Study Points
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.
Study Points
Click on any objective to view test questions.
- Define burnout and its relationship to job dissatisfaction and stress.
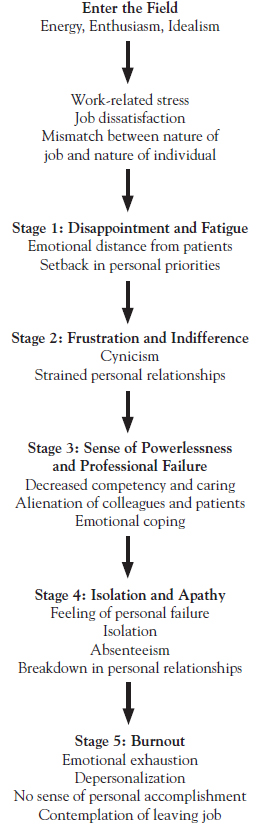
- Describe the developmental stages of burnout.
- Identify work environment and personal risk factors for burnout.
- Describe the personal and professional consequences of nursing burnout and the nursing shortage.
- Describe tools available to assess for and identify burnout.
- Identify strategies for individuals and institutions/organizations to help prevent and cope with burnout.
Burnout is described by Maslach as
Click to ReviewMaslach emphasizes that burnout is not a problem related to an individual [21]. Instead, her research indicates that burnout is a problem of the social environment in which people work and is a function of how people within that environment interact with one another and perform their jobs [21]. She notes that burnout is more likely when there is a "major mismatch between the nature of the job and the nature of the person who does the job" [21]. These mismatches are at the core of the development of burnout. The term burnout is now usually limited to mean burnout as described by Maslach: a syndrome of emotional exhaustion, depersonalization, and reduced personal accomplishment [18].
Isolation and apathy characterize which stage of burnout?
Among nurses, burnout is often directly linked to
Click to ReviewAmong nurses, burnout is often directly linked to work-related stress and job dissatisfaction. A systematic review demonstrated that work-related stress is significantly related to job satisfaction, with higher stress levels associated with less job satisfaction [70]. Further, low job satisfaction is associated with burnout [70]. In 2022, a large-scale survey of nearly 18,000 nurses showed that 71% were satisfied with their career choice (the majority reported they were "extremely satisfied"), a 10% decrease in satisfaction from the previous decade. The study found that about half of nurses reported feeling emotionally drained (50.8%), used up (56.4%), fatigued (49.7%), burned out (45.1%), or at the end of the rope (29.4%) a few times per week or every day [37]. Given these facts, an understanding of the prevalence and causes of job dissatisfaction among nurses can help to define the sources of stress and burnout. Studies have indicated that among nurses, factors within the work environment are greater predictors of job dissatisfaction and nurse retention than factors related directly to the care of patients [45].
In 2022, what was the top reason that nurses cited when leaving their job or position or for a different nursing job or position?
Click to ReviewREASONS GIVEN FOR LEAVING A NURSING JOB OR POSITION, 2022
Specific Work-Related Reason Percentage Leaving for a Different Nursing Job or Position Burnout 51.2% Inadequate staffing 46.1% Stressful work environment 45.3% Seeking better pay or benefits 41.1% Lack of good management/leadership 39.5% Received promotion or career advancement 23.7% Scheduling issues and inconveniences 22.7% High-risk working conditions 19.6% Physical demands of job 15.0% Lack of advancement opportunities 14.9% Leaving Nursing Completely Retirement 47.2% Burnout 35.8% Stressful work environment 28.3% Inadequate staffing 25.1% Lack of good management/leadership 23.2% Family caregiving obligations 18.2% Physical demands of job 13.5% Scheduling issues and inconveniences 13.1% High-risk working conditions 11.5% Lack of collaboration 9.3% With regard to setting, the highest rates of job dissatisfaction have been reported among nurses in which environment?
Click to ReviewWith regard to setting, the highest rates of job dissatisfaction have been reported among nurses in nursing homes and hospitals, even for nurses who do not provide direct patient care [45]. Job satisfaction in 2021 was highest among nurses employed in outpatient, ambulatory, and other clinical settings. In a survey of more than 95,000 nurses, the most common sources of dissatisfaction for hospital and nursing home nurses were opportunities to advance, professional status, work schedule, and independence at work [68]. Salary/wages and benefits (e.g., health insurance, retirement, tuition reimbursement) have also been common sources of dissatisfaction but have had little influence on burnout [68,69].
According to studies, the mean patient-to-nurse ratio in U.S. hospitals is
Click to ReviewA major source of burnout, work overload is created primarily by inadequate staffing, a prevalent problem in today's hospitals and nursing homes [65,69,72,79]. Studies have shown that the mean patient-to-nurse ratio in U.S. hospitals is approximately 5:1 [69,74]. Nurses have consistently reported that these ratios are inadequate for providing high-quality care. In a study of 534 hospitals (26,005 nurses), staffing was considered to be poor in 25% [69]. In a survey of nearly 11,000 RNs, only 46% said there was enough staff to accomplish the necessary work and 48% said there were not enough RNs on staff to provide high-quality care [67]. A 2022 survey showed that that only 33% of nurses had the time needed to spend with patients [43]. A 2021 study in New York State demonstrated a savings of 4,370 patient lives and a cost savings of $720 million when hospitals were staffed at a 4:1 patient-to-nurse ratio [44]. Increased patient-to-nurse ratios are associated with lower rates of job satisfaction and higher rates of burnout; inadequate staffing was the reason that 46.4% of still-employed nurses gave for changing their position or employer, and the reason that 35.8% of nurses left the profession altogether [7,45,70]. In a study of more than 10,000 nurses, the rate of burnout increased 23% for every additional patient per nurse [7].
In 2022, approximately what percentage of nurses worked more than 40 hours per week?
Click to ReviewOther factors also contribute to increased workload, including a high number of work hours per week, extended shifts, overtime (often mandatory), many consecutive days of work, rotating shifts, weekend work, and on-call requirements. Among more than 235,000 nurses in a 2022 survey, nearly 30% worked more than 40 hours per week, with 19% working 41 to 50 hours per week and 10.6% working more than 50 hours per week [37]. In addition to long work weeks, nurses typically work long workdays. Twelve-hour shifts offer many benefits to nurses and patient care, and as a result, the percentage of nurses who routinely work these shifts has increased to approximately 65% to 80% [94]. However, moderate-to-high levels of acute fatigue and moderate levels of chronic fatigue have been found among nurses working 12-hour shifts [95]. Several studies have indicated a strong relationship between long work hours or 12-hour shifts and adverse nurse outcomes, such as increased fatigue, job dissatisfaction, burnout, and intention to leave the job [94,96].
Studies have shown that nurses spend what percentage of their time at work on electronic health records and documentation requirements?
Click to ReviewDocumentation requirements with electronic health records are another source of stress and time. Studies have shown that nurses spend between 15% to 40% of their time at work on electronic health records and documentation requirements [6,80,81].
In a large survey of nurses, the highest level of satisfaction was given to relationships with
Click to ReviewIn one survey of 76,000 registered nurses, the highest level of satisfaction was given to relationships with other nurses. Still, the survey showed that one-third of nurses were dissatisfied with interactions with their peers [112]. A 2017 survey of 600 nurses found that 45% had been verbally harassed by other nurses [65]. Interpersonal conflict with other nurses is a stress factor in and of itself, but a lack of close working relationships deprives nurses of their colleagues as a source of support. This lack of support is important, as nurses have ranked their peers as providing the most support within the hospital community, and higher levels of support from co-workers have been related to lower levels of emotional exhaustion on the MBI. Similarly, lack of peer cohesion has correlated with high levels of emotional exhaustion and depersonalization, or cynicism [6].
Which of the following conflict resolution styles has associated with a lower rate of burnout among nurses?
Click to ReviewAlthough resolving conflicts can mitigate stress, the style of conflict resolution has also been a significant predictor of burnout. A study of three conflict resolution styles—avoidance, confrontational, and cooperative—showed that the avoidance and confrontational styles were associated with a higher rate of burnout, while the cooperative style was associated with a lower rate [113,114].
Which of the following statements regarding demographic risk factors for burnout is TRUE?
Click to ReviewEducational status seems to have an effect, with higher levels of burnout among workers with higher levels of education [18]. This difference could be the result of the expectations associated with advanced education and job choices [18].
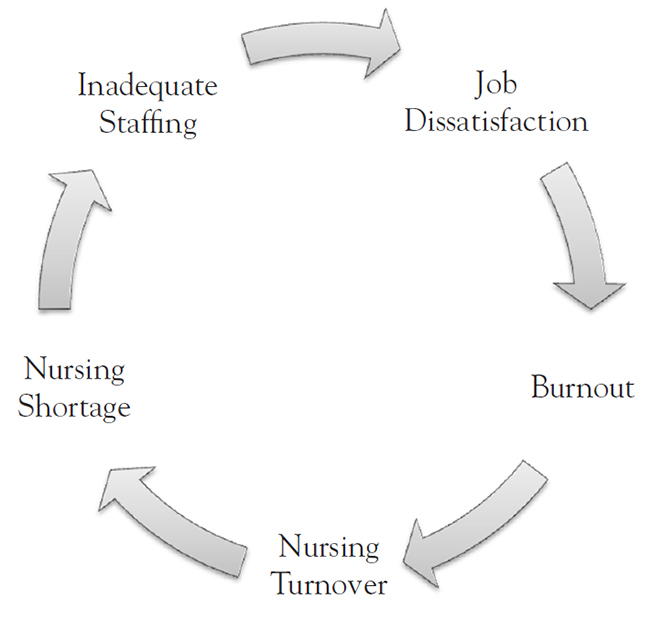
All of the following are part of the nursing shortage/burnout cycle, EXCEPT:
Click to ReviewWhat is the most common physical symptom of stress?
Click to ReviewMOST COMMON PHYSICAL AND PSYCHOLOGICAL SYMPTOMS RELATED TO STRESS
Symptoms Frequency Physical Headache 59% Fatigue 57% Change in sleep habits 53% Upset stomach 34% Muscle tension 30% Change in appetite 33% Psychological Feeling overwhelmed 57% Feeling depressed or sad 57% Nervousness/anxiety 56% Constant worrying 53% Difficulty making decisions 31% Forgetfulness 21% Which clinical entity, similar to burnout, occurs when an individual is exposed to the trauma or suffering of others, leading to emotional strain?
Click to ReviewCompassion fatigue (also called vicarious or secondary trauma) occurs when an individual is exposed to the trauma or suffering of others, leading to emotional strain [38]. Compassion fatigue may be the result of one or multiple instances of witnessing (directly or indirectly) suffering or trauma. An individual with compassion fatigue is often able to still care and be involved, although emotional distress can vary from mild to severe; an individual with burnout may become indifferent, cynical, disengaged, and distant. The major difference between compassion fatigue and burnout is the involvement of trauma; burnout is not trauma-related, but instead is the result of chronic workplace stress [38].
To better understand the specific source of burnout, which of the following tools can be used in conjunction with the Maslach Burnout Inventory (MBI)?
Click to ReviewThe Areas of Worklife Survey (AWS) is an assessment tool that is designed to be used in conjunction with the MBI, and measures the likely cause of burnout in the workplace based on six key areas: workload, control, reward, community, fairness, and values [39]. The AWS uses individual assessment to assist in determining strengths and weaknesses in an organization or work environment in order to determine areas of improvement or adjustment. It should be noted, however, that the MBI and AWS were not meant to be used as an isolated diagnostic tool. Rather, Maslach notes, "When the MBI is used correctly, and in strategic combination with other relevant information, the findings can help leaders design effective ways to build engagement and establish healthier workplaces in which employees will thrive" [56].
Because the length of the MBI/AWS may limit its usefulness, researchers have explored the use of single-item measures from the instrument. Studies of healthcare professionals have shown that responses to one question in the emotional exhaustion subscale ("I feel burned out from my work") and one statement in the depersonalization subscale ("I have become more callous toward people since I took this job") correlate well with the results of the full MBI [50,51]. More recently, a nonproprietary single-item measure has been shown to be a reliable substitute for the single-item measure on the emotional exhaustion subscale of the MBI [52].
The use of psychological assessment tools in conjunction with the MBI can help professionals gain a better understanding of the sources of stress for individuals. The General Health Questionnaire, developed by Goldberg, is designed to measure common mental health problems (domains of depression, anxiety, somatic symptoms, and social withdrawal) and was developed as a measure to identify individuals who are likely to have or be at risk for the development of psychiatric disorders [53]. The General Health Questionnaire is frequently used in conjunction with the MBI to evaluate psychological morbidity and burnout, as the pathways to both are related [54].
The General Health Questionnaire has been translated into several languages and is available in a variety of versions, with a range of 12 to 60 items; the version with 28 items (GHQ-28) has been used most often in workplace settings [54]. A score of 0 to 3 is assigned to four possible responses ("not at all," "no more than usual," "rather more than usual," and "much more than usual") to such questions as:
Have you found everything getting on top of you?
Have you been getting scared or panicky for no good reason?
Have you been getting edgy and bad tempered?
Which of the following is the most essential element of self-care in preventing burnout among nurses?
Click to ReviewThe concept of self-care is one that is emphasized in every book or article on preventing job stress and burnout across occupations. Self-care warrants particular emphasis for nurses, as they have been trained to put the care of others ahead of themselves. It is important for nurses to recognize that self-care is not equivalent to selfishness; rather, self-care is essential for energizing, restoring, and maintaining the physical and emotional stamina to reduce fatigue and manage stress Research has shown that self-care strategies are associated with lower levels of burnout among nurses [18,119,124,125]. Self-care involves several universal lifestyle habits, such as proper diet, exercise, sleep, and regular health care. Maintaining a healthy lifestyle through these habits is vital to avoiding the physical effects of stress [2]. The need for appropriate sleep hygiene is the most essential element for nurses, as fatigue can have serious outcomes for both the nurse and patient. One study showed that 49% of nurses at an academic medical center averaged less than the recommended 7 hours of sleep per night, and the overall average nightly sleep time was only 6.6 hours. In addition, 27% used medication to help them sleep, and 13% used medications to stay awake. Symptoms consistent with chronic insomnia were identified in 31% of nurses sampled [33]. In 2020, the Well-Being Initiative, a collaborative effort by multiple nursing associations, published the Guide to Sleeping Better and Restoring Energy for nurses, after finding that 72.8% of nurses are suffering with sleep challenges (either excessive sleep or sleeplessness) [34]. There is widespread documentation that sleep disturbances are associated with a high risk of fatigue, which is linked to job satisfaction and burnout [117,119,124,125]. The following are recommended for proper sleep, nutrition, and exercise needed to alleviate stress and prevent burnout [34,119,125]:
Prioritize sleep
Maintain a regular sleep schedule on duty and off-duty days.
Try to get 7 to 9 hours in a 24-hour period.
Create a comfortable, cool, dark sleeping environment.
Wind down with gentle stretches, meditation, or progressive relaxation exercises.
Track sleep with wearable fitness tracker, phone, or sleep diary.
Restore energy
Use light to prompt wakefulness (open a window or turn on a light).
Take mental breaks to walk or practice mindfulness.
Eat healthy foods and do not skip meals.
Monitor caffeine (limit intake to 400 mg per day, avoid six hours prior to sleep, do not use as a substitute for sleep).
Take a 20-minute nap to restore energy or longer if needed to catch up on sleep.
If necessary, "bank" sleep ahead of time to prepare for longer periods of no sleep.
Participate in regular exercise—find activities that fit into your daily routine
Do not rely on medications to enhance alertness
Which of the following approaches are useful to help nurses restore energy?
Click to ReviewThe concept of self-care is one that is emphasized in every book or article on preventing job stress and burnout across occupations. Self-care warrants particular emphasis for nurses, as they have been trained to put the care of others ahead of themselves. It is important for nurses to recognize that self-care is not equivalent to selfishness; rather, self-care is essential for energizing, restoring, and maintaining the physical and emotional stamina to reduce fatigue and manage stress Research has shown that self-care strategies are associated with lower levels of burnout among nurses [18,119,124,125]. Self-care involves several universal lifestyle habits, such as proper diet, exercise, sleep, and regular health care. Maintaining a healthy lifestyle through these habits is vital to avoiding the physical effects of stress [2]. The need for appropriate sleep hygiene is the most essential element for nurses, as fatigue can have serious outcomes for both the nurse and patient. One study showed that 49% of nurses at an academic medical center averaged less than the recommended 7 hours of sleep per night, and the overall average nightly sleep time was only 6.6 hours. In addition, 27% used medication to help them sleep, and 13% used medications to stay awake. Symptoms consistent with chronic insomnia were identified in 31% of nurses sampled [33]. In 2020, the Well-Being Initiative, a collaborative effort by multiple nursing associations, published the Guide to Sleeping Better and Restoring Energy for nurses, after finding that 72.8% of nurses are suffering with sleep challenges (either excessive sleep or sleeplessness) [34]. There is widespread documentation that sleep disturbances are associated with a high risk of fatigue, which is linked to job satisfaction and burnout [117,119,124,125]. The following are recommended for proper sleep, nutrition, and exercise needed to alleviate stress and prevent burnout [34,119,125]:
Prioritize sleep
Maintain a regular sleep schedule on duty and off-duty days.
Try to get 7 to 9 hours in a 24-hour period.
Create a comfortable, cool, dark sleeping environment.
Wind down with gentle stretches, meditation, or progressive relaxation exercises.
Track sleep with wearable fitness tracker, phone, or sleep diary.
Restore energy
Use light to prompt wakefulness (open a window or turn on a light).
Take mental breaks to walk or practice mindfulness.
Eat healthy foods and do not skip meals.
Monitor caffeine (limit intake to 400 mg per day, avoid six hours prior to sleep, do not use as a substitute for sleep).
Take a 20-minute nap to restore energy or longer if needed to catch up on sleep.
If necessary, "bank" sleep ahead of time to prepare for longer periods of no sleep.
Participate in regular exercise—find activities that fit into your daily routine
Do not rely on medications to enhance alertness
All of the following tactics for "working smarter" should be especially emphasized to nurses, EXCEPT:
Click to ReviewMaslach defined working smarter as setting realistic goals, doing things differently (when possible), not taking things personally, and taking time away [18]. Setting realistic goals involves moving from abstract, idealistic goals to well-defined specific goals, which can help individuals gain a better sense of accomplishment. Varying work routines can help avoid feelings of being in a rut and provide a sense of better control. Taking things less personally involves objectifying negative interactions and situations to help decrease emotional involvement, thereby reducing stress.
Working smarter also means taking time away and organizing time more effectively. A typical response to work overload is to work longer or harder to help make the situation "get better" [18]. However, this approach will only exacerbate stress and burnout, not relieve it. The need to take some time away from work must be especially emphasized to nurses, most of whom do not routinely take breaks or do not take effective breaks. One study showed that appropriate breaks were least likely among nurses working the longest hours, and that approximately 60% of nurses are usually not completely free of patient care responsibilities during breaks for rest or meals [93]. Rest breaks are particularly important for nurses working the night shift, to relieve symptoms of fatigue, which can be detrimental to both nurses' well-being and patient safety [6,97]. Taking some time away from work—even if only a few minutes at a time—to stretch, take a walk, make a personal phone call, read, meditate, or just sit and relax can help nurses "recharge" and will improve performance and increase productivity more effectively than working continuously [1]. Facilities must help ensure that nurses take breaks and meals appropriately, as will be discussed later. Other time management techniques include scheduling a block of unplugged, uninterrupted time (no phones, pagers, or e-mails) to complete paperwork more efficiently, creating "to do" lists to maintain control over tasks, and increasing organizational skills [1,104].
Which of the following is NOT one of the components of the American Association of Critical-Care Nurses' standards for a healthy work environment?
Click to ReviewOrganizations and institutions can help protect nurses from burnout by creating an organizational culture of trust, support, and open communication and fostering a healthy work environment [6,18]. Creating a healthy work environment has become a priority for enhancing nurse job satisfaction and retention and improving patient safety and satisfaction. The American Association of Critical-Care Nurses (AACN) developed standards for a healthy work environment, noting that such an environment is necessary for clinical excellence and good patient outcomes. Six components were noted to be essential for establishing and sustaining a healthy work environment [101]:
Appropriate staffing
Meaningful recognition
True collaboration
Skilled communication
Effective decision making
Authentic leadership
Which of the following has been recommended by many nursing associations to address fatigue?
Click to ReviewInstitutions should also consider implementing innovative measures to ensure that nurses take breaks and meal periods. Some interventions that have been successful are encouraging going outside for breaks, setting longer meal periods, adding shorter shifts to cover meal periods, a buddy system for breaks, tuning off cell phones and pagers during breaks, nurse managers' coverage of breaks, and monitoring and documentation of breaks to ensure they are taken [88,102].
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.