Study Points
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.
Study Points
Click on any objective to view test questions.
- Describe cardiac conduction and the components of an ECG waveform.
- Use your knowledge of the pathophysiology of atrial fibrillation, including key defining characteristics, to differentiate it from other arrhythmias and predict impact on normal functioning.
- Outline common cardiac and noncardiac causes of atrial fibrillation.
- List key clinical data, including subjective symptoms, past medical history, physical assessment findings, and diagnostic/laboratory tests, important to obtain when assessing a patient with atrial fibrillation.
- Identify key components that should be considered in the development of the medical plan of care, including the issue of generic drug substitution.
- Compare and contrast antiarrhythmic medications appropriate to use for acute and chronic rate control for patients with atrial fibrillation.
- Outline the use of pharmacologic therapy in the restoration of normal sinus rhythm, including indications for use and procedure for administration.
- Describe electrical cardioversion, including indications and pre- and postprocedure care.
- Discuss antiarrhythmic medications that may be used to maintain normal sinus rhythm in a patient following successful spontaneous, electrical, or pharmacologic cardioversion.
- Select appropriate pharmacologic measures that may be used to reduce risk of thromboembolic events in persons with atrial fibrillation.
- Discuss the use of radiofrequency ablation of the atrioventricular (AV) node in the clinical management of atrial fibrillation.
- Describe the causes and recommended management of atrial fibrillation in adult patients following coronary artery bypass graft surgery and in patients with Wolff-Parkinson-White syndrome.
- Using simulated case study data, develop a best practice strategy for the clinical management of atrial fibrillation.
In the normal heart, the speed of conduction is slowed in the
Click to ReviewIn the normal heart, the heartbeat is initiated by the sinoatrial (SA) node. From the SA node, the electrical impulse travels through both the right and left atria, causing depolarization of the atria. Atrial depolarization is followed by atrial contraction and atrial repolarization. The electrical impulse travels from the atria to the atrioventricular (AV) node located in the inferior wall of the right atrium. The speed of conduction slows in the AV node to allow time for the atria to depolarize, contract, and complete ventricular filling. From the AV node, the electrical impulse travels through the bundle of His located in the septum of the heart. The bundle of His divides into the right and left bundle branches. These branches divide further into the smaller fibers of the Purkinje system. Electrical conduction through the His-Purkinje system is rapid, causing rapid depolarization of both the right and left ventricles. Depolarization of the ventricular cells spreads from the apex of each ventricle to the base and moves from the endocardium to the epicardium. Ventricular depolarization is followed by ventricular contraction and ventricular repolarization [9,10,11].
A prolonged QT interval indicates
Click to ReviewWhen changes occur in the normal cardiac cycle, the normal ECG waveform is altered to reflect them. For example, prolonged repolarization is reflected in a prolonged QT interval. A slowing of conduction from the SA node through the AV node may be reflected in a prolonged PR interval. Abnormal conduction of the electrical impulse through the ventricles results in a QRS interval that is wider than usual or bizarre in shape. Careful analysis of the changes in a patient's ECG can provide valuable information in the diagnosis and treatment of the arrhythmia [6,15].
Of the following, which is a key defining characteristic of atrial fibrillation?
Click to ReviewThe two key defining characteristics of atrial fibrillation are (Figure 2) [5,17,19]:
Total absence of normal sinus P waves. The absence of P waves indicates that the heartbeat was not initiated in the SA node, or normal pacemaker, of the heart. The P waves are replaced by fibrillatory (fib) waves. These fib waves may be so fine that they are indiscernible or barely discernible; or, they may be very coarse and more clearly seen on the ECG tracing.
An irregularly irregular ventricular response when conduction through the AV node is normal.
A key characteristic that can differentiate AV nodal re-entrant tachycardia from atrial fibrillation is
Click to ReviewIn AV nodal re-entrant tachycardia, the ventricular rate falls between 150 and 250 bpm. Because of the abrupt onset and termination of the re-entrant SVT, the nonspecific term paroxysmal supraventricular tachycardia has been used to refer to these tachyarrhythmias. With improved knowledge of the electrophysiology of re-entrant SVT, greater specificity in nomenclature, based on the mechanisms of re-entry, has been possible [30]. With AV nodal re-entrant tachycardia, no evidence of atrial activity is present. The ventricular rhythm is regular. The arrhythmia has an abrupt onset and termination, with episodes lasting from seconds or minutes to days, and may occur in persons with no history of heart disease as well as in elderly persons with chronic heart disease. The arrhythmia may be differentiated from sinus tachycardia by rate; sinus tachycardia rarely exceeds a rate of 150 to 160 bpm in an adult at rest. It may also be differentiated from atrial fibrillation because the rhythm is regular. It may be differentiated from atrial flutter by rate; the usual rates associated with AV nodal re-entrant tachycardia are too slow for 1:1 (atrial to ventricular) conduction in atrial flutter and too fast for 2:1 conduction [17,30].
Cardiac problems linked to the development of atrial fibrillation include which of the following?
Click to ReviewAs a secondary arrhythmia, atrial fibrillation may be caused by cardiac and noncardiac causes. Common cardiac causes include [37,38,39]:
Hypertension
Rheumatic heart disease
Mitral valve disease (e.g., mitral stenosis, mitral valve prolapse, mitral valve annular calcification)
Congestive cardiomyopathy/congestive heart failure
Acute myocardial infarction
Sick sinus syndrome
Pericarditis
Hypertrophic cardiomyopathy
May occur following cardiac/coronary artery bypass graft (CABG) surgery
One noncardiac cause linked to the development of atrial fibrillation is
Click to ReviewThe persons at highest risk to develop atrial fibrillation are those with long-standing hypertension, valvular heart disease, left ventricular hypertrophy, depressed left ventricular function, and coronary artery disease. Atrial fibrillation associated with cardiovascular disease may initially have a paroxysmal onset; however, the arrhythmia can continue to progress to persistent or chronic atrial fibrillation. Noncardiac, systemic diseases may also cause atrial fibrillation. Diabetes mellitus is a major risk factor for the development of atrial fibrillation. Other noncardiac causes include [2,37,38,39]:
Hyperthyroidism
Male sex
Advancing age
Obesity
Obstructive sleep apnea
Genetic factors
Alcohol and drug use
Noncardiac surgery
Noncardiac diagnostic procedure
Pulmonary conditions/hypoxemia caused by pulmonary conditions (e.g., pneumonia, chronic obstructive pulmonary disease [COPD])
Pulmonary embolus
Over-the-counter use of some herbs, such as ephedra or ginseng
A physical assessment finding commonly associated with atrial fibrillation is
Click to ReviewPhysical assessment findings in atrial fibrillation may include the following [28,37]:
Rapid heart rate and irregularly irregular heart rhythm
Irregular jugular venous pulsations
Variable loudness of S1
Variable pulse pressure. This results from the variable ventricular filling caused by the irregular conduction of atrial impulses through the AV node to the ventricles.
A blood pressure that appears to vary widely. In atrial fibrillation with a controlled or slow ventricular response, there may be long pauses between some beats. When an electronic, noninvasive blood pressure device is used (or when the pressure is released too rapidly during manual auscultation of blood pressure), the systolic blood pressure reading may vary widely. Taking serial blood pressure readings and using an average of readings to estimate the patient's actual blood pressure may be needed.
Hypotension, especially if cardiac output is significantly reduced
Signs of congestive heart failure, such as decreased oxygen saturation and rales/crackles in lung fields
Signs of poor peripheral perfusion, such as diminished peripheral pulses and impaired capillary filling
The initial goal for a patient with atrial fibrillation with a rapid ventricular response is
Click to ReviewBased on a thorough evaluation of the patient's status and other factors, one or more medical goals should be identified. The initial goal for a patient who is hemodynamically unstable is the immediate restoration of normal sinus rhythm through electrical cardioversion. The initial goal for patients who present with atrial fibrillation with a rapid ventricular response is rate control. Once the patient's status has stabilized, long-term goals may be developed. When developing long-term goals, consider the following points [17,28,40,45,46,47,48,49]:
Use of antiarrhythmic therapy may not be necessary for persons with asymptomatic paroxysmal atrial fibrillation.
Use of antiarrhythmic therapy is indicated for persons who experience severe symptoms with paroxysmal atrial fibrillation.
Long-term rate control is indicated for persons with paroxysmal, persistent, or permanent atrial fibrillation.
Long-term rate control is also indicated for patients who have repeatedly reverted to atrial fibrillation following electrical or pharmacologic cardioversion. Ablation for symptomatic persistent atrial fibrillation and for severely symptomatic recurrent atrial fibrillation may be indicated. AV nodal ablation is usually reserved for elderly patients, because it leads to pacemaker dependency.
Catheter ablation performed in experienced centers may be indicated to maintain sinus rhythm in select patients with significantly symptomatic, paroxysmal atrial fibrillation who have failed treatment with an antiarr-hythmic drug and have normal or mildly dilated left atria, normal or mildly reduced LV function, and no severe pulmonary disease.
Catheter ablation is indicated for symptom-atic patients with atrial fibrillation who have Wolff-Parkinson-White (WPW) syndrome. Prompt direct-current cardioversion is recommended for patients with WPW syndrome and rapid ventricular response who are hemodynamically compromised.
Restoration of normal sinus rhythm is indicated for those who have persistent signs of decreased cardiac output during episodes of atrial fibrillation.
Direct-current cardioversion may be indicated as part of a long-term management strategy to restore sinus rhythm in patients with atrial fibrillation.
Maintenance of normal sinus rhythm may be indicated for persons who spontaneously convert from atrial fibrillation to sinus rhythm.
Maintenance of normal sinus rhythm is indicated for persons who are successfully converted by pharmacologic or electrical means.
Elimination or interruption of the arrhythmia through radiofrequency ablation (of the focal source of the arrhythmia or the AV node) is indicated for patients who cannot tolerate antiarrhythmic therapy, whose arrhythmia is not successfully controlled by optimal doses of antiarrhythmic therapy, or who cannot be successfully cardioverted through pharmacologic or electrical means. Some patients with atrial fibrillation who also have atrial flutter may benefit from treatment with radiofrequency ablation.
To receive FDA approval, a generic medication must meet all of the following criteria, EXCEPT:
Click to ReviewWhen a pharmaceutical company develops a new drug, the company may apply for one or more patents for (1) the drug itself; (2) the manufacturing process; (3) how the drug is delivered to the bloodstream; or (4) how the medication is to be used. Although the patent gives the company exclusive rights to the new drug for 17 years, this period often involves at least 10 years of development. In reality, the company may have only seven years to exclusively sell the drug. A newly developed drug is given several names. The generic name, which is the medication's official name (derived from the drug's chemical name, structure, and/or formula), must be unique. Generic names are frequently difficult to pronounce, remember, and spell. The new drug is also given a trade name or proprietary name that signifies that the drug is the exclusive property of its company. Trade names are simpler, easier to remember, and often emphasize an attribute of the medication. Trade names must also be unique. After the patent on a specific drug has expired, other companies may manufacture and sell that drug under its generic name. Generics are frequently sold at a lower price than trade/proprietary drugs. Generic versions of a drug must meet FDA approval, specifically the following three points [51,52]:
The generic preparation must contain the same amount of active drug ingredient as the original proprietary preparation.
The generic must be manufactured according to federal standards as defined in the Good Manufacturing Practices.
In the human body, the generic medication must be released in equivalent fashion (i.e., same rate, to same extent) as the proprietary drug. This is referred to as "bioequivalence." Bioequivalence is established by a drug company through the use of small research studies. For time-release medications, the process of establishing bioequivalence is more strict, extensive, and time-consuming. Because there is more variation inherent in the use of time-release forms, more extensive testing is required to ensure bioequivalence. Because of the cost and extensiveness of the process, very few time-release generic drugs are available.
Proprietary and generic versions of a medication may vary in several respects [33,52]:
Appearance of the medication. By law the size, color, and shape of the generic must significantly differ from the proprietary. Patients will notice the difference.
Different inactive ingredients. While the active ingredients must be the same, the inactive components may vary. Inactive ingredients are routinely used in medications to add bulk, to keep the tablet from crumbling/disintegrating until use, to help the medication dissolve, or to provide a pleasant taste. There have been instances in which the difference in inactive ingredients has changed the absorption of the active ingredients.
Variable bioequivalence. Regulations permit as much as a 20% variation in bioequivalence. For medications, such as antiarrhythmic medications that may have a very narrow margin for therapeutic effect, this variation may alter how effective the generic medication is in managing the patient's arrhythmia.
Which of the following is a recommendation with regard to the use of generic medications for antiarrhythmic therapy?
Click to ReviewPractically speaking, the use of a generic substitution means that the patient could experience different effectiveness with different preparations. Random switching from proprietary to generic or from one generic to another could increase side effects, decrease rate control, and cause more frequent relapse from normal sinus rhythm to atrial fibrillation. For that reason, any generic substitution of antiarrhythmic medications should be done very carefully. With many antiarrhythmic medications, very small variations in the serum blood level may influence the effectiveness of the medication in controlling the arrhythmia and significantly increase the risk of proarrhythmias and serious side effects. Physician groups have made the following recommendations regarding the use of generic antiarrhythmic medications [46]:
Regardless of the preparation used, closely monitor the patient's status and serum drug levels. Adjust dosage as indicated by data.
Avoid substitution of antiarrhythmic medications for patients with life-threatening arrhythmias, arrhythmias that cause loss of consciousness, or when a change in drug level (increase) can cause life-threatening proarrhythmias.
Use a generic for less serious arrhythmias if an easy, reliable assay is available and a therapeutic drug level is stable and sustained over time.
If generic substitution is necessary, give preference to generic medications that have only one preparation available, thus avoiding multiple switches from one generic product to another. Also give preference to a generic preparation that is widely available in hospital and outpatient pharmacies.
If switching from a proprietary to a generic medication, re-establish effectiveness and proper dose with the new preparation.
The physician may wish to specify on the prescription the exact preparation of a medication to be dispensed. Some states have regulations that limit the physician's ability to specify preparations. Also, specifying a proprietary medication may present a financial issue for the patient; insurance companies may not cover the higher cost preparation.
For persons in atrial fibrillation with a rapid ventricular response, the usual IV bolus dose of diltiazem is
Click to ReviewDiltiazem acts by blocking calcium transport into the myocardial and vascular smooth muscle cells. As a result, conduction through the SA and AV nodes is slowed, and the refractory period of the AV node is prolonged. Ventricular rate is slowed, but the underlying atrial arrhythmia is not corrected. Diltiazem should be administered initially as an IV bolus. The usual dose is a 0.25 mg/kg bolus administered over a two-minute period. Diltiazem has a rapid onset of action. If effective, it should slow the patient's heart rate within three to seven minutes of administration. If the initial dose is ineffective in slowing the patient's heart rate, the bolus may be repeated at a higher dose of 0.35 mg/kg over two minutes. The patient's heart rate and rhythm and blood pressure should be monitored during administration. Bradycardia, bradyarrhythmias such as heart block, and hypotension may occur. To achieve or maintain rate control, a continuous infusion may be started following bolus administration. The infusion may be started at 10 mg/hour and increased in increments of 5 mg/hour to achieve rate control if no undesirable side effects occur. Diltiazem should be used with caution in patients with congestive heart failure, known pre-existing conduction defects, and significant hypotension [33,60].
Which of the following statements is TRUE regarding the use of esmolol in atrial fibrillation?
Click to ReviewEsmolol is a short-acting beta-adrenergic blocker that slows ventricular rate in atrial fibrillation by slowing conduction through the AV node. Initial administration is an IV bolus dose/loading dose of 0.5 mg/kg administered over one minute [28]. The bolus should be followed with an infusion of 0.05 mg/kg/min for four minutes. If the desired rate control is achieved, the infusion should be continued at that rate. If adequate rate control is not achieved at that dose, the bolus should be repeated followed by an infusion of 0.1 mg/min for four minutes. The total dose should not exceed 200 mcg/kg/min [33]. This procedure may be repeated until rate control is achieved or undesirable side effects occur. The patient's heart rate, ECG rhythm, and blood pressure should be monitored during the administration. Hypotension may occur. Once rate control is achieved, the infusion should be reduced to 0.025 mg/kg/min. Because esmolol has a short half-life, the therapeutic effects and side effects usually reverse within 10 to 20 minutes after the infusion is stopped. Because the therapeutic effects wear off quickly, care should be taken when switching the patient to an oral preparation to prevent relapse/loss of rate control. To transition the patient to oral medication, the first dose of the oral medication should be administered while the patient is still receiving esmolol. Thirty minutes after the first oral dose is given, the esmolol infusion should be reduced by one-half. The second dose of the oral agent should be administered at its scheduled time. One hour after the scheduled administration of the second oral dose, assess the patient's heart rate, ECG rhythm, and blood pressure. If rate control is maintained, the esmolol infusion may be discontinued. Note: Esmolol has no oral preparation; long-term control by oral agent requires a different agent [33].
A drug of choice for chronic rate control for persons in atrial fibrillation who also have an active lifestyle is
Click to ReviewOral diltiazem preparations provide chronic rate control in atrial fibrillation and are a drug of choice for persons who have a physically active lifestyle; however, their use for rate control is unlabeled [33]. Diltiazem comes in immediate- and extended-release forms. Immediate-release doses must be taken three to four times per day; extended-release forms require only daily dosing. In addition to bradycardia, hypotension, and heart block, other side effects of oral diltiazem include flushing, angina, insomnia, headache, nausea, syncope, and signs of congestive heart failure. Care should be taken when diltiazem is combined with negative inotropic drugs, other calcium channel blockers, and digoxin. Combination therapy increases the risk of bradycardia, conduction abnormalities, hypotension, and signs of congestive heart failure [33,60].
Severe digitalis toxicity may be reversed by the use of
Click to ReviewOral digoxin may be the first drug of choice for patients with atrial fibrillation and congestive heart failure caused by systolic dysfunction [67]. Digoxin does not provide adequate rate control during exercise or activity. The usual oral maintenance dose of digoxin is 0.125–0.25 mg daily. Serum digoxin levels should be monitored periodically. The patient should be monitored for signs of digitalis toxicity. The patient and/or family should be taught to recognize key signs of toxicity. These include nausea and vomiting, headache, unexplained weakness, malaise, and visual disturbances as well as slow heart rate. ECG changes that may occur with digitalis toxicity include sinus bradycardia, heart block, and multiple tachyarrhythmias. Digitalis toxicity is more likely to occur in elderly persons. Electrolyte imbalances such as hypokalemia, renal failure, or combined therapy with other antiarrhythmic agents may potentiate the effects of digoxin and increase the risk of digitalis toxicity. Severe digitalis toxicity may be treated with digoxin immune Fab [33].
Of the following, which statement most accurately describes the action of ibutilide?
Click to ReviewIbutilide is a drug approved by the FDA for the acute termination of atrial fibrillation and atrial flutter. A Class III antiarrhythmic, ibutilide acts by prolonging the duration of the action potential, the atrial refractory period, and the ventricular refractory period. It also slightly slows the sinus rate and conduction through the AV node. Ibutilide's exact mechanism of action is unknown [33]. On a cellular level, it has been reported to exert its effects by both blocking repolarizing potassium currents and initiating an inward depolarizing sodium current [56]. Ibutilide does not appear to have a direct impact on cardiac output, but monitoring for conduction disturbances and heart block is recommended [33].
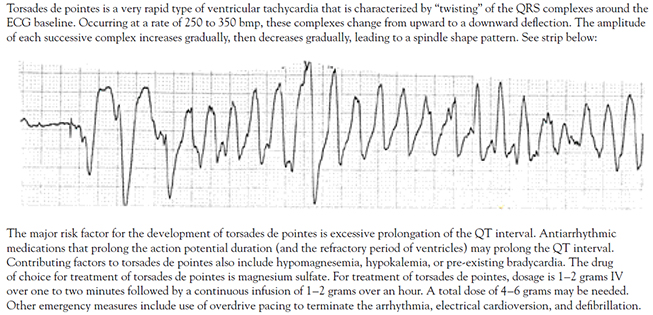
The treatment of choice for torsades de pointes is
Prior to initiating dofetilide therapy, other antiarrhythmic medications that prolong the QT interval should be
Click to ReviewFor persons with normal renal function, studies have shown that an oral dose of 500 mcg twice daily is effective in restoring normal sinus rhythm. In the presence of impaired renal function, the dose should be reduced. The dose may be as low as 125 mcg twice daily. The usual range for the maintenance dose (normal renal function) is 125–500 mcg twice daily. The administration protocol is as follows [33]:
Admit the patient to an inpatient facility approved for dofetilide administration.
Antiarrhythmic medications associated with prolonged QT interval (primarily Class I, Class III) should be discontinued; the guideline is at least three or more half-lives before initiation of dofetilide. Digoxin, beta blockers, and calcium channel blockers may be used to control ventricular rate during the withdrawal period of these drugs.
Electrolyte imbalances, especially potassium and magnesium, should be corrected before therapy is initiated.
QTc should be monitored periodically. Dosage should be reduced if QTc increases by more than 15% or exceeds 500 msec within two to three hours after initial dose. See the package labeling or website information for specific dosage reduction guidelines.
After the second dose, if the QTc interval is greater than 500 msec (or 550 msec in the presence of ventricular conduction abnormalities), dofetilide should be discontinued.
Continue ECG monitoring for a minimum of three days.
One toxic effect associated with amiodarone administration is
Click to ReviewAmiodarone has received increasing attention for its ability to convert atrial fibrillation to normal sinus rhythm and to prevent atrial fibrillation in patients undergoing CABG surgery [54,57,75]. Categorized as a Class III antiarrhythmic, amiodarone has properties of all four classes. It inhibits conduction through the AV node, prolongs the action potential and refractory period, and inhibits adrenergic stimulation. It may be safely used for patients with congestive heart failure, coronary artery disease, and persons with accessory pathway conduction. The proarrhythmic effects associated with amiodarone include bradycardia, heart block, ventricular fibrillation, and ventricular tachycardias including torsades de pointes. Hypotension may occur with IV administration. Amiodarone is associated with multiple severe side effects and toxic effects. These include pulmonary fibrosis, impaired vision from corneal deposits, photosensitive skin, thyroid dysfunction, and liver dysfunction [33,76]. Prior to beginning amiodarone therapy, the physician should obtain baseline data. Appropriate data includes a chest x-ray, pulmonary function tests, thyroid function tests, liver function tests, and renal studies. Patients receiving amiodarone therapy should be monitored for development of toxic effects. Serious toxicity, including death due to bradycardia ending in cardiac arrest, has been reported [33]. If symptoms develop, amiodarone should be discontinued. Use of the lowest effective maintenance dose is highly recommended due to the multitude and severity of side effects associated with amiodarone therapy. The FDA has issued a warning regarding concurrent use of amiodarone and simvastatin [77]. In patients who are taking both simvastatin and amiodarone, the dose of simvastatin should not exceed 20 mg/day [33,73].
Electrical cardioversion is the treatment of choice for persons with
Click to ReviewElectrical cardioversion has been found to be an effective and safe method for restoring normal sinus rhythm in a number of patients. It is the treatment of choice for persons with hemodynamically unstable atrial fibrillation [28]. Electrical cardioversion is also indicated for [28,40]:
Persons for whom there is a reasonable expectation that normal sinus rhythm can be restored and maintained
Persons who require "atrial kick" to relieve incapacitating or unpleasant symptoms, improve exercise tolerance, and increase their ability to perform their usual daily activities
Persons who would benefit from normal sinus rhythm but who have not been able to be successfully cardioverted pharmacologically (i.e., "failed" pharmacologic cardioversion)
Prior to electrical cardioversion, a patient should be adequately anticoagulated with an INR maintained between 2.0–3.0 for
Click to ReviewAppropriate anticoagulation management around the time of cardioversion is essential for reducing thromboembolic risk. Results of observational studies suggest that thromboembolic risk after cardioversion is highest in the first 72 hours and that the majority of events occur within 10 days [82]. As indicated, anticoagulation before cardioversion is required for most patients. Warfarin should be initiated, and the dose adjusted to reach and maintain a target goal of an international normalized ratio (INR) of 2.5 (range: 2.0 to 3.0). After the patient has been maintained for three weeks at that therapeutic goal, cardioversion may be performed. Following cardioversion, anticoagulation should be maintained for four weeks [28,40].
Because it prolongs the QT interval, disopyramide therapy is NOT recommended as a first drug of choice for patients with
Click to ReviewDisopyramide may be administered in a short- or sustained-release form. Because it prolongs the QT interval, it is not indicated as a first drug of choice for persons who also have hypertension. The combination of left ventricular hypertrophy caused by long-standing hypertension and a prolonged QT interval greatly increases the risk of proarrhythmias such as torsades de pointes [33].
The drug of choice for treatment of atrial fibrillation that has no identifiable cause is
Click to ReviewFlecainide is the drug of choice for the treatment of atrial fibrillation that has no identifiable cause. It is recommended for use only in the absence of structural heart disease and should not be prescribed for patients who have had a recent myocardial infarction or have abnormal left ventricular function [33].
For persons at low risk for cerebrovascular accident, the recommended anticoagulation therapy is
Click to ReviewTwo medications used commonly in prevention of thromboembolic events are aspirin and warfarin. They may be used singly or in combination to prevent thromboembolic events, but the efficacy of combination therapy has not been established [119,120,121,122]. Warfarin in comparison to aspirin leads to a 39% relative risk reduction in stroke [123]. Rather than adding aspirin, the AHA/ACC/HRS Task Force recommends increasing the intensity of the anticoagulant to a maximum target INR of 2.0–3.0 [28]. Aspirin acts by decreasing platelet aggregation. Because it offers only modest protection against stroke for patients with atrial fibrillation, its use may be considered for low-risk patients [28,49]. As noted, low-risk patients include those who are younger than 65 years of age and have no underlying cardiac disease. It may also be recommended for use in patients, particularly elderly persons, who cannot safely take warfarin. The usual adult dose of aspirin is 81–325 mg oral per day [49].
Which of the following is an indication for radiofrequency ablation of the AV node?
Click to ReviewRadiofrequency ablation of the AV node is an interventional therapy commonly used in the management of atrial fibrillation. The relative safety of radiofrequency energy has contributed to the widespread adoption of this technique as a therapeutic modality for atrial fibrillation [136,137]. Radiofrequency ablation has been found to be effective for persons who have significant symptoms with atrial fibrillation and/or poorly controlled ventricular rate who also [19,40,49,58,138,139]:
Have remained in atrial fibrillation despite attempts at electrical or pharmacologic cardioversion or who quickly revert to atrial fibrillation following cardioversion (referred to as "failed cardioversion")
Cannot take antiarrhythmic medications because of severe side effects or the development of proarrhythmias
Have inadequate rate control despite optimal dosing of appropriate antiarrhythmic agents
Which of the following interventions represent appropriate care following electrophysiology testing?
Click to ReviewELECTROPHYSIOLOGY TESTING AND ABLATION
Electrophysiology testing is an invasive diagnostic cardiovascular procedure that can confirm and pinpoint the location of accessory conduction pathway(s) in the heart. It is performed in a specially equipped cardiac catheterization lab. Multiple catheters are introduced through the femoral vein into the right side of the heart. Each catheter contains 4 to 16 electrodes for monitoring the heart's electrical activity. The catheters are positioned in various locations in the heart; common sites include the high right atrium, the apex of the right ventricle, the AV junction/His bundle, and the coronary sinus. During the procedure, specific pacing protocols are used to determine the location and characteristics of any accessory pathways. Based on the location and characteristics of the accessory pathway(s), a treatment plan will be developed. Treatment options include medical management of the syndrome and associated arrhythmias and radiofrequency ablation of the accessory pathway(s). If the pathway is to be ablated, another catheter (the ablation catheter) is advanced to the site, and more extensive/precise mapping of the accessory pathway is done. The location of the ablation catheter is adjusted until it is close to the pathway. Radiofrequency energy waves are applied to the pathway until pre-excitation disappears and the tachyarrhythmia cannot be restarted. The procedure may last from three to five hours. Postprocedure care involves bedrest, frequent vital signs, and observing the femoral insertion sites for bleeding or hematoma formation. The recommended postoperative therapy to prevent atrial fibrillation in patients who have undergone coronary artery bypass graft surgery is administration of
Click to ReviewFor prevention of postoperative atrial fibrillation following CABG, many sources recommend that beta-blocker therapy be initiated (or resumed) as soon as reasonably possible following surgery [156,158]. Use of a beta blocker for development of atrial fibrillation following cardiac surgery is a class I recommendation in AHA/ACC/HRS guidelines [28]. Prophylactic use of other antiarrhythmic agents has not been recommended. Use of digoxin has been found to have little effect and is not recommended [28]. Preoperative administration of statins may reduce postoperative atrial fibrillation and shorten the patient's stay on the ICU and in the hospital [28,159]. Studies have found that the postoperative prophylactic use of amiodarone reduces the risk of atrial fibrillation and decreases the total cost of care [158,160,161]. However, the use of amiodarone and other antiarrhythmic medications, such as calcium channel blockers and procainamide has been linked to the unacceptable side effects of bradycardia and hypotension [75]. Early intervention for patients who develop increasingly frequent premature atrial contractions (PACs) has been recommended by some clinicians. However, there is no consensus regarding the best treatment. Immediate intervention is indicated for persons who develop atrial fibrillation in the postoperative period. Based on an assessment of the patient's symptoms and hemodynamic status, medical treatment may involve intravenous medications for rate control, pharmacologic cardioversion, or electrical cardioversion along with identification and correction of factors that may contribute to the development of arrhythmias such as hypokalemia and hypomagnesemia. If atrial fibrillation persists despite appropriate therapy, anticoagulation therapy should be started as soon as the surgeon decides it is feasible. Four to six weeks following surgery, the patient's status should be re-evaluated [162,163]. In some persons, postoperative atrial fibrillation is a relatively transient arrhythmia that may spontaneously resolve. However, for others, the arrhythmia may persist and require medical management as previously described for persons with coronary artery disease [28,40].
ECG characteristics associated with Wolff- Parkinson-White syndrome include
Click to ReviewDuring early fetal development, a number of bundles of fibers exist that connect the atria and ventricles. As fetal development progresses, these connections disappear until the AV node is left as the only functional electrical connection between atria and ventricles. In persons with WPW, one or more of these fibrous connecting bundles has persisted into adulthood. The connecting bundle, called an accessory pathway, provides an alternative route for the conduction of an electrical impulse through the heart. Depending on a number of factors, an electrical impulse may travel only through the normal conducting pathway, through both the normal and the accessory pathways, or only through the accessory pathway. When the impulse travels through the accessory pathway, it bypasses the normal delay in the AV node and reaches the ventricles early. It initiates ventricular depolarization before the impulse traveling down the normal conduction pathway can reach the ventricles. The ventricles depolarize abnormally. The abnormal conduction through the accessory pathway alters the normal ECG waveform. The changes include [164]:
A shortened PR interval (less than 0.12 sec). The PR interval is shortened because the impulse from the atria reaches the ventricles through the accessory pathway more rapidly than normal.
The presence of a delta wave. A delta wave is a slurring of the initial deflection (either positive or negative) of the QRS complex. It reflects the early, abnormal depolarization of the ventricles that occurs when the impulse travels through the accessory pathway.
An abnormally widened QRS complex (greater than 0.12 sec). The widened, abnormal QRS occurs when most of the ventricular depolarization is stimulated by an impulse traveling down the accessory pathway. In normal conduction, both ventricles depolarize almost simultaneously. With accessory pathway conduction, one ventricle is stimulated to depolarize before the other.
Abnormal ST waves. An ST wave represents repolarization. When depolarization is abnormal, the pattern of repolarization will also be abnormal.
The initial drug of choice for the management of atrial fibrillation in Wolff-Parkinson-White syndrome is
Click to ReviewWhen a patient with WPW presents with atrial fibrillation with rapid ventricular response, the patient's hemodynamic status should be immediately assessed. If there are signs of hemodynamic instability, such as hypotension, signs of congestive heart failure, or ischemic chest pain, the patient should be immediately cardioverted [28,164]. If the patient is not hemodynamically unstable, rate control is the high priority. Appropriate medication selection is critical. Use of medications such as verapamil and digoxin that slow or block conduction through the AV node will aggravate atrial fibrillation in WPW and run the risk of accelerating the ventricular rate to the point that ventricular fibrillation can occur [33,164]. The treatment of choice for hemodynamically stable patients with atrial fibrillation and WPW is IV procainamide or ibutilide [28]. Verapamil, diltiazem, adenosine, digoxin (oral or intravenous), and intravenous amiodarone can precipitate ventricular fibrillation and should not be used [28].
In the case study of acute-onset atrial fibrillation, Patient D's risk factors for the development of atrial fibrillation include
Click to ReviewPatient D is a man, 68 years of age, who presents to the emergency department late one evening complaining of increasing shortness of breath, dizziness, and the sensation of his "heart racing." On admission, his heart rate is 160 bpm, blood pressure 100/50 mm Hg, respirations 26 breaths per minute, and oxygen saturation 88% on room air. Patient D says that his symptoms started abruptly earlier that day and have steadily become worse. He reports a history of long-standing hypertension, coronary artery disease, and a recent percutaneous transluminal angioplasty with placement of two stents.
Comments and rationale: Symptoms such as those Patient D presents are common indications of acute onset atrial fibrillation with rapid ventricular response. His past medical history is positive for risk factors for the development of atrial fibrillation. These include a positive cardiac history, with hypertension and coronary artery disease, as well as increasing age.
A QTc interval of 580 msec is
Click to ReviewLaboratory tests are ordered, including a complete blood count, serum electrolytes, renal and hepatic function tests, chest x-ray, urinalysis, and PT/INR. A peripheral IV access is established. Continuous telemetry monitoring is maintained, and Patient W's vital signs are monitored every four hours. Her heart rate remains between 48 and 52 bpm. Patient W's oral antiarrhythmic medication is discontinued. Analysis of Patient W's ECG shows that her QTc is 580 msec. The therapeutic options of electrical cardioversion, radiofrequency ablation, and continued oral antiarrhythmic therapy with insertion of a demand pacemaker are discussed with the patient. The patient expresses reluctance to undergo pacemaker insertion at this time. With the patient's agreement, she is scheduled for electrical cardioversion. Patient W expresses the understanding that pacemaker insertion or ablation with pacemaker insertion might still be required if cardioversion is unsuccessful or if she becomes symptomatic on therapy to maintain sinus rhythm following successful cardioversion.
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.