drugs and the monoamine transporter cycle. Trends Pharmacol Sci. 2015;36(1):41-51.
72. Cozzi NV, Sievert MK, Shulgin AT, Jacob P 3rd, Ruoho AE. Inhibition of plasma membrane monoamine transporters by beta-ketoamphetamines. Eur J Pharmacol. 1999;381(1):63-69.
73. Prosser JM, Nelson LS. The toxicology of bath salts: a review of synthetic cathinones. J Med Toxicol. 2012;8(1):33-42.
74. Baumann MH, Partilla JS, Lehner KR. Psychoactive "bath salts:" not so soothing. Eur J Pharmacol. 2013;698(1-3):1-5.
75. Baumann MH, Ayestas MA Jr, Partilla JS, et al. The designer methcathinone analogs, mephedrone and methylone, are substrates for monoamine transporters in brain tissue. Neuropsychopharmacology. 2012;(5)37:1192-1203.
76. Rothman RB, Baumann MH. Monoamine transporters and psychostimulant drugs. Eur J Pharmacol. 2003;479(1-3):23-40.
77. Murray BL, Murphy CM, Beuhler MC. Death following recreational use of designer drug "bath salts" containing 3,4-methylenedioxypyrovalerone (MDPV). J Med Toxicol. 2012;8(1):69-75.
78. National Alliance for Model State Drug Laws. An Introduction to Synthetic Drugs. Available at https://namsdl.org/wp-content/uploads/An-Introduction-to-Synthetic-Drugs.pdf. Last accessed November 18, 2021.
79. Watterson LR, Kufahl PR, Nemirovsky NE, et al. Potent rewarding and reinforcing effects of the synthetic cathinone 3,4-methylenedioxypyrovalerone (MDPV). Addict Biol. 2014;19(2):165-174.
81. Paillet-Loilier M, Cesbron A, Le Boisselier R, Bourgine J, Debruyne D. Emerging drugs of abuse: current perspectives on substituted cathinones. Subst Abuse Rehabil. 2014;5:37-52.
82. Advisory Council on the Misuse of Drugs. ACMD Report on the Consideration of the Cathinones. Available at https://www.gov.uk/government/publications/acmd-report-on-the-consideration-of-the-cathinones. Last accessed November 18, 2021.
83. Simmler LD, Buser TA, Donzelli M, et al. Pharmacological characterization of designer cathinones in vitro. Br J Pharmacol. 2013;168(2):458-470.
84. Saha K, Partilla JS, Lehner KR, et al. Second-generation mephedrone analogs, 4-MEC and 4-MePPP, differentially affect monoamine transporter function. Neuropsychopharmacology. 2015;40(6):1321-1331.
85. Rickli A, Hoener MC, Liechti ME. Monoamine transporter and receptor interaction profiles of novel psychoactive substances: para-halogenated amphetamines and pyrovalerone cathinones. Eur Neuropsychopharmacol. 2015;25(3):365-376.
86. European Monitoring Centre for Drugs and Drug Addiction. Synthetic Cathinones Drug Profile. Available at http://www.emcdda.europa.eu/publications/drug-profiles/synthetic-cathinones. Last accessed November 18, 2021.
87. U.S. Drug Enforcement Administration. 4-Methylmethcathinone (Mephedrone). Available at http://www.deadiversion.usdoj.gov/drug_chem_info/mephedrone.pdf. Last accessed November 17, 2021.
88. Angoa-Pérez M, Kane MJ, Briggs DI, et al. Mephedrone does not damage dopamine nerve endings of the striatum but enhances the neurotoxicity of methamphetamine, amphetamine and MDMA. J Neurochem. 2013;125(1):102-110.
89. National Alliance for Model State Drug Laws. Novel Psychoactive Substances and Analogues: 2017 Legislative Session Bill Status Update. Available at http://namsdl.dynamicwebware.com/News%20Tab/Highlighted%20Issues/NPS%20and%20Analogues%202017%20Bill%20Status%20Update.pdf. Last accessed November 14, 2021.
90. U.S. Drug Enforcement Administration. 3,4-Methylenedioxypyrovalerone (MDPV). Available at https://www.deadiversion.usdoj.gov/drug_chem_info/mdpv.pdf. Last accessed November 21, 2021.
91. DanceSafe. Available at https://dancesafe.org. Last accessed November 20, 2021.
92. Winstock AR, Mitcheson LR, Deluca P, et al. Mephedrone, new kid for the chop? Addiction. 2011;106(1):154-161.
93. Keary CJ, Nejad SH, Rasimas JJ, Stern TA. Intoxications associated with agitation, tachycardia, hypertension, and fever: differential diagnosis, evaluation, and management. Prim Care Companion CNS Disord. 2013;15(3).
94. Ross EA, Reisfield GM, Watson MC, Chronister CW, Goldberger BA. Psychoactive "bath salts" intoxication with methylenedioxypyrovalerone. Am J Med. 2012;125(9):854-858.
95. Penders TM, Gestring RE, Vilensky DA. Intoxication delirium following use of synthetic cathinone derivatives. Am J Drug Alcohol Abuse. 2012;38(6):616-617.
96. Goshgarian AM, Benford DM, Caplan JP. Bath salt abuse: neuropsychiatric effects of cathinone derivatives. Psychosomatics. 2011;52(6):593-594.
97. Goodnough A, Zezima K. An Alarming New Stimulant, Legal in Many States. Available at https://www.nytimes.com/2011/07/17/us/17salts.html?_r=0. Last accessed November 17, 2021.
98. Spiller HA, Ryan ML, Weston RG, Jansen J. Clinical experience with and analytical confirmation of "bath salts" and "legal highs" (synthetic cathinones) in the United States. Clin Toxicol (Phila). 2011;49(6):499-505.
99. Adebamiro A, Perazella MA. Recurrent acute kidney injury following bath salts intoxication. Am J Kidney Dis. 2012;59(2):273-275.
100. Borek HA, Holstege CP. Hyperthermia and multiorgan failure after abuse of "bath salts" containing 3,4-methylenedioxypyrovalerone. Ann Emerg Med. 2012;60(1):103-105.
101. National Institute on Drug Abuse. Synthetic Cathinones ("Bath Salts") DrugFacts. Available at https://www.drugabuse.gov/publications/drugfacts/synthetic-cathinones-bath-salts. Last accessed November 17, 2021.
102. Papanti D, Orsolini L, Francesconi G, Schifano F. "Noids" in a nutshell: everything you (don't) want to know about synthetic cannabimimetics. Adv Dual Diagn. 2014;7(3):137-148.
103. European Monitoring Centre for Drugs and Drug Addiction. Understanding the "Spice" Phenomenon. Available at https://www.emcdda.europa.eu/publications/thematic-papers/understanding-spice-phenomenon_en. Last accessed November 18, 2021.
104. European Monitoring Centre for Drugs and Drug Addiction. Synthetic Cannabinoids and "Spice" Drug Profile. Available athttps://www.emcdda.europa.eu/publications/drug-profiles/synthetic-cannabinoids. Last accessed November 18, 2021.
106. Goss C. Treatment considerations for patients using so-called legal recreational drugs. JEMS. 2015;40(7):1-12.
107. Sullivan JW. New Drugs of Abuse. Available at http://www.upstate.edu/poison/pdf/community/synthetic_drugs_sullivan.pdf. Last accessed November 18, 2021.
108. Spaderna M, Addy PH, D'Souza DC. Spicing things up: synthetic cannabinoids. Psychopharmacology (Berl). 2013;228(4):525-540.
109. Hurst D, Loeffler G, McLay R. Psychosis associated with synthetic cannabinoid agonists: a case series. Am J Psychiatry. 2011;168(10):1119.
110. van Amsterdam J, Brunt T, van den Brink W. The adverse health effects of synthetic cannabinoids with emphasis on psychosis-like effects. J Psychopharmacol. 2015;29(3):254-263.
111. Gatch MB, Forster MJ, Janowsky A, Eshleman AJ. Abuse liability profile of three substituted tryptamines. J Pharmacol Exp Ther. 2011;338(1):280-289.
112. Tittarelli R, Mannocchi G, Pantano F, Romolo FS. Recreational use, analysis and toxicity of tryptamines. Curr Neuropharmacol. 2015;13(1):26-46.
113. U.S. Drug Enforcement Administration. 5-Methoxy-N,N-diisopropyltryptamine. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/5meodipt.pdf. Last accessed November 18, 2021.
114. Carroll FI, Lewin AH, Mascarella SW, Seltzman HH, Reddy PA. Designer drugs: a medicinal chemistry perspective. Ann N Y Acad Sci. 2012;1248:18-38.
115. European Monitoring Centre for Drugs and Drug Addiction. Europol Joint Report on a New Psychoactive Substance: Methoxetamine (2-(3-methoxyphenyl)-2-(ethylamino)cyclohexanone). Available at https://www.emcdda.europa.eu/publications/joint-report/methoxetamine. Last accessed November 18, 2021.
116. Coppola M, Mondola R. Methoxetamine: from drug of abuse to rapid-acting antidepressant. Med Hypotheses. 2012;79(4):504-507.
117. Kjellgren A, Jonsson K. Methoxetamine (MXE): a phenomenological study of experiences induced by a "legal high" from the Internet. J Psychoactive Drugs. 2013;45(3):276-286.
118. Elliott SP, Brandt SD, Wallach J, Morris H, Kavanagh PV. First reported fatalities associated with the "research chemical" 2-methoxydiphenidine. J Anal Toxicol. 2015;39(4):287-293.
119. Lynch K, American Association for Clinical Chemistry. Drug Testing: the Moving Target. Available at https://www.aacc.org/~/media/files/meetings-and-events/resources-from-past-events/conferences/2015/profprac/slides-and-handouts/designerdrugs_handouts_lynch.pdf?la=en. Last accessed November 18, 2021.
120. U.S. Drug Enforcement Administration. Khat. Available at https://www.dea.gov/factsheets/khat. Last accessed November 18, 2021.
121. Johnson MW, MacLean KA, Reissig CJ, Prisinzano TE, Griffiths RR. Human psychopharmacology and dose-effects of salvinorin A, a kappa-opioid agonist hallucinogen present in the plant Salvia divinorum. Drug Alcohol Depend. 2011;115(1-2):150-155.
122. U.S. Drug Enforcement Administration. Salvia divinorum and Salvinorin A. Available at https://www.deadiversion.usdoj.gov/drug_chem_info/salvia_d.pdf. Last accessed November 18, 2021.
123. Addy PH, Garcia-Romeu A, Metzger M, Wade J. The subjective experience of acute, experimentally-induced Salvia divinorum inebration. J Psychopharmacol. 2015;29(4):426-435.
124. U.S. Drug Enforcement Administration. Kratom (Mitragyna speciosa korth). Available at https://www.deadiversion.usdoj.gov/drug_chem_info/kratom.pdf. Last accessed November 18, 2021.
125. Vilke GM, Bozeman WP, Dawes DM, Demers G, Wilson MP. Excited delirium syndrome (ExDS): treatment options and considerations. J Forensic Leg Med. 2012;19(3):117-121.
126. American College of Emergency Physicians, ACEP Excited Delirium Task Force. White Paper Report on Excited Delirium Syndrome. Available at https://www.prisonlegalnews.org/media/publications/acep_report_on_excited_delirium_syndrome_sept_2009.pdf. Last accessed November 18, 2021.
127. Penders TM, Gestring RE, Vilensky DA. Excited delirium following use of synthetic cathinones (bath salts). Gen Hosp Psychiatry. 2012;34(6):647-650.
130. Mash D, Duque L, Pablo J, et al. Brain biomarkers for identifying excited delirium as a cause of sudden death. Forensic Sci Int. 2009;190(1-3):e13-e19.
131. Lusthof KJ, Oosting R, Maes A, Verschraagen M, Dijkhuizen A, Sprong AG. A case of extreme agitation and death after the use of mephedrone in the Netherlands. Forensic Sci Int. 2011;206(1-3):e93-e95.
132. Scheppke KA, Braghiroli J, Shalaby M, Chait R. Prehospital use of IM ketamine for sedation of violent and agitated patients.West J Emerg Med. 2014;15(7):736-741.
133. Keseg D, Cortez E, Rund D, Caterino J. The use of prehospital ketamine for control of agitation in a metropolitan firefighter-based EMS system. Prehosp Emerg Care. 2015;19(1):110-115.
134. Burnett AM, Peterson BK, Stellpflug SJ, et al. The association between ketamine given for prehospital chemical restraint with intubation and hospital admission. Am J Emerg Med. 2015;33(1):76-79.
135. Burnett AM, Salzman JG, Griffith KR, Kroeger B, Frascone RJ. The emergency department experience with prehospital ketamine: a case series of 13 patients. Prehosp Emerg Care. 2012;16(4):553-559.
136. van Loggerenberg CJ. Emergency management of drug abuse in South Africa. S Afr Med J. 2012;30(11):409-412.
137. Addolorato G, Leggio L, Abenavoli L, Gasbarrini G, Alcoholism Treatment Study Group. Neurobiochemical and clinical aspects of craving in alcohol addiction: a review. Addict Behav. 2005;30(6):1209-1224.
138. Clapp P, Bhave SV, Hoffman PL. How adaptation of the brain to alcohol leads to dependence: a pharmacological perspective. Alcohol Res Health. 2008;31(4):310-339.
139. Baguley IJ, Heriseanu RE, Cameron ID, Nott MT, Slewa-Younan S. A critical review of the pathophysiology of dysautonomia following traumatic brain injury. Neurocrit Care. 2008;8(2):293-300.
140. Baguley IJ, Heriseanu RE, Nott MT, Chapman J, Sandanam J. Dysautonomia after severe traumatic brain injury: evidence of persisting overresponsiveness to afferent stimuli. Am J Phys Med Rehabil. 2009;88(8):615-622.
141. Srinivasan S, Tchoyoson Lim CC, Thirugnanam U. Paroxysmal autonomic instability with dystonia. Clin Auton Res. 2007;17(6):378-381.
142. Bone RC, Balk RA, Cerra FB, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Chest. 2009;136(5 Suppl):e28.
143. Dalmau J, Tüzün E, Wu HY, et al. Paraneoplastic anti-N-methyl-d-aspartate receptor encephalitis associated with ovarian teratoma. Ann Neurol. 2007;61(1):25-36.
144. Fink M, Taylor MA. The many varieties of catatonia. Eur Arch Psychiatry Clin Neurosci. 2001;251(Suppl 1):I8-I13.
145. Iqbal MM, Basil MJ, Kaplan J, Iqbal T. Overview of serotonin syndrome. Ann Clin Psychiatry. 2012;24(4):310-318.
147. Gold JA, Rimal B, Nolan A, Nelson LS. A strategy of escalating doses of benzodiazepines and phenobarbital administration reduces the need for mechanical ventilation in delirium tremens. Crit Care Med. 2007;35(3):724-730.
148. Dunkley EJ, Isbister GK, Sibbritt D, Dawson AH, Whyte IM. The Hunter Serotonin Toxicity Criteria: simple and accurate diagnostic decision rules for serotonin toxicity. QJM. 2003;96(9):635-642.
150. Carhart-Harris RL, King LA, Nutt DJ. A web-based survey on mephedrone. Drug Alcohol Depend. 2011;118(1):19-22.
151. Dargan PI, Albert S, Wood DM. Mephedrone use and associated adverse effects in school and college/university students before the UK legislation change. QJM. 2010;103(11):875-879.
152. Winstock A, Mitcheson L, Ramsey J, Davies S, Puchnarewicz M, Marsden J. Mephedrone: use, subjective effects and health risks. Addiction. 2011;106(11):1991-1996.
153. Coppola M, Mondola R. 3,4-methylenedioxypyrovalerone (MDPV): chemistry, pharmacology and toxicology of a new designer drug of abuse marketed online. Toxicol Lett. 2012;208(1):12-15.
154. Zimmermann US, Winkelmann PR, Pilhatsch M, et al. Withdrawal phenomena and dependence syndrome after the consumption of "spice gold." Dtsch Arztebl Int. 2009;106(27):464-467.
155. Advisory Council on the Misuse of Drugs. Consideration of the Novel Psychoactive Substances ("Legal Highs"). Available at https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/119139/acmdnps2011.pdf. Last accessed November 21, 2021.
156. Winstock AR, Mitcheson L. New recreational drugs and the primary care approach to patients who use them. BMJ. 2012;344:e288.
157. Karila L, Weinstein A, Aubin HJ, Benyamina A, Reynaud M, Batki SL. Pharmacological approaches to methamphetamine dependence: a focused review. Br J Clin Pharmacol. 2010;69(6):578-592.
158. Rose ME, Grant JE. Pharmacotherapy for methamphetamine dependence: a review of the pathophysiology of methamphetamine addiction and the theoretical basis and efficacy of pharmacotherapeutic interventions. Ann Clin Psychiatry. 2008;20(3):145-155.
159. U.S. Drug Enforcement Administration. DEA Announces Intent to Schedule Kratom. Available at https://www.dea.gov/press-releases/2016/08/30/dea-announces-intent-schedule-kratom. Last accessed November 18, 2021.
160. Wright TH, Harris C. Twenty-One Cases Involving Alpha-Pyrrolidinoyalerophenone (α-PVP). J Anal Toxicol. 2016;40(5):396-402.
161. U.S. Drug Enforcement Administration. About Synthetic Drugs. Available at https://www.deadiversion.usdoj.gov/synthetic_drugs/about_sd.html. Last accessed November 8, 2021.
Mention of commercial products does not indicate endorsement.