Evidence has shown that epidural analgesia is more effective than systemic narcotics in the management of acute pain for a variety of postoperative populations, including trauma procedures, thoracotomy, upper abdominal surgery, and orthopedic procedures. Benefits of the epidural route for the administration of pain management medications include improved analgesia with longer lasting pain relief using fewer doses and less sedation, resulting in earlier restoration and improvement in pulmonary function, decreased metabolic-stress response, and earlier ambulation. The purpose of this continuing education activity is to educate acute care nurses and surgical staff about the use of epidural analgesia as a method of pain control.
This course is designed for nurses and allied surgical staff in postoperative areas including recovery, critical care, oncology, neurology, orthopedics, and obstetrics.
The purpose of this course is to educate acute care nurses and allied surgical staff about the use of epidural analgesia as a method of pain control in a variety of settings.
Upon completion of this course, you should be able to:
- Describe the historical evolution that preceded the use of epidural analgesia as a method of pain management.
- Review spinal anatomy, including differences between the epidural and subarachnoid spaces.
- Identify key points in patient selection and preparation for epidural analgesia.
- Discuss the action of epidural narcotics.
- Compare the advantages and disadvantages of the various epidural administration methods.
- Outline patient safety considerations applicable to the administration of epidural analgesia.
- Discuss physiologic parameters to assess in a patient receiving epidural analgesia.
- Describe narcotic- and catheter-related side effects/complications of epidural analgesia and appropriate nursing interventions.
- Discuss common nursing diagnoses and interventions for the patient receiving epidural analgesia.
Margo A. Halm, RN, PhD, NEA-BC, FAAN, received an Associate Degree of Nursing in 1981 from Iowa Central Community College, a BSN and Master of Arts in Nursing from the University of Iowa, in 1985 and 1987 respectively, and a PhD from the University of Minnesota in 2005. She is a member of the American Association of Critical Care Nurse's, and Sigma Theta Tau International. Dr. Halm has presented nationally and internationally, coauthored articles, and conducted nursing research studies on topics such as epidural analgesia, complementary therapies, women and heart disease, family presence during resuscitation and other family-centered interventions. Currently, Dr. Halm practices as the Associate Chief Nurse Executive of Nursing Research and Evidence-Based Practice at the VA Portland Health Care System in Portland, OR.
Contributing faculty, Margo A. Halm, RN, PhD, NEA-BC, FAAN, has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Mary Franks, MSN, APRN, FNP-C
The division planner has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
Sarah Campbell
The Director of Development and Academic Affairs has disclosed no relevant financial relationship with any product manufacturer or service provider mentioned.
The purpose of NetCE is to provide challenging curricula to assist healthcare professionals to raise their levels of expertise while fulfilling their continuing education requirements, thereby improving the quality of healthcare.
Our contributing faculty members have taken care to ensure that the information and recommendations are accurate and compatible with the standards generally accepted at the time of publication. The publisher disclaims any liability, loss or damage incurred as a consequence, directly or indirectly, of the use and application of any of the contents. Participants are cautioned about the potential risk of using limited knowledge when integrating new techniques into practice.
It is the policy of NetCE not to accept commercial support. Furthermore, commercial interests are prohibited from distributing or providing access to this activity to learners.
Supported browsers for Windows include Microsoft Internet Explorer 9.0 and up, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Supported browsers for Macintosh include Safari, Mozilla Firefox 3.0 and up, Opera 9.0 and up, and Google Chrome. Other operating systems and browsers that include complete implementations of ECMAScript edition 3 and CSS 2.0 may work, but are not supported. Supported browsers must utilize the TLS encryption protocol v1.1 or v1.2 in order to connect to pages that require a secured HTTPS connection. TLS v1.0 is not supported.
The role of implicit biases on healthcare outcomes has become a concern, as there is some evidence that implicit biases contribute to health disparities, professionals' attitudes toward and interactions with patients, quality of care, diagnoses, and treatment decisions. This may produce differences in help-seeking, diagnoses, and ultimately treatments and interventions. Implicit biases may also unwittingly produce professional behaviors, attitudes, and interactions that reduce patients' trust and comfort with their provider, leading to earlier termination of visits and/or reduced adherence and follow-up. Disadvantaged groups are marginalized in the healthcare system and vulnerable on multiple levels; health professionals' implicit biases can further exacerbate these existing disadvantages.
Interventions or strategies designed to reduce implicit bias may be categorized as change-based or control-based. Change-based interventions focus on reducing or changing cognitive associations underlying implicit biases. These interventions might include challenging stereotypes. Conversely, control-based interventions involve reducing the effects of the implicit bias on the individual's behaviors. These strategies include increasing awareness of biased thoughts and responses. The two types of interventions are not mutually exclusive and may be used synergistically.
#30874: Epidural Analgesia Update
The purpose of this course is to educate healthcare professionals about the use of epidural analgesia as a method of pain control. Evidence has shown that epidural analgesia is more effective than systemic narcotics in the management of acute pain for a variety of postoperative populations, including trauma procedures, thoracotomy, upper abdominal surgery, and orthopedic procedures.
By diffusing across the dura and subarachnoid space, epidural narcotics alter pain transmission by binding to mu receptors in the spinal cord. Benefits of the epidural route include improved analgesia with longer lasting pain relief using fewer doses and less sedation. This results in earlier restoration and improvement in pulmonary function, decreased metabolic-stress response, and earlier ambulation.
Preservative-free morphine and fentanyl are the most commonly administered narcotics via intermittent or continuous epidural routes[1]. Onset of analgesia ranges from 15 to 60 minutes, with a duration of 4 to 24 hours. Local anesthetics (e.g., bupivacaine) may also be used, especially in patients who have developed opioid tolerance.
Nursing responsibilities in caring for the patient receiving epidural analgesia include [1]:
Monitoring administration of the narcotic and effectiveness of pain control
Assessing pulmonary, neurologic, and catheter status
Monitoring for and managing narcotic-related side effects and catheter-related complications, such as respiratory depression, nausea/vomiting, pruritus, postdural headache, epidural abscess/hematoma, and catheter migration/shearing/occlusion
Assisting with catheter removal
Evaluating physical and emotional aspects postprocedure
The ancient Greeks were the first to describe the use of narcotics. However, not until the turn of the 20th century did reports of the first epidural anesthetics appear. In the mid-1970s an understanding of the mode of action of narcotics was developed. When discovered, endorphins (endogenous opioid-like compounds) were thought to modulate the transmission of pain by acting on spinal cord opioid receptors. The substantia gelatinosa, an area of the spinal cord found to be rich in opioid receptors, was recognized as a key feature in pain transmission. Then, in the 1980s, intrathecal opioids were initially used in the treatment of intractable cancer pain, an event that led to the eventual widespread postoperative use of spinal opioids [2]. Today, epidural analgesia is an alternative to traditional pain management methods in a variety of clinical settings.
The spinal cord extends from the foramen magnum at the base of the skull to the superior border of L2. It is composed of both white and gray matter. Pain receptors are located within the gray matter of the cord. The spinal cord is covered with meninges, or layers of connective tissue. The innermost layer, the pia mater, is closest to the spinal cord. As a smooth and vascular membrane, the pia mater contains many blood vessels that nourish the cells of the spinal cord.
The arachnoid mater, the middle layer, is a thin and transparent covering. Located between the arachnoid and pia mater is the subarachnoid or intrathecal space. The subarachnoid space extends from the cranium to the sacrum and contains cerebrospinal fluid (CSF) and nerve roots. The dura mater is the outermost meningeal layer. Between the dura mater and the vertebrae is a ligament called the ligamentum flavum, which lines the vertebral canal. Between the dura mater and the ligamentum flavum is the epidural space. As a potential space, it also extends from the base of the skull to the coccyx. It contains fatty and connective tissue, lymph and blood vessels, and spinal nerve roots. The epidural space functions as a fatty pad that surrounds the spinal cord and is a potential depot for lipid-soluble narcotics [2,3].
In contrast, the intrathecal space is usually accessed for a one-time administration of a narcotic bolus. The intrathecal route is used most often in anesthesia practice and for patients who require pain relief for a short duration. The main advantages of this route are its speed and reliability; however, additional doses cannot be given. Because intrathecal narcotic doses are approximately one-tenth of those used with the epidural route, the catheter is removed after administration to prevent infection or accidental overdose. Therefore, a larger volume and higher dose of narcotic is needed when utilizing the epidural route for pain management [2,4].
Patient selection for epidural analgesia is determined by two major factors: the type of pain experienced and the patient's surgical procedure and/or medical condition.
Pain can be classified in various ways. For instance, there are somatic, visceral, and neuropathic types of pain, each of which is associated with different etiologies. Somatic pain results from activation of nociceptors by thermal, mechanical, or chemical stimuli in the superficial or deep tissues. As peripheral receptors are activated, the pain perception is transmitted to the spinal cord and higher cerebral cortex, where pain is perceived. Usually constant and well-localized, somatic pain is often described as sharp, aching, or throbbing. By contrast, visceral pain results from some type of organ damage or dysfunction. Depending upon the exact etiology, visceral pain may have many different descriptions, such as deep, dull, aching, boring, or pressure-like. Lastly, neuropathic pain, originating in the nervous system, is often described as a burning, tingling, or numbing sensation.
Pain sensations traveling from the periphery to the spinal cord are mediated by three types of specialized fibers: large myelinated A fibers (A-beta); small myelinated A fibers (A-delta); and unmyelinated C fibers. Each type of nerve fiber carries a different type of sensation. Stimulation of A-beta fibers can block pain signals, essentially closing the pain "gate." A-delta fibers transmit fast-traveling pain that is pricking in sensation and highly discriminated, such as acute surgical pain. These types of pain sensations are poorly relieved by epidural analgesia [2,5]. However, the majority of pain stimuli (approximately 60% to 70%) are carried more slowly by unmyelinated C fibers. These pain sensations are characterized as dull and aching [5]. While continuous dull pain from deep structures responds the best to epidural analgesia, intermittent dull pain is poorly relieved. Central pain does not respond at all to epidural narcotics [2].
Epidural analgesia is indicated in the management of both acute and chronic pain. Acute postoperative populations that may benefit from epidural analgesia include [2,4,6,7,8,9]:
Thoracic procedures (e.g., thoracotomy, bilateral lung volume reduction, lung transplant)
Upper abdominal procedures (e.g., esophagogastrectomy, abdominal aortic aneurysm resections, liver resection)
Orthopedic procedures (e.g., laminectomy, hip replacement)
Peripheral vascular procedures
Gynecologic/urologic procedures (e.g., vaginal deliveries, cesarean section)
Trauma patients, such as those with rib fractures or other orthopedic/multiple injuries, also obtain relief with this pain management method. Patients who are predisposed to pulmonary complications due to pre-existing medical conditions, such as chronic obstructive pulmonary disease or decreased mobility, or who have a need for pulmonary hygiene, are considered the best candidates [2,6,7]. Patients undergoing procedures such as amputation have also been studied in relation to epidural analgesia. Studies of the use of pre-emptive analgesia preoperatively to decrease phantom pain sensations in patients who have undergone amputation have yielded mixed results [8,10,11,12,13,14,15].
Patients with chronic pain are also candidates for receiving epidural analgesia. The epidural route appears to be successful in relieving pain associated with gynecologic and colorectal tumors [16]. Cancer patients, especially those with regionalized pain below T1 that has been poorly controlled by systemic narcotics due to dose-limiting side effects, such as sedation and respiratory depression, are likely candidates [17,18,19]. Perioperative epidural use may also be associated with improved colon cancer survival in patients without metastases [16,20]. Tumor infiltration of bone seems to be more likely to respond to the epidural route than tumors that infiltrate nerve.
Epidural analgesia may also be indicated in patients with chronic nonmalignant pain, such as low back conditions, multiple sclerosis, and severe osteoporosis, as it may alleviate the chronic drowsiness associated with systemic narcotics [7,17,21]. However, the rapid development of tolerance may be a major limiting factor to more widespread use of epidural analgesia in patients with chronic pain [22]. Although not clearly understood, there appears to be cross-tolerance between narcotics administered epidurally and those given systemically. As a result, patients who require high doses of systemic narcotics will eventually require high epidural doses for optimal pain relief [6].
While numerous reports in the literature document the effectiveness of epidural analgesia for acute and chronic pain, criteria for specific patients most likely to benefit have not been clearly identified. More research is needed to investigate the effectiveness of epidural narcotics with different patient populations [6].
Just as there are several indications for epidural analgesia in the acute care setting, several contraindications also exist. The first absolute contraindications for epidural analgesia are patient refusal and a history of true allergic reaction to a narcotic class. In the case of allergy, which is very rare, another opioid class may be utilized in place of the original drug. Patients who have abnormal hemostasis (e.g., thrombocytopenia, abnormal prothrombin time/partial thromboplastin time values) or who are receiving anticoagulants such as heparin, warfarin, aspirin, or enoxaparin are also contraindicated due to the increased risk of developing an epidural hematoma at the catheter insertion site. Patients who have a systemic infection or a localized infection at the puncture site are contraindicated due to the increased risk of developing an epidural abscess or meningitis [7,23].
The last two contraindications for epidural analgesia are related to neurologic status. Patients who have undergone a recent laminectomy with opening of the dura are contraindicated due to the risk of catheter migration into the subarachnoid space and accidental overdose. Increased intracranial pressure also poses considerable risk. In the event that the dura is inadvertently nicked during catheter placement, the loss of CSF could cause cerebellar or tentorial herniation [7].
Regardless of the indication for epidural analgesia, patients and their family members must be adequately informed about this type of pain control. Prior to placement of the catheter, patients/families should be allowed to voice any concerns. Explanations should be given in layperson's terms about how epidural analgesia works and any adverse effects that may be experienced. Emphasize that side effects are temporary and can be treated. Patients may also require reassurance that epidurals do not cause sleep but that the drugs will control their perception of pain. Lastly, patients should know how long the epidural is intended to be utilized, what analgesic regime will be followed, and that the epidural drugs will not be stopped without provision for alternative pain control.
With the advent of epidural analgesia, many catheters were placed in the lower lumbar region, between L4–L5. In this location, catheter placement is technically easier to perform as the spinal cord terminates above this area [2]. However, with increased utilization of epidural analgesia, it has been shown that pain may be best relieved by placing the catheter at different sites depending on the location of the patient's pain and/or surgical incision [8].
The actual site for catheter placement is determined by the dermatome innervating the area of pain. With thoracic procedures, the catheter is placed between T2–T8, depending upon whether the upper or lower lobes of the lung are affected. Mund et al. reported that the majority of epidural catheters in lung transplant patients were inserted at the level of T9 (with a range from T4–L4) [18]. Similarly, with upper abdominal, orthopedic and peripheral vascular procedures, catheters are placed between T4–L1, T10–L3, and L4–L5, respectively. In the case of trauma, the epidural catheter is placed directly at the site of injury [8]. Selecting the proper dermatome level is even more important when the patient will receive epidural local anesthetics (compared to opioids) as these agents block both afferent and efferent nerve fibers [5,24].
Insertion of an epidural catheter is done by an anesthesiology professional (anesthesiologist or certified nurse anesthetist) or physician in another specialty who has been granted clinical privileges by the institution. Epidural catheters may be placed in the operating room or as a sterile procedure at the patient's bedside. Strict aseptic technique must be used during the insertion, as well as with any contact with the solution, infusion, dressing, or site, to prevent contamination. Nursing responsibilities center on ensuring proper positioning and assisting with the procedure. The lateral position is used for catheter insertion, with the patient's hips and head flexed. This position allows for maximal separation between the intervertebral spaces. The site is then prepared using topical antiseptic and sterile drapes [2,4,7,25].
A local anesthetic, such as lidocaine, is injected into the insertion site. A sterile syringe with air or preservative-free, sterile normal saline is attached to a blunt spinal needle, inserted into the selected interspace, and advanced using gentle pressure. This technique, known as loss of resistance, is the commonly used, and currently most reliable, placement technique as the three tough ligaments that surround the spinal cord do not permit injection unless the needle has entered the epidural space. After the needle has entered the epidural space, normal saline or air may then be easily injected. The potential of intrathecal placement or nicking the dura is decreased by the fact that the flow from the needle pushes the dural layer away. The hanging drop technique is another method for catheter placement; however, it is less reliable. With this technique, it is believed that as the spinal needle enters the epidural space, negative pressure draws a drop of normal saline inward [2,7,26]. As an additional measure, some centers place epidural catheters under fluoroscopy or ultrasound guidance in patients with difficult or unclear anatomy [25,26].
With either technique, a flexible catheter is threaded through the spinal needle and advanced 2–3 cm into the epidural space. The spinal needle is then carefully removed and a slide-lock adapter is attached to the end of the catheter. This adapter permits attachment of the catheter to an injection port or infusion tubing [25]. A filter is also attached to the infusion tubing to ensure the injectate remains sterile and to prevent introduction of microparticles or bacteria into the epidural space. The filter may also be used with intermittent administration setups [7,27].
Catheter placement must be verified to avoid injection of the narcotic into the intrathecal space. The two techniques used to verify catheter placement are aspiration and the use of a test dose [25]. However, the inability to aspirate or the presence of a negative test dose does not guarantee correct catheter placement [7].
The aspiration method involves attaching a 3-cc syringe filled with 2 mL of preservative-free sterile normal saline to the end of the catheter and aspirating gently for 30 seconds. If no aspirate is obtained, the catheter should be in the epidural space. If more than 1 mL of clear fluid that tests positive for glucose is obtained, the catheter is most likely in the subarachnoid space. Bloody aspirate indicates that the catheter has punctured an epidural vein [2,4,7].
Additional verification of catheter placement may be performed by administering a test dose of a local anesthetic, such as bupivacaine or 1.5% lidocaine with 1:200,000 epinephrine. An increase in heart rate or blood pressure indicates that the tip of the catheter is in an epidural vein. Loss of sensory or motor function in the lower extremities or lower abdomen with a decrease in blood pressure over one to five minutes indicates that the catheter tip is in the intrathecal space. In the presence of these findings, the narcotic should be withheld until catheter placement can be fully assessed [2,7].
New technology is being explored for effectiveness in guiding the needle, identifying entry, and confirming the catheter location within the epidural space, including ultrasound techniques, fluoroscopy, bioimpedence, and epidurography [26]. However, further studies are required.
After the catheter is inserted and placement verified, the final step involves dressing the site and securing the catheter. A sterile transparent occlusive dressing is applied to permit easy inspection of the site. In addition, the catheter should be taped securely up the patient's back and positioned at the head for easy access during administration [25]. To prevent catheter dislodgement, in most cases the dressing and/or tape should never be changed, only reinforced as needed [4,7,28]. In some cases, if the epidural catheter will continue to be used after 96 hours, the dressing may need to be changed. Please consult hospital policies and procedures and proceed accordingly [28].
Epidural catheters should be marked clearly to prevent accidental injection of medications. Administration sets without additional injectate ports should be used (if possible) or the ports should be taped. System connections should be assessed to ensure they are tight, dry, and intact. The infusion tubing and pumps should then be clearly labeled with a fluorescent sticker, and a sign should be placed above the bed to clearly identify that the patient has an epidural catheter [5,29]. As noted, strict aseptic technique should be utilized whenever assisting with epidural catheter insertion, or handling the epidural catheter, infusion tubing and connections, and solutions [27,28].
Epidural analgesia is a form of localized pain control. By the process of diffusion, narcotics travel across the dura and subarachnoid space and bind to mu receptors located in the substantia gelatinosa of the dorsal horn of the spinal cord. After these narcotics bind to opioid receptors, they block the release of substance P, a neurotransmitter. When substance P is decreased or absent, nociceptive impulses (pain sensations) do not travel the ascending fibers to the higher brain centers. As a result, the patient does not perceive pain [5].
The rate of narcotic diffusion across the epidural space is affected by lipid solubility. In other words, the more lipid-soluble the drug, the more rapidly it diffuses across the epidural space to the opioid receptors in the spinal cord. With rapid diffusion, less drug is available to migrate to higher brain centers via the CSF or systemic circulation. Even though small amounts of epidural narcotics do reach the supraspinal levels, analgesia is provided with fewer side effects than seen with the systemic route [6,7].
Epidural narcotics also have a selective action on opioid receptors within the spinal cord. The narcotic remains at the segmental level of the spinal cord where injected and, consequently, does not block sensory, motor, or sympathetic nerve fibers. As a result, patients experience little adverse motor, sensory, cardiovascular, or central nervous system effects typically associated with use of systemic narcotics, including abnormal heart rate/blood pressure or sedation [2,4].
Epidural analgesia is associated with several clinical benefits. These advantages include [2,4,7]:
Drug benefits: Longer duration and lower total doses
Response benefits: Improved analgesia, less sedation, earlier ambulation, and reduced morbidity from lessened complications, such as pulmonary problems or effects from the metabolic stress response
Outcome benefits: Improved pulmonary and gastrointestinal function and shortened length of hospital stay
In the category of drug advantages, the first benefit is the longer duration of analgesic effect. When administered into the epidural space, 5 mg of morphine has a duration of 6 to 24 hours, compared to three to four hours when given systemically [7]. As a result, patients receiving epidural analgesia require an overall lower total dosage of narcotic than those who receive systemic narcotics via intramuscular (IM) injection, intravenous (IV) injection, or patient-controlled analgesia (PCA) [2,30]. In a study of epidural analgesia in lung transplant patients, patients who received medication via the epidural route had a duration of analgesia of 3.76 days versus 6.0 days in the IV PCA group before oral medications were started [18]. In cancer patients, longer-lasting analgesia without sedation means that patients are more alert, less depressed, more able to resume daily activities when possible, and more likely to be cared for at home [6].
In terms of patient response benefits, improved analgesia has been documented. Epidural narcotics provide more constant pain relief, without the peaks and valleys of serum drug levels associated with parenteral administration [29]. In one comparative analysis, three different epidural drug dosages or combinations were evaluated in patients undergoing thoracic, abdominal, orthopedic, or cardiac surgery for impact on pain intensity scores. Visual analog scale (VAS) pain scores were significantly lower in those receiving epidural fentanyl 5 mg/mL and bupivacaine 1 mg/mL, compared to ropivacaine 2 mg/mL or fentanyl 10 mg/mL and bupivacaine 1 mg/mL [31]. In another study, the probability of a VAS >40 mm was significantly lower in elective postoperative patients receiving epidural (20% probability) versus systemic narcotics (40% probability) [32]. The probability of having moderate-to-severe pain in the first 24-hour period was also significantly less in the epidural group.
The benefit of less sedation is directly related to the smaller narcotic dose required due to the longer duration associated with the epidural route. By remaining at the level of the spinal cord where they are injected, many epidural narcotics do not migrate to higher brain centers via the CSF or systemic circulation. This phenomenon, known as rostral spread, is responsible for the sedation and disorientation commonly associated with systemic narcotics [7]. Lipophilic drugs (e.g., fentanyl) are less likely to result in rostral spread than hydrophilic drugs (e.g., morphine).
Epidural analgesia leads to other clinical improvements and prevention of complications. Improvement in pulmonary function is yet another benefit of epidural analgesia. Patients receiving epidural narcotics experience an earlier improvement in pulmonary function tests (PFTs) when compared to those receiving systemic narcotics [7,33]. In one study of gastroplasty and thoracotomy patients, researchers identified that all patients had decreased PFTs [30]. However, the epidural patients had a less marked decrease in PFTs and returned to their preoperative values two days earlier than the systemic group.
In addition to an earlier restoration of pulmonary function, epidural patients experience fewer pulmonary complications. The incidence of atelectasis and pneumonia may be decreased because patients with more consistent pain control may have an increased ability to participate in pulmonary toilet activities, such as coughing and deep breathing [2,7,33,34]. Secondly, many patients receiving epidural narcotics spend less time on the ventilator and/or have less need for tracheostomy [35]. In one study, lung transplant patients who received epidural analgesia were extubated at an average of 1.46 days after surgery (range: 0.4 to 4.75 days) [23]. Reintubation rates have also been reported to be lower in lung transplant patients who received epidural analgesia (29%) versus IV PCA narcotics (55%) [18]. The reduction of these pulmonary comorbidities is especially significant for the critically ill patient in that gram-negative pneumonias may be associated with a mortality rate ranging from 33% to 70% [34,36].
Epidural narcotics may also decrease the metabolic-stress response associated with surgery and trauma. This response is characterized by an increased release of cortisol, catecholamines, and antidiuretic hormone causing hyperglycemia, sodium and water retention, potassium wasting, and muscle protein breakdown. Epidural narcotics reduce fluid mobilization and retention, the presence of which may further compromise the patient's pulmonary status and lead to respiratory distress and pulmonary edema. This clinical benefit is especially significant for congestive heart failure patients who have undergone upper abdominal surgery [7,34].
Additional studies have investigated the effects of epidural anesthesia on other patient outcomes. In one study on major vascular surgery, researchers found patients who had combined general and epidural anesthesia with postoperative epidural analgesia had significantly lower cardiac morbidity than those patients who only received general anesthesia with postoperative systemic opioid analgesia [37]. Epidural analgesia in high-risk cardiac surgical patients is associated with hemodynamic stability, decreased catecholamine response, good pulmonary function, and early extubation and discharge from intensive care [38]. Evidence of epidural anesthesia's impact on reducing thromboembolic, pulmonary, and gastrointestinal postoperative complications is also encouraging, and it is suggested that epidural anesthesia may be a significant factor in reducing gastrointestinal complications, such as postoperative ileus, in major abdominal surgery patients [39].
Earlier ambulation is the second patient response benefit of the epidural route. In one study of obese patients after upper abdominal surgery, epidural patients ambulated without assistance earlier than IM patients (23 hours versus 30 hours) [30]. Early mobilization may be a significant factor in reducing thromboembolic complications. In combination, improved pulmonary function and earlier mobilization are two of the most significant factors responsible for decreased morbidity and mortality and length of stay (LOS) in patients receiving epidural analgesia. While these findings are encouraging, more research is needed in various populations to compare the impact of epidural versus systemic narcotics on pulmonary complications and ambulation status, as well as on level of alertness and patients' ability to participate in their own care. For instance, in one study, more rapid rehabilitation was not found to be a benefit in elderly total knee replacement surgery patients who received epidural analgesia (compared to PCA) [40]. Additionally, epidural analgesia was not associated with better pain relief or higher patient satisfaction than PCA in this population.
Mixed findings have been reported in relation to LOS. In some studies, epidural analgesia has been associated with shorter hospital stays. In a study of rib fracture patients, those receiving epidural narcotics had a shorter intensive care unit (ICU) stay (6 days versus 18 days) and overall hospital stay (15 days versus 47 days) compared to patients receiving systemic narcotics [35]. In another study of patients undergoing spinal fusion with instrumentation, epidural analgesia with bupivacaine resulted in patients tolerating a full diet earlier and being discharged an average of 0.5 days sooner than the PCA group [41]. On the other hand, McBeath and colleagues found no difference in LOS in total knee or hip replacement patients receiving either continuous epidural morphine or bupivacaine or PCA opioids (morphine or meperidine) [42]. Additionally, a retrospective analysis of more than 1,500 thoracotomy patients showed no difference between LOS in patients receiving epidural analgesia versus systemic opioid-based therapy [43]. Other outcome benefits have been reported. A study of patients with multiple rib fractures found that epidural analgesia was associated with decreased rates of nosocomial pneumonia and shorter durations of mechanical ventilation [44,45]. More studies are warranted to address the impact that epidural analgesia has on the postoperative course, including the ICU and total hospital LOS [7].
Only preservative-free drugs are administered into the epidural space, as preservatives are neurotoxic and may cause injury to the spinal cord. The two most commonly used narcotics are morphine and fentanyl [2]. Common dosing, as well as the peak and duration of these drugs, are listed in Table 1. However, it is important to note that the epidural dose depends on the patient's height, age, and type of surgery (e.g., lower abdominal versus thoracic procedures) [7]. With any of these agents, the larger the volume of drug infused, the greater the chance for rostral spread to the brainstem, which is responsible for central side effects.
Morphine has a longer duration and is used when the patient requires analgesia over several days. As a result, monitoring for respiratory depression is required for at least 24 hours following administration of the first dose [47]. In addition, this medication is highly water-soluble and is prone to retention in the CSF and systemic circulation. Because more of the drug is available to migrate toward higher brain centers, patients receiving morphine are prone to more frequent side effects than those receiving fentanyl [7]. The maximum dose is 10 mg/day for opioid-naïve patients and 20 mg/day for opioid-tolerant patients [47]. Morphine preparations specifically indicated for epidural use are preferred over generic preparations due to sterility and quality control concerns [48].
In contrast, fentanyl is a synthetic narcotic that is 100 times more potent than morphine. As a highly lipid-soluble drug, it diffuses quickly to opioid receptors, with an onset of 10 to 15 minutes. Another main advantage of fentanyl's lipophilicity is that it leaves less drug available for rostral spread, which results in fewer narcotic-related side effects. Fentanyl has a relatively short duration (one hour or less) and is used when analgesia is needed for a short time. Respiratory depression occurs in more than 10% of patients but is more common in elderly patients [47]. Therefore, monitoring for respiratory depression periodically throughout the duration of the initial dose is necessary.
Other drugs that may be administered via the epidural route include alfentanil, ketamine, meperidine, methadone, clonidine, hydromorphone, and sufentanil, though most of these are off-label uses [47]. Of these, meperidine and methadone are both highly lipid soluble. Therefore, each drug has a quick analgesic onset but a short duration when given by bolus. However, these epidural drugs do not offer advantages over either morphine or fentanyl [6,7].
After epidural administration begins, it is important to taper systemic narcotics. The length of time required to taper systemic narcotics varies from patient to patient and depends on how long the patient has been receiving narcotics. Gradual tapering is essential to prevent narcotic withdrawal syndrome, which can occur whenever narcotics are abruptly stopped by any previous administration route (IM, SL, IV, PO, rectal, or buccal). In addition to the variables previously discussed, dosage of the epidural narcotic will also vary from patient to patient, depending upon whether they are narcotic naïve or if they have received a long-term course of narcotics. Patients with acute pain can be expected to require a lower total daily dose of epidural narcotic compared to a chronic pain patient [6].
Local anesthetics may also be administered via the epidural route. Bupivacaine, a long-acting local anesthetic, is the most often used agent. It may be administered either alone or in combination with epidural opioids, such as morphine or fentanyl, for a synergistic effect and reduction of side effects. Local anesthetics are especially useful for patients who have developed a tolerance to opioids because analgesic action is not dependent only on opioids [5].
The level of blockade achieved with local anesthetics is dependent upon both the concentration or dose and the volume of the infusion. For instance, with bupivacaine, effective analgesia is often achieved with concentrations of 1.25 mg/mL or less. If combined with opioids, the concentration of the opioid generally ranges from 0.05–0.1 mg/mL morphine or 2–5 mcg/mL fentanyl. Volumes of continuous infusions vary between 8–20 mL/hour depending upon the surgical site, catheter location, and individual patient needs [5].
In a study by Scott and colleagues, various concentrations of epidural ropivacaine were evaluated in patients after major lower abdominal surgery to determine their attenuation of IV opioids analgesia and minimization of motor block [49]. Total PCA morphine over 21 hours was significantly less in the 0.2% ropivacaine group (mean: 7.5 mg) compared to control (mean: 43.3 mg) and other ropivacaine concentrations (0.1% mean: 18.7 mg; 0.3% mean: 19 mg). Additionally, VAS scores for pain associated with coughing were significantly lower for all ropivacaine groups after four hours of epidural infusion compared to the control group. In terms of intensity of motor block, the 0.2% ropivacaine concentration provided the best analgesia with minimal motor block compared to the other concentrations. In another study, 61 high-risk patients were randomized to receive either 15 mL of 0.75% ropivacaine or 0.5% bupivacaine [50]. Analgesia effects were assessed using VAS scores, motor block, volume of local anesthetic used, and patient satisfaction. Adverse effects were noted, and patients were monitored for changes in heart rate and mean arterial blood pressure. Patients initially achieved a greater intensity of motor block with bupivacaine, but no significant differences were noted between the two drugs at 30 minutes. Similar durations of motor block, motor block profiles, and VAS scores were noted in both patient groups and no major side effects were noted in either group [50].
Epidural narcotics may be administered by a number of techniques. These administration routes include intermittent bolus injection, continuous infusion, PCA, or implantable ports and infusion pumps for long-term use. In 2023, the American Society for Pain Management Nursing (ASPMN) reaffirmed its position statement that "supports the role of RNs in the administration and management of analgesia via catheter technique including monitoring for potential side effects or complications of care among patients of all ages and in all settings" [46]. The American Society of Anesthesiologists also reaffirmed their position in 2023, asserting that an RN qualified by education, experience, credentials and on-going competency assessment who follows a patient-specific protocol written by a qualified physician should, under the direction of a physician anesthesiologist, be allowed to [52]:
Initiate, adjust, and discontinue analgesic catheter infusions
Administer analgesic boluses through the catheter as prescribed by a physician
Replace empty medication containers and/or delivery devices using proper aseptic technique
Monitor the catheter insertion site
Remove the catheter if coagulation status has been assessed and deemed acceptable by a physician supervisor or written policies
Monitor the patient for analgesic efficacy and side effects
Treat analgesic-related side effects under physician direction
Intermittent administration involves injecting a narcotic bolus at a timed interval and may be used with either acute or chronic pain conditions. The major advantage of intermittent injections is that dosing is based on each individual patient's need. Primary disadvantages include inconsistent analgesia and narcotic-related side effects due to redosing intervals and fluctuating narcotic blood levels; changes in respiratory rate and end-tidal carbon dioxide (CO2) consistent with respiratory depression; and the need for a healthcare provider to administer the dose. The major nursing consideration associated with this route is that iodine-based topical antiseptic solutions should be used to prep the injection port prior to administration. The injection port should not be cleansed with alcohol or other antiseptics as these agents may cause neurotoxicity if they enter the epidural space [7,27].
Continuous infusions deliver epidural drugs at a constant rate by means of an infusion pump, avoiding the peaks and valleys associated with the intermittent technique. This method of administration provides more consistent analgesia due to a constant blood level of the prescribed opioid and also allows a lower total volume of drug to be infused at one time. As a result, fewer side effects, such as respiratory depression, occur with continuous infusions. In addition, the rate of the infusion may be titrated to the patient's response, providing the optimal level of analgesia. The major disadvantage of this route is reliance on an infusion pump and the potential for equipment malfunction [7].
PCA is another option for delivering a fixed rate of epidural narcotics. The major advantage of the PCA route is that the patient may administer additional bolus doses above and beyond the basal rate on an as needed basis. Therefore, this route gives the patient some control to alleviate their pain, especially when sudden increases in pain are experienced [6,7]. PCA has been shown to be both safe and efficacious in appropriately chosen adults, adolescents, and children, and many studies have shown that patients prefer this method of analgesia over intermittent injections [50,53,54].
Implantable ports or infusion pumps are the last option for delivering epidural narcotics. Implantable devices are used for patients requiring long-term pain management, such as oncology populations. With implantable ports, the epidural catheter is surgically placed at the indicated interspace and then tunneled subcutaneously around the patient's trunk. The catheter exits on an accessible location of the abdomen so the injection port can be accessed for either intermittent or continuous infusions [6]. Nonprogrammable fixed-rate infusion pumps deliver a predetermined constant rate of infusion and allow for a change in the dose by changing the drug concentration in the reservoir. Programmable pumps (i.e., variable delivery rate pumps) allow for alterations to the dose, single doses, timed-specific doses, or changes in the continuous infusion rate [8].
Implantable ports consist of an implantable silicone catheter (sized from 4–12 F), and an implantable titanium or silicone port with a self-sealing rubber septum. This port contains an internal reservoir that can be repeatedly accessed by injection with a 90-degree non-coring needle. These needles vary from ½ to ¾ inches, and the appropriate needle length should be chosen based on the patient's size and the depth of the port. The needle should first be connected to extension tubing and flushed with 5 cc of normal saline. Using sterile technique, the site should be cleansed from the center of the port outward 2–3 inches in a circular motion first using alcohol, then followed with an iodine-based antiseptic. Accessing the port is done by stabilizing it between the thumb and index finger of the non-dominant hand. Using the other hand, the needle is inserted perpendicular to the center of the port. The needle should be pushed firmly through the patient's skin and portal septum until it hits the bottom of the platform. Once in the portal body, aspirate for blood; if positive, flush with 10 cc of normal saline. When ready for epidural analgesia, connect the infusion to the extension set and stabilize the needle in the port by covering with an occlusive dressing. To discontinue the infusion, keep the port stabilized between the thumb and index finger, hold needle firmly, and withdraw using even pressure [55,56,57].
It has been a customary nursing practice to cleanse the portal body with povidone-iodine-based solutions prior to accessing the port. This practice is done to disinfect the port and minimize the patient's risk of infection. One study investigated this practice and questioned whether or not a trace amount of povidone-iodine solution could pose some risk for toxicity, especially if the solution were systemically absorbed. In this study, three different techniques were compared: commercially available 10% povidone-iodine swabsticks, commercially available 10% povidone-iodine pledgets, and 4-inch square gauze pads saturated with 10% povidone-iodine solution. A significant difference was found with the three cleansing techniques, and the 10% povidone-iodine pledget introduced the least iodine contamination. The findings of this study are considered preliminary, and more research is needed before nurses routinely abandon the practice of using povidone-iodine for disinfection [19,58,59].
Infusion pumps may also be implanted into a subcutaneous pocket of the abdomen to administer continuous epidural infusions [7]. Both options require surgery and carry a potential for infection. Patients who are likely candidates for implantable ports or infusion pumps include those whose life expectancy is greater than a few months with pain below the mid-cervical dermatome that has been unsuccessfully treated with aggressive analgesics and is inappropriate for neurosurgical procedures [6]. Patient/family teaching for these patients should include an explanation of the procedure in terms the patient can understand, expectations for postoperative pain or discomfort and self-care responsibilities, medication preparation, the procedure for injection, assessing the exit site and tunnel area for signs and symptoms of infection, catheter care and dressing changes, refill schedules and procedures, obtaining supplies and narcotics, and follow-up care [9,27].
The Institute of Medicine's 1999 report Crossing the Quality Chasm revealed that 44,000 to 98,000 patient deaths in the United States each year are due to preventable medical errors [60]. One decade later, a HealthGrades study showed that from 2007 to 2009 there were 79,670 in-hospital deaths attributable to "patient safety events" among Medicare recipients alone [61]. A 2018 study showed that, among the approximately 1 million Medicare patients discharged from hospitals in October 2018, 25% experienced an adverse event or temporary harm event during their stay; of the reported adverse events, 10% of events resulted in patient death (more than 3,000 preventable deaths) and the events cost an estimated $324 million in a single month [51]. Although these figures should be balanced against the more than 35.5 million Medicare hospitalizations each year, preventable adverse events occur all too often and cost the U.S. healthcare system approximately $7.3 billion annually [51,61].
It has been identified that about 80% of all deaths from medication errors are caused by 20 drugs, including opioids and anesthetics that are commonly infused via epidural catheters [62]. Furthermore, about 60% of all life-threatening errors occur with IV therapy. These high-alert medications have a heightened risk of causing significant patient harm when used in error. These drugs contribute to large numbers of medication errors and, when improperly administered, result in poor patient outcomes.
The Joint Commission has created patient safety goals, many of which revolve around safe medication usage and administration [63]. Several patient safety goals are relevant for patients receiving epidural analgesia. First, it is necessary to verify the patient's name and date of birth (two identifiers) when administering epidural medications, including dosage changes. Another patient safety goal focuses on eliminating wrong-site, wrong-patient, and wrong-procedure surgery by conducting a "surgical pause" or "time-out" [64]. During the surgical pause, make sure the team conducts a verification process prior to insertion of the epidural catheter to confirm the correct patient, procedure, and site prior to proceeding [64]. If any concerns arise, assertively speak up on behalf of the patient's safety. Follow the institution's protocol for marking the procedure site and documenting the pause in the patient's health record.
Other national patient safety goals are also important in relation to epidural analgesia. These goals include ensuring that unacceptable abbreviations are eliminated to improve the effectiveness of communication among caregivers, IV and PCA pumps have free-flow protection, medications are standardized and the number of drug concentrations are limited to tighten the safety net for high-alert medications, and staff comply with the current Centers for Disease Control and Prevention (CDC) hand hygiene guidelines to reduce the risk of healthcare-acquired infections [65]. The CDC's guidelines include the use of non-antimicrobial soap when hands are visibly dirty or contaminated and alcohol-based waterless handrub for routine hand cleansing.
Another intervention to improve safety with administration of epidural medications is the use of dual verification. Dual verification, the independent verification by a person competent to administer the medication, is necessary with medications like epidural narcotic infusions because of their high risk of adverse patient outcomes should an error occur. Consider dual verifications on all initial epidural pump set-ups and programming changes (i.e., dose or concentration changes). A well-conducted dual verification includes:
Order detail (drug, dose, concentration, and route)
Medication label
Protocol, if applicable
Programming and any calculations (weight, body surface area, age if applicable, and dilution and syringe volume)
To be effective, this dual verification should be separately conducted. Check your institution's policy regarding use of dual verification and documentation process.
As these patient safety goals portray, patient safety has become tightly woven into the fabric of healthcare organizations. Ideally, all staff members will feel responsible for safety and pursue it on a daily basis. All members of the healthcare team should appropriately identify unsafe conditions and behaviors and intervene to correct them. Healthcare professionals actively care about safety by recognizing safe work practices and coaching peers and colleagues to eliminate unsafe behaviors. In summary, when administering high-alert medications, such as epidural narcotics, utilize these 13 evidence-based strategies for infusion safety [62]:
Follow policies, procedures, and protocols.
Ask for a pharmacist's review.
Confirm the order.
Use standard equipment and drug concentrations.
Control the environment.
Know and use the right equipment.
Identify the patient in at least two ways.
Use a labeling system.
Obtain an independent double-check.
Decide if you should give the drug.
Titrate the dosage.
Check for adverse reactions.
Report significant changes.
The goals of nursing management for a patient receiving epidural analgesia for pain control focus on optimizing comfort and minimizing side effects related to the narcotics and/or catheter placement. In order to accomplish these goals, the assessment phase must include an ongoing evaluation of the patient's pain level, vital signs, neurologic status, and catheter site.
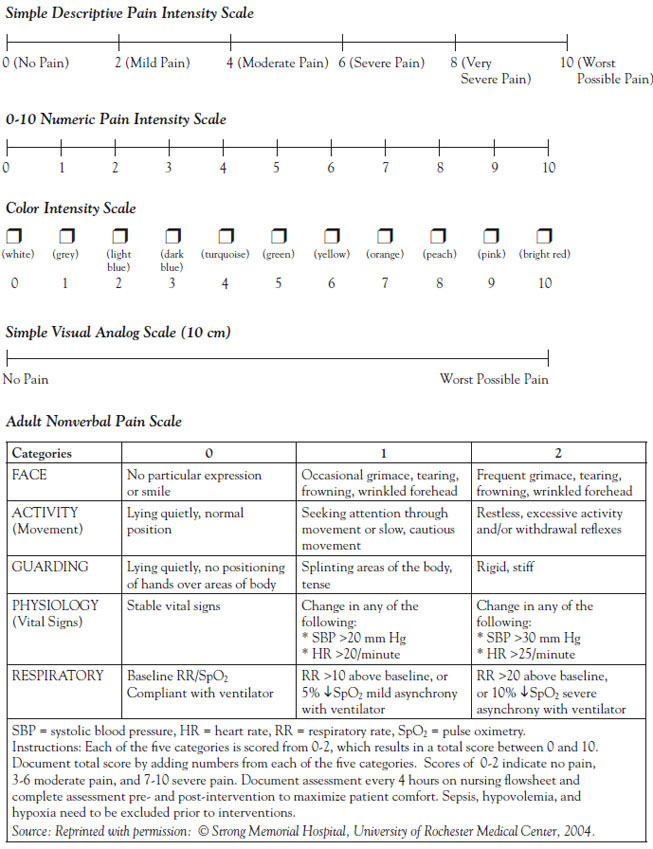
The first parameter to assess is the patient's level of pain. While several tools for pain assessment are available, the most commonly used tool in clinical practice is a VAS (Figure 1)[5]. Various scales may be used, including 0–5, 0–10, or 0–100. The patient is asked what number they would assign to their level of pain, with 0 representing no pain and the largest number equaling the worst pain. These numerical ratings can then be utilized to compare subsequent pain ratings and provide an evaluation of ongoing analgesia. However, pain is a subjective experience, and a rating of 7 for one patient may not be the same in another patient. Therefore, the following assessment questions will further guide evaluating the effectiveness of the epidural route:
What number on a 0–10 scale would you give your pain when it is the worst that it gets?
When is it the least painful?
At what number is the pain at an acceptable level for you?
These questions help assess each individual patient's tolerance of pain. The pain rating that is acceptable to the patient then becomes the goal that is worked toward [6].
Some patients may have difficulty assigning a number to their level of pain. In these cases, the choice of descriptive words (e.g., no pain, a little pain, a lot of pain, too much pain) may be helpful for assessment purposes. These words can then be converted to 0–3 scale for documentation and trending. Another method for pain assessment involves the use of a vertical 10-point VAS. With this technique, the patient is asked to mark their level of pain directly on the scale [66]. Behavioral pain scales are also necessary for those patients who may be cognitively impaired or unable to respond, such as vented and paralyzed or sedated patients. With these scales, a pain intensity score can be obtained by scoring the patient's verbal response, body movement, facial cue, and tactile responses. In addition, as most nurses today practice in ethnically diverse regions, incorporation of multilingual pain scales to allow adequate pain assessment of patients is necessary.
Other important pain assessment parameters, beyond pain intensity, include the location, onset/duration, and aggravating and alleviating factors. With the emphasis by the Joint Commission on pain assessment and pain management, documentation of what has always constituted a thorough and comprehensive pain assessment has become more critical for patient care.
Regardless of the scale used, pain ratings should initially be obtained every hour until the onset of analgesia and then every two to four hours throughout duration of the analgesic effect. Objective physiologic indicators of pain should also be noted, including dilated pupils, pallor, perspiration, nausea and vomiting, and increased heart rate, blood pressure, and respiratory rate [5]. Documentation of pain ratings and other objective pain indicators and the amount of drug infused each hour should be noted on a flowsheet to assist trending and evaluation of ongoing analgesia.
Reassessment of pain and the patient's response to the epidural intervention completes the comprehensive pain assessment. Reassessment is generally recommended at 60 minutes, but with the faster onset of the epidural route, an earlier reassessment interval after dose changes may be warranted. The goal for pain is a rating of less than 3 on the 10-point scale (or the patient's goal for pain relief). The simplest way to assess the effectiveness of an epidural intervention is to reassess the patient's pain with the 10-point scale, but a narrative note is acceptable also. If pain was not lessened, document how the plan of care has changed to reduce the patient's pain. For optimal pain control, the epidural narcotic dose and/or frequency should be adjusted by the physician for patients who complain of inadequate analgesia (i.e., pain ratings over patient's reported acceptable range) [46]. Prior to administration, first check the infusion pump, catheter site, and connections for leakage. If no technical problems are discovered and the patient's pain has not been well controlled, assess whether everything that is indicated for the patient has been tried, such as systemic and adjuvant analgesics, cutaneous stimulation, distraction techniques, relaxation therapy, or imagery [6].
For this standard of pain management to be met, nurses must accept the responsibility of accurately reporting pain assessment findings. Alarmingly, the undertreatment of pain has continued to be widespread [67]. A 2009 study found that 53% of medical inpatients experienced pain (38% with severe pain), and 18% experienced less than 50% analgesic efficacy [68]. Subsequent studies have reported similar findings [69]. In a survey of nurses' decisions about assessment and treatment of pain in two different vignettes, nurses continued to undertreat severe pain [67]. Nurses in this study were more influenced by the patient's behavior than the patient's self-report of pain, especially in relation to decisions about opioid titration. Nurses were less likely to increase a previously safe (but ineffective) dose of opioid for a smiling versus a grimacing patient. Additionally, nurses tended to favor their personal opinions about the patient's pain rather than recorded pain assessments in making decisions regarding opioid dose. These findings contribute to the further undertreatment of pain [67]. Furthermore, studies have shown that patients avoid or delay communicating their pain. Many reasons may explain this behavior, such as not wanting to complain or concern about taking the provider away from other patients [70]. Teaching patients how to communicate their pain to healthcare providers may result in more accurate pain assessments and, therefore, better pain management. Such teaching can also emphasize that effective pain control can avert postoperative complications, such as atelectasis and immobility, and improve patient health outcomes [70].
Monitoring of vital signs is imperative in patients with epidural catheters. Heart rate, blood pressure, and respiratory rate should be monitored hourly for the duration of analgesia. Specifically, vital signs should be monitored for 8 hours in patients receiving fentanyl and for 24 hours in patients receiving morphine [47].
In addition, pulse oximetry should be used to assess oxygen saturation. However, pulse oximetry should not replace routine assessment of respiratory rate as increased CO2 levels can occur despite normal oxygen saturation values—especially if the patient is receiving supplemental oxygen therapy. Both respiratory rate and depth should be assessed every hour for the maximum duration of the first dose and then every four hours. The physician should be notified if the respiratory rate falls below baseline or to less than 10 breaths per minute. Arterial blood gas analysis should be performed if the patient exhibits signs of hypoventilation to confirm elevated CO2 levels. Carbon dioxide levels greater than 50 mm Hg or a gradual rise from baseline are considered indicative of respiratory depression [2,46].
Neurologic assessment is the third component to monitor in the patient receiving epidural analgesia. Assessment of the patient's level of consciousness (LOC) is important because respiratory depression, a rare but life-threatening complication associated with epidural agents, may not be accompanied by a decrease in respiratory rate. A validated sedation scale (Table 2) should be used to assess for signs of respiratory depression [71]. Vital signs and neurologic assessment should be monitored longer than the duration of analgesia if the patient experiences a change in LOC or displays other signs of respiratory depression [4].
SEDATION SCALE IN ASSESSING FOR SIGNS OF RESPIRATORY DEPRESSION
| Sedation Level | Description |
|---|---|
| 0 = No sedation | Awake and alert |
| 1 = Mild sedation | Occasionally drowsy, easy to arouse |
| 2 = Moderate sedation | Frequently drowsy, easy to arouse |
| 3 = Severe sedation | Somnolent, difficult to arouse |
| S = Sleep | Normal sleep, easy to arouse |
A second component of the neurologic assessment should focus on the presence of paresthesias. Paresthesias may be due to the contact of the epidural catheter with neural tissue. Inform the patient that paresthesias are expected during catheter placement and will only last a short time. If numbness or tingling persists, contact the physician for verification of catheter placement. The administration of drugs with preservatives may also cause paresthesias [4]. If local anesthetics have been administered, assessment of motor function is important. Such assessment can be monitored on a 0–4 scale:
0 = No movement
1 = Moves legs on bed
2 = Lifts legs and falls back
3 = Lifts legs and holds
4 = Normal movement
At least every four hours, the catheter site should be checked for intactness or the presence of wetness and for signs of infection. Mild erythema and tenderness at the catheter site are considered normal findings due to bruising and trauma during catheter insertion. However, the physician should be notified if drainage, increasing redness or warmth, or fever is present so that the catheter may be removed. In addition, assess for other neurologic signs that may indicate the development of meningitis, such as headache, persistently high fevers, and nuchal rigidity [5,23,28,29].
A very important aspect of caring for the epidural analgesia patient is monitoring for narcotic-related side effects and catheter-related complications. The most common adverse effects and complications associated with epidural catheters and standard nursing assessments for patients receiving epidural narcotics and/or anesthetics are outlined inTable 3 [7].
NURSING ASSESSMENT FOR PATIENTS RECEIVING EPIDURAL ANALGESIA
| Assessment | Data | Frequency | ||||
|---|---|---|---|---|---|---|
| Pain | 0–10 scale, objective indicators (e.g., increased heart rate, respiratory rate, blood pressure; pallor; nausea/vomiting) | Every two to four hours | ||||
| Vital signs |
|
| ||||
| Neurologic status | Level of consciousness, sensory level, motor strength, paresthesias | Hourly for duration of analgesia | ||||
| Epidural catheter site | Catheter site, dressing, complications (e.g., pain on injection, postdural headache, epidural abscess/hematoma, catheter occlusion/migration/shearing) | Every four hours | ||||
| Narcotic-related side effects | Respiratory depression, hypotension, nausea/vomiting, pruritus, urinary retention | Every four hours |
In general, the side effects of epidural narcotics are no different than those seen with opioids given by other routes. These side effects include respiratory depression, hypotension, nausea and vomiting, pruritus, constipation, and urinary retention [47]. With the exception of urinary retention, the incidence of narcotic-related side effects is dose-dependent. However, the incidence of side effects is higher with the intrathecal method [5]. While further research is needed to compare the rates of narcotic-related side effects of epidural versus systemic narcotics utilized in the management of postoperative patients, one systematic review found that epidural analgesia provided better pain management, reduced adverse events, and reduced length of stay compared with systemic administration [72].
The side effects of epidural local anesthetics may differ from those seen with opioids alone. Local anesthetics are often associated with sensory loss in the region of the block, motor weakness in the lower extremities, alterations in respiratory function, venous pooling and postural hypotension, and urinary retention [5].
The most serious narcotic-related side effect associated with epidural analgesia is respiratory depression. It is manifested by a decrease in the depth of respirations or tidal volume, followed later by a decrease in respiratory rate. Initially, the patient may be able to maintain an adequate respiratory rate but the hyperventilation that occurs does not allow adequate oxygen CO2 exchange. This impaired gas exchange leads to mental status changes indicative of increasing CO2 levels. Therefore, a decrease in the patient's LOC or arousability is considered the first and the best indicator of respiratory depression [5]. Any changes in mentation, such as sedation or confusion, should be considered indicators of hypoxia and/or hypercarbia until ruled out by arterial blood gas levels. As discussed, frequent assessment of the patient's level of sedation is important for early detection and treatment [2]. Several factors place patients at greater risk for the development of respiratory depression (Table 4). Respiratory depression is rarely seen in chronic pain patients because many of these patients have developed a tolerance from previous narcotic administration [6].
RESPIRATORY DEPRESSION: RISK FACTORS
|
Early-Onset Respiratory Depression
The incidence of early-onset respiratory depression is estimated to be less than 1%. It generally occurs within one to two hours of administration and is due to vascular uptake of the opioids from the epidural space. In other words, the narcotic is absorbed by the epidural veins into the systemic circulation. A second mechanism may be the rapid achievement of narcotic concentrations in the brain via the internal vertebral venous system [2,27,46,73].
Delayed-Onset Respiratory Depression
Delayed-onset respiratory depression is relatively uncommon, with an estimated incidence ranging from 0.3% to 5%. With an insidious onset, its peak incidence is 6 to 12 hours after the initial dose; however, it can occur up to 24 hours after administration of the last dose. Delayed-onset respiratory depression related to the lipid and water solubility of the opioids is caused by cephalad diffusion of the narcotic in the CSF to the fourth ventricle, where agonism with opioid receptors of central respiratory centers occurs. Peak CSF concentrations usually occur within five hours [2,27,46].
Because morphine is highly water soluble, it rapidly diffuses cephalad in the CSF via rostral spread. As a result, delayed-onset respiratory depression is more common with morphine. In contrast, fentanyl is highly lipid soluble with greater uptake by the spinal cord. Limited diffusion occurs into the CSF, and thus, respiratory depression in these patients is unlikely [2,5].
Treatment
The first step in managing patients with respiratory depression is withholding additional narcotic boluses or stopping the continuous epidural infusion. The patient should be placed on supplemental oxygen and arterial blood gases obtained. Naloxone, a narcotic antagonist, is also indicated to reverse the respiratory depressant effects, generally for respiratory rates less than eight breaths per minute. The goal of this treatment is to reverse the undesirable side effect while maintaining the beneficial analgesic effects. Naloxone is supplied in 0.4 mg/mL vials. The vial may be diluted with 9 mL of preservative-free normal saline to obtain a 0.04 mg/mL concentration. Small doses, ranging from 0.04–0.4 mg, are repeated (up to a maximum of 0.8 mg) until the desired effect is achieved [47].
After the initial dose, the patient should be continually assessed for the need for additional treatment. Because naloxone has a much shorter half-life (approximately 30 minutes) than narcotics (especially epidural narcotics), repeated administration by either bolus or an infusion may be needed to maintain sufficient plasma levels and reverse the respiratory depressant effects. Naloxone must be titrated slowly, as rapid narcotic reversal may result in hypertension, cardiac dysrhythmias, pulmonary edema, and cardiac arrest due to pain-induced activation of the sympathetic nervous system. Other causes of respiratory depression should be considered if improvement is not achieved with this treatment [47]. The return of pain is possible with naloxone administration, and it is important to review alternative pain management strategies with the patient because additional narcotic doses are not immediately advised [46].
Hypotension is a second potential narcotic-related side effect of epidural analgesia. However, as epidural narcotics have a localized action and do not produce sympathetic nervous system blockade, they generally have little effect on blood pressure. Therefore, if a patient who has received epidural narcotics becomes hypotensive, consider other more common etiologies. The hypotensive state may be a result of fluid volume changes or immobility postoperatively, in which case IV fluids are indicated [7,46]. More rarely, hypotension may be due to allergic reactions, ranging from mild urticaria to cardiovascular collapse. Treatment is determined by the severity of the reaction, from antihistamines to vasopressor support such as IV epinephrine. Other interventions to maintain airway, breathing, and circulation are indicated as needed [7].
Local anesthetics are not specific to sensory afferent fibers, and they do block autonomic and motor efferent fibers. This sympathetic blockade can lead to hypotension and exacerbate or intensify postural hypotension due to hypovolemia. As a result, postural hypotension may restrict early ambulation and potentially increase morbidity. Therefore, assessment of the patient's motor strength prior to ambulation is critical [5,74]. Additionally, assistance with ambulation should be provided to ensure patient safety. Olson and colleagues identified several risk factors for postoperative hypotension in total knee arthroplasty patients who received epidural analgesics/anesthetics [75]. These risk factors included the use of preoperative diuretics, low diastolic blood pressure in the post-anesthesia unit, low postoperative systolic blood pressure on the day of surgery, total fluid intake first postoperative day, and low hemoglobin the third postoperative day. Assessment of these parameters in this population is important in the surveillance of postoperative epidural analgesia.
Pruritus is the most frequently reported narcotic-related side effect of epidural analgesia. The incidence ranges from 28% to 100%, occurring with both acute and chronic administration [2]. Pruritus tends to increase during pregnancy and with co-administration of steroids. The greater intensity of pruritus with epidural narcotics may occur from altered cutaneous sensation or from the effect of the narcotic on the central mechanism located in the medulla [46]. While pruritus is not dose-related, it may continue for the duration of the narcotics' effect. However, some reports identify that pruritus may abate in 48 to 72 hours in patients receiving continuous morphine administration [6,7].
Itching may be local or generalized on the face (especially the nose and palate), trunk, and legs. It may mimic an allergic reaction with a rash, wheals, or edema. An increase in body temperature may also be an exacerbating factor. Treatment is symptomatic, and patients may respond to antihistamines such as 25–50 mg diphenhydramine IM/IV every six to eight hours or 25 mg hydroxyzine IM. In some cases, pruritus may be severe enough to warrant the administration of naloxone titrated to relief. The standard dose of IV naloxone ranges from 0.04–0.4 mg for the treatment of narcotic-related side effects [47].
With an estimated incidence of 17% to 35%, nausea and vomiting may occur as the opioid diffuses from the site of the epidural injection to the chemoreceptor trigger zone for vomiting located in the 4th ventricle [2,46]. This side effect usually occurs four to six hours after administration and may be associated with activity, such as turning and coughing [7]. As with hypotension, searching for other causes of nausea and vomiting, such as abdominal distention or pain, should be attempted first.
Treatment is symptomatic with antiemetics such as prochlorperazine (2.5–10 mg every three to four hours IV, or 5–10 mg every three to four hours IM), metoclopramide (10–20 mg IV, IM), or droperidol (0.625–1.25 mg IV) [47]. However, use extreme caution with the concurrent administration of droperidol (maximum initial dose: 2.5 mg). Droperidol relieves nausea but may potentiate the respiratory depressant effects of epidural narcotics, as may other sedating medications, including midazolam, systemic narcotics, antihistamines, and psychotropics [47]. Small doses of naloxone may also be effective in reducing nausea and vomiting without interrupting analgesia [46].
Urinary retention is another frequently occurring narcotic-related side effect. With an incidence between 22% and 100%, it is the only narcotic-related side effect that does not appear to be dose-dependent [2,76]. It usually occurs in the first 24 to 48 hours and then resolves spontaneously. Signs and symptoms include a lack of urge to void and bladder distention. The underlying mechanism may be the action of the narcotic on the spinal nerves innervating the detrusor muscle, thereby altering bladder tone (atonia) and predisposing to bladder over distension and increased residual volumes [76]. For unknown reasons, urinary retention occurs more often in elderly men, patients with pre-existing bladder disorders, and during pregnancy and the postoperative period. A study of patients after total knee arthroplasty found that use of epidural analgesia was a significant predictor of urinary retention [77]. Urinary retention may lead to urinary tract infections, which in turn can cause hematogenous seeding and infection of the postoperative joint [6,46].
Nursing management involves monitoring intake and output and assessing for bladder distention. Many centers insert an indwelling Foley catheter for the duration that the epidural catheter remains in place. If a Foley catheter is not used, intermittent catheterization may be necessary. However, catheterization in some populations, like total knee arthroplasty, may in fact further increase the risk of infection [77]. The administration of bethanechol or 0.04–0.4 mg naloxone IV may also help reduce the occurrence of this side effect [46,47].
Although rare, a number of catheter-related complications may occur with epidural analgesia. These complications include pain on injection, postdural headache, epidural hematoma or infection, catheter occlusion, catheter migration, or catheter shearing.
Although epidural catheters are small and the resistance to injection is high, patients may feel the expansion of the epidural space and/or the cooler temperature of the medication. Pain on injection is usually felt at the site where the catheter empties into the epidural space and is most often caused by injecting the medication too quickly. As it may also indicate infection or a misplaced catheter, full assessment of catheter placement by the physician is warranted when there is pain on injection [46].
Postdural puncture headache, caused by epidural catheter placement, has an incidence ranging from less than 1% to 70%, depending on the needle used (size and type), procedure, and age and sex of the patient. Incidence has been found to be inversely related to the experience of the anesthetist [78]. Postdural puncture headache occurs more often in adults younger than 40 years of age, and men are affected twice as often as women [2,79]. Commonly, the headache occurs within 48 hours of the puncture and lasts from days to weeks [78]. Dural puncture may be intentional, as with intrathecal catheter placement, or accidental during epidural insertion, causing CSF to leak from the intrathecal space through the puncture hole and resulting in a decrease in CSF volume and intracranial pressure.
The use of smaller, blunt-ended needles has been shown to minimize the size of the dural opening and speed closure of the puncture [2]. One study found that use of the smallest gauge needles (of all styles) drops incidence rates of postdural puncture headache consistently below 4% in procedures not intended to pierce the dura [78]. Another study compared the force required for puncture associated with various needle designs and gauges in samples of bovine dura and found that, among needles of the same gauge, there was a significant variation in the amount of required force and CSF leakage based on design [80]. For example, pencil-point style needles required greater penetrating force and caused significantly less leakage than same gauge Quincke needles; however, for all styles, the smaller gauges resulted in less CSF loss upon puncture. More recent studies report that pencil-point needles are superior to cutting needles at reducing the occurrence of postdural headache, headache severity, and the need for epidural blood patches to seal the puncture [81,82].
The resultant headache is postural in nature, exacerbated by an upright position (such as standing), coughing, or shaking the head and is relieved by lying flat. It is the result of stretch and tension on pain-sensitive intracranial vessels, nerves, and tentorium when the upright position is assumed. The headache is described as dull or throbbing, occurring in the frontal or occipital regions. Other signs and symptoms that are often associated include nausea and vomiting, diplopia, photophobia, tinnitus, and diminished hearing. Conservative management includes bedrest, hydration (which helps the production of CSF), analgesics and antiemetics, and use of an abdominal binder. An autologous epidural blood patch may also be utilized to seal the dural puncture and prevent further leakage of CSF. With this technique, 10 cc of the patient's blood is removed from a peripheral vein and injected through an epidural needle at the location of the dural puncture. The patient's blood migrates and forms a venous clot to seal the dural puncture and stop the CSF leak. The blood patch has a success rate of 89% to 95% and is associated with few complications in low-risk (i.e., not immunocompromised) patients [7,79].
As with any indwelling percutaneous and tunneled catheter, there is the risk of superficial or deep skin and soft tissue infection with epidural analgesia, a risk that varies directly with the length of time the catheter is left in place. Careful aseptic insertion technique with a minimum of trauma, good skin surface and dressing management, and regular inspection of the catheter site for signs of inflammation are each important in minimizing the risk of infection.
Bacterial colonization of the subcutaneous catheter tract and tip is thought to be a major precursor to clinical infection. The rate of epidural catheter colonization has been assessed prospectively in 205 patients receiving short-term postoperative analgesia [83]. In one study of cultures obtained at the time of catheter removal, the rate of colonization of the subcutaneous and tip segments of the catheter was 10.5% and 12.2%, respectively. Skin flora, such as coagulase-negative staphylococci (CoNS), accounted for the majority of isolates. Eleven patients had positive catheter tip cultures: seven CoNS, one Staphylococcus aureus, one Enterococcus, and one Acinetobacter; all had the same organism isolated in large numbers from the adjacent skin and catheter segment sites. Identified risk factors for bacterial colonization of the catheter were adverse catheter site events (e.g., accidental hub disconnection, damage to dressing), adjacent skin colonization, and blood transfusion. The authors concluded that strict aseptic technique at catheter placement and careful attention to maintenance of skin sterility adjacent to the site should reduce rates of catheter tip colonization and decrease the incidence of catheter-related infection [83].
Epidural catheter-associated infections are of two types: superficial (skin and soft tissue) and deep (meninges, epidural space). In one review, the incidence of superficial infection was 4.3%, while reported deep infection rates were much less frequent, ranging from 0% to 0.7% [23]. Common mechanisms of infection include contamination of the exit site and spread along the catheter tract, contamination during needle or catheter insertion, hematogenous seeding from a distant focus of infection, and intraluminal spread via contaminated epidural infusion solutions. Difficult catheter insertions that result in undue trauma at the level of the dura may play a role in the development of epidural space infection. The incidence of infection appears to vary with the site of catheter placement, as one report found that the risk of infection was highest with thoracic epidural catheter usage [23]. One retrospective analysis found that tunneling of thoracic epidural catheters is associated with a lower risk of catheter-related infections [84]. Early local signs of catheter-site infection are erythema, warmth, tenderness, subcutaneous induration, and drainage from the catheter tract [7].
Epidural Abscess or Hematoma
The development of an epidural abscess or hematoma deep to the catheter site is a rare yet potentially serious complication. Bleeding into the epidermal space, from catheter placement trauma or erosion of an epidural venule or arteriole, tends to occur early after catheter insertion and is extremely rare unless the patient has a coagulopathy (e.g., thrombocytopenia, clotting factor deficiency, anticoagulant therapy). As indicated, the incidence of epidural abscess is less than 1% [23].
While rare, epidural hematoma and abscess are potentially life-threatening complications. Clinically, both present as a mass effect: localized pain, swelling or tenderness at the catheter site, radiculopathy, and other spinal cord compression signs [7]. Compression of sensory and motor neural elements in and about the spinal cord results in a variety of neurologic deficits. These include heaviness, numbness and tingling, lancinating pain, and loss of motor function below the affected level (e.g., lower extremities with lumbar catheters). Therefore, the patient's neurologic status should be assessed at least every four hours, including degree of back discomfort, motor strength, and sensory level. The physician should be notified if the patient reports new or unexpected degree of back pain, experiences a change in sensation, or is found to have loss of sensation or diminished motor strength in the extremities. Careful neurologic examination and consideration of magnetic resonance imaging should follow [7,23].
Occlusion of the epidural catheter may be due to various causes. The most common causes include the development of a blood or fatty clot within the catheter, contact of the tip of the catheter against an epidural vein, or kinking of the catheter [7]. Some epidural catheters are virtually kink-resistant due to the coil housed within the lumen of the catheter. If the epidural catheter does become occluded, the patient will not receive analgesia and will complain of returning pain [7]. In this situation, reassessment of catheter patency and placement is warranted.
After the epidural catheter is placed and the needle is removed, it is unlikely that the catheter will migrate and penetrate the dura. While dural puncture most often occurs during placement, the catheter must always be aspirated to verify correct placement prior to administering an epidural narcotic. The catheter dressing should also be assessed routinely to confirm that it is dry and intact. If the dressing is wet and catheter migration is suspected, notify the physician [7].
If the epidural catheter does migrate, a larger amount of narcotic may enter the CSF. With increased analgesia, the patient has a greater risk of respiratory depression, cardiovascular collapse, and neurologic changes, such as altered LOC, seizures, and paresthesias [7]. In these situations, the narcotic should be withheld until catheter placement can be reassessed and alternative routes for the administration of analgesics should be selected.
If the patient is receiving local anesthetics and the epidural catheter migrates into the subarachnoid space, these agents can infuse directly into the CSF and cause the level of blockade to rise. This blockade may affect the respiratory muscles. In addition, local anesthetic toxicity may occur when serum concentrations of the drug elevate. Signs of symptoms of toxicity include tinnitus, visual disturbances, and seizures [5].
Another rare catheter-related complication is shearing or breakage of the epidural catheter. This complication most often occurs during insertion or removal of the catheter. Shearing can be avoided by taping and stabilizing the catheter securely after insertion. Avoid bending the catheter. Again, if the dressing is wet or the catheter is leaking fluid, notify the physician [7]. If the catheter breaks off, the tip is generally not removed as these catheters are nontoxic and non-allergenic. If neurologic sequelae or infection develops, the catheter tip is retrieved surgically [4].
Postprocedure evaluation is an important component of care in the patient receiving epidural analgesia for pain management. While ongoing analgesia is evaluated throughout the intervention, the final phase of evaluation begins with catheter removal. Evaluation helps measure the patient's progress (or lack of progress) toward the goal of controlling pain and minimizing side effects and/or complications. In addition to these physical aspects, the patient's perspective on the effectiveness of epidural analgesia as a pain management modality should also be assessed.
Epidural catheters generally remain in place until the patient is comfortable taking oral analgesics for approximately 24 hours. This point is critical because the time of changing narcotic routes is the most vulnerable period for undermedicating patients. The dose of narcotic for the new route should be calculated using an equianalgesic chart and the patient/family educated about the new route. Assess the patient's comfort level and either increase or decrease the dose according to the patient's individual response [6].
While dependent upon hospital policy, catheters are usually left in place for up to 96 hours after placement [4,7,28]. In many hospitals, physicians remove the dressing and catheter. However, the ASPMN has released and reaffirmed a practice statement that supports the role of nurses in managing the catheter and monitoring for potential side effects or complications [46]. Although the placement of epidural catheters and initial testing and prescription of analgesic therapy lies with the responsibility of an anesthesiology professional, this practice statement advocates for the role of the RN in removing epidural catheters. Removal of epidural catheters by RNs is contingent upon a specific order from a qualified anesthesia professional or physician provider if educational criteria have been met and the procedure is permitted by both state law and institutional policy/protocol [46].
For catheter removal, the patient should be placed in the lateral decubitus position with full flexion of the spinal canal (just like with insertion) for maximal opening of the intervertebral spaces [4]. If hospital policy allows RNs to remove epidural catheters, gently remove the tape and transparent dressing from the patient's back. Then, remove the catheter by withdrawing slowly and using steady, gentle traction. Never apply force to the epidural catheter. If the catheter does not remove easily, leave the catheter and attempt later or contact the physician. Remember, the epidural catheter is only 3–5 cm in length and should come out easily.
After the catheter is removed, inspect the tip for intactness. Many epidural catheters have a colored mark at the tip for ease of identification. The presence of a mark at the tip indicates that the catheter is intact. If the catheter breaks, notify the physician. After removal, the catheter site should be inspected frequently for signs and symptoms of infection [4]. Patients should also be instructed not to get out of bed unassisted. It is not uncommon for patients to feel dizzy when first getting up and their legs may be weak, so assistance is necessary to promote safety. Further evaluation focuses on reviewing the effect of epidural analgesia on the patient's physiologic status. The expected patient outcomes that should be evaluated include [3,4,6,46]:
Vital signs maintained at baseline
Pulmonary system
Adequate ventilation (respiratory rate >10 breaths per minute with adequate depth of respiration)
Skin and mucous membrane color normal
Arterial blood gases within normal range
Patient able to cough and deep breathe with little difficulty
Neurologic system
LOC at baseline
No motor or sensory changes (motor strength at baseline, no complaints of paresthesias)
Pain
Minimal discomfort (patient reports decreased level of pain on 0–10 scale and objective signs of pain absent)
Patient able to move about freely (both in and out of bed)
No immobility-related complications (e.g., pneumonia, deep vein thrombosis)
Catheter
Little or no pain on injection
No signs/symptoms of infection at catheter site (e.g., redness, induration, exudate) or meningitis (elevated white blood cells, fever, nuchal rigidity, change in LOC, cloudy CSF aspirate)
No catheter-related complications (e.g., catheter migration/shearing)
Side effects
Little or no pruritus
Little or no nausea and vomiting
Little or no urinary retention (i.e., patient able to void spontaneously, urinary output adequate)
Patient verbalizes understanding of teaching related to epidural analgesia
Beyond the immediate postprocedure phase, quality improvement is another important mechanism to evaluate the effectiveness and safety of epidural analgesia for a population of patients. Tools may be developed to evaluate if: the narcotics administered were appropriate and effective for individual patients; the frequency of supplemental analgesics was adequate in relation to patient pain ratings; and assessment parameters were evaluated according to established protocols. In addition, the incidence of side effects and complications should be monitored, along with the appropriateness and effectiveness of nursing/medical interventions to treat these conditions [3].
Some patients may need to talk about their experience with pain. This need may be present whether patients' pain was well controlled or not or if their pain has subsided and pain relief measures are no longer needed. Nurses can assist patients in assimilating their pain experience by encouraging expression of what they remember about the pain sensations, associated thoughts and feelings, reactions to pain, and how other people related to them while they were in pain. Actively listening to patients describe their experience and supporting their reactions may help some individuals emotionally assimilate the feelings that may continue after the pain sensations are over [6].
1. Alteration in pulmonary function related to epidural narcotic or anesthetic administration
Expected Outcomes
Respiratory rate will be greater than 10 breaths per minute.
Depth of respirations will be adequate.
Arterial blood gases will remain at baseline.
LOC will remain at baseline.
Nursing Interventions
Monitor rate/depth of respirations and oxygen saturation per pulse oximeter and/or apnea monitor.
Assess for neurologic signs of CO2 retention (decreased LOC).
Maintain patent IV or saline lock.
Avoid concurrent administration of additional narcotics or sedatives without consulting a physician.
If respiratory rate falls below 10 breaths per minute, contact a physician.
Administer supplemental oxygen and obtain arterial blood gases to verify elevated CO2 levels.
Administer naloxone per protocol.
Withhold additional epidural narcotic doses and review alternative pain management strategies with patient/family.
2. Potential alteration in hemodynamics secondary to sympathetic nervous system blockade associated with local anesthetics
Expected Outcomes
Patient will experience minimal hypotension.
Blood pressure will be maintained at baseline.
Nursing Interventions
Monitor blood pressure every hour after administration of epidural anesthetic.
Administer IV fluids per order if fluid volume deficit present.
Monitor motor strength and orthostatic blood pressures prior to activity; ambulate patient with assistance only.
If patient is receiving epidural opioids only, assess for other causes of hypotension, such as allergic reaction or postural hypotension. Administer IV fluids, antihistamines, or vasopressors as indicated per physician orders.
3. Potential alteration in comfort: Pain secondary to rapid injection of epidural narcotic, inadequate titration, or catheter occlusion, or postdural headache related to dural nick during catheter placement
Expected Outcomes
Maximal pain relief will be obtained.
Catheter will remain unoccluded.
Patient will experience minimal discomfort related to postdural headache.
Nursing Interventions
Administer epidural narcotic slowly if using intermittent technique to decrease pain associated with injection.
Administer epidural narcotic via continuous infusion, if possible, to maintain consistent plasma opioid levels.
Assess level of pain on 0–10 VAS every two to four hours; reassess effectiveness of epidural narcotic dosage based on patient's pain ratings and objective pain indicators.
Assess catheter dressing and tape every shift to ensure site is dry and intact and that catheter is patent and unkinked.
Notify physician of increased pain ratings or if catheter occlusion is suspected. Withhold analgesic until full catheter assessment is performed.
Instruct patient to inform nurse of headache after catheter insertion.
If the patient complains of a headache, maintain supine position, as the headache is postural in nature and worsens with the upright position.
Administer analgesics per physician's order and encourage consumption of fluids.
Assist with autologous blood patch if indicated; 10 cc of patient's blood will be inserted through the epidural catheter to clot and seal the dural puncture.
4. Alteration in comfort: Pruritus secondary to rostral spread of epidural narcotic
Expected Outcome
Minimal pruritus will be experienced by the patient.
Nursing Interventions
Monitor body temperature as pruritus may be exacerbated by an increased body temperature.
Instruct patient to inform nurse of any itching.
Report any complaints of pruritus to the physician.
Administer antihistamine, such as diphenhydramine (25–50 mg IV); repeat as needed to prevent further episodes.
Administer small doses of naloxone (0.04–0.4 mg IV) as needed.
5. Alteration in comfort: Nausea and vomiting secondary to rostral spread of epidural narcotic
Expected Outcome
Minimal nausea and vomiting will be experienced by the patient.
Nursing Interventions
Instruct patient to inform nurse of nausea or vomiting episodes.
Notify physician if patient complains of nausea and/or vomiting.
Administer antiemetics (prochlorperazine or metoclopramide) or small doses of naloxone (0.04–0.4 mg) per protocol.
Use extreme caution when administering sedating antiemetics such as droperidol. This medication may have a synergistic enhancement of the analgesic, increasing the risk of respiratory depression.
As nausea and vomiting usually occur within the first four to six hours after administration, routine prophylaxis is not necessary.
6. Alteration in urinary elimination: Urinary retention secondary to effect of epidural narcotic on spinal nerves innervating bladder
Expected Outcomes
Bladder distention will be absent.
Urge to void will be intact.
Nursing Interventions
Instruct patient to inform nurse of distended bladder. Notify physician of decreased urinary output or bladder distention.
Administer bethanechol per physician's order.
Catheterize as needed or insert indwelling Foley catheter per order.
Remove Foley catheter when epidural catheter is discontinued and monitor elimination patterns.
7. Potential for infection related to indwelling epidural catheter or catheter shearing
Expected Outcomes
Signs of redness, swelling, or purulent drainage at the catheter insertion site are absent.
No signs or symptoms of meningitis will be present.
Nursing Interventions
Assess catheter insertion site for pain, tenderness, or other signs of infection.
Assess for fever, nuchal rigidity, or changes in LOC. Notify physician if present.
Assess catheter tip upon removal. Verify that the tip is intact by the presence of a black-colored mark.
Notify the physician if the catheter tip is not intact upon removal.
8. Potential for injury related to migration of epidural catheter into subarachnoid space or development of epidural abscess/hematoma
Expected Outcomes
Catheter will not migrate out of epidural space.
Epidural abscess or hematoma will be absent.
Nursing Interventions
Assess catheter placement prior to administration of epidural narcotic. Aspirate catheter and assess returns. If no aspirate is obtained, epidural placement is confirmed. In the presence of bloody aspirate or more than 1 mL of clear fluid that tests positive for glucose, the catheter has most likely migrated into the subarachnoid space.
Assess catheter insertion site every shift. Note that the dressing is dry and intact. If the dressing is wet or leaking fluid, notify the physician that catheter migration is suspected.
Assess catheter site for signs/symptoms of infection and evidence of hematoma formation (enlarged hardened area) every four hours.
Perform neurologic assessment every four hours (sensory level and motor function). Inform physician of loss of sensation or decreased motor strength.
9. Knowledge deficit related to use of epidural analgesia as a method of pain control
Expected Outcome
Patient/family will understand purpose of epidural analgesia, including risks and benefits.
Nursing Interventions
Inform the patient/family about the procedure used to insert the epidural catheter.
Teach the patient how to use the pain rating scale and to inform the nurse of decreased levels of analgesia.
Explain the onset and duration of analgesia that may be expected.
Teach the patient/family that epidural analgesia will control pain and not totally eliminate pain (unless epidural anesthetics are used).
Inform the patient to tell the nurse if side effects are experienced at the onset (e.g., nausea/vomiting, pruritus, bladder distention).
If the epidural catheter is intended for long-term use, teach the patient/family about home care.
Patient A is 64 years of age and was scheduled to undergo a thoracotomy for the resection of a lung nodule. On the morning of surgery, Patient A was transferred to the preoperative holding area where an arterial line, peripheral IVs, and an epidural catheter were inserted. A 16F Foley catheter was also inserted to monitor urine output and prevent urinary retention associated with epidural analgesia.
For epidural catheter placement, the patient was positioned in the left lateral decubitus position with his hips and neck fully flexed. The selected site for the catheter, the T10–T11 interspace, was draped and prepped with antiseptic. The thoracic epidural catheter was then inserted using the loss of resistance technique. To verify placement, the catheter was aspirated with no returns of CSF or bloody fluid. A filter was attached to the slide-lock adapter, and the catheter port was cleansed with antiseptic prior to dosing the catheter. Patient A received an initial bolus of 5 mg morphine and 75 mcg fentanyl, followed by a continuous infusion of 0.3 mg morphine per hour. A sterile occlusive dressing was placed at the insertion site, and the catheter was taped securely along the patient's back, with the end of the catheter positioned over his shoulder. The administration set was clearly labeled "epidural catheter."
After he was transferred to the operating room, the patient was intubated and anesthetized. A left thoracotomy incision was made, and the procedure ensued. At the end of the procedure, one chest tube was placed in the left pleural space. After the operation was completed, the patient was extubated and placed on a 50% oxygen mask and transferred to the cardiothoracic ICU.
In the ICU, patient assessment included frequent monitoring of vital signs, especially respiratory rate and tidal volume. After the patient awoke from anesthesia, nursing assessment also focused on his level of pain, neurologic status, and observation for narcotic-related side effects and catheter-related complications. On initial assessment, Patient A's respiratory rate was 20 breaths per minute with an oxygen saturation of 100%. The electrocardiogram monitor showed sinus rhythm with a rate of 98 beats per minute and a few isolated unifocal premature ventricular contractions. Arterial blood pressure was 104/72 mm Hg. When he recovered from anesthesia, he was awake, alert and oriented, with a sedation rating of 2. Patient A rated his pain as a "3" on a 0–10 VAS and stated his pain primarily occurred with pulmonary toilet (coughing and deep breathing) and turning due to his bilateral chest tubes. The Pain Service continued orders for a 0.3 mg continuous infusion of morphine for pain management. Assessment of the epidural catheter revealed that the dressing was dry and intact. The site was slightly erythematous, with some bruising noted. However, the site was free of signs and symptoms of infection, abscess, or hematoma development. Later that evening, Patient A began complaining of pruritus. The itching was present in his face and neck but was especially intense in his truncal region. A slightly raised erythematous rash soon became apparent. Patient A was medicated with 25 mg IV diphenhydramine, which was repeated in six hours due to his continued complaints of intense itching.
On the morning of the first postoperative day, Patient A's respirations became shallow and his respiratory rate dropped to eight breaths per minute. Although he was still arousable with a sedation rating of 3, the physician ordered a set of arterial blood gases. The PCO2 level had climbed to 63 from his baseline in the lower 50s. These assessment findings suggested delayed-onset respiratory depression. As a result, the continuous infusion of morphine was turned off and the patient received 0.2 mg of naloxone slow IV push. The naloxone dose was repeated in 30 minutes with an additional 0.1 mg IV. Patient A continued to rate his pain a "3" on a 0–10 VAS. Thus, the respiratory depressant effects were reversed without negating the beneficial analgesic effects of the morphine infusion. Patient A remained on a 50% face mask, which was supplemented with 7 L per nasal cannula.
Eight hours later, the patient's level of consciousness was at baseline and respirations were greater than 12 breaths per minute with a good tidal volume. The morphine infusion was restarted at 0.3 mg per hour. With good pain relief, Patient A was able to be assisted to the chair for activity. On the second postoperative day with continued good pain relief, the patient was up to the chair and ambulated twice for 150–250 feet with assistance from physical therapy.
After three days, the epidural catheter was removed by the anesthesiologist. Again, Patient A was placed in the lateral decubitus position with his hips and neck flexed and the occlusive dressing was removed. The epidural catheter was then slowly and carefully removed and the tip of the catheter was inspected. The black colored marking was present on the tip of the catheter, indicating it was fully intact upon removal. In assessing the catheter site, only a small degree of erythema was noted. After discontinuation of epidural analgesia, the patient's Foley catheter was removed and he obtained good pain relief with oxycodone/acetaminophen and nonsteroidal anti-inflammatory agents, including ibuprofen and ketorolac. Effective pain control helped Patient A meet his postoperative recovery goals, including pulmonary toilet, maintaining adequate nutrition for wound healing and general strength, and gradual activity progression. After the air leak sealed, the right mediastinal tube was discontinued.
1. Criner GJ, Barnette RE, D'Allonzo GE (eds). Critical Care Study Guide: Text and Review. 2nd ed. New York, NY; Springer; 2010.
2. Bragg C. Practical aspects of epidural and intrathecal narcotic analgesia in the intensive care setting. Heart Lung. 1989;18(6):599-608.
4. Bauer M, George III JE, Seif J, Farag E. Recent advances in epidural analgesia. Anesthesiol Res Pract. 2012;309219:1-14.
5. Chumbley G, Thomas S. Care of the patient receiving epidural analgesia. Nurs Stand. 2010;25(9):35-40.
6. McCaffery M, Beebe A. Pain: Clinical Manual for Nursing Practice. St. Louis, MO: C.V. Mosby; 1989.
7. Manion SC, Brennan TJ. Thoracic epidural analgesia and acute pain management. Anesthesiology. 2011;115(1):181-188.
8. Benzon H, Rathmell JP, Wu CL, et al. Practical Management of Pain. 6th ed. St. Louis, MO: C.V. Mosby; 2022.
9. Ganapathi S, Roberts G, Mogford S, Bahlmann B, Ateleanu B, Kumar N. Epidural analgesia provides effective pain relief in patients undergoing open liver surgery. Br J Pain. 2015;9(2):78-85.
10. Raichle KA, Osborne TL, Jensen MP, Ehde DM, Smith DG, Robinson LR. Preoperative state anxiety, acute postoperative pain, and analgesic use in persons undergoing lower limb amputation. Clin J Pain. 2015;31(8):699-706.
11. Ypsilantis E, Tang TY. Pre-emptive analgesia for chronic limb pain after amputation for peripheral vascular disease: a systematic review. Ann Vasc Surg. 2010;24(8):1139-1146.
12. Bloomquist T. Amputation and phantom limb pain: a pain-prevention model. AANA J. 2001;69(3):211-217.
13. Buchheit T, Pyati S. Prevention of chronic pain after surgical nerve injury: amputation and thoracotomy. Surg Clin North Am. 2012;92(2):393-407.
14. McCormick Z, Chang-Chien G, Marshall B, Huang M, Harden RN. Phantom limb pain: a systematic neuroanatomical-based review of pharmacologic treatment. Pain Med. 2014;15(2):292-305.
15. Borghi B, D'Addabbo M, Borghi R. Can neural blocks prevent phantom limb pain? Pain Manag. 2014;4(4):261-266.
16. Cummings KC 3rd, Xu F, Cummings LC, Cooper GS. A comparison of epidural analgesia and traditional pain management effects on survival and cancer recurrence after colectomy: a population-based study. Anesthesiology. 2012;116(4):797-806.
17. The Joint Commission. R3 Report Issue 11: Pain Assessment and Management Standards for Hospitals. Available at https://www.jointcommission.org/standards/r3-report/r3-report-issue-11-pain-assessment-and-management-standards-for-hospitals. Last accessed February 1, 2024.
18. Mund G, Dogra S, Lucas L, Blau WS, Calhoun P. Epidural Analgesia in Lung Transplant Patients. Available at http://www.csen.com/anesthesia/lung-transplant.htm. Last accessed February 1, 2024.
19. Paice JA, DuPen A, Schwertz D. Catheter port cleansing techniques and the entry of povidone-iodine into the epidural space. Oncol Nurs Forum. 1999;26(3):603-605.
20. Christopherson R, James KE, Tableman M, Marshall P, Johnson FE. Long-term survival after colon cancer surgery: a variation associated with choice of anesthesia. Anesth Analg. 2008;107(1):325-332.
21. American Society of Anesthesiologists Task Force on Chronic Pain Management. Practice guidelines for chronic pain management: an updated report by the American Society of Anesthesiologists Task Force on Chronic Pain Management and the American Society of Regional Anesthesia and Pain Medicine. Anesthesiology. 2010;112:1-24.
22. Carroll IR, Angst MS, Clark JD. Management of perioperative pain in patients chronically consuming opioids. Reg Anesth Pain Med. 2004;29(6):576-591.
24. Sugden A, Cox F. How to Assess Epidural Blockade. Available at https://www.nursingtimes.net/clinical-archive/perioperative-nursing/how-to-assess-epidural-blockade-14-03-2006/. Last accessed February 1, 2024.
25. Chawla J. Epidural Nerve Block. Available at https://emedicine.medscape.com/article/149646-overview#a01. Last accessed February 1, 2024.
26. Elsharkawy H, Sonny A, Chin KJ. Localization of epidural space: a review of available technologies. Journal Anaesthesiol Clin Pharmacol. 2017;33(1):16-27.
27. Hayek SM, Goomber R. A review of epidural catheter-related infections. Hosp Pract. 2012;40(2):176-185.
28. Sethna NF, Clendenin D, Athiraman U, Solodiuk J, Rodriguez DP, Zurakowski D. Incidence of epidural catheter-associated infections after continuous epidural analgesia in children. Anesthesiology. 2010;113(1):224-232.
29. Freise H, Van Aken HK. Risks and benefits of thoracic epidural anaesthesia. Br J Anaesth. 2011;107(6):859-868.
30. Rawal N, Sjöstrand U, Christoffersson E, Dahlström B, Arvill A, Rydman H. Comparison of intramuscular and epidural morphine for postoperative analgesia in the grossly obese: influences on postoperative ambulation and pulmonary function. Anesthes Analg. 1984;63(6):583-592.
31. Towell TJ, Maric S, Jones M, Wyatt R, Duthie DJ. Introducing ropivacaine into a department's epidural analgesic practice: improving acute pain service practice. Clin Perform Qual Health Care. 2000;8(4):217-221.
32. Svenson I, Sjöström B, Haljamäe H. Assessment of pain experiences after elective surgery. J Pain Symptom Manage. 2000;20(3):193-201.
33. Tenenbein PK, Debrouwere R, Maguire D, et al. Thoracic epidural analgesia improves pulmonary function in patients undergoing cardiac surgery. Can J Anaesth. 2008;55(6):344-350.
34. Bignami E, Landoni G, Biondi-Zoccai GG, et al. Epidural analgesia improves outcome in cardiac surgery: a meta-analysis of randomized controlled trials. J Cardiothorac Vasc Anesth. 2010;24(4):586-597.
35. Ullman DA, Fortune JB, Greenhouse BB, Wimpy RE, Kennedy TM. The treatment of patients with multiple rib fractures using continuous thoracic epidural narcotic infusion. Reg Anesth. 1989;14(1):43-47.
36. Shi SH, Kong HS, Jia CK, et al. Risk factors for pneumonia caused by multidrug-resistant Gram-negative bacilli among liver patients. Clin Transplant. 2010;24(6):758-765.
37. Yeager MP, Glass DD, Neff RK, Brinck-Johnsen T. Epidural analgesia and analgesia in high-risk surgical patients. Anesthesiology. 1987;66(6):729-736.
38. Mehta Y, Arora D, Vats M. Epidural analgesia in high risk cardiac surgical patients. HSR Proc Intensive Care Cardiovasc Anesth. 2012;4(1):11-14.
39. Augestad KM, Delaney CP. Postoperative ileus: impact of pharmacological treatment, laparoscopic surgery and enhanced recovery pathways. World J Gastroenterol. 2010;16(17):2067-2074.
41. Van Boerum DH, Smith JT, Curtin MJ. A comparison of the effects of patient-controlled analgesia with intravenous opioids versus epidural analgesia on recovery after surgery for idiopathic scoliosis. Spine (Phila Pa 1976). 2000;25(18):2355-2357.
42. McBeath DN, Shah J, Sebstian L, Sledzinkski K. The effect of patient controlled analgesia and continuous epidural infusion on length of hospital stay after total knee or total hip replacement. CRNA. 1995;6(1):31-36.
43. Kampe S, Weinreich G, Darr C, et al. The impact of epidural analgesia compared to systemic opioid-based analgesia with regard to length of hospital stay and recovery of bowel function: retrospective evaluation of 1,555 patients undergoing thoracotomy.J Cardiothorac Surg. 2014;9:175.
44. Bulger EM, Edwards T, Klotz P, Jurkovich GJ. Epidural analgesia improves outcome after multiple rib fractures. Surgery. 2004;136(2):426-430.
45. Pöpping DM, Elia N, Marret E, Remy C, Tramèr MR. Protective effects of epidural analgesia on pulmonary complications after abdominal and thoracic surgery: a meta-analysis. Arch Surg. 2008;143(10):990-999.
46. Elliot JE, Fischer M, Meloche K, et al. Registered nurse management and monitoring of analgesia by catheter techniques: position statement. Pain Management Nursing. 2023;24(3):P246-P247.
47. LexiComp Online. Available at https://online.lexi.com. Last accessed February 4, 2021.
49. Scott DA, Chamley DM, Mooney PH, Deam RK, Mark AH, Hägglöf B. Epidural ropivacaine infusion for postoperative analgesia after major lower abdominal surgery—a dose finding study. Anesth Analg. 1995;81(5):982-986.
50. Korula S, George GM, Ipe S, Abraham SP. Epidural anesthesia and post-operative analgesia for bilateral inguinal mesh hernioplasty: comparison of equipotent doses of ropivacaine and bupivacaine. Saudi J Anaesth. 2011;5(3):277-281.
51. U.S. Department of Health and Human Services, Office of Inspector General. Adverse Events in Hospitals: A Quarter of Medicare Patients Experienced Harm in October 2018. Available at https://oig.hhs.gov/oei/reports/OEI-06-18-00400.pdf. Last accessed February 1, 2024.
52. American Society of Anesthesiologists. Statement on the Role of Registered Nurses in the Management of Continuous Regional Analgesia. Available at https://www.asahq.org/standards-and-practice-parameters/statement-on-the-role-of-registered-nurses-in-the-management-of-continuous-regional-analgesia. Last accessed February 1, 2024.
53. Macintyre P. Safety and efficacy of patient-controlled analgesia. Br J Anaesth. 2001;87(1):36-46.
54. Paul JE, Bertram B, Antoni K, et al. Impact of a comprehensive safety initiative on patient-controlled analgesia errors. Pain Med. 2010;113(6):1427-1432.
55. The Royal College of Anaesthetists. Best Practice in the Management of Epidural Analgesia in the Hospital Setting. Available at https://fpm.ac.uk/sites/fpm/files/documents/2020-09/Epidural-AUG-2020-FINAL.pdf. Last accessed February 1, 2024.
56. Christianson D. Caring for a patient who has an implanted venous port. Am J Nurs. 1994;94(11):40-44.
58. Goudet V, Timsit JF, Lucet JC, et al. Comparison of four skin preparation strategies to prevent catheter-related infection in intensive care unit (CLEAN trial): a study protocol for a randomized controlled trial. Trials. 2013;27:14:114.
59. Lai NM, Lai NA, O'Riordan E, Chaiyakunapruk N, Taylor JE, Tan K. Skin antisepsis for reducing central venous catheter-related infections. Cochrane Database Syst Rev. 2016;(7):CD010140.
60. Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press; 2001.
61. Agency for Healthcare Research and Quality. HealthGrades Eighth Annual Patient Safety in American Hospitals Study. Available at https://psnet.ahrq.gov/issue/healthgrades-eighth-annual-patient-safety-american-hospitals-study. Last accessed February 1, 2024.
62. Dennison RD. High-alert drugs: strategies for safe IV infusions. Am Nurse Today. 2006;1(2):28-33.
63. The Joint Commission. 2024 Comprehensive Accreditation Manual for Hospitals. Oakbrook Terrace, IL: Joint Commission on the Accreditation of Healthcare Organizations; 2023.
65. Centers for Disease Control and Prevention. Guideline for hand hygiene in health-care settings: recommendations of the Healthcare Infection Control Practices Advisory Committee and the HICPAC/SHEA/APIC/IDSA hand hygiene task force. MMWR. 2002;51(RR16):1-44.
66. Dalton JA, Carlson J, Lindley C, Blau W, Youngblood R, Greer SM. Clinical economics: calculating the cost of acute postoperative pain medication. J Pain Symptom Manage. 2000;19(4):295-308.
67. McCaffery M, Ferrell BR, Pasero C. Nurses' personal opinions about patients' pain and their effect on recorded assessments and titration of opioids doses. Pain Manag Nurs. 2000;1(3):79-87.
68. Morris AC, Howie N. Pain in medical inpatients: an under-recognised problem? J R Coll Physicians Edinb. 2009;39(4):292-295.
69. Albrecht E, Taffe P, Yersin B, Schoettker P, Decosterd I, Hugli O. Undertreatment of acute pain (oligoanalgesia) and medical practice variation in prehospital analgesia of adult trauma patients: a 10 yr retrospective study. Br J Anaesth. 2013;110(1):96-106.
70. McDonald DD, McNulty J, Erickson K, Weiskopf C. Communicating pain and pain management needs after surgery. Appl Nurs Res. 2000;13(2):70-75.
71. Devlin JW, Skrobik Y, Gélinas C, et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit Care Med. 2018;46(9):e825-e873.
72. Guay J, Kopp S. Epidural pain relief versus systemic opioid-based pain relief for abdominal aortic surgery. Cochrane Database Syst Rev. 2016;(1):CD005059.
73. Cashman JN, Dolin SJ. Respiratory and haemodynamic effects of acute postoperative pain management: evidence from published data. Br J Anaesth. 2004;93(2):212-223.
74. Roffey P, Thangathurai D, Mogos M, Black D, Mikhail M. Postural hypotension blamed on epidural. J Pain Symptom Manage. 2001;22(2):634-635.
75. Olson B, Ustanko L, Melland H, Langemo D. Variables associated with hypotension in postoperative total knee arthroplasty patients receiving epidural analgesia. Orthop Nurs. 1992;11(4):31-37, 62.
76. Ladak SS, Katznelson R, Muscat M, Sawhney M, Beattie WS, O'Leary G. Incidence of urinary retention in patients with thoracic patient-controlled epidural analgesia (TPCEA) undergoing thoracotomy. Pain Manag Nurs. 2009;10(2):94-98.
77. Lingaraj K, Ruben L, Chan YH, Das SD. Identification of risk factors for urinary retention following total knee arthroplasty: a Singapore hospital experience. Singapore Med J. 2007;48(3):213-216.
78. Turnbull DK, Shepherd DB. Post-dural puncture headache: pathogenesis, prevention and treatment. Br J Anaesth. 2003;91(5):718-729.
79. Calderon R, Copenhaver D. Postdural puncture headache. J Pain Palliat Care Pharmacother. 2013;27(4):406-407.
80. Westbrook JL, Uncles DR, Sitzman BT, Carrie LE. Comparison of the force required for dural puncture with different spinal needles and subsequent leakage of cerebrospinal fluid. Anesth Analg. 1994;79(4):769-772.
81. Zorrilla-Vaca A, Healy R, Zorrilla-Vaca C. Finer gauge of cutting but not pencil-point needles correlate with lower incidence of post-dural puncture headache: a meta-regression analysis. J Anesth. 2016;30(5):855-863.
82. Xu H, Liu Y, Song WY, et al. Comparison of cutting and pencil-point spinal needle in spinal anesthesia regarding postdural puncture headache: a meta-analysis. Medicine (Baltimore). 2017;96(14):e6527.
1. Carmichael JC, Keller DS, Baldini G, et al. Clinical practice guidelines for enhanced recovery after colon and rectal surgery from the American Society of Colon and Rectal Surgeons and Society of American Gastrointestinal and Endoscopic Surgeons. Dis Colon Rectum. 2017;60(8):761-784. Available at https://fascrs.org/ascrs/media/files/downloads/Clinical%20Practice%20Guidelines/clinical_practice_guidelines_for_enhanced_recovery-3.pdf. Last accessed March 14, 2024.
2. Galvagno SM Jr, Smith CE, Varon AJ, et al. Pain management for blunt thoracic trauma: a joint practice management guideline from the Eastern Association for the Surgery of Trauma and Trauma Anesthesiology Society. J Trauma Acute Care Surg. 2016;81(5):936-951. Available at https://www.east.org/education-career-development/practice-management-guidelines/details/thoracic-trauma-blunt-pain-management-of. Last accessed March 14, 2024.
Mention of commercial products does not indicate endorsement.