Type 2 diabetes represents a growing healthcare crisis on a national and worldwide scale. As the population increases, including growing subpopulations of obese and elderly individuals, type 2 diabetes is anticipated to endure as one of the top causes of morbidity and mortality in the United States. Fortunately, novel agents, formulations, and devices have been developed that can help patients reach A1c goals with less negative impact on quality of life, although balancing patient needs, glycemic targets, and unwanted side effects is still considered to be difficult by many healthcare professionals. Significant barriers in type 2 diabetes remain. Research has yet to determine the optimal A1c target that should be assigned to most diabetes patients, and low levels of therapeutic adherence continue to counteract treatment efficacy. Still, as knowledge and technology advances, there is the potential these obstacles will be overcome and outcomes in type 2 diabetes will be vastly improved.
- INTRODUCTION
- EPIDEMIOLOGY OF TYPE 2 DIABETES
- PATHOPHYSIOLOGY OF TYPE 2 DIABETES
- DIAGNOSIS OF TYPE 2 DIABETES
- TREATMENT OPTIONS IN TYPE 2 DIABETES
- ISSUES SURROUNDING TIGHT GLYCEMIC CONTROL
- THE ROLE OF ADHERENCE IN ACHIEVING TREATMENT GOALS
- OTHER STRATEGIES TO MAXIMIZE ADHERENCE
- CONCLUSION
- Works Cited
- Evidence-Based Practice Recommendations Citations
This course is designed for all physicians, physician assistants, nurses, pharmacists, and pharmacy technicians involved in the care of patients with type 2 diabetes.
The purpose of this course is to provide healthcare providers with the information necessary to develop treatment regimens associated with optimal adherence and provide adequate patient education, counseling, and support.
Upon completion of this course, you should be able to:
- Apply epidemiologic trends in type 2 diabetes mellitus (T2DM) to current practice so at-risk patient populations can be more easily identified, assessed, and treated for T2DM.
- Utilize knowledge of the pathophysiology and diagnosis of T2DM to create comprehensive treatment strategies that target critical pathways in T2DM development and progression.
- Identify the therapies for T2DM that are supported by contemporary evidence and are in adherence with current guideline recommendations.
- Discuss the risks and benefits of tight glycemic control when setting and achieving A1c targets in patients with T2DM.
- Describe strategies to improve patient adherence to T2DM medication by developing treatment regimens associated with optimal adherence and providing adequate patient education, counseling, and support.
John J. Whyte, MD, MPH, is currently the Chief Medical Officer at WebMD. In this role, he leads efforts to develop and expand strategic partnerships that create meaningful change around important and timely public health issues. Previously, Dr. Whyte was the Director of Professional Affairs and Stakeholder Engagement at the FDA’s Center for Drug Evaluation and Research and the Chief Medical Expert and Vice President, Health and Medical Education at Discovery Channel, part of the media conglomerate Discovery Communications.
Prior to this, Dr. Whyte was in the Immediate Office of the Director at the Agency for Healthcare Research Quality. He served as Medical Advisor/Director of the Council on Private Sector Initiatives to Improve the Safety, Security, and Quality of Healthcare. Prior to this assignment, Dr. Whyte was the Acting Director, Division of Medical Items and Devices in the Coverage and Analysis Group in the Centers for Medicare & Medicaid Services (CMS). CMS is the federal agency responsible for administering the Medicare and Medicaid programs. In his role at CMS, Dr.Whyte made recommendations as to whether or not the Medicare program should pay for certain procedures, equipment, or services. His division was responsible for durable medical equipment, orthotics/prosthetics, drugs/biologics/therapeutics, medical items, laboratory tests, and non-implantable devices. As Division Director as well as Medical Officer/Senior Advisor, Dr. Whyte was responsible for more national coverage decisions than any other CMS staff.
Dr. Whyte is a board-certified internist. He completed an internal medicine residency at Duke University Medical Center as well as earned a Master’s of Public Health (MPH) in Health Policy and Management at Harvard University School of Public Health. Prior to arriving in Washington, Dr. Whyte was a health services research fellow at Stanford and attending physician in the Department of Medicine. He has written extensively in the medical and lay press on health policy issues.
Contributing faculty, John J. Whyte, MD, MPH, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
John M. Leonard, MD
Margo A. Halm, RN, PhD, NEA-BC, FAAN
Randall L. Allen, PharmD
The division planners have disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#94524: Type 2 Diabetes: Treatment Strategies for Optimal Care
Diabetes mellitus describes a group of metabolic diseases that cause prolonged, elevated blood glucose levels. This condition affects approximately 38.4 million Americans, or 11.6% of the U.S. population [1]. Although there are several types of diabetes (including type 1 or insulin-dependent diabetes and gestational diabetes), type 2 diabetes mellitus (T2DM) comprises 90% to 95% of all cases [2,3].
The impact of T2DM is shocking. In 2021, it was the eighth leading cause of death, was the underlying cause of an estimated 103,294 deaths, and was identified as a contributing factor to an additional 399,401 deaths in the United States [1]. Much of the morbidity and mortality of T2DM results from the numerous complications associated with the disease, including heart disease, stroke, elevated blood pressure, blindness, kidney disease, and neuropathy [1]. These conditions contribute to a total U.S. cost of diabetes of $413 billion, including $307 billion in direct medical costs and $106 billion in indirect costs such as disability, work loss, and premature mortality [1]. The economic burden of T2DM is paralleled by an equally substantial personal and social burden; T2DM is associated with significant decreases in health-related quality of life [4]. Given the extensive negative impact of T2DM, it is critical that healthcare providers optimize treatment of this condition to minimize its negative effects on morbidity, mortality, and quality of life.
Trends in T2DM have rapidly changed in the past 50 years, with a sharp increase in prevalence and incidence seen in the early 1990s and leveling out in the late 2000s. While the prevalence, or total number of existing cases, of T2DM continues to rise, the incidence, or rate of new cases of diagnosed T2DM, has been declining since 2008 [5]. Among adults 18 years of age or older, the age-adjusted incidence of diagnosed diabetes was similar in 2000 (6.2 per 1,000 adults) and 2021 (5.8 per 1,000 adults). A significant decreasing trend in incidence was detected after 2008 (8.4 per 1,000 adults) through 2021 [1,5]. Additional data are needed to determine the cause for the decline and if the incidence will continue to decrease.
The prevalence of T2DM is still increasing, but at a much slower pace than seen in previous decades; this slower rate is thought to be in part due to improved self-management techniques and healthcare services, resulting in patients living longer [5]. One study illustrates the upward trend, noting that the prevalence of diabetes among U.S. adults increased 74% between 1976–1980 and 1999–2004, from 5.08% to 8.83% [6]. During 2001–2020, the age-adjusted prevalence of total diabetes increased among adults 18 years of age and older. Prevalence estimates for total diabetes were 10.3% in 2001–2004 and 13.2% in 2017–2020 [1]. In the United States, the crude prevalence of diagnosed diabetes in adults (age ≥18 years) increased from 6.5% in 2002 to 9.6% in 2022 [7]. In 2010, researchers estimated that the U.S. prevalence of diabetes could be as high as 28% of the total population by 2050, but based on updated trends of diabetes, newer estimates using similar methods estimate that the prevalence of diabetes will be approximately 18% in 2060 [8,9].
Several causes for the extreme increase in incidence of T2DM in the late 20th century have been noted. First, the U.S. population is expanding annually, resulting in an increase in the number of people with T2DM [10]. Second, rising rates of overweight and obesity correlate with the rising incidence of T2DM, as these factors have a positive association [5,11]. Rates of obesity were 15% in 1980, 23% in 1994, 31% in 2000, 35% in 2011–2012, and more than 42% in 2017–2018 [5,12,13]. Among those with diabetes, 89.8% of patients are overweight or obese, with 47.1% being obese (body mass index [BMI] >30 kg/m2 to ≤39.9 kg/m2) and 15.7% being classified as severely obese (BMI >40 kg/m2) [1,6]. Third, because T2DM disproportionately affects elderly individuals, rising rates of T2DM are anticipated to reflect the steadily growing population of adults 65 years of age and older [10,14]. It has also been observed that T2DM appears to be occurring at a greater frequency in younger adults. Between 1988–1994 and 1999–2000, the mean age at diagnosis of T2DM decreased from 52 years to 46 years, and in 2015, more than one-half of new cases were among adults 45 to 64 years of age [5,15]. Rates of incidence, both increasing and decreasing, can be attributed to changing diagnostic criteria, improved physician recognition of T2DM, and increased public awareness, making additional research necessary to determine if changes in incidence rates are due to prevention and treatment strategies or if the rates reflect a shifting trend toward earlier onset of T2DM [15].
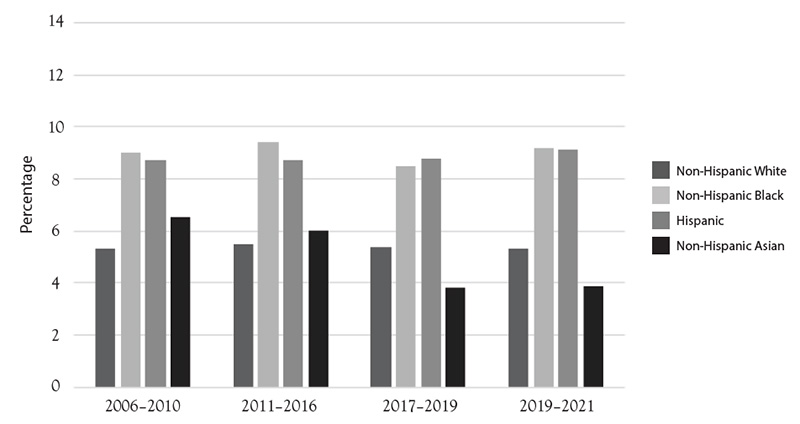
T2DM is marked by a number of disparities among affected groups, most notably within specific racial and ethnic populations. For example, while the number of non-Hispanic White persons in the United States with T2DM far exceeds the number of non-Hispanic Black individuals with this condition, the percentage of non-Hispanic Black individuals with T2DM (12.1%) is significantly greater than that of non-Hispanic White Americans (6.9%) (Figure 1) [1]. Hispanic Americans also appear to be disproportionately affected by T2DM, with studies indicating rates of T2DM to be significantly higher in this population compared to non-Hispanic White individuals (11.7% and 6.9%, respectively) [1]. Asian Americans have a slightly higher rate (9.1%) compared to non-Hispanic White Americans (6.9%) [1]. In addition, the group reporting the largest percentage of T2DM, at 13.6% of the total adult population, is American Indians and Alaska Natives [1]. Increasing numbers of members of high-risk minority groups in the United States contribute to the overall projected rise of T2DM [8]. Therefore, targeting these populations for prevention, intervention, and education is a strategy that can be employed to mitigate the impact of T2DM across the nation.
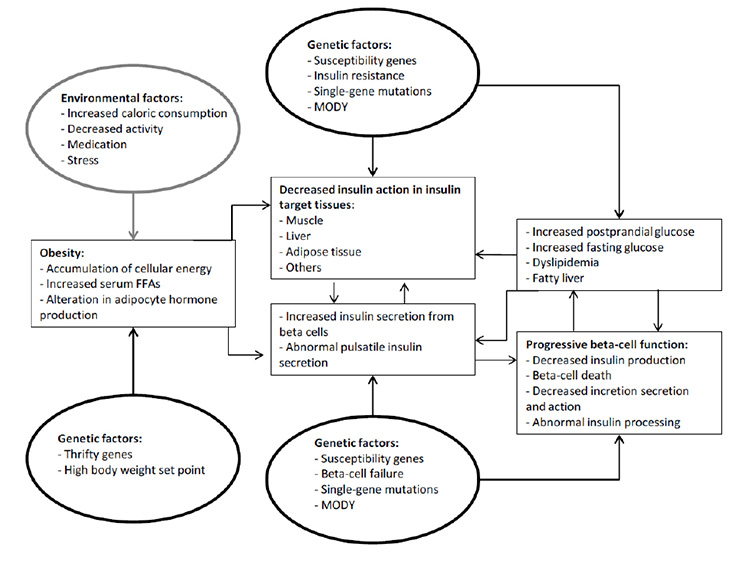
A number of predisposing risk factors have been attributed to the development of T2DM, most notably obesity, which affects cellular metabolism, serum free fatty acids, and adipocyte hormone production (Figure 2) [16,17,18]. Other environmental factors, including poor diet (evidenced by increased caloric intake as well as decreased food quality) and decreased activity, amplify these effects, as can certain medications and ongoing stress [16,19]. However, these factors alone are not adequate to initiate T2DM; certain genetic characteristics must also be present. To date, a large number of loci possessing common variants have been implicated in diabetes susceptibility, aided in great part by genome-wide association—a hypothesis-generating approach directed at linking new loci with a disease or trait of interest (in this instance, T2DM) [20,21]. The exact combination of genetic and environmental factors that generates T2DM is as yet unknown, but research continues to elucidate potential contributors.
Impaired insulin secretion is a key mechanism in the development of T2DM. The framework for this process is built on the understanding that insulin is secreted from beta cells and hyperglycemia occurs when beta-cell secretion of insulin is inadequate respective to the glucose load [22]. In healthy individuals, glucose ingestion (and resultant increase in plasma glucose concentration) triggers the production and release of insulin by pancreatic beta cells [22]. In those with T2DM, insulin response to glucose declines as a result of a functional beta-cell deficiency [23]. This defect has been demonstrated by findings that islet function appears to be approximately 50% of normal at the time of diagnosis and is supported by data from the United Kingdom Prospective Diabetes Study (UKPDS), in which patients who achieved beta-cell function greater than 55% with sulfonylurea monotherapy were less likely to require additional therapy to maintain glycemic targets [24]. Thus, it is now understood that insulin sensitivity is inversely and proportionally related to beta-cell function [24]. These processes are further exacerbated when the inability of the pancreas to adapt beta-cell mass to insulin demand (referred to as pancreas plasticity) results in a decrease in functional beta-cell mass [16]. Studies have revealed an approximate 40% reduction in beta-cell mass in patients with impaired glucose tolerance and a 60% reduction in beta-cell mass in patients with T2DM compared to healthy individuals [24].
Incretin hormones, hormones released from gut endocrine cells during meals, also play a significant role in insulin secretion [25]. Glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP) may be responsible for as much as 70% of postprandial insulin secretion in healthy individuals, but demonstrate severely reduced or even absent effects in those with T2DM, often referred to as the incretin effect. This incretin effect is believed to contribute to the impaired insulin regulation and glucagon secretion that are the hallmarks of T2DM, and studies have demonstrated that improved glycemic control in patients with T2DM partially restores the impaired action of GLP-1 and GIP [16].
Another central mechanism of T2DM is insulin resistance, which is characterized by the failure of insulin to decrease plasma glucose levels through hepatic glucose suppression and stimulation of glucose uptake in skeletal muscle and adipose tissue [22]. Consequently, inefficient glucose utilization is replaced by cellular utilization of fats and proteins. Factors that contribute to insulin resistance are complex and may include defective insulin-mediated cell signaling pathways, decreased muscle glycogen syntheses, and reduced numbers of skeletal muscle, liver, and adipose tissue insulin receptors (particularly in obese individuals). In many cases, insulin resistance may be the earliest detectable marker for T2DM [22]. Patients who transition from normal glucose tolerance to T2DM typically experience a 40% decrease in insulin sensitivity, which is further accentuated by chronic hyperglycemia and elevated free fatty acids.
An additional regulator of glucose homeostasis is the liver, which is involved in several processes, including hepatic glucose output/uptake and insulin clearance [26]. In healthy individuals, peripheral glucose uptake is equal to circulatory glucose input from the liver, gut, and kidney [26]. The hyperglycemia of T2DM is the result of abnormally high hepatic glucose output stemming from hepatic insulin insensitivity (unlike healthy individuals, in which hyperinsulinemia would suppress hepatic glucose output) [26]. This increased hepatic glucose output closely correlates with the severity of fasting hyperglycemia. Although the postabsorptive levels of chronic hyperinsulinemia observed in mild hyperglycemia offset hepatic insulin resistance and maintain normal hepatic glucose output, moderate fasting hyperglycemia is associated with significant increases in hepatic glucose output [22].
Adipocyte dysfunction has been implicated in abnormal metabolism and altered fat disposition, an important pathway of glucose intolerance in T2DM [22]. Excessive caloric intake causes adipocytes to undergo excessive hypertrophy, resulting in adipocyte dysfunction and adipose tissue endocrine and immune reactions [27]. As fat accumulates (with preference to the abdominal-perivisceral region), excessive free fatty acids are released into the portal system [27]. This, combined with the resistance of fat cells to insulin's antilipolytic effects, induces hepatic/muscular insulin resistance and impairs insulin secretion—disturbances that are referred to as lipotoxicity [22]. This phenomenon also causes fat cells to produce excessive amounts of insulin resistance-inducing, atherosclerotic-provoking, and inflammatory cytokines (inducing a state of chronic, low-grade inflammation). It also diminishes fat cells' ability to secrete adequate amounts of insulin-sensitizing adipocytokines [22,27]. All of these effects contribute to the development of insulin resistance, impaired insulin secretion, and ultimately, T2DM.
Amino acid metabolism may play a key role early in the development of type 2 diabetes. Studies suggest that the risk of future diabetes is higher in normoglycemic individuals with high fasting plasma concentrations of select amino acids and that amino acid metabolism is disturbed in diabetes [28,29].
Diagnosis of T2DM primarily focuses on glycated hemoglobin (A1c), a shift from historical methods of assessing fasting plasma glucose (FPG) or the two-hour value derived from the 75-gram oral glucose tolerance test (OGTT) [30]. This method of T2DM diagnosis was recommended in 2009 by an international expert committee comprised of representatives from the American Diabetes Association (ADA), the International Diabetes Federation (IDF), and the European Association for the Study of Diabetes (EASD). The recommendation was based on epidemiologic data demonstrating a corresponsive relationship between A1c, FPG, and two-hour plasma glucose (PG) thresholds. A1c offers several advantages over FPG and OGTT, such as improved patient convenience, greater stability, and less daily deviations resulting from stress and illness. However, this test is more costly and has limited availability worldwide. Moreover, limited (controversial) data suggest that glycation rates can vary according to race. Perhaps most importantly, A1c results do not 100% correlate with FPG and the two-hour PG test [30]. Still, the reduced sensitivity of A1c is generally believed to be offset by the benefits of enhanced practicality convenience, thus the recommendation from the ADA, IDF, and EASD.
According to the ADA, a diagnosis of T2DM can be confirmed in patients whose A1c level is 6.5% or higher. T2DM can also be diagnosed with FPG ≥126 mg/dL, two-hour PG ≥200 mg/dL during an OGTT, or random plasma glucose ≥200 mg/dL in patients with classic symptoms of hyperglycemia or hyperglycemia crisis [30]. Prediabetes—a condition in which glucose levels are below diagnosis criteria but higher than a normal range—can also be diagnosed in those with FPG 100–125 mg/dL, two-hour PG 140–199 mg/dL in OGTT, or A1c level of 5.7% to 6.4%, although the World Health Organization and several other diabetes groups define prediabetes at a FPG of 110 mg/dL [30].
In asymptomatic patients, T2DM testing should be considered in adults of any age with a BMI ≥25 kg/m2 (or ≥23 kg/m2 in Asian Americans) who have one or more additional risk factors for diabetes. Those without risk factors should undergo testing beginning at 35 years of age. Because as much as one-quarter of Americans, and nearly one-half of Asian and Hispanic Americans, with diabetes may be undiagnosed, efforts are underway to assess the efficacy of prediabetes identification in preventing T2DM [30].
Several specialty organizations, including the American College of Endocrinology (ACE), the American Association of Clinical Endocrinologists (AACE), and the ADA, have published position papers addressing the standards of care and approach to therapy for patients with diabetes [30,31,32,33]. The American College of Physicians (ACP), in a practice guideline published in 2012, and updated in 2017, provides a good overview of clinical considerations and recommendations for oral therapy (Table 1) [34]. These groups are in agreement that effective management of T2DM requires careful attention to nonpharmacologic and pharmacologic modalities of therapy combined with patient education and self-management training.
AMERICAN COLLEGE OF PHYSICIANS RECOMMENDATIONS AND CLINICAL CONSIDERATIONS FOR ORAL MEDICATION IN T2DM
| Recommendations | |||||||
| |||||||
| Clinical Considerations | |||||||
|
Despite skepticism by some clinicians, providing dietary information to patients has been found to be an effective intervention. The U.S. Preventive Services Task Force, an independent panel of experts in primary care and prevention that systematically reviews the evidence of effectiveness and develops recommendations for clinical preventive services, found good evidence that medium-to high-intensity counseling interventions can produce medium-to-large changes in average daily intake of core components of a healthy diet (including saturated fat, fiber, fruits, and vegetables) among adult patients at increased risk for diet-related chronic disease [35]. Instead of counseling patients about specific diets, it is more useful to focus on healthy eating.
In a retrospective review of 125 obese patients (who also met the criteria for metabolic syndrome) enrolled in a weight-loss program, a mean weight loss of 15% of initial body weight resulted in an average 19 mg/dL decrease in fasting glucose [36]. Weight reduction of as little as 5% body weight (often as little as 5 to 10 pounds) is associated with lower incidence of diabetes and related complications.
Reviewing and modifying diet is one of the most important steps in helping patients manage diabetes and, if indicated, lose weight. Strong evidence shows that eating patterns that are low in calorie density improve weight loss and weight maintenance and moderate evidence suggests that healthy eating patterns are associated with a reduced risk of T2DM in adults [37]. The U.S. Department of Agriculture Food Patterns and the Dietary Approaches to Stop Hypertension (DASH) Eating Plan are examples of eating patterns that are low in calorie density. In addition, patients with diabetes are advised to consume less sodium per day (less than 1,500 mg) than the maximum recommendation for healthy adults [37].
As a simple rule, to induce weight loss, patients' caloric intake should be reduced by 500–1,000 calories per day from the current level. This reduction will produce the recommended weight loss of one to two pounds per week in most patients [37].
Because of the complexities associated with diet-related behavior and because meal planning is so important to diabetes management, medical nutrition therapy provided by a registered dietitian is advocated [30,32,38]. Medical nutrition therapy is defined as nutritional diagnostic, therapy, and counseling services for the purposes of disease management, which are furnished by a registered dietitian or nutrition professional. Medical nutrition therapy, when provided by a registered dietitian, is reimbursed by the Medicare program [38,39]. Whenever possible, healthcare providers should be prepared to work with dieticians as part of an interdisciplinary diabetes care team. Frequently, however, access to a dietician is not feasible for patients whose healthcare plans do not cover this service or for those who live in remote geographic areas. In some settings, a nurse may assume responsibility for teaching dietary management to patients with diabetes.
The primary benefit of exercise to people with diabetes is that it has been found to increase glucose utilization by the tissues, thereby lowering blood glucose concentration [40]. In some people with T2DM, a regular program of physical activity can increase insulin sensitivity to the degree that medications can be reduced or discontinued. Because people with diabetes are at increased risk for heart disease, exercise has the added benefit of its favorable effect on cardiovascular status. The benefits of regular exercise to people with diabetes can be summarized as:
Improved insulin sensitivity
Reduction in body fat and weight
Reduction in incidence of cardiac disease
Improved lipid profile
Increase in high-density lipoproteins
Improved control of hypertension
Improved self-esteem
Reduced psychological stress
The ADA, along with other authorities, recommends at least 150 minutes of moderate intensity aerobic exercise per week [40,41]. (The ADA encourages 200 to 300 minutes of physical activity per week for long-term weight maintenance [30]). Adults with T2DM should engage in both aerobic and resistance training for optimal glycemic outcomes. Because reduction in insulin resistance from a single bout of exercise lasts for 24 to 72 hours afterward, there should be no more than two consecutive days between exercise sessions [40].
It is important to inform patients that assuming a more active lifestyle does not necessarily mean that they must adopt a structured exercise program. Experts advocate the benefits of incorporating moderate-intensity exercise into everyday activities. For example, making it a habit to use stairs instead of an elevator on a regular basis contributes to a more active lifestyle with cardiovascular benefits. Likewise, keeping active by doing such routine tasks as walking the dog, raking leaves, or washing the car can also be beneficial. It is suggested that, if done in increments lasting at least 10 minutes per session with an accumulation of 30 minutes or more per day, these types of activities can increase overall health and fitness [40,41].
Although physical activity can provide health benefits to a variety of patients, individuals with diabetes should be advised to seek a physician's approval before beginning an exercise program if they plan to engage in something more vigorous than brisk walking [40]. Several comorbidities associated with diabetes must be considered prior to recommending a more strenuous exercise program to ensure the program is safe and enjoyable. The role of routine stress testing before beginning an exercise program is controversial [40].
Patients who use insulin or sulfonylureas are at risk for hypoglycemia during or after exercise if proper adjustments are not made. Several factors influence the blood glucose response to exercise, including the timing, amount, and intensity of the exercise. Patients at risk for hypoglycemia are advised to carefully monitor their blood glucose before and after exercise to determine their response to a particular activity. Adjustments to medications and/or food intake can then be made prior to exercise based upon these findings.
Treatment of T2DM should be administered with the goal of conserving beta-cell function and mass, delaying disease progression, and preventing complications [2]. Due to the heterogenic nature of T2DM, treatment of this condition should not be approached with a "one-size-fits-all" mindset [32]. Instead, therapeutic selection should be individualized based on the patient's specific characteristics. A1c level is typically used to monitor long-term glycemic control and can help to indicate treatment inefficiency and guide therapeutic selection and adjustment [2]. Target A1c levels vary according to organization, but most recommend an A1c level of either ≤7% or ≤6.5%. (Further discussion of A1c targets is provided in the next section.) Although lifestyle modification, such as weight reduction and increased physical activity, continues to be the cornerstone of diabetes therapy, this approach may not sufficiently control A1c depending upon the extent of disease progression. When this is the case, a number of different pharmacotherapies can be used either alone or together to help patients achieve their target A1c level (Table 2) [30,31]. When selecting therapy, it is important to remember several points: duration of disease correlates with decreased beta-cell function, the desired degree of A1c decrease can help to guide therapeutic selection, and side effect profiles of T2DM medications vary substantially and should be incorporated into treatment decisions [2]. It is also important to consider the patient's preferred route of administration and any comorbid conditions (e.g., obesity, cardiovascular disease, depression, or osteoporosis) [2]. After these factors are assessed, treatment selection can more successfully address both treatment goals and patient preferences.
PROFILES OF ANTIDIABETIC MEDICATIONS
| Benefits/Risks | Medications | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| MET | GLP-1 RA | SGLT-2i | DPP-4i | AGi | TZD | SU/GLN | COLSVL | BCR-QR | Insulin | PRAML | |||
| Hypoglycemia | Neutral | Neutral | Neutral | Neutral | Neutral | Neutral |
| Neutral | Neutral | Moderate to severe | Neutral | ||
| Weight | Slight loss | Loss | Loss | Neutral | Neutral | Gain | Gain/Neutral | Neutral | Neutral | Gain | Loss | ||
| Renal adjustment |
Contraindicated if eGFR <30 mL/min/1.73m2 | Insufficient evidence | Check medication-specific eGFR thresholds | Dose adjustment necessary (except with linagliptin) | Not recommended | Neutral | Moderate to severe/Mild | Neutral | Neutral | Moderate to severe | Neutral | ||
| GI symptoms | Mild to Moderate | Moderate | Neutral | Neutral | Moderate | Neutral | Neutral | Mild | Moderate | Neutral | Moderate | ||
| CHF | Neutral | Unclear | Reduced risk | Moderate | Insufficient evidence | Possible increased risk/Neutral | Neutral | Neutral | Safe | Moderate | Insufficient evidence | ||
| ASCVD | Neutral | Safe | Possible benefitb | Neutral | Insufficient evidence | May reduce stroke risk | Neutral | Neutral | Safe | Possible benefit | Insufficient evidence | ||
Biguanides, specifically metformin, are the most widely used first-line T2DM medication. Both the AACE/ACE and the ADA/EASD recommend metformin as first-line therapy in most patients with T2DM, except where contraindicated [31,32]. Biguanides inhibit expression of hepatic gluconeogenic genes, thereby reducing fasting plasma glucose levels [2]. Metformin offers several benefits, including an oral route of administration (to be dosed once or twice daily) and a weight-neutral, non-hypoglycemia-inducing side-effect profile [32]. In addition, generic formulations of metformin are available, which may be preferred in patients who are unable to afford the cost of this agent due to high co-pays or lack of prescription insurance [2].
However, metformin is associated with gastrointestinal side effects and should be avoided in patients at risk for lactic acidosis (rare) [32]. Another drawback of metformin lies in its clearance through the kidneys. Historically, one of the most important risk factors for elevated metformin concentrations (leading to lactic acidosis) was the inability to clear the drug efficiently [42]. As a result, there was a long-standing FDA warning contraindicating metformin in men and women with serum creatinine concentrations ≥1.5 mg/dL and ≥1.4 mg/dL, respectively. However, in 2016, after a review of literature, the FDA removed this warning and labeling now indicates that metformin can be safely used in those with mild kidney function impairment and in some patients with moderate impairment [31,32,42,43]. Because this treatment is typically unable to maintain long-term glycemic control throughout the duration of the disease, additional therapy is typically necessary [2]. Metformin can be easily combined with other T2DM agents, including secretagogues, dipeptidyl peptidase-4 (DPP-4) inhibitors, thiazolidinediones (TZDs), GLP-1 agonists, and insulin. Additionally, there is ongoing acceptance that other approaches (e.g., GLP-1 agonists, sodium-glucose cotransporter 2 inhibitors [SGLT2i]) may be appropriate in the setting of ASCVD, CHF, and diabetic kidney disease [31; 32].
Secretagogues (meglitinides), one of the oldest classes of oral antidiabetic agents, work to stimulate insulin release through the closure of adenosine triphosphate-sensitive potassium channels on pancreatic beta cells [44]. Thus, they are most useful in cases where beta-cell function is still detectable [2]. Despite the fact that secretagogues quickly and effectively lower A1c, they are not considered a first-line treatment due to the short-term sustainability of this effect [2,32].
The various secretagogues have different profiles. Sulfonylureas are relatively long-acting secretagogues that can decrease both fasting plasma and postprandial glucose levels, whereas glinides are short-acting secretagogues that decrease postprandial glucose levels only [2]. These oral agents are intended to be taken with meals; the morning meal if dosed daily, or the morning and evening meals (or bedtime with food) for twice-daily dosing [2]. Both types of secretagogues are associated with modest weight gain and risk of hypoglycemia, although glinides may carry a lower risk of the latter [31]. In addition, some studies have suggested these agents may be associated with a secondary failure rate in excess of other T2DM drugs resulting from exacerbation of islet dysfunction [45]. The central benefit of secretagogues is cost. These agents have generic equivalents, and many are available in combination with other drugs, such as metformin or the TZD pioglitazone [2].
TZDs enhance glucose uptake in peripheral tissue, improving insulin sensitivity in skeletal muscle (thereby lowering both fasting plasma and postprandial glucose levels) and reducing hepatic glucose production [2,32]. The beneficial effects of TZDs on blood glucose levels appear to be more durable and longer lasting compared to metformin and the secretagogues [2]. This drug class has been found in clinical trials to reduce visceral adipose tissue and carotid intima-media thickness [2,46,47]. TZDs can worsen fluid retention and should not be used in persons with symptomatic heart failure [31]. It is important to note that TZDs require the presence of insulin (either endogenous or exogenous) for adequate glucose uptake into peripheral tissue, and beneficial effects are not typically observed until four to eight weeks of therapy [2]. Still, when used as a second-or third-line therapy, TZDs can be highly effective, especially when used early in the disease course and combined with other antidiabetic agents. Pioglitazone is now the only TZD that is approved for T2DM. In 2010, use of the TZD rosiglitazone was restricted by the FDA after studies linked the drug to increased risk of myocardial infarction [48,49]. The agency continued to monitor the drug's safety, and, in 2013, removed several of the prescribing and dispensing restrictions. In 2015, the FDA removed the final remaining restrictions placed on the use of rosiglitazone [50]. The weight gain that is associated with pioglitazone is counter-balanced by a low risk for hypoglycemia and an oral dosing scheme that does not necessarily require food [2]. Pioglitazone has also been associated with an increased risk for bladder cancer. Although this is still being studied, the FDA recommends that the use of pioglitazone be avoided in patients with active bladder cancer [48,51].
Because GLP-1 release in the gut has been found to play a key role in postprandial insulin secretion, GLP-1 agonists have been developed to help stimulate insulin and amylin secretion from pancreatic beta cells in a glucose-dependent fashion and suppress postprandial glucagon secretion, leading to decreased hepatic gluconeogenesis, slowed gastric emptying, and consequentially, increased satiety [2,32]. These agents provide 6 to 10 times more pharmacologic concentrations of GLP-1 than the endogenous hormone. The reduction in appetite caused by GLP-1 agonists offers an advantage of weight loss, which is modest in most cases but can be significant in some individuals [1,31]. However, use of this agent can be limited by nausea and vomiting, particularly during the early phase of treatment, as well as by its injectable route of administration and the potential for increased risk of pancreatitis [1,31].
There are long-acting (liraglutide, exenatide, dulaglutide, semaglutide) and short-acting (exenatide, lixisenatide) GLP-1 agonists. Long-acting agents can be dosed once weekly, while short-acting therapies require twice-daily administration with meals [2]. Long-acting GLP-1 agonists appear to help reduce triglyceride levels and free fatty acids, and short-acting GLP-1 agonist use has been associated with a reduced likelihood of cardiovascular events compared to other glucose-lowering agents [2]. These agents are not approved as first-line therapy but are effective in combination with other agents including metformin, pioglitazone, sulfonylureas, and basal insulin (although concomitant use with secretagogues or insulin may increase the risk of hypoglycemia) [2,48].
DPP-4 inhibitors (alogliptin, saxagliptin, linagliptin, sitagliptin) also target GLP-1 and the incretin effect. But unlike GLP-1 agonists, DPP-4 inhibitors restrict DPP-4 to prevent enzymatic inactivation of endogenous GLP-1, thereby prolonging the availability of endogenous GLP-1 and increasing GLP-1 concentrations in the gastrointestinal tract [2]. By inhibiting more than 80% of DPP-4 activity over a 24-hour period, these agents produce an estimated 1.5-to 4-fold increase in active postprandial GLP-1 levels, resulting in increased insulin and amylin secretion from beta cells and decreased glucagon secretion and liver glucose production [2]. DPP-4 inhibitors offer many benefits, including oral route of administration (with or without food), low hypoglycemia risk, a weight-neutral profile, and a potential cardiovascular benefit [2,31]. They are also associated with a lower incidence of nausea and vomiting compared to GLP-1 agonists. However, like TZDs, DPP-4 inhibitors require the presence of insulin (either endogenous or exogenous) for efficacy [2]. These second-or third-line drugs are often used in combination with other agents; they have been studied and are often used with metformin, pioglitazone, sulfonylureas, and basal insulin [2].
Canagliflozin, the first in the new class of diabetes medications referred to as sodium-glucose co-transporter 2 (SGLT2) inhibitors, was approved by the FDA in 2013, with dapagliflozin and empagliflozin approved in 2014, ertugliflozin approved in 2017, and bexagliflozin approved in 2023 [48,52,53,54]. This class acts by inhibiting SGLT2 in the proximal renal tubules, which reduces reabsorption of filtered glucose from the tubular lumen and lowers the renal threshold for glucose. SGLT2 is the main site of filtered glucose reabsorption, and reduction of filtered glucose reabsorption and lowering the renal threshold result in increased urinary excretion of glucose and improved plasma glucose concentrations. The recommended initial dose of canagliflozin is 100 mg once daily prior to the first meal of the day [48,52]. The dose may be increased up to 300 mg/day, unless the patient has impaired renal function. Dapagliflozin is dosed at 5 mg once daily in the morning and may be increased to 10 mg/day, while empagliflozin is started at 10 mg daily and may be increased to 25 mg per day, if necessary. Ertugliflozin is dosed at 5 mg once daily to a maximum of 15 mg daily [48,53,54]. The daily dose of bexagliflozin is 20 mg every morning [48]. These agents are approved for use with diet and exercise to improve the control of T2DM in adult patients. They have been studied for use as monotherapy and in combination with other antidiabetics, including metformin, sulfonylureas, pioglitazone, and insulin [52,53,54]. The most common side effects are vulvovaginal candidiasis and urinary tract infection.
An FDA safety review has resulted in new warnings to the labels of all SGLT2 inhibitors about the risks of ketoacidosis and serious urinary tract infections, which could result in hospitalization [55]. The review identified 73 cases of ketoacidosis in patients with type 1 or type 2 diabetes treated with SGLT2 inhibitors between March 2013 and May 2015. In addition, 19 cases of life-threatening blood and kidney infections that started as urinary tract infections were reported between March 2013 and October 2014. The FDA advises that patients should stop taking their SGLT2 inhibitor and seek immediate medical attention if any symptoms of ketoacidosis arise (e.g., dehydration, excessive thirst, excessive or frequent urination). The agency also recommends that healthcare providers assess for ketoacidosis and urinary tract infections in patients with suggestive symptoms, and discontinue the drug and institute treatment promptly if ketoacidosis is suspected [48,55]. In 2017, the FDA added a boxed warning to canagliflozin due to an increased risk of leg and foot amputation, as confirmed by data from two large clinical trials [56]. In 2018, the FDA issued a warning about rare but serious necrotizing fasciitis of the perineum associated with SGLT2 inhibitor therapy [57]. In 2020, with a revision published March 2022, the FDA approved changes to the prescribing information for SGLT2 inhibitors recommending that they be stopped temporarily before scheduled surgery [58]. Canagliflozin, dapagliflozin, empagliflozin, and bexagliflozin should each be stopped at least three days prior to surgery, and ertugliflozin should be stopped at least four days prior to surgery [48,58].
Amylin, or islet amyloid polypeptide, is co-secreted with insulin in the islets of Langerhans of patients with diabetes [59]. Amylin directly targets the brain and indirectly targets the gastrointestinal tract, pancreas, and liver to delay gastric emptying, induce satiety, and suppress postprandial glucagon secretion [2,48]. Pramlintide is an amylin analogue that works synergistically with insulin to decrease hepatic gluconeogenesis [2,48,59]. As an injectable monotherapy, this agent carries a low risk of hypoglycemia. It also imparts weight-loss and cardiovascular benefits [2]. Pramlintide is approved for use as an adjunct to bolus insulin therapy (with or without metformin or sulfonylureas) and is therefore typically used later in the disease course [48].
Dopamine agonists also work directly on the brain to increase dopamine levels, resulting in decreased hepatic glucose output and postprandial glucose levels [2]. Like amylin analogues, dopamine agonists are associated with weight loss and beneficial cardiovascular effects and have little association with hypoglycemia. They, too, are infrequently used as first-or second-line agents, as studies of these agents as combination therapy are limited.
AGIs work in the gastrointestinal tract to decrease postprandial excursions by delaying the absorption of carbohydrates [2]. Due to their side effects (primarily flatulence), these agents are infrequently used in the United States [2,31].
Exogenous insulin works much like endogenous insulin in that it causes cells in the liver, muscle, and fat tissue to take up glucose from the blood and store it as glycogen. Due to the progressive nature of T2DM, injectable or inhaled insulin therapy is typically required at some point in the disease course, with the goal of creating as normal a glycemic profile as possible without causing unacceptable weight gain or hypoglycemia [32]. Basal insulin is usually offered first when insulin therapy becomes necessary, as this approach offers relatively uniform insulin coverage over a 24-hour period, with peakless time-action curves producing a more consistent effect [31,32]. Intermediate-acting, long-acting, and insulin detemir formulations are available, with the latter two offering a slightly lower risk for overnight hypoglycemia and weight gain.
Due to progressive diminution of insulin secretory capacity, prandial insulin therapy with short-acting insulins is typically initiated eventually [31]. These types of insulin provide improved (and more affordable) postprandial glucose control but have more complicated pharmacokinetic profiles. At all times, insulin therapy should be tailored to an individual patient's prevailing glucose trends and dietary/exercise habits.
The ACE, the AACE, and the ADA have each provided guidelines for the step-wise selection of therapies for T2DM [30,31,32,33]. Lifestyle modification (e.g., healthy diet, weight control, increased physical activity) is recommended as a first step in glycemic control, although a consensus statement from the AACE/ACE states that lifestyle optimization efforts should not delay needed pharmacotherapy in higher risk individuals [31]. The AACE/ACE emphasize that minimizing risk of weight gain and promoting weight loss in patients with adiposity-based chronic disease should be a high priority [31].
Should pharmacotherapy become necessary, metformin should be the initial drug of choice, although an AACE/ACE algorithm denotes that TZDs, sulfonylureas, DPP-4 inhibitors, or GLP-1 agonists can be used alone or together for therapeutic initiation depending on the presenting A1c level and with consideration of other factors [31]. Two-or three-drug combinations with metformin plus other oral antidiabetes drugs are recommended when first-line therapy is deemed inadequate, with all organizations agreeing that insulin should be reserved for failure of triple combination therapy. To measure efficacy, all groups recommend regular assessment of A1c. Although target A1c levels vary slightly according to organization, all agree that elevated A1c indicates treatment inadequacy and warrants treatment escalation.
It has been well documented that poor glycemic control is associated with additional disease and economic burden. Uncontrolled blood glucose has been found to impose multiple care requirements, additional healthcare costs, and greater risk of disabling complications such as diabetic retinopathy, chronic kidney disease, and cardiovascular disease [32,60]. Likewise, reducing A1c levels has been shown to significantly reduce the risk for microvascular complications. Therefore, it seems reasonable T2DM outcomes should universally improve as A1c decreases. However, some evidence has shown that tight glycemic control, defined as A1c ≤6.5%, may impose additional risks compared to a more modest A1c level of <7.0% [61]. As a result, a divergence in recommended A1c targets has occurred in guideline recommendations, causing confusion and disagreement among providers who care for patients with T2DM.
The AACE recommends an A1c target level of ≤6.5% unless contraindicated by specific factors, such as age and hypoglycemia risk [31]. The AACE emphasizes that "the key word is 'safe' with consideration of patient-specific characteristics that would recommend a less stringent A1c target (e.g., 7% to 8%)" [31]. This goal is different than that set forth by the ADA and EASD, which recommend a target A1c of <7.0% [32]. In addition, in 2018, the ACP controversially recommended a target A1c of 7% to 8% for most patients with diabetes [62,63]. The recommendation for tight glycemic control by the AACE is based on data from numerous older trials. The Diabetes Control and Complications Trial, the Epidemiology of Diabetes Interventions and Complications Study, and the UKPDS trial data between 1993 and 2008 are supportive of an A1c target of ≤6.5%, as are findings from the 2000 Kumamoto Study and the Steno-2 trial by Gaede et al. [64,65,66,67,68,69,70,71,72]. Although some of these trials are relatively dated, further evidence was provided by three landmark trials: the Action to Control Cardiovascular Risk in Diabetes (ACCORD) study, the Action in Diabetes and Vascular disease (ADVANCE) trial, and the VA Diabetes Trial (VADT) [73,74,75]. In these studies, lower A1c levels correlated with reduced incidence of microvascular and sometimes macrovascular complications.
Of these studies, the ADVANCE trial provides a particularly strong rationale for tight glycemic control, as it was designed specifically to evaluate the effect of intensive glycemic control on death from cardiovascular disease, nonfatal myocardial infarction or nonfatal stroke, and new or progressing neuropathy or retinopathy [61,74]. More than 11,000 patients with T2DM were enrolled in this trial, with a median age of 67 years, a median duration of T2DM of 8 years, and a mean A1c of 7.5% upon study entry. Patients were required to have a history of major macrovascular or microvascular disease or at least one risk factor for macrovascular disease. Outcomes of this study revealed no adverse effects of intensive glycemic therapy (with an A1c target of ≤6.5%). In fact, tight glycemic control was associated with a non-significant trend toward lower cumulative mortality and a beneficial effect on macrovascular and microvascular complications (when assessed collectively) [61]. Both intensive and standard glycemic control groups also experienced improvements in blood pressure and low-density lipoprotein cholesterol levels.
These findings have been supported by other studies. A 2011 meta-analysis evaluated the effect of intensive glucose-lowering treatment on all-cause mortality, cardiovascular death, and microvascular events in T2DM [76]. In this meta-analysis, intensive therapy was associated with reductions in risk of non-fatal myocardial infarction and microalbuminuria, as well as a 9% reduction in all-cause mortality and a 14% reduction in cardiovascular death, causing authors to conclude that intensive glucose-lowering treatment demonstrated "limited benefit." In a 2010 meta-analysis assessing the impact of intensive versus standard glucose control on microvascular and macrovascular complications in both type 1 and type 2 diabetes in more than 30,000 patients, intensive glucose control was found to reduce the risk of developing microvascular complications, including retinopathy, nephropathy, and neuropathy, by 25% to 76% [77]. Moreover, intensive control was associated with a 10% to 15% decrease in nonfatal myocardial infarction, particularly in patients with T2DM. Similar results were demonstrated in a separate 2010 meta-analysis studying the effect of intensive glucose control on all-cause and cardiovascular mortality, myocardial infarction, and stroke in T2DM [78]. In this analysis of six reports from four randomized trials including more than 27,000 patients, intensive glucose control (mean A1c: 6.6%) was associated with a 14% reduction in non-fatal myocardial infarction, but it did not affect mortality or the risk for non-fatal stroke. Although two of the studies noted a significantly increased risk of hypoglycemia in intensive glycemic control groups, none concluded that this risk definitively outweighed the benefits of this strategy to lower A1c target [76,77].
Alternatively, some data challenge the importance of tight glycemic control in T2DM. In the VADT study, no beneficial effect of intensive glycemic control was observed when the entire study population was taken into consideration [61]. In fact, a deleterious effect was observed in association with tight glycemic control in patients who had T2DM for 15 years or more. This is suggestive of a potential "window of opportunity" early in the disease course for intensive control that closes over time [61]. Moreover, in the ACCORD study, the intensively treated group experienced a number of negative effects, including a three-fold increased risk of hypoglycemia and severe hypoglycemia and excessive weight gain—a well-known risk factor for increased mortality [61]. However, it is important to note that in the ACCORD trial, a 1.4% reduction in A1c was achieved within four months in the intensive control group [61]. The more gradual reduction in A1c observed in the ADVANCE trial may have influenced the apparent beneficial effect of intensive glycemic control on outcomes [61]. Still, in the ADVANCE trial, much like in the ACCORD study, excessive weight gain (and associated morbidity and mortality) was positively correlated with intensive glycemic control. Likewise, in a 2011 meta-analysis of 14 clinical trials involving approximately 28,600 patients with T2DM, intensive glycemic control did not appear to significantly impact the relative risk of all-cause or cardiovascular mortality, and study authors were unable to find sufficient evidence for the beneficial effect of intensive control on microvascular outcomes [79]. Given the severe risk of hypoglycemia that was found to accompany intensive glycemic control (with a 30% increased relative risk), authors concluded that intensive glycemic control does not appear to reduce all-cause mortality and that data fail to clearly demonstrate a benefit on cardiovascular mortality, non-fatal myocardial infarction, or microvascular complications. Other questions remain regarding the benefit of intensive glycemic control in T2DM, including duration of follow-up required to demonstrate beneficial effects, extent of influence glycemic control has on outcomes (given the numerous risk factors in T2DM), and extent of influence glycemic control has on pre-existing macrovascular outcomes [61].
A review of the literature on the impact of tight glycemic control in patients with T2DM, which included systematic reviews, meta-analyses of contemporary randomized trials, and guidelines, found no significant impact of tight glycemic control on the risk of dialysis/transplantation/renal death, blindness, or neuropathy and no significant effect on all-cause mortality, cardiovascular mortality, or stroke. The authors did find a consistent 15% relative-risk reduction of nonfatal myocardial infarction. Between 2006 and 2008, most statements (47% to 83%) endorsed the benefit of tight glycemic control. After 2008 (ACCORD), only a minority (21% to 36%) did [80].
Based on these data, it appears that although tight glycemic control may have a beneficial effect on microvascular outcomes and mortality, the risk for hypoglycemia and weight gain that accompany this therapeutic approach might detract from the appeal of this strategy. While most experts concede that the evidence is currently inconclusive, future studies are anticipated to shed further light on this subject. In the interim, it is important that physicians weigh the risks and benefits of intensive glycemic control when setting A1c targets in their patients.
Patient age must also be considered when assessing the risks and benefits of intensive glycemic control. Hypoglycemia (especially severe hypoglycemia) poses a considerable risk to elderly patients [81]. The hypothesized benefit of intensive glycemic control in this population stems from improved cardiovascular outcomes. However, the ACCORD, ADVANCE, and VADT trials failed to demonstrate a positive correlation between intensive glucose control and reduced cardiovascular events [82]. In fact, the ACCORD study found that intensive glucose control was associated with an increased risk for cardiovascular and all-cause mortality in certain cases [82]. On the other hand, a 10-year follow-up of the tight glucose intervention arm of the UKPDS study demonstrated reduced risk for myocardial infarction, diabetes-related death, and all-cause mortality, indicating a long-term benefit of intensive glycemic control that eventually translates into a protective cardiovascular effect. These findings suggest that intensive control may provide a cardiovascular benefit if initiated early in the disease course, but not in elderly patients with advanced T2DM [81,82]. Despite the prospective cardiovascular benefits of an A1c level ≤6.5%, achieving reduced A1c levels without exposing elderly patients to increased hypoglycemia-related risk is challenging. It is therefore critical that A1c targets be individualized in this patient population so reduced A1c is not achieved at the expense of overall patient health. Medical, psychological, functional (i.e., self-management abilities), and social domains should be assessed in this patient population to determine appropriate treatment targets and therapeutic approaches. Elderly patients also should be screened for polypharmacy, cognitive impairment, depression, urinary incontinence, fall risk, persistent pain, and frailty as these may affect diabetes self-management and diminish quality of life [30]. Factors that favor more stringent glycemic goals include [30]:
Short diabetes duration
Low hypoglycemia risk
Low treatment risks and burdens
Pharmacotherapy with cardiovascular, kidney, weight, and other benefits
No cardiovascular complications
Few or minor comorbidities
Conversely, factors that favor less stringent glycemic goals include [30]:
Long diabetes duration
High hypoglycemia risk
High treatment risks and burdens
Pharmacotherapy without nonglycemic benefits
Established cardiovascular complications
Severe, life-limiting comorbidities
As with many chronic diseases, medication adherence is a significant barrier to optimal outcomes in T2DM. Adequate adherence to T2DM therapies, which is typically defined as collecting and/or taking >80% of prescribed medication, appears to vary significantly, although the vast majority of studies on this topic report some level of nonadherence among most patients with T2DM. An estimated 36% to 93% of individuals with T2DM are believed to practice inadequate adherence to oral antidiabetic agents, a considerably broad percentage [83]. Insulin nonadherence is similarly indefinite, reported to affect between 19% and 46% of patients with T2DM [84,85]. Paradoxically, anticipated patient nonadherence actually dissuades a significant number of providers from initiating insulin [86]. Research suggests that nonadherence is a relatively immediate response in many patients with T2DM. Rather than tapering off medication over a substantial period of time, evidence suggests that patients often fail to fill second or additional prescriptions, and many discontinue medication within a year of prescription, actions suggestive of causative factors beyond simple medication fatigue [87]. The consequences of medication nonadherence are significant, ultimately resulting in hundreds of billions of dollars in additional economic cost and increased risk of mortality among nonadherent individuals compared to adherent patients with T2DM [85,88,89]. To reduce the personal and societal burden of nonadherence to antidiabetes medication, it is important that healthcare professionals understand the factors that contribute to suboptimal compliance, as well as strategies to overcome these barriers (Table 3).
STRATEGIES FOR OVERCOMING BARRIERS TO MEDICATION ADHERENCE IN T2DM
| Barrier | Strategy | ||||
|---|---|---|---|---|---|
| Oral and Non-Insulin Therapies | |||||
| Fear of side effects |
| ||||
| Treatment complexity |
| ||||
| Insulin Therapy | |||||
| Fear of side effects |
| ||||
| Needle anxiety/treatment complexity |
| ||||
| Negative patient attitude |
| ||||
| Other Barriers | |||||
| Medication cost | Work with managed care programs and patient financial profile to ensure easy access to medication. | ||||
| Clinical inertia | Improve patient-provider communication to obtain feedback on adherence. | ||||
Depression and diabetes distress are prevalent in persons with T2DM and can result in nonadherence to medication regimens. Potential formal tools to screen for depression include the WHO Well-being Index, the Patient Health Questionaire-9 (PHQ-9), or the Beck Depression Inventory [31,90,91,92]. Appropriate referral for cognitive-behavioral therapy or medical intervention should be considered when depression is present.
The challenges associated with adherence to all T2DM therapies, including oral and non-insulin therapies, are multifactorial and complex, exponentially increasing the level of difficulty many patients have in overcoming these obstacles. Among the numerous reasons for reduced adherence to T2DM medication, the most frequently reported include fear of side effects (especially weight gain, hypoglycemia, and injection site reactions), inconvenience or complexity of prescribed treatment regimens, cost-associated access challenges, and low levels of patient knowledge and education regarding the importance of therapies for glycemic control [89,93]. It is important to note that hypoglycemia, a side effect that is experienced by 38% of those receiving combination oral antidiabetic therapy, is a significant risk factor for suboptimal adherence and negatively affects patient perceptions of treatment efficacy, convenience, and safety [93,94]. Effectively balancing therapeutic efficacy with tolerability is one action that can greatly increase the likelihood for treatment adherence, although it not an achievement that is easily obtained. The use of newer medications can help to reduce the impact of side effects, such as prescribing GLP-1 agonists in patients who are concerned with weight gain. Taking steps that swiftly and effectively correct hypoglycemic events can also help to improve both treatment adherence and glycemic control. To address treatment complexity, oral fixed-dose combination therapy can reduce the number of pills to be taken in any given day, thereby improving adherence. Studies have found that switching from multiple, individual oral therapies (often referred to as "loose-pill combinations") to fixed-dose combinations can significantly increase adherence [93,95,96,97]. Likewise, reducing the frequency of dosing (e.g., from twice-daily to once-daily regimens) has been found to increase adherence by as much as 19% [93,98]. Beyond these measures, taking steps to ensure that a patient's individual concerns and preferences are addressed and educating patients regarding the consequences of hyperglycemia and the importance of glycemic control can further optimize adherence [93].
Many of the barriers to insulin adherence are similar to those of oral medications, including side effect concerns and inconvenient dosing schedule, which can be overcome utilizing the previously discussed recommendations [99]. However, insulin therapy is accompanied by additional factors that can reduce adherence, such as needle anxiety and negative patient perceptions. Many patients associate insulin therapy with poor prognosis or as a form of punishment for inadequate self-management [89,99].
A number of steps can be taken to improve adherence to insulin therapy. Numerous developments have addressed patients' concerns regarding needles. Needles are now smaller and narrower, reducing the fear and pain associated with injections, and pen devices can improve convenience, dosing accuracy, and dosing discretion [99]. In fact, studies have found that pen devices significantly improve medication adherence compared to syringes [99,100,101].
Newer formulations of insulin offer variations in characteristics, such as onset of effect, peak effect, and duration of effect. These formulations provide patients with a more customized therapeutic strategy that can better meet their physiologic needs [99]. Also, fixed-dose, premixed insulins that combine a long- and short-acting insulin can be considered for patients with concerns about multiple insulins and injections. Although premixed insulin requires fewer injections, it also has less flexibility for dosing adjustments and may increase hypoglycemia [31]. Nonetheless, premixed insulin may offer an alternative to achieve adequate glycemic control due to simplicity of the insulin regimen and increased adherence [31]. Finally, providing adequate patient education on the importance of insulin and dispelling misguided beliefs that insulin therapy is a form of punishment or an indication of self-management failure can improve psychological responses to insulin and increase the likelihood of adherence.
Additional factors have been found to affect adherence, regardless of therapeutic selection. Increased medication cost is one factor that has been correlated with nonadherence in T2DM. One study found that for each $5 increase in patient cost, the adjusted odds of being adherent decrease by 15% [102]. Working with patients to reduce costs through utilization of managed care and other programs designed to limit patient spending can help to overcome this barrier.
Clinical inertia is another phenomenon that has been attributed to high rates of nonadherence to T2DM medications. Clinical inertia is characterized by recognition of a problem paired with failure to take corrective action and contributes to nonadherence when physicians acknowledge their patients are not adhering to their prescribed T2DM regimen and achieving glycemic control, but take no steps to correct the problem [103]. Improving provider-patient communication is a critical step in interrupting clinical inertia and improving adherence [104]. Research suggests that patient-provider communication in T2DM is largely inadequate, with physicians tending to misinterpret patients' needs and patients often wishing for more active involvement, information, and access to their physicians [105]. Good communication involves determining the patient's attitudes and beliefs to ascertain what education is needed. To obtain feedback on adherence, clinicians must be able to work within cultural attitudes and modify language to meet the health literacy level of the patient. Optimal patient-provider communication can help to alleviate patient concerns, set achievable goals, and improve overall patient satisfaction. Some communication behaviors that have been found to be positively associated with health outcomes include empathy, reassurance and support, explanations, positive reinforcement, humor, discussion of psychosocial issues, health education and information sharing, courtesy, and summarization and clarification [106]. Salient patient factors affecting medication adherence include the patient's level of self-efficacy, their belief in medications as helpful, perceived barriers to consistent medication use, and strong patient-provider communication [107]. Factors essential for effective communication and a successful relationship are knowledge of the patient's language preference; an understanding of and respect for the patient's personal cultural values, beliefs, and practices (referred to as cultural competency); and an awareness of the patient's health literacy level [108,109,110].
Language, cultural competency, and health literacy are significant issues, given the growing percentages of racial/ethnic populations. According to U.S. Census Bureau data from 2023, more than 68 million Americans speak a language other than English at home, with more than 26.2 million (8.4% of the population) reporting that they speak English less than "very well" [111]. Clinicians should ask their patients what language they prefer for their medical care information, as some individuals prefer their native language even though they have said they can understand and discuss symptoms in English [112].
The national standards on Culturally and Linguistically Appropriate Services (CLAS) include four behaviors related to language access services that are mandated for healthcare organizations [108]. Although they are not mandated for individual healthcare providers, the Office of Minority Health encourages clinicians to meet the standards to make their practices more culturally and linguistically accessible. These standards are [108]:
Offering and providing language assistance services, including bilingual staff and interpreter services, at no cost to each patient/consumer with limited English proficiency at all points of contact in a timely manner during all hours of operation
Providing patients with both verbal offers and written notices (in their preferred language) that inform them of their right to receive language assistance services
Ensuring the competence of language assistance provided to patients with limited English proficiency by interpreters and bilingual staff and avoiding the use of the patient's family and friends as interpreters
Making easily understood patient-related materials available and posting signage in the languages of the commonly encountered groups and/or groups represented in the practice area
In addition to the CLAS standards, Healthy People 2030 addresses health literacy as a social determinant of health and, as such, has identified four objectives to improve the health literacy of Americans [113].
Convenience and cost lead many clinicians to use "ad hoc" interpreters (e.g., family members, friends, bilingual staff members) instead of professional interpreters. However, professional interpreters are preferred for several reasons. Several states have laws about who can interpret medical information for a patient, so healthcare professionals should check with their state's health officials about the use of ad hoc interpreters [114]. Even when allowed by law, the use of a patient's family member or friend as an interpreter should be avoided, as the patient may not be as forthcoming with information and the family member or friend may not remain objective [114]. Children should especially be avoided as interpreters, as their understanding of medical language is limited and they may filter information to protect their parents or other adult family members [114]. Individuals with limited English language skills have actually indicated a preference for professional interpreters rather than family members [115].
Most important, perhaps, is the fact that clinical consequences are more likely with ad hoc interpreters than with professional interpreters [116]. A systematic review of the literature showed that the use of professional interpreters facilitates a broader understanding and leads to better clinical care than the use of ad hoc interpreters, and many studies have demonstrated that the lack of an interpreter for patients with limited English proficiency compromises the quality of care. The use of professional interpreters improves communication (errors and comprehension), utilization, clinical outcomes, and patient satisfaction with care [117,118].
Cultural competency is essential for addressing healthcare disparities among minority groups [108]. Among the issues that clinicians should understand are the patients' belief systems regarding health, healing, and wellness; their perceptions on illness, disease, and their causes; their health behaviors and attitudes toward healthcare providers; and the role of the family in decision making [108,119]. Understanding these aspects is integral to a successful patient-clinician relationship as well as to optimal health outcomes. For example, healthcare professionals should raise the topic of health-related customs, such as the use of complementary and alternative medicines, as the use of these therapies varies substantially among racial/ethnic populations, may compromise the effect of traditional therapies, and is often not disclosed by the patient [120,121,122].
Knowledge of the patient's health literacy is also important, as the patient's understanding of his or her disease and its management is essential to ensuring adherence to the treatment plan and the patient's role in self-management. Yet most individuals lack adequate health literacy. According to the National Assessment of Health Literacy, 14% of individuals in the United States have "below basic" health literacy, which means they lack the ability to understand health information and make informed health decisions [123,124]. According to the Center for Health Care Strategies (CHCS), a Medicaid partner, nearly 9 out of 10 adults in the United States struggle with health literacy [125]. A systematic review of more than 300 studies showed that an estimated 26% of patients had inadequate literacy and an additional 20% had marginal literacy [126]. Health literacy varies widely according to race/ethnicity, level of education, and gender, and clinicians are often unaware of the literacy level of their patients [110,127]. Predictors of limited health literacy are poor self-rated reading ability, low level of education, male sex, and non-White race [127,128]. Several instruments are available to test patients' literacy levels, and they vary in the amount of time needed to administer and in their reliability in identifying low literacy [110,123,127,129]. Healthcare organizations should assume that even strong readers can have difficulty understanding healthcare information and navigating the healthcare environment. Providers can informally identify patients who have limited health literacy by assessing whether the patient frequently misses appointments, fails to complete or accurately complete registration forms, identifies medications by their appearance rather than by reading the label, or avoids follow-up regarding tests or referrals [130].
Clinicians should adapt their discussions and educational resources to a patient's identified health literacy level and degree of language proficiency. The use of plain language (free of medical jargon), asking patients to repeat pertinent information, regularly assessing recall and comprehension, providing educational resources in a variety of formats (e.g., print, oral, web-based, video), and using culturally appropriate and translated educational materials can all help ensure that patients better understand their disease and its management, ultimately leading to higher quality care.
An excellent patient-provider relationship can also set a framework of ongoing support, which is critical for any chronic, long-term condition. Modern technology is starting to be incorporated into adherence improvement strategies. Studies of short message service and real-time medication monitoring suggest these strategies may be useful for improving adherence to T2DM medication, and Internet self-management programs hold great promise for assisting patients in all aspects of diabetes care, including medication adherence [131,132,133]. It is likely that strategies will be developed in the near future that successfully merge technology and health care for improved adherence in T2DM.
T2DM represents a growing healthcare crisis on a national and worldwide scale. As the population increases, including growing subpopulations of obese and elderly individuals, T2DM is anticipated to endure as one of the top causes of morbidity and mortality in the United States. Fortunately, novel agents, formulations, and devices have been developed that can help patients reach A1c goals with less negative impact on quality of life, although balancing patient needs, glycemic targets, and unwanted side effects is still considered to be difficult by many healthcare professionals. Significant barriers in T2DM remain. Research has yet to determine the optimal A1c target that should be assigned to most patients with T2DM, and low levels of therapeutic adherence continue to counteract treatment efficacy. Still, as knowledge and technology advance, there is the potential these obstacles will be overcome and outcomes in T2DM will be vastly improved.
1. Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2021. Available at https://www.cdc.gov/diabetes/php/data-research/index.html. Last accessed February 11, 2025.
2. Cornell S, Dorsey VJ. Diabetes pharmacotherapy in 2012: considerations in medication selection. Postgrad Med. 2012;124(4):84-94.
3. Centers for Disease Control and Prevention. Diabetes Report Card 2021. Available at https://www.cdc.gov/diabetes/communication-resources/diabetes-statistics.html. Last accessed February 11, 2025.
4. Grandy S, Fox DM. Change in health status (EQ-5D) over 5 years among individuals with and without type 2 diabetes mellitus in the SHIELD longitudinal study. Health Qual Life Outcomes. 2012;10(1):99.
5. Rowley WR, Bezold C, Arikan Y, et al. Diabetes 2030: insights from yesterday, today, and future trends. Popul Health Manag. 2017;20(1):6-12.
6. Gregg EW, Cheng YJ, Narayan KM, Thompson TJ, Williamson DF. The relative contributions of different levels of overweight and obesity to the increased prevalence of diabetes in the United States: 1976–2004. Prev Med. 2007;45(5):348-352.
7. Centers for Disease Control and Prevention, United States Diabetes Surveillance System. Diagnosed Diabetes: Total, Adults Aged 18+ Years, Age-Adjusted Percentage, National. Available at https://gis.cdc.gov/grasp/diabetes/diabetesatlas-surveillance.html. Last accessed February 11, 2025.
8. Boyle JP, Thompson TJ, Gregg EW, Barker LE, Williamson DF. Projection of the year 2050 burden of diabetes in the U.S. adult population: dynamic modeling of incidence, mortality, and prediabetes prevalence. Popul Health Metr. 2010;8:29.
9. Lin J, Thompson TJ, Chnge YJ, et al. Projection of the future diabetes burden in the United States through 2060. Popul Health Metr. 2018;16:9.
10. Danaei G, Finucane MM, Lu Y, et al. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 27 million participants. Lancet. 2011;378(9785):31-40.
11. Mokdad AH, Ford ES, Bowman BA, et al. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA. 2003;289(1):76-79.
12. National Center for Health Statistics. Prevalence of Overweight, Obesity, and Severe Obesity Among Adults Aged 20 and Over: United States, Trends 1960–1962 Through 2017-2018. Available at https://www.cdc.gov/nchs/data/hestat/obesity-adult-17-18/obesity-adult.htm#. Last accessed February 11, 2025.
13. Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in obesity among adults in the United States, 2005 to 2014. JAMA. 2016;315(21):2284-2291.
14. Drab SR. Recognizing the rising impact of diabetes in seniors and implications for its management. Consult Pharm. 2009;24(Suppl B):5-10.
15. Koopman RJ, Mainous AG 3rd, Diaz VA, Geesey ME. Changes in age at diagnosis of type 2 diabetes mellitus in the United States, 1988 to 2000. Ann Fam Med. 2005;3(1):60-63.
16. Freeman JS. A physiologic and pharmacological basis for implementation of incretin hormones in the treatment of type 2 diabetes mellitus. Mayo Clin Proc. 2010;85(Suppl 12):S5-S14.
17. Hussain I. Pathogenesis. In: Meneghini LF (ed). Medical Management of Type 2 Diabetes. 8th ed. Alexandria, VA: American Diabetes Association: 2020: 29-48.
18. Sears B, Perry M. The role of fatty acids in insulin resistance. Lipids Health Dis. 2015;14:121.
19. Campbell RK. Fate of the beta-cell in the pathophysiology of type 2 diabetes. J Am Pharm Assoc. 2009;49(Suppl 1):S10-S15.
20. Vimaleswaran KS, Loos RJ. Progress in the genetics of common obesity and type 2 diabetes. Expert Rev Mol Med. 2010;12:e7.
21. Kreienkamp RJ, Voight BF, Gloyn AL, et al. Genetics of type 2 diabetes. In: Lawrence JM, Casagrande SS, Herman WH, et al. (eds). Diabetes in America [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK); 2023.
22. Triplitt C. Examining the mechanisms of glucose regulation. Am J Manag Care. 2012;18(1 Suppl):S4-S10.
23. Karaca M, Magnan C, Kargar C. Functional pancreatic beta-cell mass: involvement in type 2 diabetes and therapeutic intervention. Diabetes Metab. 2009;35(2):77-84.
24. Wajchenberg BL. Beta-cell failure in diabetes and preservation by clinical treatment. Endocr Rev. 2007;28(2):187-218.
25. Holst JJ, Vilsbøll T, Deacon CF. The incretin system and its role in type 2 diabetes mellitus. Mol Cell Endocrinol. 2009;297(1-2):127-136.
26. Home PD, Pacini G. Hepatic dysfunction and insulin insensitivity in type 2 diabetes mellitus: a critical target for insulin-sensitizing agents. Diabetes Obes Metab. 2008;10(9):699-718.
27. Capurso C, Capurso A. From excess adiposity to insulin resistance: the role of free fatty acids. Vascul Pharmacol. 2012;57(2-4):91-97.
28. Wang TJ, Larson MG, Vasan RS, et al. Metabolite profiles and the risk of developing diabetes. Nat Med. 2011;17(4):448-453.
29. Zhu H, Bai M Xie X, et al. Impaired amino acid metabolism and its correlation with diabetic kidney disease progression in type 2 diabetes mellitus. Nutrients. 2022;14(16):3345.
30. American Diabetes Association. Standards of medical care in diabetes—2025. Diabetes Care. 2025;48(Suppl 1):S1-S344.
31. Samson SL, Vellanki P, Blonde L, et al. American Association of Clinical Endocrinology consensus statement: comprehensive type 2 diabetes management algorithm—2023 update. Endocr Pract. 2023;29(5):305-340.
32. Davies MJ, Aroda VR, Collins BS, et al. Management of hyperglycemia in type 2 diabetes, 2022: a consensus report by the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2022;45(11):2753-2786.
33. AACE Task Force for Developing a Diabetes Comprehensive Care Plan Writing Committee. American Association of Clinical Endocrinologists and American College of Endocrinology—American Association of Clinical Endrocrinology clinical practice guideline: developing a diabetes mellitus comprehensive care plan – 2022 update. Endocr Pract. 2022;28(10):923-1049.
34. Qaseem A, Barry MJ, Humphrey LL, Forciea MA. Oral pharmacologic treatment of type 2 diabetes mellitus: a clinical practice guideline update from the American College of Physicians. Ann Intern Med. 2017;166(4):279-290.
35. U.S. Preventive Services Task Force. Behavioral counseling in primary care to promote a healthy diet: recommendations and rationale. Am J Prev Med. 2003;24(1):93-100.
36. Case CC, Jones PH, Nelson K, O'Brian Smith E, Ballantyne CM. Impact of weight loss on the metabolic syndrome. Diabetes Obes Metab. 2002;4(6):407-414.
37. U.S. Department of Health and Human Services and Department of Agriculture. Dietary Guidelines for Americans, 2020-2025. 9th ed. Washington, DC: U.S. Department of Health and Human Services; 2020.
38. Morris SF, Wylie-Rosett J. Medical nutrition therapy: a key to diabetes management and prevention. Clinical Diabetes. 2010;28(1):12-18.
39. Medicare. Your Medicare Coverage: Nutrition Therapy Services. Available at https://www.medicare.gov/coverage/nutrition-therapy-services. Last accessed February 11, 2025.
40. Colberg SR, Sigal RJ, Yardley JE, et al. Physical activity/exercise and type 2 diabetes: a position statement of the American Diabetes Association. Diabetes Care. 2016;39(11):2065-2079.
41. Haskell WL, Lee IM, Pate RR, et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med Sci Sports Exerc. 2007;39(8):1423-1434.
42. Lipska KJ, Bailey CJ, Inzucchi SE. Use of metformin in the setting of mild-to-moderate renal insufficiency. Diabetes Care. 2011;34(6):1431-1437.
43. U.S. Food and Drug Administration. FDA Revises Warnings Regarding Use of the Diabetes Medicine Metformin in Certain Patients with Reduced Kidney Function. Available at https://www.fda.gov/media/96771/download. Last accessed February 11, 2025.
44. Rodbard HW, Jellinger PS, Davidson JA, et al. Statement by an American Association of Clinical Endocrinologists/American College of Endocrinology consensus panel on type 2 diabetes mellitus: an algorithm for glycemic control. Endocr Pract. 2009;15(6):540-559.
45. Pelligra A, Mrugala J, Griess K, et al. Pancreatic islet protection at the expense of secretory function involves serine-linked mitochondrial one-carbon metabolism. Cell Rep. 2023;42(6):112615.
46. Dormandy J, Charbonnel B, Eckland D, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive study (PROspective pioglitAzone Clinical Trial In macroVascular Events): a randomized controlled trial. Lancet. 2005;366(9493):1279-1289.
47. Mazzone T, Meyer PM, Feinstein SB, et al. Effect of pioglitazone compared with glimepiride on carotid intima-media cardiovascular system thickness in type 2 diabetes: a randomized trial. JAMA. 2006;296(21):2572-2581.
48. Lexicomp Online. Available at https://online.lexi.com/lco/action/login. Last accessed February 11, 2025.
49. Nissen SE, Wolski K. Rosiglitazone revisited: an updated meta-analysis of risk for myocardial infarction and cardiovascular mortality. Arch Intern Med. 2012;170(14):1191-1201.
50. Tucker ME. FDA Lifts Final Regulatory Restrictions on Rosiglitazone. Available at https://www.medscape.com/viewarticle/856056. Last accessed February 11, 2025.
51. Lewis JD, Ferrara A, Peng T, et al. Risk of bladder cancer among diabetic patients treated with pioglitazone: interim report of a longitudinal cohort study. Diabetes Care. 2011;34(4):916-922.
52. U.S. Food and Drug Administration. FDA Approves Invokana to Treat Type 2 Diabetes. Available at https://wayback.archive-it.org/7993/20170112023858/http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm345848.htm. Last accessed February 11, 2025.
53. U.S. Food and Drug Administration. FDA Approves Farxiga to Treat Type 2 Diabetes. Available at https://wayback.archive-it.org/7993/20170112023850/http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm380829.htm. Last accessed February 11, 2025.
54. U.S. Food and Drug Administration. FDA Approves Jardiance to Reduce Cardiovascular Death in Adults With Type 2 Diabetes. Available at https://www.fda.gov/news-events/press-announcements/fda-approves-jardiance-reduce-cardiovascular-death-adults-type-2-diabetes. Last accessed February 11, 2025.
55. U.S. Food and Drug Administration. SGLT2 Inhibitors: Drug Safety Communication – FDA Revises Labels of SGLT2 Inhibitors for Diabetes to Include Warnings About Too Much Acid in the Blood and Serious Urinary Tract Infections. Available at https://www.fda.gov/drugs/drug-safety-and-availability/fda-revises-labels-sglt2-inhibitors-diabetes-include-warnings-about-too-much-acid-blood-and-serious. Last accessed February 11, 2025.
56. U.S. Food and Drug Administration. FDA Confirms Increased Risk of Leg and Foot Amputations with the Diabetes Medicine Canagliflozin (Invokana, Invokamet, Invokamet XR). Available at https://www.fda.gov/media/104870/download. Last accessed February 11, 2025.
57. U.S. Food and Drug Administration. FDA Warns about Rare Occurrences of a Serious Infection of the Genital Area with SGLT2 Inhibitors for Diabetes. Available at https://www.fda.gov/drugs/drug-safety-and-availability/fda-warns-about-rare-occurrences-serious-infection-genital-area-sglt2-inhibitors-diabetes. Last accessed February 11, 2025.
58. U.S. Food and Drug Administration. Drug Safety Communication: FDA Revises Labels of SGLT2 Inhibitors for Diabetes to Include Warnings About Too Much Acid in the Blood and Serious Urinary Tract Infections: 3-19-2020 Update; Revised 3-15-2022. Available at https://www.fda.gov/drugs/drug-safety-and-availability/fda-revises-labels-sglt2-inhibitors-diabetes-include-warnings-about-too-much-acid-blood-and-serious. Last accessed February 11, 2025.
59. Adeghate E, Kalász H. Amylin analogues in the treatment of diabetes mellitus: medicinal chemistry and structural basis of its function. Open Med Chem J. 2011;5(Suppl 2):78-81.
60. Ali MK, McKeever Bullard K, Imperatore G, Barker L, Gregg EW. Characteristics associated with poor glycemic control among adults with self-reported diagnosed diabetes—National Health and Nutrition Examination Survey, United States, 2007–2010. MMWR. 2012;61(2):32-37.
61. Rodbard HW, Trence DL, Mechanick JI. Should the recommendation of the American Association of Clinical Endocrinologists for a hemoglobin A1c target of 6.5% be modified? A critical reappraisal of recent studies of intensive glycemic control. Endocr Pract. 2008;14(6):791-795.
62. Qaseem A, Wilt TJ, Kansagara D, et al. Hemoglobin A1c targets for glycemic control with pharmacologic therapy for nonpregnant adults with type 2 diabetes mellitus: a guidance statement update from the American College of Physicians. Ann Intern Med. 2018;168(8):569-576.
63. PR Newswire. American Diabetes Association® Deeply Concerned About New Guidance from American College of Physicians Regarding Blood Glucose Targets for People with Type 2 Diabetes. Available at https://www.prnewswire.com/news-releases/american-diabetes-association-deeply-concerned-about-new-guidance-from-american-college-of-physicians-regarding-blood-glucose-targets-for-people-with-type-2-diabetes-300611159.html. Last accessed February 11, 2025.
64. Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329(14):977-986.
65. Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications Research Group. Retinopathy and nephropathy in patients with type 1 diabetes four years after a trial of intensive therapy. N Engl J Med. 2000;342(6):381-389.
66. Nathan DM, Cleary PA, Backlund JY, et al. Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes.N Engl J Med. 2005;353(25):2643-2653.
67. Nathan DM, Lachin J, Cleary P, et al. Intensive diabetes therapy and carotid intima-media thickness in type 1 diabetes mellitus. N Engl J Med. 2003;348(23):224-303.
68. United Kingdom Prospective Diabetes Study Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352(9131):837-853.
69. Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405-412.
70. Shichiri M, Kishikawa H, Ohkubo Y, Wake N. Long-term results of the Kumamoto Study on optimal diabetes control in type 2 diabetic patients. Diabetes Care. 2000;23(Suppl 2):B21-B29.
71. Gaede P, Vedol P, Larsen N, Jensen GV, Parving HH, Pedersen O. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Engl J Med. 2003;348(5):383-393.
72. Gaede P, Lund-Andersen H, Parving HH, Pedersen O. Effect of a multifactorial intervention on mortality in type 2 diabetes. N Engl J Med. 2008;358(6):580-591.
73. Action to Control Cardiovascular Risk in Diabetes Study Group. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med. 2008;358(24):2545-2559.
74. ADVANCE collaborative group. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560-2572.
75. Duckworth W, Abraira C, Moritz T, et al. Glucose control and vascular complications in veterans with type 2 diabetes. N Engl J Med. 2009;360(2):129-139.
76. Boussageon R, Bejan-Angoulvant T, Saadatian-Elahi M, et al. Effect of intensive glucose lowering treatment on all-cause mortality, cardiovascular death, and microvascular events in type 2 diabetes: meta-analysis of randomised controlled trials. BMJ. 2011;343:d4169.
77. Mattila TK, de Boer A. Influence of intensive versus conventional glucose control on microvascular and macrovascular complications in type 1 and 2 diabetes mellitus. Drugs. 2010;70(17):2229-2245.
78. Marso SP, Kennedy KF, House JA, McGuire DK. The effect of intensive glucose control on all-cause and cardiovascular mortality, myocardial infarction and stroke in persons with type 2 diabetes mellitus: a systematic review and meta-analysis. Diab Vasc Dis Res. 2010;7(2):119-130.
79. Hemmingsen B, Lund SS, Gluud C, et al. Intensive glycaemic control for patients with type 2 diabetes: systematic review with meta-analysis and trial sequential analysis of randomised clinical trials. BMJ. 2011;343:d6869.
80. Rodriguez-Gutierrez R, Montori VM. Glycemic control for patients with type 2 diabetes mellitus: our evolving faith in the face of evidence. Circ Cardiovasc Qual Outcomes. 2016;9(5):504-512.
81. Triplitt C. Cardiac risk factors and hypoglycemia in an elderly patient: how good is good enough? Consult Pharm. 2010;25(Suppl B):19-27.
82. Macisaac RJ, Jerums G. Intensive glucose control and cardiovascular outcomes in type 2 diabetes. Heart Lung Circ. 2011;20(10):647-654.
83. Bailey CJ, Kodack M. Patient adherence to medication requirements for therapy of type 2 diabetes. Int J Clin Pract. 2011;65(3): 314-322.
84. Cramer JA. A systematic review of adherence with medications for diabetes. Diabetes Care. 2004;27(5):1218-1224.
85. Salas M, Hughes D, Zuluaga A, Vardeva K, Lebmeier M. Cost of medication nonadherence in patients with diabetes mellitus: a systematic review and critical analysis of the literature. Value Health. 2009;12(6):915-922.
86. Ratanawongsa N, Crosson JC, Schillinger D, Karter AJ, Saha CK, Marrero DG. Getting under the skin of clinical inertia in insulin initiation: the Translating Research Into Action for Diabetes (TRIAD) Insulin Starts Project. Diabetes Educ. 2012;38(1):94-100.
87. Hertz RP, Unger AN, Lustik MB. Adherence with pharmacotherapy for type 2 diabetes: a retrospective cohort study of adults with employer-sponsored health insurance. Clin Ther. 2005;27(7):1064-1073.
88. Bundrick Harrison L, Lingvay I. Appointment and medication non-adherence is associated with increased mortality in insulin-treated type 2 diabetes. Evid Based Med. 2013;18(3):112-113.
90. Topp CW, Ostergaard SD, Sondergaard S, Bech P. The WHO-5 well-being index: a systematic review of the literature. Psychother Psychosom. 2015;84(3):167-176.
91. Kroenke K, Spitzer RL, Williams JBW. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16:606-613.
92. American Psychological Association. Beck Depression Inventory. Available at https://www.apa.org/pi/about/publications/caregivers/practice-settings/assessment/tools/beck-depression. Last accessed February 11, 2025.
93. Nau DP. Recommendations for improving adherence to type 2 diabetes mellitus therapy—focus on optimizing oral and non-insulin therapies. Am J Manag Care. 2012;18(Suppl 3):S49-S54.
94. Alvarez Guisasola F, Tofé-Povedano S, Krishnarajah G, Lyu R, Mavros P, Yin D. Hypoglycaemic symptoms, treatment satisfaction, adherence and their associations with glycaemic goal in patients with type 2 diabetes mellitus: findings from the Real-Life Effectiveness and Care Patterns of Diabetes Management (RECAP-DM) Study. Diabetes Obes Metab. 2008;10(Suppl 1):25-32.
95. Vanderpoel DR, Hussein MA, Watson-Heidari T, Perry A. Adherence to a fixed-dose combination of rosiglitazone maleate/metformin hydrochloride in subjects with type 2 diabetes mellitus: a retrospective database analysis. Clin Ther. 2004;26(12):2066-2075.
96. Thayer S, Arondekar B, Harley C, Darkow TE. Adherence to a fixed-dose combination of rosiglitazone/glimepiride in subjects switching from monotherapy or dual therapy with a thiazolidinedione and/or a sulfonylurea. Ann Pharmacother. 2010;44(5):791-799.
97. Hutchins V, Zhang B, Fleurence RL, Krishnarajah G, Graham J. A systematic review of adherence, treatment satisfaction and costs, in fixed-dose combination regimens in type 2 diabetes. Curr Med Res Opin. 2011;27(6):1157-1168.
98. Donnelly LA, Morris AD, Pearson ER. Adherence in patients transferred from immediate release metformin to a sustained release formulation: a population-based study. Diabetes Obes Metab. 2009;11(4):338-342.
99. Campbell RK. Recommendations for improving adherence to type 2 diabetes mellitus therapy—focus on optimizing insulin-based therapy. Am J Manag Care. 2012;18(Suppl):S55-S61.
100. Lee WC, Balu S, Cobden D, Joshi AV, Pashos CL. Medication adherence and the associated health-economic impact among patients with type 2 diabetes mellitus converting to insulin pen therapy: an analysis of third-party managed care claims data. Clin Ther. 2006;28(10):1712-1725.
101. Baser O, Bouchard J, DeLuzio T, Henk H, Aagren M. Assessment of adherence and healthcare costs of insulin device (FlexPen) versus conventional vial/syringe. Adv Ther. 2010;27(2):94-104.
102. Hunt J, Rozenfeld Y, Shenolikar R. Effect of patient medication cost share on adherence and glycemic control. Manag Care. 2009;18(7):47-53.
103. Zafar A, Davies M, Azhar A, Khunti K. Clinical inertia in management of T2DM. Prim Care Diabetes. 2010;4(4):203-207.
104. Siminerio LM. Approaches to help people with diabetes overcome barriers for improved health outcomes. Diabetes Educ. 2008;34(Suppl 1):18S-24S.
105. Hajos TR, Polonsky WH, Twisk JW, Dain MP, Snoek FJ. Do physicians understand type 2 diabetes patients' perceptions of seriousness; the emotional impact and needs for care improvement? A cross-national survey. Patient Educ Couns. 2011;85(2):258-263.
106. Beck RS, Daughtridge R, Sloane PD. Physician-patient communication in the primary care office: a systematic review. J Am Board Fam Pract. 2002;15(1):25-38.
107. Huang YM, Shiyanbola OO, Chan HY, Smith PD. Patient factors associated with diabetes medication adherence at different health literacy levels: a cross-sectional study at a family medicine clinic. Postgrad Med. 2020;132(4):328-336.
108. Office of Minority Health. Think Cultural Health. National Culturally and Linguistically Appropriate Services Standards: Communication and Language Assistance. Available at https://thinkculturalhealth.hhs.gov/clas/standards. Last accessed February 11, 2025.
109. Paez K, Allen JK, Beach MC, Carson KA, Cooper LA. Physician cultural competence and patient ratings of the patient-physician relationship. J Gen Intern Med. 2009;24(4):495-498.
110. Powers BJ, Trinh JV, Bosworth HB. Can this patient read and understand written health information? JAMA. 2010;304(1):76-84.
111. U.S. Census Bureau. Selected Social Characteristics in the United States: 2023. Available at https://data.census.gov/table/ACSDP5Y2023.DP02?d=ACS%205-Year%20Estimates%20Data%20Profiles&table=DP02. Last accessed February 11, 2025.
112. Karliner LS, Napoles-Springer AM, Schillinger D, Bibbins-Domingo K, Pérez-Stable EJ. Identification of limited English proficient patients in clinical care. J Gen Intern Med. 2008;23(10):1555-1560.
113. Healthy People 2030. Health Literacy. Available at https://odphp.health.gov/healthypeople/priority-areas/social-determinants-health/literature-summaries/health-literacy. Last accessed February 11, 2025.
114. Sevilla Mátir JF, Willis DR. Using bilingual staff members as interpreters. Fam Pract Manag. 2004;11(7):34-36.
115. Ngo-Metzger Q, Massagli MP, Clarridge BR, et al. Linguistic and cultural barriers to care: perspectives of Chinese and Vietnamese immigrants. J Gen Intern Med. 2003;18(1):44-52.
116. Flores G. Language barriers to health care in the United States. N Engl J Med. 2006;355(3):229-231.
117. Flores G. The impact of medical interpreter services on the quality of health care: a systematic review. Med Care Res Rev. 2005;62(3):255-299.
118. Karliner LS, Jacobs EA, Chen AH, Mutha S. Do professional interpreters improve clinical care for patients with limited English proficiency? A systematic review of the literature. Health Serv Res. 2007;42(2):727-754.
119. Surbone A. Family, autonomy, and cultural differences. In: Perry M (ed). American Society of Clinical Oncology 2006 Educational Book. Alexandria, VA: American Society of Clinical Oncology; 2006: 156-159.
120. Chao MT, Wade C, Kronenberg F. Disclosure of complementary and alternative medicine to conventional medical providers: variation by race/ethnicity and type of CAM. J Natl Med Assoc. 2008;100(11):1341-1349.
121. Graham RE, Ahn AC, Davis RB, O'Connor BB, Eisenberg DM, Phillips RS. Use of complementary and alternative medical therapies among racial and ethnic minority adults: results from the 2002 National Health Interview Survey. J Natl Med Assoc. 2005;97(4):535-545.
122. Rhee TG, Evans RL, Johnson PJ, et al. Racial/ethnic differences in the use of complementary and alternative medicine in US adults with moderate mental distress: results from the 2012 National Health Interview Survey. J Primary Care Community Health. 2017;8(2):43-54.
123. Committee on Health Literacy, Board on Neuroscience and Behavioral Health. Health Literacy: A Prescription to End Confusion. Washington, DC: The National Academies Press; 2004.
124. Kutner M, Greenberg E, Jin,Y, Paulsen C, White S. The Health Literacy of America's Adults: Results from the 2003 National Assessment of Adult Literacy. Washington, DC: National Center for Education Statistics; 2006.
125. Center for Health Care Strategies. Health Literacy Fact Sheets. Available at https://www.chcs.org/resource/health-literacy-fact-sheets/. Last accessed February 11, 2025.
126. Paasche-Orlow MK, Parker RM, Gazmararian JA, Nielsen-Bohlman LT, Rudd RR. The prevalence of limited health literacy. J Gen Intern Med. 2005;20(2):175-184.
127. Shah LC, West P, Bremmeyr K, Savoy-Moore RT. Health literacy instrument in family medicine: the "newest vital sign" ease of use and correlates. J Am Board Fam Med. 2010;23(2):195-203.
128. Jeppesen KM, Coyle JD, Miser WF. Screening questions to predict limited health literacy: a cross-sectional study of patients with diabetes mellitus. Ann Fam Med. 2009;7(1):24-31.
129. Weiss BD, Mays MZ, Martz W, et al. Quick assessment of literacy in primary care: the newest vital sign. Ann Fam Med. 2005;3(6):514-522.
130. Center for Health Care Strategies. Fact Sheet: Identifying Limited Health Literacy. Available at https://www.chcs.org/resource/identifying-limited-health-literacy/. Last accessed February 11, 2025.
131. Vervloet M, van Dijk L, Santen-Reestman J, van Vlijmen B, Bouvy ML, de Bakker DH. Improving medication adherence in diabetes type 2 patients through real time medication monitoring: a randomized controlled trial to evaluate the effect of monitoring patients' medication use combined with short message service (SMS) reminders. BMC Health Serv Res. 2011;11:5.
1. American Diabetes Association Professional Practice Committee. 2. Diagnosis and classification of diabetes: Standards of Care in Diabetes—2025. Diabetes Care. 2025;48(Supplement_1):S27-S49. Available at https://diabetesjournals.org/care/article/48/Supplement_1/S27/157566/2-Diagnosis-and-Classification-of-Diabetes. Last accessed February 19, 2025.
2. Doyle-Delgado K, Chamberlain JJ, Shubrook JH, Skolnik N, Trujillo J. Pharmacologic approaches to glycemic treatment of type 2 diabetes: synopsis of the 2020 American Diabetes Association's Standards of Medical Care in Diabetes Clinical Guideline. Ann Intern Med. 2020;173(10):813-821. Available at https://www.acpjournals.org/doi/10.7326/M20-2470. Last accessed February 19, 2025.
Mention of commercial products does not indicate endorsement.