Study Points
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.
Study Points
Click on any objective to view test questions.
- Identify diseases that are more prevalent among men than among women.
- Describe the health implications of male gender identity and identify strategies to improve communication with male patients.
- Explain the diagnosis and treatment of benign prostate conditions and prostate cancer.
- Apply guideline recommendations for prostate cancer screening.
- Describe treatment options and assist patients in selecting a management strategy for localized prostate cancer.
- Distinguish among benign testicular conditions.
- Discuss the diagnosis and treatment options for testicular cancer.
- Discuss the differences between male and female breast cancer.
- Discuss diagnosis and treatment options, and assist patients in selecting a treatment strategy for sexual dysfunction (premature ejaculation and erectile dysfunction).
- Devise a strategy for diagnostic testing and treatment of late-onset hypogonadism.
- List factors affecting male infertility.
- Promote patient education and disease prevention, implement effective screening, and select guideline-appropriate treatment of sexually transmitted infections.
- Identify issues of particular concern for men who have sex with men.
- Discuss the effects of substance misuse, depression, and stress/anger on the physical and psychosocial well-being of men.
- Discuss the importance of educating men about the need for screening, routine health maintenance, and healthy lifestyle.
Which of the following causes of death occurs at a higher rate for men compared with women?
Which of the following causes of death is more prevalent among Black men than men of other races or ethnicities?
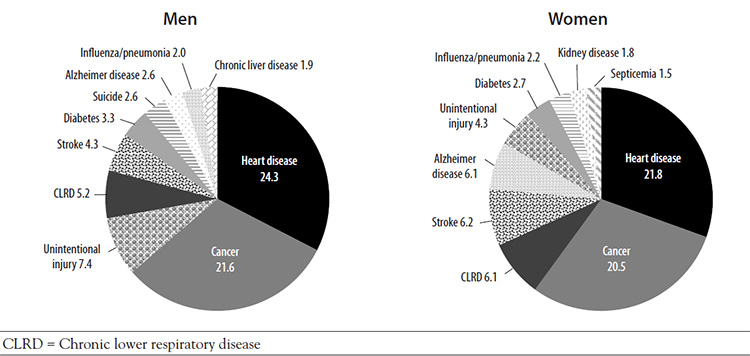
Click to ReviewTEN LEADING CAUSES OF DEATH FOR MEN ACCORDING TO RACE/ETHNICITY, 2018
Leading Causes of Death Mortality Rate and Rank All Men White Black/African American Hispanic/Latino Asian/Pacific Islander American Indian/Alaskan Native Cardiovascular diseases 24.4% (1) 24.8% (1) 24.1% (1) 20.2% (1) 23.1% (2) 18.9% (1) Cancer 22.2% (2) 22.2% (2) 19.7% (2) 19.4% (2) 24.7% (1) 15.9% (2) Unintentional injuries 6.8% (3) 6.9% (3) — 11.3% (3) 5.3% (4) 13.7% (3) Chronic lower respiratory diseases 5.3% (4) 5.8% (4) 3.2% (7) 3.3% (6) 3.2% (6) 3.6% (7) Stroke 4.2% (5) 4.1% (5) 5.0% (4) 4.7% (4) 6.7% (3) 2.9% (8) Diabetes mellitus 3.1% (6) 2.9% (6) 4.4% (6) 4.2% (5) 4.2% (5) 5.7% (5) Suicide 2.5% (7) 2.7% (8) — 3.1% (8) 2.6% (8) 4.2% (6) Alzheimer disease 2.5% (8) 2.9% (7) 7.9% (3) 2.3% (9) 2.3% (9) — Influenza and pneumonia 2.0% (9) 2.0% (9) 1.7% (10) 3.2% (7) 3.2% (7) 2.2% (10) Chronic liver disease 1.9% (10) 1.7% (10) — 4.1% (6) — 6.1% (4) Assault (homicide) — — 4.5% (5) 2.2% (10) — 2.3% (9) Kidney disease — — 2.7% (8) — 2.0% (10) — Septicemia — — 1.7% (9) — — — The cancer accounting for the greatest number of deaths in men is
Click to ReviewWhich of the following statements about deaths caused by unintentional injury is TRUE?
Click to ReviewMen's predilection for risky behavior is reflected in the high rate of unintentional injury, which accounts for 7.4% of deaths among men (compared with 4.3% for women) [7,8]. There is wide variation in this rate across race/ethnicity, with much higher rates among American Indian/Alaska Native men (13.7%) and Hispanic/Latino men (11.3%) [11]. The trend of more fatal unintentional injuries among men is evident in countries around the world; an analysis of accidental deaths among men and women in 36 countries showed higher rates for men [2]. Across all age-groups, the rates were higher in the United States than the median rate for all countries. Accidental deaths are related primarily to motor vehicle injuries, violence, and occupation, and the rates in all categories are higher for men than for women. The rate of death related to motor vehicle injuries for men is slightly higher than for women (16.0 vs. 6.3 per 100,000), and the percentage of fatal unintentional firearm-related injuries deaths occur overwhelmingly more often among men (82.7%) than women (17.3%) [25]. Similarly, fatal occupational injuries occur predominantly in men (57% vs. 6%) [26].
Which of the following best describes the effect of male gender identity on men's health?
Click to ReviewHelp- and information-seeking behavior related to male gender identity is another factor that affects men's health. In general, men are reluctant to seek health care or talk about their health because they see such help-seeking as a sign of weakness or vulnerability and a threat to their masculinity [4,35,36]. These reports are substantiated by data on utilization of healthcare resources, which indicate that men have fewer office visits to doctors or other health care professional than women; in 2018, 23.9% of men had no office visits, compared with 12.5% of women [37]. In addition, men are more likely to lack a usual source of health care (18.6% vs. 10.7%) [37]. Men have reported several reasons for not having a usual source of care, and the reasons vary among racial/ethnic populations [39]. The reason given most often is that they are seldom or never sick, and this may be related to men's perceptions of invulnerability [39,40]. Other reasons given include not finding time and not being able to take time away from work [38]. Cultural values, such as machismo, lead many Hispanic men to avoid health care until there is no other choice [40]. This may contribute to the low rate of healthcare use among Hispanic men, which is the lowest across racial/ethnic populations [40]. Other reasons for the low use of healthcare services among Hispanic men are lack of health insurance, low understanding of the healthcare system, fear of poor functional outcomes, and a low perception of the quality of the patient-clinician interaction [40]. In the Black population, men have reported to avoid healthcare services because of fears and concerns about their negative health behaviors and history [41].
Acute bacterial prostatitis is
Click to ReviewBoth acute and chronic bacterial prostatitis occur in approximately 5% to 10% of men with symptoms related to prostatitis. Chronic nonbacterial prostatitis/chronic pelvic pain syndrome is the most common type, occurring in approximately 90% of symptomatic men [60]. These three types of prostatitis are addressed here; asymptomatic inflammatory prostatitis is an incidental finding during evaluation of another genitourinary condition such as prostate cancer or infertility [61].
It has been estimated that prostatitis accounts for approximately 2 million outpatient visits per year in the United States, with a direct cost of care of nearly $4,000 per patient per year [61]. The condition can have a substantial impact on the quality of life, causing pain and sexual dysfunction, as well as decreased libido and erectile and ejaculatory dysfunction [62,63].
Chronic prostatitis/chronic pelvic pain syndrome has the greatest impact on the quality of life of all types of prostatitis. Studies have found that the effect of chronic pelvic pain syndrome on the quality of life is similar to that of angina, congestive heart failure, diabetes mellitus, and Crohn disease [61]. Symptoms fluctuate over time; one study showed that 43% of men had symptoms within 11 months of follow-up, and another showed that 31% of men had moderate or marked improvement during two years of follow-up [64,65]. Chronic prostatitis/chronic pelvic pain syndrome also causes patient anxiety at the initial visit. Most men with symptoms worry that they have an infection (71%) or cancer (68%), and concerns at one-year follow-up have included worsening symptoms without treatment, cancer, infection, and need for surgery [65]. These concerns have led to an increased number of physician visits [65].
The prevalence of prostatitis has been reported to be approximately 8%, ranging from about 2% to 10% [66]. In patients younger than 35 years of age, the most common variant of the syndrome is acute bacterial prostatitis. Among older patients, nonbacterial prostatitis (NIH types II and IV) is the most common [67]. The results of studies have suggested that the symptoms of prostatitis increase the risk for BPH, lower urinary tract symptoms, and prostate cancer [66].
The cause of acute and chronic bacterial prostatitis is usually lower urinary tract infection with gram-negative organisms, most notably Escherichia coli [60,61]. Most men with prostatitis, however, have no evidence of urinary tract infection [61]. Other causes may include a primary voiding dysfunction problem; presence of Chlamydia trachomatis, Ureaplasma species, or Trichomonas vaginalis; uncommon organisms (e.g., Mycobacterium tuberculosis); HIV; cytomegalovirus; and inflammatory conditions (e.g., sarcoidosis) [67].
The risk factors for prostatitis have not been clearly defined. In a study of 463 men with chronic prostatitis/chronic pelvic pain and 121 asymptomatic age-matched controls, the lifetime prevalence of several self-reported medical conditions were significantly greater among men with prostatitis, specifically neurologic disease (41% vs. 14%); hematopoietic, lymphatic, or infectious disease (41% vs. 20%); psychiatric conditions (29% vs. 11%); nonspecific urethritis (12% vs. 4%); and cardiovascular disease (11% vs. 2%) [68]. The authors of that study noted that more research is needed to determine if such conditions contribute to the pathogenesis of chronic prostatitis/chronic pelvic pain. A history of STIs has been noted to be associated with an increased risk for prostatitis symptoms [66].
Several other urogenital conditions should be considered in the differential diagnosis of prostatitis, including BPH, cystitis, erectile dysfunction, prostate cancer, STI, and urolithiasis [69,70,353]. Of the four types of prostatitis, acute bacterial prostatitis is the easiest to diagnose and treat. Patients with acute prostatitis present with irritative symptoms (dysuria, urinary frequency, and urgency), and obstructive voiding symptoms (hesitancy, incomplete voiding, straining to urinate); the syndrome may also include signs of systemic infection, such as chills and fever [70,353]. Pain most commonly occurs in the prostate/perineum and scrotum and/or testes; pain referred to the penis or lower back also occurs [70]. Urine samples should be cultured to determine the causative micro-organism.
When diagnosing prostatitis,
Click to ReviewChronic bacterial prostatitis is distinguished from acute disease by time, being defined by persistence of symptoms for at least three months, and systemic symptoms are usually absent [58,70]. The condition should be suspected when the patient's history includes recurrent urinary tract infections, usually with the same bacterial strain [61]. The patient should complete an NIH Chronic Prostatitis Symptom Index to obtain a baseline score for the severity of symptoms [59]. This index includes questions related to three domains—pain, urinary symptoms, and quality-of-life impact—and has been shown to be a valid, reliable tool for measuring prostatitis symptoms [70,71]. Computed tomography (CT) can determine if there are structural or functional abnormalities of the urinary tract [60,61].
The diagnostic evaluation for acute or chronic bacterial prostatitis includes a urinalysis and urine culture [61,70]. When acute prostatitis is suspected, digital rectal exam should be performed gently so as not to precipitate bacteremia and sepsis. The prostate will usually be enlarged, boggy, and tender, though absence of tenderness on initial examination does not exclude the diagnosis of prostatitis. There are no standardized criteria for the diagnosis of chronic prostatitis/chronic pelvic pain syndrome [61,69]. The Meares-Stamey four-glass test was developed in the late 1960s to screen for prostatitis; the test involves collecting urine samples before and after prostatic massage, as well as collecting prostatic fluid during the massage [72]. Cultures are done on the specimens, and the presence of micro-organisms in the prostatic fluid indicates chronic prostatitis [61,72]. The accuracy and reliability of the test has not been established, and studies have shown that the test is not used often, even by urologists [61,69]. There is also a two-glass version of the test that has correlated well with the four-glass version, but that, too, is not often used [61]. The Meares-Stamey test is not helpful for diagnosing chronic pelvic pain syndrome. Men who have substantial lower urinary tract symptoms and pelvic pain may be candidates for urodynamic evaluation, as voiding dysfunction is common in such cases [61].
Which of the following statements about the treatment of chronic prostatitis/chronic pelvic pain syndrome is most accurate?
Click to ReviewFor chronic bacterial prostatitis, the choice of antibiotic depends on the sensitivity of the micro-organism, and the antibiotic should be one that penetrates the prostate [61]. The typical first-line treatment is a four- to six-week course of a fluoroquinolone, and treatment is usually more effective if begun soon after symptoms begin [61,70,73,74]. Trimethoprim-sulfamethoxazole may also be considered [70].
Treatment for chronic prostatitis/chronic pelvic pain syndrome is complex; evidence on the effect of traditional treatment options has been conflicting, and treatment options are often not effective in managing symptoms. The most commonly studied pharmacologic options are antibiotics, alpha-blockers, anti-inflammatory agents, steroid inhibitors, and muscle relaxants, and often, a combination of these agents provides the most effective management [74]. Antibiotics, particularly fluoroquinolones, have improved symptoms, even in some patients in whom a bacterial cause has not been identified [74]. Studies have shown that an antibiotic and an alpha-blocker is more effective than an antibiotic alone [70]. A meta-analysis showed that alpha-blockers, antibiotics, and a combination of the two all significantly improve symptoms (according to scores on the NIH Chronic Prostatitis Symptom Index), with the combination providing the greatest benefit [75]. However, another meta-analysis showed that these same agents—alone and in combination—were not associated with a statistically or clinically significant decrease in symptom scores [76]. The combination of an alpha-blocker (doxazosin) with an anti-inflammatory agent (ibuprofen) and a muscle relaxant (thiocolchicoside) led to a statistically and clinically significant reduction in the total score on the NIH Chronic Prostatitis Symptom Index in one systematic review; according to the findings of another systematic review, the three-agent combination was not superior to monotherapy [74,76]. Researchers have cautioned that publication bias may cause overestimation of the beneficial effects of alpha-blockers and that the placebo effect has been significant in many studies [75,76]. Addressing a hypothesis that the pain related to chronic prostatitis may have a neuropathic origin, pregabalin has been evaluated as a management strategy, but a systematic review found that the drug did not improve symptoms and caused side effects in a large percentage of men [77].
An established risk factor for benign prostatic hypertrophy (BPH) is
Click to ReviewThe prevalence of BPH increases with age, from approximately 8% of men 31 to 40 years of age to approximately 90% of men in their 80s [80,81]. Risk factors identified in one study included increased age, prostatic volume, and peak urinary flow rate [82]. Other factors, including some that are modifiable, include obesity, diet, dyslipidemia, hypertension, alcohol use, and smoking [83]. The relative risk for BPH (and common comorbidities) may be higher for Black and Hispanic men than for White men and is thought to be related in part to genetic differences based on race/ethnicity; however, observational studies have produced variable results [81,84].
According to American Urological Association guidelines, which of the following is the preferred approach for a man who has BPH with mild symptoms (a score of 6 on the AUA Symptom Index) and no prostatic enlargement?
Click to ReviewThe AUA guideline recommends watchful waiting as the preferred approach for men who have mild symptoms (a score of less than 8 on the AUA Symptom Index) [78]. This approach may also be taken for men with moderate-to-severe symptoms (score of 8 or more) who are not bothered by the symptoms and have no complications [87]. Watchful waiting should include yearly evaluations similar to the initial one [78]. Lifestyle changes and behavioral interventions are considered reasonable first-line treatments for all patients. Symptoms may be reduced by avoiding decongestants and antihistamines, decreasing fluid intake (and avoiding caffeine and alcohol) prior to bedtime, and increasing physical activity and weight loss [78].
Which of the following has NOT been found to be a risk factor for prostate cancer?
Click to ReviewThe known risk factors for prostate cancer are advanced age, Black race, and a family history of the disease (especially when diagnosed at a younger age) [16,97]. The risk for prostate cancer may also be increased for men with symptoms of prostatitis [66].
In regard to the prevention of prostate cancer, finasteride has been associated with
Click to ReviewSeveral studies have been undertaken to determine the efficacy of chemoprevention agents and dietary supplements to reduce the risk of prostate cancer. The chemoprevention agents evaluated belong to the class of 5-alpha reductase inhibitors, a class of drugs approved for the treatment of BPH. One drug in this class, finasteride, was evaluated in the first large-scale chemoprevention study, the Prostate Cancer Prevention Trial (PCPT), a seven-year study involving nearly 19,000 men 55 years of age or older. In that study, finasteride significantly reduced the prevalence of prostate cancer (18% vs. 24% for the placebo group) [98]. Dutasteride was shown to decrease the risk of prostate cancer in the REDUCE trial, and extended follow-up indicated a low rate of new prostate cancer diagnoses [99,100]. The initial results of the PCPT and REDUCE trials led the American Society of Clinical Oncology (ASCO) and the AUA to develop a joint guideline recommending finasteride and dutasteride for the prevention of prostate cancer [90]. However, reanalysis of the results of the trials showed that the risk for high-grade prostate cancer was increased and the reduction in prostate cancer risk was seen primarily for less fatal subtypes of prostate cancer that are often not treated [100,101]. In 2011, the FDA decided against approving the two drugs for the prevention of prostate cancer, noting that the risk-benefit profile is not favorable for chemoprevention [91,101,102]. As stated earlier, the FDA revised the labels of all 5-alpha reductase inhibitors to note the increased risk of higher-grade prostate cancer associated with the drugs [92]. The ASCO/AUA guideline was withdrawn, and experts have called for more research to determine whether 5-alpha reductase inhibitors have a role in the prevention of prostate cancer [101,102,103].
Prostate cancer screening has been shown to lead to
Click to ReviewThere is no question that available screening methods and enhanced awareness has led to an increased number of men in whom prostate cancer is diagnosed at an earlier stage. The primary benefit of screening is a lower stage and grade of cancer at the time of diagnosis, and the high rate of localized disease at the time of diagnosis (92% to 96%) reflects, in part, the increased number of cancers that are detected earlier through screening [102,108,109]. Despite this benefit, an effect of screening on mortality has not been clearly demonstrated. After 13 years of follow-up in the National Cancer Institute's Prostate, Lung, Colon, and Ovary (PLCO) trial, there was no benefit of annual screening on mortality [110]. A meta-analysis (five randomized controlled trials) similarly demonstrated no effect of screening on prostate cancer-specific or overall mortality [111]. However, data from the European Randomized Study of Screening for Prostate Cancer demonstrated that screening reduced the risk for prostate cancer death by 7% to 9% per year [112].
Which of the following statements about prostate-specific antigen (PSA) is TRUE?
Click to ReviewPSA density is the result of dividing the PSA level by the volume of the prostate, as measured by transrectal ultrasonography, and a higher result suggests a greater likelihood of prostate cancer [97]. Greater PSA density has correlated with the presence of prostate cancer, as well as with the pathologic stage of the tumor and its aggressiveness and progression after treatment [124]. The use of PSA density has been limited by the lack of precision of total PSA, of measurement of prostate volume, and of the need to carry out transrectal ultrasonography [97]. In addition, PSA density does not offer much benefit compared with other PSA derivatives [97]. PSA velocity is the rate at which a PSA level increases over a period of time, and it has been most helpful for longitudinal monitoring of men younger than 50 years of age who have normal PSA levels and no prostate enlargement [97]. A high PSA velocity alone should not prompt biopsy but instead, aid in decision making [97]. The test is not useful for men with PSA values greater than 10 ng/mL [97]. The ratio of complexed PSA to total PSA provides information comparable to the ratio of free to total PSA, and the use of complexed PSA has been approved as a detection aid (in conjunction with DRE) for men 50 years of age or older; however, the test is not widely used in practice [97].
According to research on the communication of risk, men best understand risk when it is discussed in the context of the
Click to ReviewEach treatment option is associated with benefits and harms, and clinicians should discuss each option in detail and provide educational resources and decision aids [129,130,131]. To gain a true understanding of a patient's preferences, treatment options should be discussed only after the patient has described his preferences [132]. Clinicians should carefully assess their patients' understanding of treatment options; studies of underserved men have shown low comprehension of common terms used in prostate cancer treatment discussions [133,134]. Attention should also be paid to how to best communicate risk. A study has shown that such terms as "number needed to treat," "odds ratio," and "relative risk reduction" were confusing to men [135]. In that study, men best understood information when it was presented as an absolute risk reduction and in a positive context; men preferred that treatment options be discussed in terms of the probability of an increase in survival (rather than a decrease in mortality) and that the discussion include the impact of treatment on patient-centered quality-of-life outcomes [135].
A man has clinically localized prostate cancer (T1c), with a Gleason score of 4 and a PSA level of 8 ng/mL. He is 68 years of age and has a life expectancy of more than 10 years. According to NCCN guidelines, which of the following is the recommended approach?
Click to ReviewThe NCCN Panel recommends active surveillance for all men with very-low-risk prostate cancer and a life expectancy of less than 20 years and believes that surveillance should be considered for men with very-low-risk prostate cancer and a life expectancy of 20 years or more [126]. In addition, the Panel recommends active surveillance for all men with low- and favorable intermediate-risk prostate cancer and a life expectancy of less than 20 years and believes that it should be considered for men with low- and favorable intermediate-risk and a life expectancy of 10 years or more [126]. With active surveillance, recommended monitoring is measurement of a PSA level no more than every 6 months, unless clinically indicated, and physical exam with DRE every 12 months [126]. An increase in PSA should prompt re-testing as transient PSA elevations are common; serial PSA increases, new DRE abnormalities, or other concerns for clinical progression should prompt re-evaluation with prostate MRI and possible prostate biopsy [126,358].
The recommended initial therapy for metastatic prostate cancer is
Click to ReviewBoth NCCN and ASCO recommend ADT as initial treatment for metastatic prostate cancer [126,155]. Researchers have evaluated the timing of ADT—early (before symptoms occur) or delayed—and early therapy has provided no overall survival benefit and only a modest decrease in risk for prostate cancer-specific mortality; because of this, the ASCO guideline does not make a recommendation for early ADT [155]. Several studies have demonstrated that intermittent ADT is as effective as continuous ADT for metastatic or locally advanced disease, with better quality of life and fewer side effects [156,157,158].
Which of the following is a distinctive sign of testicular torsion?
Click to ReviewThe most common misdiagnosis of testicular torsion is epididymitis [164,167]. The first step should be to determine the onset of pain, as testicular torsion is associated with pain of sudden onset; in contrast, the onset of pain is insidious in epididymitis and other conditions [164,165]. The physical examination also plays an important role in distinguishing testicular torsion from epididymitis. A key distinction is the absence of the cremasteric reflex in testicular torsion, which has been found to have a sensitivity of at least 99% in two studies of boys [167,168]. To elicit this reflex, the medial thigh is stroked or pinched, which causes contraction of the cremaster muscle and elevation of the testis. If the testicle moves at least 0.5 cm, the reflex is positive [164]. Other distinguishing features include the area of tenderness, appearance of the scrotum, and testicular lie (Table 9) [164,165,167,168].
The primary symptom associated with acute epididymitis is
Click to ReviewMen with acute epididymitis usually present with unilateral pain and tenderness in the testicle [173]. Additional symptoms include dysuria, urinary frequency or urgency, and symptoms related to the source of infection (e.g., fever, chills, or pain). Urinalysis and urine culture should be done to determine the presence of infection [175,176].
Varicoceles usually are
Click to ReviewA varicocele is a dilated, tortuous inflammation of the veins of the spermatic cord above the testicle. A prevailing thought has been that the superior mesenteric artery compresses the left renal vein over the aorta, also known as the "nutcracker effect" [178]. This theory has been confirmed by studies that have shown that varicoceles are less common in obese men [178,179]. It has also been suggested that the condition is caused by damage to the contractile mechanism of the smooth muscle organization of spermatic veins [180]. As a result of anatomic differences, the condition is more common in the left testicle, but advances in imaging have led to reports of high rates of bilaterality [181]. Varicocele can cause discomfort in the scrotal area, but usually the condition is asymptomatic [165].
The frequency of varicocele among adolescents and young adults is approximately 15% to 20%, and the rate is higher among men who have some level of infertility, with reports of 77% and 81% in some studies [181,182]. A study of older men (mean age: 60.7 years) demonstrated a prevalence of 42% [183].
Varicoceles vary in size, and large ones can be identified through physical examination alone. Varicoceles can have an adverse effect on spermatogenesis, and infertility has been associated with varicoceles that can be palpated [182]. The most significant finding is a feeling of a "bag of worms" when the scrotum is palpated [165,182]. The varicocele may disappear or be substantially reduced when the patient is recumbent [182]. Smaller varicoceles can be detected by asking the patient to perform the Valsalva maneuver in the standing position [182]. In older men (at least 60 years of age), varicoceles have been associated with significantly smaller and soft testes [183]. Color Doppler ultrasonography is the diagnostic procedure of choice when the findings of the clinical examination are inconclusive [182].
The primary risk factor for testicular cancer is
Click to ReviewAmong the several risk factors for testicular cancer, the primary one is cryptorchidism, which can increase the risk 11-fold [177]. Other risk factors include a family history of the disease, testicular dysgenesis, and Klinefelter syndrome [177]. A history of cancer in one testicle confers an increased risk (2% to 5%) of cancer in the contralateral testicle over the 25 years following diagnosis [192].
Nonseminoma testicular cancer is associated with an elevated
Click to ReviewAccording to the NCCN guideline for the treatment of testicular cancer, testicular ultrasonography is optional if a diagnosis is obvious from the physical examination, but the guideline notes that this diagnostic test is usually done to define the lesion [177]. Both the NCCN and ASCO recommend measuring serum levels of alpha-fetoprotein (AFP), human chorionic gonadotropin (beta-hCG), and lactate dehydrogenase (LDH) to help determine if the testicular mass is a germ cell tumor and, if so, whether it is a seminoma or a nonseminoma [177,194]. A nonseminoma is associated with an elevated AFP level; in contrast, an elevated level of beta-hCG, with a normal AFP level, usually indicates a seminoma [177]. Additional evaluation should include a chest x-ray and CT of the abdomen and pelvis to determine if lymph nodes are involved [177]. If metastatic disease is suspected, further imaging studies, such as bone scan, magnetic resonance imaging, or positron emission tomography, may be necessary. Open biopsy is not usually performed [177].
The primary adverse effect of chemotherapy for testicular cancer is
Click to ReviewThe follow-up evaluation plays an important role in assessing for the long-term effects of treatment. The primary effect of chemotherapy is oligospermia, but sperm production can be recovered [195,196]. A population-based study found that 70% of testicular cancer survivors fathered children [197]. Secondary acute leukemias have been reported to develop after chemotherapy and radiation therapy, and other consequences of platinum-based chemotherapy include hearing deficits and impaired renal function [198,199]. Melanomas and cancers at many sites have been associated with radiation therapy, occurring 10 years or more after treatment [198]. Lastly, the risk of cardiac events has been increased for testicular cancer survivors who had been treated with radiation therapy and/or chemotherapy [200].
Which of the following statements about male breast cancer is most accurate?
Click to ReviewBRCA2 mutation is found in approximately 4% to 16% of men with breast cancer [203].
A painless subareolar lump or swelling is the most common presenting symptom, occurring in approximately 85% of men with breast cancer [201,204]. Other common symptoms are nipple retraction, localized pain, or nipple ulceration, bleeding, or discharge. About 1% to 2% of men will have no symptoms [201,204]. In diagnosing male breast cancer, the primary consideration is to distinguish cancer from gynecomastia, which is present in about 30% of healthy men [202].
The approach to the diagnostic evaluation of male breast cancer is the same as for female breast cancer. A history and physical examination will help determine potential risk factors and identify the clinical features. Mammography has good sensitivity and specificity, and ultrasonography may be useful, especially for detecting involvement of the lymph nodes [202]. Biopsy is essential for elucidating the pathologic characteristics. In male breast cancers, the overexpression of estrogen receptor and progesterone receptors is likely [203,205].
As noted, data on male breast cancer are limited, and recommendations for treatment have been extrapolated from the literature on female breast cancer and from small series of men with the disease. Modified radical mastectomy is used most often, with lumpectomy rarely performed [203]. Sentinel node biopsy has also been effective in men [206,207]. Adjuvant radiation therapy has been associated with a lower local recurrence rate and a higher survival rate [202,203]. Adjuvant chemotherapy has been carried out according to guidelines for women at high risk for recurrence. Adjuvant hormone therapy has a clear role in the treatment of men with hormone receptor-positive cancer, with reductions in recurrence and death [204,208]. In addition, tamoxifen has led to a 50% response rate for metastatic breast cancer [202].
Premature ejaculation
Click to ReviewThe reported prevalence of premature ejaculation in the United States has varied widely, ranging from 5% to 40%, depending primarily on the definition [210,212]. The highest prevalence is found among men who are 60 years of age or older [214].
There are no established criteria for the diagnosis of premature ejaculation; clinicians should assess medical, relationship, and sexual history and perform a focused physical examination to make the diagnosis [354]. Laboratory studies or physiologic testing is needed only if the history or physical examination suggests a complex cause [212,354]. Among the details to be elicited from the history are [212]:
Frequency and duration of premature ejaculation
Relationship of premature ejaculation to specific partners
Degree of stimulus resulting in premature ejaculation
Nature and frequency of sexual activity (foreplay, masturbation, intercourse, use of visual cues)
Impact of premature ejaculation on sexual activity
Types and quality of personal relationships and quality of life
Aggravating or alleviating factors
Relationship to drug use or misuse
The patient's partner may be helpful in providing a description of the problem, and care should be taken to distinguish premature ejaculation from erectile dysfunction [212]. The AUA recommends that, for men with concomitant premature ejaculation and erectile dysfunction, erectile dysfunction should be treated first [212].
The treatment approaches for premature ejaculation include psychologic, behavioral, and pharmacologic therapies, and the risks and benefits of all options should be discussed with the patient and, when possible, his partner [212,354]. Behavioral therapy was once considered to be the standard therapy, but studies have shown that the best approach may involve a combination of therapies to address the limitations of each approach as well as the multimodal causes of premature ejaculation [210,217,218]. The 2022 AUA/Sexual Medicine Society of North America guideline recommends that, in addition to pharmacologic treatment, providers consider referring men with premature ejaculation to a mental health professional with expertise in sexual health [354].
No medication has been approved for the treatment of premature ejaculation, leaving the pharmacologic treatment to involve the off-label use of serotonin reuptake inhibitors or topical anesthetics that act by prolonging the latency of ejaculation [210,212,218,219,354]. The recommended first-line pharmacotherapeutic options are "on demand" clomipramine; a nonselective serotonin reuptake inhibitor; daily selective serotonin reuptake inhibitor (e.g., fluoxetine, paroxetine, sertraline); and topical penile anesthetics [212,354]. The doses studied have varied, and dosing is prescribed as either continuous (daily regimen) or situational (taken only before sexual activity); the optimal duration of therapy has not been determined (Table 10) [212,354]. The side effects of these drugs have not been evaluated outside the depression setting, but the effects appear to be similar for men who are not using the drug for depression, with the most common effects being nausea, dry mouth, and drowsiness [212].
Which of the following has the strongest association with erectile dysfunction?
Click to ReviewErectile dysfunction has been reported to be more common among men with comorbidities; independent risk factors include age, diabetes, metabolic syndrome, cardiovascular disease, obesity, and sedentary lifestyle [214,234,235]. Among men with no known cardiovascular disease, erectile dysfunction has preceded coronary artery disease, stroke, and peripheral artery disease by an average of three years (range: two to five years) [236]. In addition, a meta-analysis (14 cohort studies; 92,757 men) showed that erectile dysfunction was an independent risk factor for cardiovascular and cerebrovascular events [237]. Other risk factors for erectile dysfunction include hormone disorders, neurologic conditions, psychologic disorders, history of surgery or radiation in the pelvic region, use of illicit drugs, and some prescription drugs (most notably, antihypertension agents) [238]. Encouraging men with these risk factors to modify their lifestyle and/or treating comorbidities may help reduce the risk of erectile dysfunction [239].
All four phophodiesterase-5 inhibitors used for treatment of erectile dysfunction are similar with respect to
Click to ReviewAfter treatment of erectile dysfunction is initiated, referral to a mental health professional should be considered to promote treatment adherence, reduce performance anxiety, and integrate therapies into a sexual relationship [355]. Both the AUA and the ACP recommend oral phosphodiesterase-5 inhibitors as first-line pharmacotherapy for erectile dysfunction in men for whom this class of drugs is not contraindicated [230,231,355]. Four drugs in the class have been approved for use in the treatment of erectile dysfunction: sildenafil (Viagra), tadalafil (Cialis), vardenafil (Levitra), and avanafil (Stendra, Spedra). Sildenafil and vardenafil differ from tadalafil with respect to the time to maximum serum level (1 hour vs. 2 hours) and serum half-life (4 hours vs. 18 hours) [230]. Furthermore, the duration of action is longest for tadalafil (up to 36 hours) [240]. The inhibitory effect of these drugs causes vascular smooth muscle relaxation in the corpus cavernosum, resulting in increased erection hardness and prolonged duration in men with erectile dysfunction who have sufficient intact vasculature [355].
Data from multiple trials and systematic reviews have demonstrated similar efficacy for phosphodiesterase-5 inhibitors in treating erectile dysfunction, particularly for sildenafil, tadalafil, and vardenafil [355]. Each of these drugs substantially improves erectile function and successful sexual intercourse compared with placebo [231]. Relative efficacy is less clear for avanafil because published comparative studies are limited. The ACP notes that there is insufficient evidence for recommending one drug over another and suggests that the choice be made according to the preferences of an individual patient with respect to ease of use, cost, and the adverse effects profile [231]. One systematic review and meta-analysis found evidence that tadalafil is the most effective agent, followed by vardenafil, with no major differences in the safety profile of any of the phosphodiesterase-5 inhibitors [241].
The side effects of all four drugs are similar, with headache, dyspepsia, facial flushing, nasal congestion, and visual disturbances being the most common events [230,240,242]. The FDA has issued two mandates to revise labeling of these agents. In 2005, the agency required labels for sildenafil, tadalafil, and vardenafil to reflect the possibility of sudden vision loss after taking the drugs for a period of time [243]. The alert was associated with several case reports suggesting a temporal association between use of one of the drugs and nonarteritic anterior ischemic optical neuropathy (NAION), a rare disorder characterized by sudden loss of vision in one eye [243,355]. However, subsequent studies showed that the risk of NAION was similar among men who were and were not taking a phosphodiesterase-5 inhibitor [244,245]. Risk factors for spontaneous NAION include older age, White race, small optic discs with low cup-to-disc ratio, and vascular disease, leading some investigators to suggest an examination of the fundus be performed on men who may be at higher risk for NAION before a phosphodiesterase-5 inhibitor is prescribed [243].
Treatment with a phosphodiesterase-5 inhibitor is contraindicated for patients who take
Click to ReviewUse of a phosphodiesterase-5 inhibitor is contraindicated in several situations. They should not be taken by men who take organic nitrates (nitroglycerin) or nitrites (amyl nitrite) [248,249]. Vardenafil should not be used for men with a history of prolonged QT interval (or who take medication to prolong the QT interval) [230]. The use of a phosphodiesterase-5 inhibitor concomitantly with an alpha-blocker for lower urinary tract symptoms may lead to increased systemic vasodilation and hypotension [230].
Late-onset hypogonadism is
Click to ReviewIn both men and women, levels of sex hormones decline with age. However, the ways in which these levels change and the symptoms associated with the decline differ greatly between men and women. There is no well-defined equivalent of menopause in men, although the phrase "andropause" is used frequently to refer to decreased testosterone and resulting symptoms. Other phrases, most notably androgen deficiency syndrome and late-onset hypogonadism, may be more accurate descriptors of the process. By any name, the condition is a complex of symptoms that includes loss of sexual satisfaction and overall well-being [251]. The condition is related to lower testosterone levels, which begin to decrease 1% to 2% each year beginning at 30 years of age [252].
Late-onset hypogonadism is distinct from hypogonadism in younger male individuals. For boys and young men, hypogonadism is related to testicular failure and is usually associated with a congenital abnormality, most often Klinefelter syndrome [251]. In older men with hypogonadism, testosterone levels are rarely as low as the levels in young men with primary hypogonadism [251].
Several important questions about late-onset hypogonadism remain unanswered [252,253]:
It is unclear whether the symptoms are caused by a reduction in testosterone or are a result of the normal physiologic process of aging.
There is no consistent level of testosterone to define hypogonadism, and there is confusion about what testosterone levels should be measured.
There is ongoing debate about the risk-benefit ratio of testosterone therapy for older men.
According to guidelines from the Endocrine Society, which of the following statements about testosterone therapy is TRUE?
Click to ReviewRECOMMENDATIONS OF THE ENDOCRINE SOCIETY REGARDING TESTOSTERONE THERAPY FOR ADULT MEN WITH HYPOGONADISM
Diagnosis and evaluation Recommendations Make a diagnosis of hypogonadism only in men with symptoms and signs consistent with testosterone deficiency and unequivocally and consistently low serum testosterone levels and/or free testosterone concentrations (when indicated). Confirm diagnosis by repeating measurement of fasting morning total testosterone. Measure serum luteinizing hormone and follicle-stimulating hormone levels to distinguish between primary (testicular) and secondary (pituitary-hypothalamic) hypogonadism. Suggestions Perform further evaluation to identify the etiology of hypothalamic, pituitary, and/or testicular dysfunction in men with hypogonadism. Measure serum testosterone level in men who have specific clinical signs and symptoms and consider measuring serum testosterone level in men who report less specific signs and symptoms. Measure morning total testosterone level by a reliable assay as the initial diagnostic test. Measure free or bioavailable testosterone level, using an accurate and reliable assay, in men in whom total testosterone concentrations are near the lower limit of the normal range and in whom alterations of sex hormone-binding globulin are suspected. Do not evaluate androgen deficiency during an acute or subacute illness. Measure bone mineral density with use of dual-energy x-ray absorptiometry scanning in men with severe androgen deficiency or low trauma fracture. Treatment Recommendations Use testosterone therapy for men with hypogonadism to induce and maintain secondary sex characteristics and correct symptoms of testosterone deficiency. Do not use testosterone therapy for men planning fertility in the near term or in men with breast or prostate cancer. Do not use testosterone therapy without further urologic evaluation in men with palpable prostate nodule or induration or a prostate-specific antigen (PSA) level of 3 or 4 ng/mL in men at high risk of prostate cancer (e.g., Black race, first-degree relative with prostate cancer). Do not use testosterone therapy for men with a hematocrit greater than 50%, untreated severe obstructive sleep apnea, severe lower urinary tract symptoms, or uncontrolled or poorly controlled heart failure, or in men with type 2 diabetes (as a means of glycemic control) who have low testosterone concentrations. Suggestions Initiate testosterone therapy with any of the following regimens, chosen on the basis of an individual man's preference, consideration of pharmacokinetics, treatment burden, and cost: Testosterone enanthate or cypionate: 75–100 mg IM weekly, or 150–200 mg IM every two weeks
Testosterone patch (nongenital): 5 mg, one or two applied nightly over the skin of the back, thigh, or upper arm (away from pressure areas)
Testosterone gel (1%): 5–10 g applied daily over a covered area of nongenital skin
Testosterone bioadhesive buccal tablet: 30 mg applied to buccal mucosa every 12 hours
Testosterone pellets: SC every three to six months (dose and regimen vary with the formulation used)
Oral testosterone undecanoate, injectable testosterone undecanoate, testosterone-in-adhesive matrix patch, and testosterone pellets, where available
Consider short-term testosterone therapy in men with HIV, low testosterone concentrations, and weight loss (when other causes of weight loss have been excluded) to induce and maintain body weight and lean mass gain. Do not routinely prescribe testosterone therapy to all men 65 years of age or older with low testosterone concentrations. Offer testosterone therapy on an individualized basis after discussing the risks/benefits with the patient. Monitoring Recommendations Evaluate the patient three to six months after the initiation of treatment and then annually. Determine hematocrit at baseline, at three to six months, and then annually. (Stop therapy if the hematocrit is higher than 54%.) Evaluate the patient for signs and symptoms of formulation-specific adverse events at each visit. Obtain a urologic consultation if there is any of the following: Increase in serum or plasma PSA level >1.4 ng/mL within any 12-month period of testosterone treatment
PSA velocity >0.4 ng/mL/yr using the PSA level after 6 months of testosterone therapy as the reference (PSA velocity should be used only if there are longitudinal PSA data for more than two years.)
Detection of a prostatic abnormality on digital rectal examination
AUA/IPSS score >19
Suggestions Monitor testosterone levels three to six months after initiation of testosterone therapy, with an aim of achieving serum testosterone levels during treatment in the mid-normal range. (For men receiving testosterone enanthate or cypionate, the aim should be a testosterone level between 350 and 600 ng/dL at one week after the injection.) Repeat bone mineral density of the lumbar spine, femoral neck, and hip after one to two years of testosterone therapy in hypogonadal men with osteoporosis or low trauma fracture. Screening Recommendation Do not screen for hypogonadism in the general population. Male infertility
Click to ReviewInfertility is clinically defined as the inability to conceive after one year of unprotected intercourse [264]. Approximately 15% of couples are unable to conceive after one year of unprotected intercourse. A male factor is the only cause in approximately 20% of infertile couples and is a contributing factor in another 20% to 40% [264]. Fertility declines with age, and research has shown that men older than 35 years of age are twice as likely to be infertile as men younger than 25 years of age [265,266]. Approximately 15% of infertile men have azoospermia, the complete absence of sperm in the ejaculate [267].
More than half of male infertility or subfertility is potentially correctable; often, the cause is unknown. The causes, both correctable and uncorrectable, include [264,268]:
Varicocele
Obstruction of a duct (epididymal, vasal, or ejaculatory)
Ejaculatory dysfunction
Testicular atrophy
Hypogonadotropic hypogonadism
Infection
Side effects of medication
Environmental toxins
Bilateral cryptorchidism
Genetic abnormality (Y chromosome microdeletion)
Congenital absence of vas deferens
Which of the following statements about the screening and prevention of STIs for men is TRUE?
Click to ReviewRecommendations for screening vary according to risk and the type of STI (Table 15) [284]. The USPSTF also recommends high-intensity behavioral counseling for all sexually active adolescents and for adults at increased risk for STIs and HIV [284]. The USPSTF has not issued recommendations for screening for HPV, but beginning in 2011, the Advisory Committee on Immunization Practices (ACIP) recommended HPV vaccination for male individuals [276]. The ACIP recommends routine use of quadrivalent HPV vaccine for boys 11 or 12 years of age and for male individuals 13 to 26 years of age who have not initiated or completed the three-dose series [276,286]. The ACIP also notes that men 27 to 45 years of age may also be vaccinated if at high risk, as determined through shared decision-making [276,285,286]. In addition, hepatitis B vaccination is recommended for any patient who is being evaluated for an STI [173].
U.S. PREVENTIVE SERVICES TASK FORCE RECOMMENDATIONS FOR SCREENING FOR SEXUALLY TRANSMITTED INFECTIONS (STIs) IN MALE INDIVIDUALS
STI Recommendation Chlamydia and gonorrhea Insufficient evidence to recommend for or against screening in men Syphilis Strongly recommend screening for individuals at increased risk Genital herpes No screening for asymptomatic adults and adolescents According to the CDC, men who are evaluated for gonorrhea should also be evaluated for infection with
Click to ReviewThe CDC recommends that all individuals who are evaluated for gonorrhea should also be evaluated for chlamydia, syphilis, and HIV infection [173]. In one study of more than 3,800 men and women, approximately 10% to 30% of individuals with gonorrhea had concomitant infection with chlamydia [290]. The typical lesions of genital HSV-2 in men appear on or around the penis and are first noted as either a single or multiple erythematosus macular lesion(s). However, these lesions are absent in many infected individuals [173]. Viral culture is the preferred test for the diagnosis of HSV-2, but it requires two to seven days for results. The sensitivity of viral culture depends on the quality of the sample and the time at which the sample is obtained; sensitivity declines as the lesion begins to heal. A PCR test is available and is suggested by the CDC for analysis of cerebrospinal fluid when central nervous system disease is suspected [173]. Type-specific serologic tests are available as laboratory assays and point-of-care tests [173]. These tests have varying degrees of sensitivity for the detection of the HSV-2 antibody (80% to 90%) and specificity of at least 96% [173].
Which of the following is recommended by the CDC for the treatment of gonorrhea?
Click to ReviewTREATMENT OF CHLAMYDIA, SYPHILIS, AND GONORRHEA AS RECOMMENDED BY THE CENTERS FOR DISEASE CONTROL AND PREVENTION
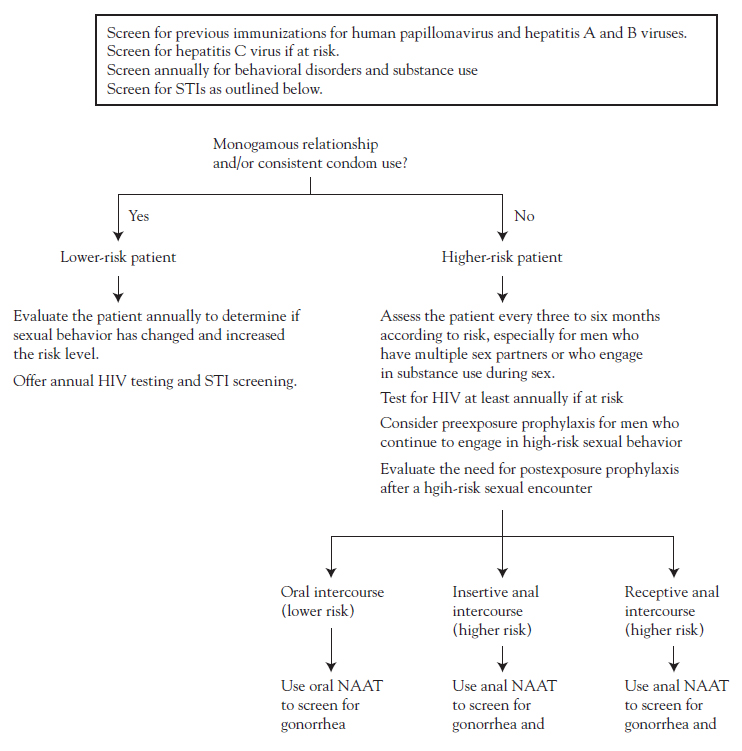
Infection Recommended Treatment Notes Chlamydia Doxycycline 100 mg orally twice daily for 7 days ALTERNATIVE REGIMENS Azithromycin 1 g orally in a single dose OR Levofloxacin 500 mg orally once daily for 7 days A meta-analysis showed treatment failure among men was higher for azithromycin than for doxycycline. Gonorrhea Ceftriaxone 500 mg IM (single dose) PLUS Doxycycline 100 mg PO twice daily for seven days, unless chlamydia infection has been excluded For persons weighing >150 kg, 1 g ceftriaxone should be administered. See guideline for alternative cephalosporin selection and dosing if ceftriaxone is not available. Primary and secondary syphilis Benzathine penicillin G 2.4 million units IM (single dose) Additional doses do not enhance efficacy. For patients allergic to penicillin, alternative regimens include doxycycline (100 mg PO, twice daily for 14 days) or tetracycline (500 mg PO, four times daily for 14 days) According to Figure 3, which of the following statements about screening for men who have sex with men is TRUE?
Which of the following statements about substance misuse is TRUE?
Click to ReviewAs noted, substance misuse is higher among men than among women in all age categories, and men are more likely to have psychosocial problems related to the misuse [28,307]. Although the rate of alcohol misuse is highest among younger men, men older than 65 years of age are of special concern because they are much more likely than women to be "problem" drinkers and to misuse a wide range of illicit as well as prescription drugs [307]. As the general population ages, the misuse of illicit drugs is expected to increase [314]. Adding to this problem is the low rate of screening for alcohol misuse in the older population and the secrecy of many men about drug use [314,315].
The alcohol screening tool that is most accurate for detecting problem drinking is the
Click to ReviewSeveral professional organizations, including the USPSTF, recommend screening and behavioral counseling intervention to reduce alcohol misuse [318]. However, reported rates of screening have been low [319]. Several screening instruments have been developed, and they vary in the number of questions, the populations for which they are best suited, and their usefulness in specific situations; no one tool is perfect [320,321,322,323]. The CAGE questionnaire, which includes four questions, is best for detecting alcohol dependency and is easy and quick to perform [320,321]. However, the test may not detect low, but risky, levels of drinking [307,324]. The Alcohol Use Disorders Identification Test (AUDIT) is the most accurate for detecting problem drinking [319,322].
The depression treatment approach that offers the best results for most men is
Click to ReviewThe treatment approach will depend on the severity of symptoms and the patient's preference. In general, a combination of psychotherapy and pharmacologic management provides the best results for most men [328,335]. Potential psychotherapy approaches include cognitive behavior therapy and interpersonal psychotherapy [300,307,328]. First-line pharmacologic treatment involves the use of selective serotonin reuptake inhibitors, such as paroxetine, sertraline, and fluoxetine [307]. This treatment approach has efficacy rates of 30% to 70% [328]. Clinicians should emphasize the importance of taking the medication as prescribed, as it may be two to four weeks before a benefit is evident [328]. Depression that is associated with chronic illness is often seen as an inevitable consequence of the disease, but the depression should be treated. Frequently, the treatment improves the overall outcome [335].
A study has shown that which of the following may be effective for educating younger men about health issues?
Click to ReviewAs a result of men's reluctance to seek help, educational strategies that provide anonymity may be particularly well-suited for them [45,339]. Print resources should be distributed through a variety of venues that men frequent, such as the workplace, schools, religious organizations, sports arenas, men's organizations or clubs, pubs, supermarkets, car and motorbike dealerships, and barbershops [45,339,340]. In addition, digital media may be effective, especially for younger men. A study showed that 90-second educational video clips on men's health, sent by e-mail, were well-received [341].
For a heterosexual man 32 years of age with no recognized risk factors, which of the following assessments/screenings should be completed at each routine examination?
Click to ReviewRECOMMENDATIONS AND SUGGESTIONS FOR HEALTH ASSESSMENTS, SCREENING, AND COUNSELING FOR MEN
Intervention Suggested Frequency Relevant Ages (Years) Recommending Body/Source Routine physical examination (with determination of height, weight, and body mass index) Every 3 to 5 years 18 to 39 — Every 1 to 2 years 40 to 49 Yearly 50 and older Blood pressure screening Every 1 to 2 years, depending on blood pressure Beginning at 18 USPSTF Cholesterol level/lipid profile At least every 5 years 40 to 75 (earlier if at increased risk) USPSTF Diabetes (type 2) and prediabetes screening Every 3 years 35 to 70 in men with overweight or obesity USPSTF Cancer-related check-up (for cancer of the thyroid, testicles, lymph nodes, oral cavity, and skin) At each routine examination Beginning at 20 ACS Assessment, Counseling, and Behavioral Interventions as Appropriate Tobacco use At each routine examination All men USPSTF Alcohol use At each routine examination All men USPSTF Drug (illicit) use At each routine examination All men ASAM Depression At each routine examination, when staff-assisted depression care supports are in place All men USPSTF Counseling Healthy diet At each routine examination Men with risk factors for cardiovascular disease and diet-related chronic diseases USPSTF Exercise At each routine examination All men AAFP, AMA, AHA, CDC Sun avoidance and use of sunscreen At each routine examination All men ACS, AAD, NIH Consensus Panel Skin examination for melanoma At each routine examination All men ACS Avoidance of sexually transmitted infections At each routine examination All sexually active men at increased risk CDC Risk of HIV infection At each routine examination All men who have sex with men AAFP Risk for hepatitis A and B At each routine examination All men who have sex with men and others at high risk AAFP Sexual health At each routine examination All men AAFP Screening Colorectal cancer Every 1 to 10 years, depending on risk and test used 45 to 75 USPSTF Osteoporosis At each routine examination By 65 ACP HIV Not established (encourage men to be tested) 15 to 65 (younger and older men at increased risk) USPSTF Visual acuity (comprehensive eye examination) Yearly Beginning at 65 AAO Abdominal aortic aneurysm (ultrasonography) Once 65 to 75 (men who have ever smoked) USPSTF Immunizations Tetanus, diphtheria, pertussis (Td/Tdap) Once (Tdap), with booster (Td or Tdap) every 10 years All men ACIP Influenza vaccine Yearly All men ACIP Pneumococcal vaccine Once 65 and older (19 to 64 if risk) (one or two doses, depending on vaccine) ACIP Hepatitis A Once All men, if risk factors are present (2 or 3 doses, depending on vaccine) ACIP Hepatitis B Once 19 to 59, and 60 and older if risk factors are present (2, 3, or 4 doses, depending on vaccine or condition) ACIP Human papillomavirus (HPV) Once 19 to 26 (2 or 3 doses depending on age at initial vaccination and condition) 26 to 45, if desired based on shared clinical decision making ACIP Zoster (shingles) Once 50 and older or younger if risk factors present (2 doses) ACIP Haemophilus influenzae type b (Hib) Once All men, if risk factors present (1 or 3 doses depending on indication) ACIP Meningococcal A, C, W, Y Once All men, if risk factors present (1 or 2 doses depending on indication) ACIP Meningococcal B Once All men, if risk factors present (2 or 3 doses depending on vaccine and indication) ACIP
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.